Coronary artery disease affects millions worldwide. It often needs more than just medicine. Angioplasty is a common treatment, but there are other choices too. Many patients get other treatments based on how bad their disease is.
Coronary artery bypass grafting (CABG) is a big surgical option. We’ll look at this and other choices. We’ll compare stent placement and bypass surgery to see their good and bad sides.
Patients should be informed about these treatment options. This helps them make better choices about their health. We’ll go into detail about each treatment. This will help you understand how to manage coronary artery disease.
Key Takeaways
- Coronary artery disease often requires intervention beyond medication.
- CABG is a commonly recommended surgical alternative to angioplasty.
- Stent placement and bypass surgery are both viable treatment options.
- Each treatment has its benefits and associated risks.
- Understanding the alternatives is key for making informed decisions.
Understanding Coronary Artery Disease

Knowing about coronary artery disease is key to keeping your heart healthy. It happens when plaque builds up in artery walls. This can cut down blood flow to the heart, leading to heart attacks or other serious issues.
How Plaque Builds Up in Arteries
Plaque buildup starts with damage to the artery’s inner layer. High blood pressure, smoking, and high cholesterol can cause this damage. Over time, the plaque narrows the artery and limits blood flow.
As plaque grows, it can become unstable and rupture. This can cause a blood clot to form, blocking the artery. This blockage can lead to a heart attack. Knowing how this happens helps in preventing and managing the disease.
Symptoms and Warning Signs
Coronary artery disease often doesn’t show symptoms until it’s advanced. But, there are signs to watch for, like:
- Chest pain or discomfort (angina)
- Shortness of breath
- Fatigue
- Pain or weakness in the arms or legs
These symptoms happen because the heart isn’t getting enough oxygen-rich blood. If you notice any of these, get medical help right away.
Risk Factors for Coronary Artery Disease
Several factors can lead to coronary artery disease. These include:
- High Blood Pressure: High blood pressure can damage arteries, making them more prone to plaque buildup.
- High Cholesterol: High levels of LDL cholesterol can help form plaque.
- Smoking: Smoking harms the arteries’ inner lining and raises the risk of plaque buildup.
- Diabetes: Diabetes can damage arteries and increase the risk of heart disease.
- Family History: A family history of heart disease can raise your risk.
Knowing these risk factors helps in preventing and catching coronary artery disease early. Tests like a cardiac nuclear scan or nuclear stress test are key in diagnosing and assessing the disease. It’s also important to be aware of the risks, like nuclear stress test radiation, and talk about them with your doctor.
The Basics of Angioplasty and Stent Placement
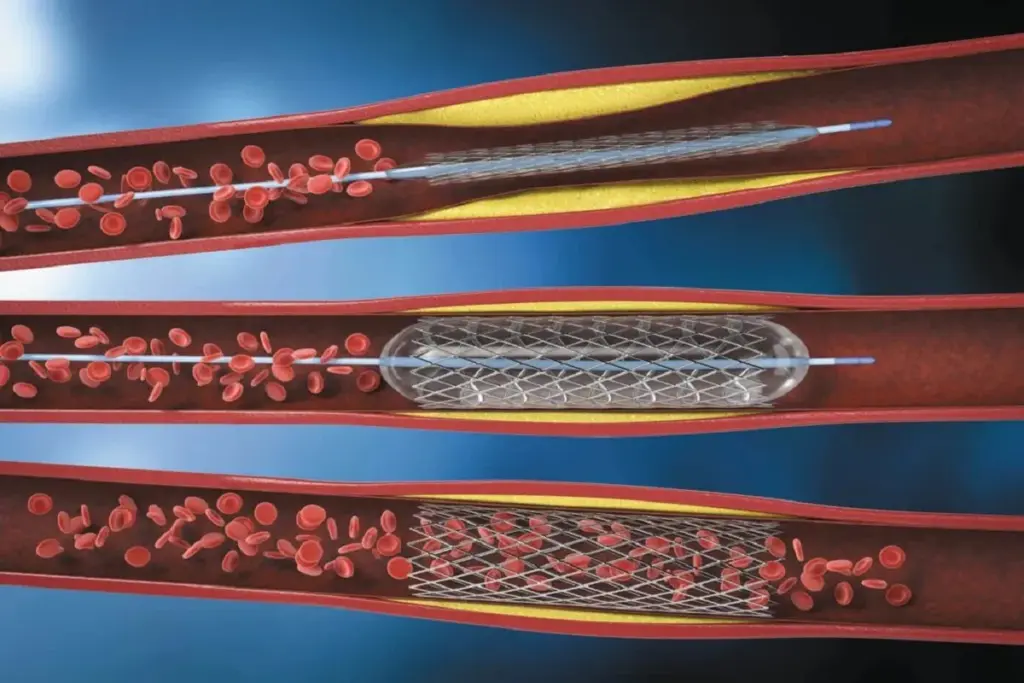
Angioplasty and stent placement have changed how we treat blocked arteries. This method is less invasive and helps many patients. It’s important to know what it involves, its benefits, and the different stents available.
