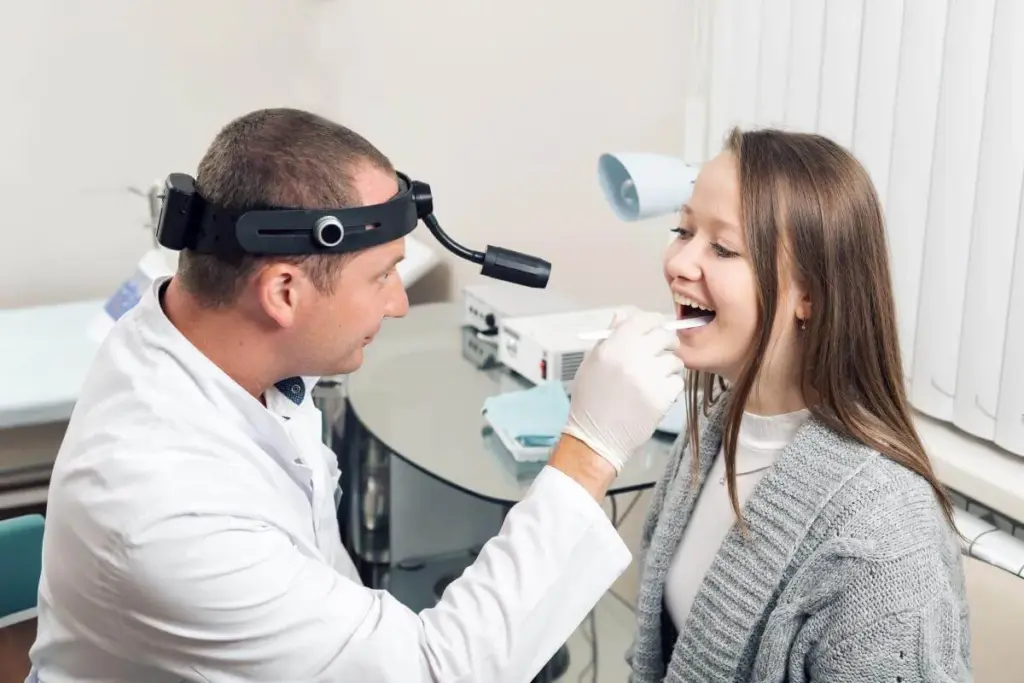
Stroboscopy is a test used to look at the voice box. It helps find problems like laryngitis. To get good results and avoid issues, it’s important to prepare well and follow safety steps.
We aim to give top-notch care, following the best practices worldwide. Our services are designed to treat patients with the best care possible. Knowing what precautions are taken during stroboscopy can make patients feel more at ease.
When doing stroboscopy, checking the patient and the equipment is key to avoid problems. Our team works hard to give the best care. We use high-quality services to make sure patients get the best results.
Key Takeaways
- Patient preparation is key for a good stroboscopy test.
- Checking the equipment is important to avoid complications.
- Stroboscopy helps find issues like laryngitis.
- We focus on innovative and complete care for our patients.
- We follow international best practices for the best patient care.
Understanding Stroboscopy in Medical Diagnostics
In medical diagnostics, stroboscopy is key for checking how the larynx vibrates when we speak. It uses a stroboscope to see the vocal cords’ movement. This is vital for spotting and treating voice problems.
Definition and Purpose of Stroboscopic Examination
Stroboscopic examination is a test that uses a stroboscope to look at how the larynx works during speech. It helps doctors see how the vocal cords vibrate. This is important for finding and fixing voice issues.
According to the, stroboscopy is a key tool for checking laryngeal function and finding problems.
Doctors use a stroboscope to see how the vocal cords move. This helps them understand how we make sound and spot any issues.
Common Applications in Voice and Laryngeal Assessment
Stroboscopy is used a lot in checking voice and laryngeal problems. It helps with patients who have voice issues like hoarseness. It also checks if voice therapy is working.
It’s also used to find and diagnose laryngeal issues like nodules and polyps. This helps doctors plan the best treatment.
Knowing how stroboscopy works helps doctors give better diagnoses and treatments for voice and laryngeal problems.
How Stroboscopes Function in Clinical Settings
Stroboscopic examination uses flashing light to study vocal fold vibrations. It helps doctors see the vocal folds clearly. This is key for diagnosing and treating voice problems.