What is Angioplasty with Stent?
Angioplasty with stent placement widens blocked arteries. “Angioplasty” uses a balloon to open the artery. “Stent placement” uses a mesh-like device to keep it open. This method improves blood flow to the heart and reduces symptoms of coronary artery disease.
A thin, flexible tube called a catheter is used. It goes through an artery in the leg or arm to the blocked artery. A balloon is then inflated to push plaque against the walls. A stent is placed to keep the artery open.
The Procedure Process
The procedure involves several steps:
- Preparation: Patients are given local anesthesia and, if necessary, sedation to relax.
- Catheter Insertion: A catheter is inserted into an artery and guided to the blocked coronary artery.
- Balloon Angioplasty: A balloon is inflated to widen the artery.
- Stent Deployment: A stent is placed to keep the artery open.
- Post-Procedure: The catheter is removed, and the artery is monitored for any complications.
The entire process is closely monitored using imaging technologies like angiography to ensure precision and safety.
Types of Coronary Stents
There are several types of coronary stents, each designed for specific needs:
- Bare-Metal Stents: Simple metal mesh stents that provide structural support.
- Drug-Eluting Stents: Stents coated with medication that helps prevent the artery from re-narrowing.
- Bioresorbable Stents: Stents made from materials that gradually dissolve, potentially reducing long-term complications.
The right stent depends on the patient’s health, the blockage’s location and severity, and past experiences.
Medical technology keeps improving, giving patients more treatment options for angioplasty and stent placement.
Limitations and Risks of Angioplasty
Angioplasty is a common treatment for heart disease. But, it’s important to know its limits and risks. We’ll look at the possible problems and how they can vary from person to person.
Potential Complications
Like any medical procedure, angioplasty can have complications. These might include bleeding, damage to blood vessels, or allergic reactions to dye. More serious issues like heart attack, stroke, or death are rare but possible. We’ll dive into these risks to help you know what to expect.
There are also long-term risks. One big worry is restenosis, when arteries narrow again after treatment.
Restenosis and Stent Failure
Restenosis is a big worry for those with stents. Stent failure can happen when the stent gets blocked. This can lead to symptoms coming back or even a heart attack. We’ll look at why this happens and how to reduce the risk.
When Angioplasty May Not Be Suitable
Angioplasty works for many with heart disease. But, it’s not for everyone. The choice depends on the blockage’s severity, your health, and other conditions. We’ll talk about who might not be a good candidate for angioplasty.
Knowing the limits and risks helps in making treatment choices. By understanding these, patients can work with doctors to find the best treatment for their heart disease.
Coronary Artery Bypass Graft (CABG) Surgery
For those with complex heart disease, CABG surgery is a good option. It creates a new path for blood to flow to the heart. This helps improve heart function.
What is Bypass Surgery?
CABG surgery, or heart bypass, helps with heart disease. It makes a new path for blood to flow. This is done by using a graft from another part of the body.
This surgery is for those with severe heart disease. It’s chosen after tests show it’s needed. These tests include coronary angiography.
The Surgical Procedure
The surgery starts with general anesthesia. This keeps the patient pain-free. The surgeon then opens the chest to reach the heart.
Depending on the heart’s condition, the surgery might use a heart-lung machine. The graft is then attached to the artery. The chest is closed, and the patient is moved to the ICU for recovery.
Types of Bypass Grafts
There are various grafts used in CABG surgery:
- Venous Grafts: These come from the leg’s saphenous vein. They are common because of their length and availability.
- Arterial Grafts: These are from the internal mammary artery or radial artery. They last longer than venous grafts.
The choice of graft depends on the patient’s health and the disease’s extent. Arterial grafts, like the left internal mammary artery, are preferred for their long-term success.
Stent vs Bypass: Comparing Treatment Options
Stent placement and CABG surgery are two ways to treat coronary artery disease. Each has its own benefits and drawbacks. It’s important to look at several key factors to see which treatment works best for each patient.
Invasiveness and Surgical Risk
Choosing between stent placement and CABG surgery often comes down to how invasive the procedure is. Stent placement is less invasive, done under local anesthesia, and only requires a small incision. CABG surgery, on the other hand, is more invasive, needing a larger chest incision and a heart-lung machine.
“Stent placement is a good choice for those at high risk for major surgery complications,” says a leading cardiologist. Yet, CABG surgery can be better for complex or multi-vessel disease.
Recovery Time and Hospital Stay
Recovery times and hospital stays vary between stent placement and CABG surgery. Stent placement usually means a quick recovery, with patients often going home the same day. CABG surgery, though, requires a longer hospital stay and recovery at home.
A study found that CABG patients stayed in the hospital for 6 days, while stent patients stayed for 1 day. This difference affects a patient’s quality of life and ability to get back to normal activities.
Long-term Effectiveness and Durability
Looking at long-term results, stent placement and CABG surgery have different outcomes. Stents can provide short-term relief but may fail over time. CABG surgery, though more invasive, offers durable results, mainly for complex disease.
A study showed CABG surgery had fewer major cardiac events at 5 years than stent placement. This means CABG might be a better long-term choice for some patients.
In conclusion, the choice between stent placement and CABG surgery depends on several factors. These include disease severity, patient health, and personal preferences. Understanding the differences in invasiveness, recovery, and long-term results helps patients make informed decisions.
Medical Therapy as an Alternative
Medical therapy includes medication and lifestyle changes. It’s key in treating coronary artery disease. This method helps manage symptoms, slow disease growth, and improve life quality.
Medication Options for Coronary Artery Disease
Many medications help manage coronary artery disease. Each has a specific role:
- Antiplatelet agents: Stop blood clots from forming.
- Beta-blockers: Make the heart work less and need less oxygen.
- Statins: Lower bad cholesterol levels.
- ACE inhibitors: Relax blood vessels, lower blood pressure, and ease heart strain.
|
Medication Type |
Purpose |
Examples |
|---|---|---|
|
Antiplatelet agents |
Prevent blood clots |
Aspirin, Clopidogrel |
|
Beta-blockers |
Reduce heart workload |
Metoprolol, Atenolol |
|
Statins |
Lower cholesterol |
Atorvastatin, Simvastatin |
|
ACE inhibitors |
Relax blood vessels |
Lisinopril, Enalapril |
Lifestyle Modifications
Lifestyle changes are also vital in managing coronary artery disease. These include:
- Dietary changes: Eat a heart-healthy diet low in fats, cholesterol, and sodium.
- Exercise: Stay active to boost heart health.
- Smoking cessation: Quit smoking to lower heart risk.
- Weight management: Keep a healthy weight to ease heart strain.
When Medical Therapy is Preferred
Medical therapy is often chosen for mild to moderate coronary artery disease. It’s preferred when the risks of surgery are higher. The decision depends on symptom severity, disease extent, and overall health.