Basic Principles of Stroboscopic Light
Stroboscopes work by shining a flashing light on the vocal folds. This light is set to match the vibration of the vocal folds. It makes the movement seem slow, allowing for a close look at how the vocal folds move.
By using stroboscopic light, we can see the mucosal wave and other small movements of the vocal folds. These movements are important for checking vocal health. The light flashes at a rate that makes the vocal fold vibration seem slow.
—Laryngologist
Types of Medical Stroboscopes Used Today
There are many types of medical stroboscopes, each with its own features and uses. Some work with rigid laryngoscopes, while others fit with flexible nasolaryngoscopes.
|
Type of Stroboscope |
Key Features |
Clinical Applications |
|---|---|---|
|
Rigid Stroboscope |
High-resolution imaging, synchronized strobe light |
Detailed examination of vocal folds during phonation |
|
Flexible Stroboscope |
Compatible with flexible nasolaryngoscopes, portable |
Examination of patients with sensitive gag reflex or anatomical limitations |
|
Digital Stroboscope |
Advanced image processing, video recording capabilities |
Enhanced diagnostic accuracy, patient education, and documentation |
When picking a stroboscope for medical use, think about image quality, how easy it is to use, and if it works with your equipment. If you’re looking to buy a stroboscope, look at what’s available for sale. Compare their features and benefits.
Pre-Procedure Patient Assessment
Before starting stroboscopy, a detailed patient check is key for safety and success. This step helps doctors spot risks and prepare, improving patient results.
Comprehensive Medical History Evaluation
Looking at a patient’s medical history is vital. We collect info on past surgeries, allergies, and health issues. This helps us predict possible problems and plan how to avoid them.
We also check the patient’s current health and symptoms. Knowing their condition lets us adjust the procedure to fit their needs. This makes the stroboscopy safe and effective.
Identifying High-Risk Patients
Spotting patients at high risk is important too. We look for those with conditions like bleeding disorders or severe lung disease. By finding these risks, we can take steps ahead to reduce them. This might mean changing our approach or having more medical staff on hand.
We also look at the patient’s overall health and how they might react to the procedure. This includes checking their anxiety levels and making sure they’re comfortable and willing to cooperate during the stroboscopy.
Patient Preparation Protocols
Thorough preparation by patients is essential for maximizing the effectiveness of stroboscopy. Good preparation makes the images clearer and keeps the patient safe and comfortable.
Physical Preparation Requirements
Before stroboscopy, patients should be ready. This means avoiding hard activities that might hurt the vocal cords. They should also not smoke and stay away from things that irritate the throat or nose.
Good oral hygiene is also key. It helps prevent infections and makes the exam better.
Dietary and Medication Restrictions Before Stroboscopy
What you eat and take before stroboscopy matters a lot. Patients often need to fast before the test to avoid choking. How long to fast depends on the patient’s health and the test type.
It’s important to tell your doctor about all medications you’re taking. Some drugs, like blood thinners, might need to be stopped before the test to avoid bleeding.
- Tell your doctor about any allergies or sensitivities to stroboscopy materials.
- Reviewing all medications is key to avoid bad reactions or problems.
Following these steps helps make the stroboscopy safe and useful. It gives doctors important information about your health.
Managing Patient Anxiety and Comfort
To make the stroboscopy experience better, we must manage patient anxiety. Patients might worry about the procedure. It’s our job to make sure they’re comfortable and know what’s happening.
Psychological Preparation Techniques
Reducing patient anxiety starts with good psychological preparation. We use several methods to help patients relax:
- Clear Communication: We explain the procedure in detail. This includes what to expect and the benefits of stroboscopy. It helps clear up fears and misconceptions.
- Empathetic Understanding: We listen to patients’ concerns and show empathy. This can greatly lower their anxiety.
- Pre-procedure Education: Giving patients educational materials or videos about stroboscopy prepares them mentally.
A study in a leading medical journal found that good patient education and communication are key. They help reduce anxiety about medical procedures.
“Patients who are well-informed about their procedure tend to have lower levels of anxiety and a more positive experience overall.”
– Journal of Medical Patient Care
Sedation Options and Considerations
In some cases, sedation is needed to keep patients comfortable during stroboscopy. We look at several factors when choosing sedation:
|
Sedation Option |
Benefits |
Considerations |
|---|---|---|
|
Mild Sedation |
Relaxes the patient without impairing their ability to respond |
Requires careful monitoring of the patient’s vital signs |
|
Moderate Sedation |
Deeper relaxation, may impair some responses |
Needs more intensive monitoring and may require additional staff |
When thinking about sedation, we must weigh its benefits against risks. It’s important to talk about these options with the patient.