With proper medical therapy, many patients can live active, fulfilling lives. This approach reduces the need for more invasive treatments.
Minimally Invasive Cardiac Surgery Options
Medical technology has improved a lot, leading to new ways to do heart surgery. These new methods are safer and less painful than old ways. They help patients heal faster and feel less pain.
Robotic-Assisted Procedures
Robotic-assisted heart surgery uses special robots to help surgeons. These robots make it easier to do complex surgeries through small cuts. This means less damage to the body and quicker healing.
It also makes surgeries more precise and lowers the risk of problems. Patients often stay in the hospital for less time.
Off-Pump Bypass Surgery
Off-pump bypass surgery is done while the heart keeps beating. It doesn’t need a heart-lung machine. This might lower the risk of some complications.
It’s good for people with certain health issues or those at high risk for other surgeries.
Minimally Invasive Direct Coronary Artery Bypass (MIDCAB)
MIDCAB is a way to do heart surgery with a small cut. It’s less invasive than traditional surgery. This means less pain and faster recovery.
It’s often used for people with single-vessel disease. Or for those who can’t have more invasive surgeries.
The following table summarizes the key aspects of the minimally invasive cardiac surgery options discussed:
|
Surgical Technique |
Key Benefits |
Potential Risks |
|---|---|---|
|
Robotic-Assisted Procedures |
Improved precision, less tissue damage, quicker recovery |
Technical malfunctions, longer operative times |
|
Off-Pump Bypass Surgery |
Avoids cardiopulmonary bypass, potentially fewer complications |
Increased complexity, possible incomplete revascularization |
|
MIDCAB |
Less invasive, less postoperative pain, faster recovery |
Limited to single-vessel disease, technically challenging |
Knowing about these options helps patients and doctors make better choices. Each method has its own good points and possible downsides. The right choice depends on the patient and the surgeon’s skills.
Enhanced External Counterpulsation (EECP) Therapy
EECP therapy is a new treatment for heart disease. It’s non-invasive, meaning it doesn’t require surgery. This makes it a promising option for improving blood flow to the heart.
The Mechanism of EECP Therapy
EECP therapy uses inflatable cuffs on the legs. These cuffs inflate and deflate with the heartbeat. This helps blood flow back to the heart better.
Who Can Benefit from EECP Treatment
EECP is for patients with coronary artery disease. It’s for those who don’t want surgery or haven’t seen results from other treatments. It’s also for patients who can’t have surgery because of other health issues.
Effectiveness and Limitations of EECP
EECP’s success varies. Some patients see big improvements, while others don’t. It’s important to talk to a doctor about the pros and cons to see if it’s right for you.
|
Benefits |
Limitations |
|---|---|
|
Non-invasive procedure |
Variable effectiveness among patients |
|
No surgical risks |
May require multiple sessions |
|
Potential improvement in symptoms and quality of life |
Not suitable for all patients with coronary artery disease |
Knowing how EECP works and who it helps is key. This way, patients and doctors can decide if it’s part of a good care plan.
Nuclear Stress Tests for Cardiac Evaluation
Nuclear stress tests are key in cardiology. They help understand the heart’s function and spot coronary artery disease. These tests check how well the heart muscle gets blood, even when stressed.
How Nuclear Stress Tests Work
A nuclear stress test has two parts: at rest and under stress. A tiny amount of radioactive tracer is injected into the blood. This tracer builds up in heart muscle areas with good blood flow.
Using a special camera, images of the heart are taken at rest and after stress. This lets doctors see how blood flow changes.
Nuclear Stress Test vs Angiogram
Nuclear stress tests and angiograms both help find coronary artery disease. But they do different things. An angiogram shows the coronary arteries’ details, like blockages.
A nuclear stress test, on the other hand, checks how well the heart muscle works and blood flows. We often use both tests together for a full heart health picture.