Understanding stroboscopic movement and using stroboscope diagrams helps us explain the procedure. This makes patients more comfortable and less anxious.
Equipment Safety Checks for Stroboscope Devices
To get accurate results, stroboscope devices need thorough safety checks. We stress the need for careful equipment safety checks. This ensures stroboscopes work safely and well in medical settings.
Pre-Procedure Equipment Inspection
Before starting, a detailed check of the stroboscope is key. We look at the light, camera, and other important parts for damage or issues. It’s important to make sure everything is clean and connected right for the best performance.
Key inspection points include:
- Inspecting the light source for intensity and color consistency
- Checking the camera for clear image quality and proper focus
- Verifying the integrity of all cables and connections
Calibration and Testing Protocols
Calibration is vital for accurate stroboscope use. We follow set protocols to adjust the device as needed. Regular tests against known standards confirm its performance.
Calibration involves:
- Adjusting the stroboscope’s frequency to match the vocal cord vibrations
- Ensuring the device’s synchronization with other diagnostic equipment
- Verifying the accuracy of the device’s measurements
|
Calibration Parameter |
Description |
Acceptable Range |
|---|---|---|
|
Frequency |
Stroboscope flash frequency |
0-1000 Hz |
|
Intensity |
Light source intensity |
0-100% |
|
Synchronization |
Sync with other diagnostic tools |
<1 ms delay |
Maintenance Requirements for Optimal Performance
Regular upkeep is key for stroboscope devices to work well. We follow a maintenance plan with cleaning, software updates, and hardware checks. This keeps the devices running smoothly and accurately.
Maintenance tasks include:
- Regular cleaning of the device and its components
- Updating software to the latest version
- Performing routine checks on hardware components
By focusing on safety checks, calibration, and maintenance, we ensure our stroboscope devices perform at their best. This supports reliable patient care.
Infection Control and Sterilization Measures
Infection control and sterilization are key in stroboscopy. As medical tech advances, keeping things clean is more important than ever. This includes using digital stroboscope and handheld stroboscope devices.
Keeping infections at bay involves several steps. These include cleaning equipment, wearing protective gear, and stopping germs from spreading. Let’s look at each of these important steps.
Sterilization of Laryngoscope Components
Laryngoscope parts must be sterilized to stop infections. The process includes:
- Breaking down the laryngoscope into parts
- Cleaning with special cleaners to get rid of dirt
- Using methods like autoclaving or ethylene oxide to sterilize
It’s vital that everyone knows how to properly clean and sterilize the equipment. This makes sure it’s safe for use.
Personal Protective Equipment Requirements
Wearing PPE is a big part of stopping infections. During stroboscopy exams, doctors and nurses should wear:
|
PPE Component |
Purpose |
|---|---|
|
Gloves |
Keep skin from touching possibly infected things |
|
Masks |
Help stop airborne germs from spreading |
|
Gowns |
Keep clothes from getting dirty |
|
Eye Protection |
Protect eyes from splashes or sprays |
The CDC says, “PPE is a key part of keeping patients safe. It’s needed for all patients.”
“The use of PPE is an essential component of standard precautions and is required for the care of all patients.” – Centers for Disease Control and Prevention (CDC)
Cross-Contamination Prevention Strategies
Stopping cross-contamination is critical when using high-speed strobe devices. Ways to do this include:
- Using disposable parts when possible
- Having strict cleaning rules for non-disposable items
- Making sure staff follow hand hygiene rules
By following these steps, we can lower the chance of infections during stroboscopy. This makes a safer place for patients and healthcare workers.
Nasal Passage Examination Safety Protocols
Nasal stroboscopy needs a deep understanding of the nasal passage anatomy. This ensures patient safety and comfort. We must avoid causing trauma or discomfort by knowing the delicate structures inside the nasal cavity.
Anatomical Considerations for Nasal Stroboscopy
The nasal passages are complex and have many structures important for breathing and smell. Knowing the anatomy of the nasal turbinates, nasal septum, and the olfactory region is key to safely navigating these areas during stroboscopy.
- The nasal turbinates are long, thin, curved bones in the nasal cavity. They can block airflow if swollen or enlarged.
- The nasal septum, which divides the two nasal cavities, can be off-center. This might make the stroboscopy procedure harder.
- The olfactory region, in the upper nasal cavity, is very sensitive. It needs careful handling to avoid damage.
Techniques to Minimize Trauma and Discomfort
To reduce trauma and discomfort during nasal stroboscopy, we use several methods. Topical anesthesia and decongestants are used to lessen pain and congestion, making the procedure easier for the patient.
- Topical anesthesia is applied to numb the area.
- Decongestants are used to lessen nasal congestion.
- The stroboscope is inserted and moved gently to avoid mucosal trauma.
Managing Nasal Passage Complications
Even with careful planning, complications can happen during nasal stroboscopy. Being ready to handle these complications is vital for patient safety. Common issues include nasal bleeding, vasovagal reactions, and nasal trauma.
|
Complication |
Management Strategy |
|---|---|
|
Nasal Bleeding |
Apply topical vasoconstrictors or use nasal packing to control bleeding. |
|
Vasovagal Reactions |
Monitor patient vital signs and be prepared to administer atropine if necessary. |
|
Nasal Trauma |
Use gentle technique and consider using a smaller stroboscope if necessary. |
By understanding the anatomy, using techniques to reduce trauma and discomfort, and being ready for complications, we can make nasal stroboscopy safe and effective. This approach not only makes the patient more comfortable but also improves the procedure’s results.
Oral Airway Examination Precautions
Using a stroboscope machine for oral airway exams needs careful attention. Oral stroboscopy is a great tool for diagnosis. But, it’s important to focus on patient positioning, managing gag reflex, and protecting the airway for safety.
Proper Positioning for Oral Stroboscopy
Getting the patient’s position right is key for a good oral stroboscopy exam. We make sure they’re comfortable, either sitting or lying down, based on the exam’s needs. Their head and neck are aligned for a clear view of the airway.
This positioning enhances the quality of the examination and minimizes discomfort for the patient.
Gag Reflex Management Techniques
Controlling the gag reflex is vital in oral stroboscopy. We use methods like topical anesthetics and careful stroboscope handling to reduce gagging. This helps patients tolerate the exam better and get a precise look at their airway.
Managing the gag reflex well is essential for a successful exam.
Airway Protection During the Procedure
Keeping the airway safe during oral stroboscopy is a top priority. We watch the patient’s breathing closely and have emergency gear ready. The strobe light lets us examine closely without stressing the patient too much.
By focusing on airway safety, we ensure a safe and useful exam.
In summary, oral airway exams with stroboscopy need careful attention. This includes the right patient position, managing gag reflex, and airway protection. By following these steps, we can use the stroboscope machine effectively. This improves diagnosis and care for patients. For those thinking of getting a stroboscope, knowing these precautions is vital for safe use.
Preventing and Managing Bleeding Complications
It’s key to manage bleeding when using stroboscopic technology. Bleeding can happen for many reasons during or after the procedure. Healthcare providers must be ready for it.
Risk Factors for Mucosal Bleeding
There are several reasons why mucosal bleeding might happen during stroboscopy. These include:
- Pre-existing mucosal lesions or inflammation
- Use of anticoagulant medications
- Poor patient preparation or cooperation
- Technical issues with the stroboscope equipment
Knowing these risk factors helps us prevent bleeding complications.
Immediate Interventions for Bleeding Events
If bleeding happens during stroboscopy, we must act fast. Our plan is to:
- Stop the procedure and check the bleeding site
- Use topical hemostatic agents if needed
- Keep a close eye on the patient’s vital signs
Handling bleeding well needs a team effort and the right tools.
Post-Procedure Bleeding Management
After the stroboscopic exam, we watch for bleeding signs. Our care plan includes:
|
Care Component |
Description |
|---|---|
|
Vital Sign Monitoring |
Watching blood pressure, heart rate, and oxygen levels closely |
|
Patient Education |
Telling patients about bleeding signs and when to get help |
|
Follow-up Care |
Setting up follow-up visits to check for complications |
By sticking to these steps, we make sure patients get the best care. This helps lower the chance of bleeding problems from stroboscopy.
Respiratory Monitoring During Stroboscopy
Monitoring a patient’s breathing is key during stroboscopy. We make sure to watch their breathing closely. This keeps them safe and comfortable during the test.
Oxygen Saturation Assessment
Checking oxygen levels is very important. We use pulse oximetry to keep an eye on these levels. This helps us catch any problems early.
Continuous monitoring lets us act fast if something changes. This helps avoid serious issues.
Emergency Protocols for Respiratory Distress
We have plans ready for emergencies. These include giving extra oxygen and using special airway tools when needed.