Cardiac Nuclear Imaging Procedures
Cardiac nuclear imaging includes many tests, like nuclear stress tests. These tests use small amounts of radioactive materials. They help diagnose and treat diseases like cancer, heart disease, and more.
Radiation Concerns in Cardiac Testing
Cardiac testing often uses procedures that expose patients to radiation. This raises concerns about risks. Nuclear stress tests, used to check for heart disease, involve radioactive material.
It’s important to understand the risks of radiation exposure. We’ll look at the risks of nuclear stress tests, the dangers, and how to reduce them.
Nuclear Stress Test Radiation Exposure
A nuclear stress test injects a radioactive tracer into the blood. The amount of radiation varies by the tracer and dose. Typically, it’s between 9 to 21 millisieverts (mSv).
For comparison, we get about 3 mSv of background radiation a year. So, a nuclear stress test is like getting several years’ worth of background radiation.
Is a Nuclear Stress Test Dangerous?
The main worry is the risk of cancer from radiation. The risk is small but not zero. For example, 10 mSv might increase the risk of fatal cancer by 1 in 2,000.
But, the test’s benefits must be weighed against the risks. For many, the test’s information is vital for heart disease management.
|
Radiation Dose (mSv) |
Estimated Lifetime Risk of Fatal Cancer |
|---|---|
|
10 |
1 in 2,000 |
|
20 |
1 in 1,000 |
Minimizing Radiation Risk
To lower radiation exposure, several steps can be taken:
- Use the least amount of radioactive tracer needed.
- Use newer, lower-radiation technologies.
- Choose patients carefully, making sure the test is needed.
- Consider non-radiation tests, like stress echocardiography, when possible.
By taking these steps, healthcare providers can reduce radiation risks. They can also get important diagnostic information.
Alternative Cardiac Imaging Tests
Cardiac imaging has grown, giving us many options instead of nuclear stress tests. We’ll look at CT angiograms, echocardiograms, and cardiac stress tests with contrast. We’ll see what each offers and what they can’t do.
CT Angiogram vs Nuclear Stress Test
A CT angiogram is a non-invasive test that uses X-rays to show the heart’s arteries. It’s different from nuclear stress tests because it clearly shows the arteries. This helps find blockages and plaque.
Key differences:
- CT angiograms are more accurate in detecting coronary artery disease.
- Nuclear stress tests evaluate heart function under stress.
- CT angiograms involve radiation exposure, but often less than nuclear stress tests.
|
Test |
Accuracy in Detecting CAD |
Radiation Exposure |
|---|---|---|
|
CT Angiogram |
High |
Moderate |
|
Nuclear Stress Test |
Moderate |
Higher |
Echocardiogram vs Nuclear Stress Test
An echocardiogram uses sound waves to create images of the heart. It checks the heart’s structure and function. It doesn’t show the coronary arteries directly but can spot heart problems.
Key differences:
- Echocardiograms are non-invasive and do not involve radiation.
- Nuclear stress tests provide information on heart function under stress.
- Echocardiograms can be used for a broader assessment of heart health.
|
Test |
Radiation |
Assessment |
|---|---|---|
|
Echocardiogram |
No |
Heart structure and function |
|
Nuclear Stress Test |
Yes |
Heart function under stress |
Cardiac Stress Test with Contrast
A cardiac stress test with contrast uses a contrast agent to improve imaging. It can be done with echocardiography or nuclear imaging. This gives clearer images of the heart’s function.
Benefits:
- Improved image quality.
- Better assessment of heart function.
- Can be used with various imaging modalities.
Understanding each cardiac imaging test’s strengths and weaknesses helps doctors choose the best one. These tests offer many benefits, like less radiation and better accuracy.
How Doctors Determine the Best Treatment Option
Choosing the right treatment for coronary artery disease is complex. We look at many factors to find the best plan. This ensures the treatment works well for each patient.
Severity and Location of Blockages
The size and spot of blockages in the heart’s arteries are key. Angiograms show us where and how bad these blockages are.