“The key to managing respiratory distress is preparedness and swift action.” – Expert in Respiratory Care
Our plans help us act quickly in emergencies. This keeps the patient safe.
Equipment for Respiratory Support
Having the right tools is essential. We have oxygen tanks, ventilators, and more. These help support the patient’s breathing.
- Oxygen tanks and delivery systems
- Ventilators and respiratory support devices
- Advanced airway management equipment
Being ready with the right tools helps us support the patient’s breathing. This ensures the best results for them.
Special Precautions for Pediatric Stroboscopy
Pediatric patients have unique needs for stroboscopic exams. Stroboscopy helps see how vocal cords work in slow motion. But, it must be adapted for kids to be safe and useful.
Age-Specific Considerations and Modifications
When doing stroboscopy on kids, their age matters a lot. Young ones might need smaller equipment. The setup also needs to fit their smaller bodies and possibly less cooperation. Using the right size laryngoscopes and having different sizes ready is key.
For babies and toddlers, the exam might be done with them lying down. This might need extra help from staff to keep the child calm. Older kids can be treated like adults, but we must watch their comfort and stress.
Parental Involvement and Support
Parents play a big role in pediatric stroboscopy. Their presence can help the child feel less scared. We suggest parents explain the exam in a way the child can understand.
Parents can also help by calming their child, holding them, or just being there. Talking clearly with parents about what to expect helps a lot.
Pediatric Sedation Safety Measures
Sometimes, kids might need sedation for stroboscopy. But, we must think carefully about this. We need to consider the benefits and risks, like breathing problems.
Safe sedation for kids means choosing the right patient, watching them closely, and being ready for emergencies. The sedative must match the child’s size, age, and health history. Keeping an eye on their vital signs, like oxygen levels, is very important.
By being careful, we can make pediatric stroboscopy safe and useful. This helps us find the best treatments for kids.
Post-Procedure Monitoring and Care
The post-procedure phase is key in stroboscopy. It affects how well a patient recovers and the final results. After a stroboscopy exam, patients need careful watching and care to stay safe and comfortable.
Recovery Room Observation Protocols
After a stroboscopy procedure, patients go to a recovery room. There, they are watched closely for any bad reactions or problems. We follow strict recovery room observation protocols to make sure patients get the right care during this important time.
We keep an eye on vital signs like heart rate and oxygen levels. Our team is ready to act fast if the patient’s condition changes. This ensures we can help them quickly if needed.
|
Monitoring Parameter |
Normal Range |
Action for Abnormal Reading |
|---|---|---|
|
Heart Rate |
60-100 bpm |
Notify physician if outside range |
|
Oxygen Saturation |
95-100% |
Administer supplemental oxygen if below 95% |
|
Blood Pressure |
90-120/60-80 mmHg |
Monitor closely; notify physician if outside range |
Discharge Instructions for Patients
Before leaving, we give patients clear discharge instructions. These help them recover smoothly at home. The instructions cover things like:
- Going back to normal activities and eating habits
- Handling side effects like throat pain or mild bleeding
- Knowing when to seek urgent medical help
- When to come back for follow-up visits and who to contact for questions
We stress the importance of following these instructions. This helps avoid complications and ensures a good recovery.
Follow-up Care Recommendations
Follow-up care is vital after stroboscopy. We suggest follow-up visits to check on the patient’s recovery and address any ongoing issues.
At these visits, we check how the patient is doing and offer more advice on managing symptoms. We also talk about any further treatment plans. Our aim is to give patients the best care throughout their recovery.
By sticking to these guidelines, we can help our patients get the best results from their stroboscopy procedures.
Training Requirements for Medical Professionals Performing Stroboscopy
Stroboscopy is a complex procedure that needs thorough training for medical professionals. It’s key for achieving the best results. As we move forward in medical diagnostics, the need for proper stroboscopy training grows. We think that detailed training is essential for making sure healthcare workers can give top-notch care.
Certification and Continuing Education
Certification programs in stroboscopy teach medical professionals about the procedure and its uses. It’s important to keep learning about new stroboscopic technology, like high-speed strobe devices. This ongoing education helps keep skills sharp and patient care at its best.
Hands-on Training Protocols
Hands-on training is vital for stroboscopy skills. It lets professionals practice with tools, like handheld stroboscope devices. We suggest training programs include lots of practice. This hands-on experience is key for mastering the technique and dealing with different clinical situations.