Big blockages or those in important spots might need CABG (Coronary Artery Bypass Grafting) or stenting.
Patient Age and Overall Health
A patient’s age and health are big factors. Older patients or those with health issues need careful treatment.
We check the patient’s health, including diabetes, high blood pressure, or kidney disease. This helps us make a treatment plan that fits.
Presence of Other Medical Conditions
Other health problems can change the treatment choice. For example, severe lung disease might make open-heart surgery risky.
We look at how other health issues affect coronary artery disease and its treatment. This ensures we provide the best care.
|
Factor |
Considerations |
Impact on Treatment |
|---|---|---|
|
Severity and Location of Blockages |
Extent and location of coronary artery blockages |
Influences choice between CABG, angioplasty, or medical therapy |
|
Patient Age and Overall Health |
Age, overall health status, presence of comorbidities |
Affects the risk assessment for surgical procedures |
|
Presence of Other Medical Conditions |
Presence of conditions like diabetes, hypertension |
Impacts the suitability of certain treatments and overall management |
Patient Decision-Making Factors
When you get a diagnosis of coronary artery disease, you face big decisions. It’s key to know that making these choices involves many factors.
Understanding Your Diagnosis
Knowing your diagnosis is the first step in making good choices about your health. Your cardiologist will tell you about your coronary artery disease. They’ll explain where and how bad the blockages are. It’s important to ask questions to get a clear picture of your situation.
Key aspects to understand include:
- The severity of your coronary artery disease
- The location of blockages and their impact on your heart
- Any symptoms you’re experiencing and how they relate to your condition
Questions to Ask Your Cardiologist
Asking the right questions helps you make informed choices. Some important questions to ask your cardiologist are:
- What are the benefits and risks of each treatment option?
- How will the recommended treatment affect my quality of life?
- Are there other treatments or therapies that might be good for my condition?
Talking about your personal preferences and concerns with your cardiologist is also important.
Getting a Second Opinion
Getting a second opinion can give you more insight and confidence in your treatment plan. It’s a common step that can help you feel more sure about your care choices.
When seeking a second opinion, consider:
- Talking to a specialist who knows a lot about coronary artery disease
- Discussing your diagnosis and treatment plan with the second doctor
- Learning about any new treatment options or therapies
By understanding your diagnosis, asking the right questions, and getting a second opinion, you can make informed decisions. This way, you can actively manage your coronary artery disease.
Recovery and Rehabilitation After Treatment
Recovery and rehabilitation are key to helping patients get back to their normal lives after treating coronary artery disease. This process includes post-procedure care, making lifestyle changes, and joining cardiac rehabilitation programs.
Post-Angioplasty Recovery
After an angioplasty, patients usually need to rest for a few days. It’s important to avoid heavy lifting and strenuous activities during this time. Most people can go back to work in about a week. But, it’s vital to follow the specific instructions from your healthcare provider.
Key aspects of post-angioplasty recovery include:
- Monitoring the puncture site for any signs of bleeding or infection
- Adhering to prescribed medications, including antiplatelet therapy
- Gradually resuming normal activities as advised by your doctor
Post-Bypass Surgery Recovery
Recovery after coronary artery bypass graft (CABG) surgery is longer and more involved than after angioplasty. We know this can be tough for patients. Our team is here to support and guide you through this time.
Some key considerations for post-bypass surgery recovery include:
- Hospital stay typically ranges from 5 to 7 days
- Full recovery can take several weeks to a few months
- Patients are advised to avoid heavy lifting and driving for several weeks
Cardiac Rehabilitation Programs
Cardiac rehabilitation is a vital part of recovery after treating coronary artery disease. These programs aim to improve heart health, reduce symptoms, and enhance quality of life.
Components of cardiac rehabilitation programs typically include:
- Exercise training to improve cardiovascular health
- Education on heart-healthy lifestyle choices
- Stress management and counseling
- Monitoring of progress and adjustment of treatment plans as needed
By joining cardiac rehabilitation, patients can greatly improve their outcomes and lower the risk of future heart issues. We encourage all patients to talk to their healthcare providers about these programs. This will help determine the best approach for their individual needs.