Competency Assessment Standards
To make sure medical professionals are skilled in stroboscopy, we need strict assessment standards. These standards should check both technical skills and the ability to read results correctly, even with complex tools like an industrial stroboscope. By setting high standards, we ensure patients get the best care.
Institutional Best Practices and Safety Protocols
Healthcare institutions must follow strict best practices and safety protocols for stroboscopy. This includes sticking to international standards, ensuring quality, and keeping detailed records. These steps help reduce risks and improve patient care.
International Standards and Guidelines
We follow international standards and guidelines for stroboscopy in medical diagnostics. These rules are key to keeping our practices safe and effective. They help us protect patients and improve our diagnostic tools.
- Guidelines from professional medical organizations
- International Organization for Standardization (ISO) standards
- Regulatory requirements from health authorities
By sticking to these guidelines, we make sure our stroboscopy meets high standards. This ensures better care for our patients.
Quality Assurance Measures
Quality assurance is vital in our stroboscopy program. We take steps to keep our equipment in top shape and our staff well-trained.
- Regular calibration and maintenance of stroboscope machines
- Ongoing training and competency assessment for healthcare professionals
- Continuous quality improvement initiatives
These efforts help us maintain top-notch care. They ensure our stroboscopy services are safe and effective.
Documentation and Reporting Requirements
Keeping accurate records is key for stroboscopy procedures. We make sure all important information is documented as required.
- Patient history and pre-procedure assessment
- Details of the stroboscopy procedure, including any complications
- Post-procedure care instructions and follow-up plans
Our documentation supports ongoing care and helps with quality improvement. It also ensures we meet regulatory standards.
Conclusion: Ensuring Safe and Effective Stroboscopy Procedures
Stroboscopy is a key tool in medical diagnosis. It needs careful preparation, safe equipment, and awareness of possible issues. By following the steps in this article, doctors can make sure stroboscopy is done right. This helps them give the best care to their patients.
To get the most from stroboscopy, it’s vital to stick to the rules. This includes following the and state rules. This means training well, getting patient consent, and using lidocaine when needed.
This way, we can make sure stroboscopy is done with great care. It leads to better health outcomes for patients. As we keep improving in medical diagnostics, the need for safe stroboscopy is more important than ever.
FAQ
What is stroboscopy and how is it used in medical diagnostics?
Stroboscopy is a way to check voice and laryngeal disorders. It shows the vocal folds in detail when someone is speaking. Doctors use it to find and treat many laryngeal problems.
What are the benefits of using stroboscopy in voice and laryngeal assessment?
Stroboscopy gives a clear view of the vocal folds. This helps doctors diagnose and treat laryngeal issues better. It’s great for checking voice problems and laryngeal diseases.
What precautions should be taken during stroboscopy to minimize complications?
To avoid problems, doctors do a full check on the patient first. They also make sure the equipment is safe. It’s important to prepare the patient well, both physically and mentally.
How is patient anxiety and comfort managed during stroboscopy?
Doctors use special techniques to calm the patient. They might use sedation or make sure the patient is comfortable during the test.
What are the infection control and sterilization measures for stroboscopy?
To keep things safe, doctors sterilize the laryngoscope and wear protective gear. They also follow steps to prevent germs from spreading. This keeps the clinic clean and safe.
How is bleeding managed during and after stroboscopy?
If there’s bleeding, doctors act fast. They might use special creams or medicines. After the test, they keep an eye on the patient to make sure everything heals well.
What are the special considerations for pediatric stroboscopy?
When it comes to kids, doctors need to think about their age and how to make them comfortable. They also have to be careful with sedation to keep the kids safe.
What training is required for medical professionals performing stroboscopy?
Doctors need a lot of training to do stroboscopy right. This includes getting certified, staying up-to-date with new methods, and practicing. They also need to show they can do the job well.
What are the institutional best practices for stroboscopy?
Clinics should follow international rules and check their quality often. They also need to keep good records and follow reporting rules. This helps them provide the best care.
What is the role of stroboscopic light in clinical settings?
Stroboscopic light helps doctors see the vocal folds clearly. This lets them check for voice and laryngeal problems more easily.
How is respiratory monitoring performed during stroboscopy?
Doctors watch the patient’s breathing closely during stroboscopy. They check oxygen levels and have plans for emergencies. They also have equipment ready to help with breathing if needed.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK567774/[7


