Conclusion
Treatment for coronary artery disease goes beyond just angioplasty. Options like stent placement and coronary artery bypass grafting (CABG) are also available. Knowing the differences between these choices is key to making the right decision for your care.
We’ve looked at many treatments for coronary artery disease. These include medical therapy, lifestyle changes, and even surgery like CABG. Each person’s case is different. The best treatment depends on the blockage’s severity, your overall health, and any other health issues you might have.
It’s important for patients to talk to their cardiologist about the best treatment plan. By understanding the options and what they mean, you can make a choice that fits your needs. This can help improve your health outcomes.
FAQ
What is the difference between a nuclear stress test and an angiogram?
A nuclear stress test is a non-invasive test that uses a small amount of radioactive material. It images the heart and its blood vessels. On the other hand, an angiogram is an invasive test. It uses contrast dye and X-rays to see the coronary arteries.
Is a nuclear stress test dangerous?
A nuclear stress test is generally safe. But, it does involve a small amount of radiation. This can be a worry for some patients. Yet, the benefits of the test usually outweigh the risks.
What are the risks of a nuclear stress test?
The risks of a nuclear stress test include radiation exposure and allergic reactions to the radioactive material. There’s also a chance of false positive or false negative results. Rarely, the test can cause a heart attack or other serious complications.
How much radiation is in a nuclear stress test?
The radiation exposure from a nuclear stress test varies. It depends on the test and the patient’s characteristics. The effective dose is usually around 10-20 millisieverts (mSv).
What are the alternatives to a nuclear stress test?
Alternatives include CT angiograms, echocardiograms, and cardiac stress tests with contrast. These tests can give similar information. But, they have different risks and benefits.
What is the difference between a stent and bypass surgery?
A stent is a small, mesh-like device inserted into a blocked artery. It keeps the artery open. Bypass surgery creates a detour around the blocked artery using a graft. Both treat coronary artery disease but have different risks and benefits.
What are the risks of angioplasty and stent placement?
The risks include bleeding, infection, and damage to the coronary arteries. There’s also a risk of restenosis, or re-narrowing of the artery. This might need more procedures.
What is coronary artery bypass graft (CABG) surgery?
CABG surgery creates a detour around a blocked artery using a graft. The graft is usually taken from another part of the body. It’s used for complex or severe coronary artery disease.
How do doctors determine the best treatment option for coronary artery disease?
Doctors look at several factors. They consider the blockage’s severity and location, the patient’s age and health, and other medical conditions.
What are the benefits of minimally invasive cardiac surgery?
Minimally invasive cardiac surgery, like robotic-assisted procedures and off-pump bypass surgery, offers benefits. These include smaller incisions, less pain, and faster recovery times.
What is Enhanced External Counterpulsation (EECP) therapy?
EECP therapy is a non-invasive treatment. It uses external counterpulsation to improve blood flow to the heart. It’s used to treat angina and other symptoms of coronary artery disease.
What is the role of medical therapy in managing coronary artery disease?
Medical therapy, including medication and lifestyle changes, is key in managing coronary artery disease. It helps control symptoms, slow disease progression, and reduce complications.
What are the factors that patients should consider when making decisions about their care?
Patients should consider their diagnosis, treatment options, and personal preferences. They should ask questions to their cardiologist and consider getting a second opinion.
What is the recovery process like after angioplasty and stent placement?
The recovery after angioplasty and stent placement involves a short hospital stay and several weeks of rest at home. Patients may need to take medications to prevent blood clots and manage symptoms.
What is the recovery process like after CABG surgery?
The recovery after CABG surgery involves a longer hospital stay and several months of recovery at home. Patients may need to take medications to manage symptoms and prevent complications.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/22872053/



































