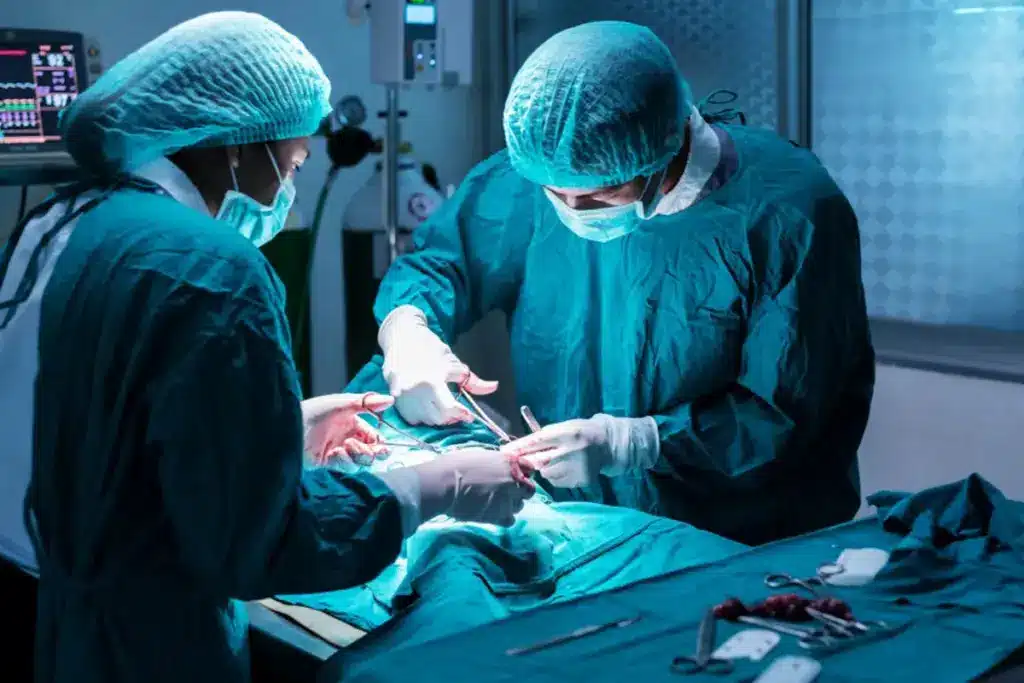
Understanding the roles of different specialists in cancer treatment is key. We often hear about surgical oncologists, but their role can be unclear. Surgical oncologists are skilled surgeons who focus on cancer surgery.
They mainly remove tumors through surgery. But, their skills also help in managing cancer with other doctors. This includes working with medical oncologists who give chemotherapy. The big question is, can a surgical oncologist also give chemotherapy, or are they only in the operating room?
Key Takeaways
- Surgical oncologists are specialized surgeons trained in cancer surgery and the multidisciplinary management of cancer.
- Their primary role involves performing operations to remove tumors.
- Surgical oncologists work closely with other specialists, including medical oncologists.
- Chemotherapy administration is typically the role of medical oncologists.
- Surgical oncologists may be involved in decisions regarding chemotherapy, but their primary focus is on surgical interventions.
Understanding the Role of a Surgical Oncologist
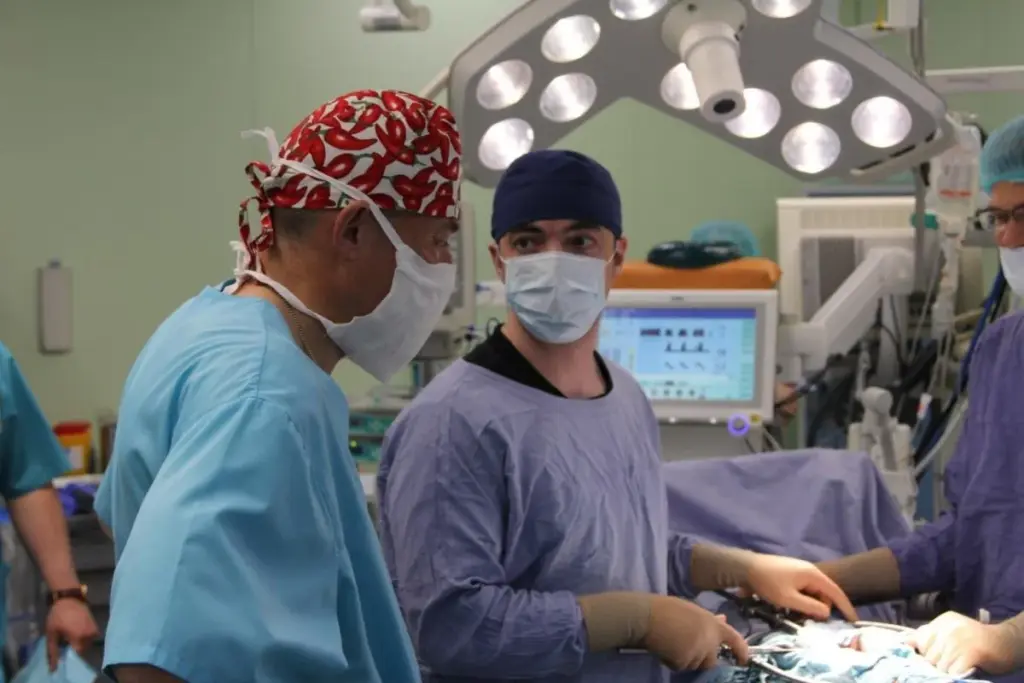
Surgical oncologists are key players in cancer care. They combine surgery skills with deep cancer knowledge. Their work goes beyond surgery, covering all aspects of cancer treatment.
Definition and Specialization
A surgical oncologist is a surgeon with extra training in cancer surgery. They know how to do tumor removal surgery and care for cancer patients well.
“Surgical oncologists understand cancer biology and surgery’s role in treatment,” showing their vital role in cancer teams.
Training and Certification Requirements
To be a surgical oncologist, one needs a general surgery residency and then a fellowship in surgical oncology. Getting certified by the Society of Surgical Oncology proves their skills.
The long training and certification make sure they know the latest oncologic surgery methods. This ensures they can give top-notch care.
Core Responsibilities in Cancer Treatment
Surgical oncologists check patients to find the best surgery for their cancer. They do surgeries and work with other doctors to treat patients fully.
They also keep up with new oncology surgical procedures. They join tumor boards to plan patient care and treatment.
The Distinction Between Surgical and Medical Oncology
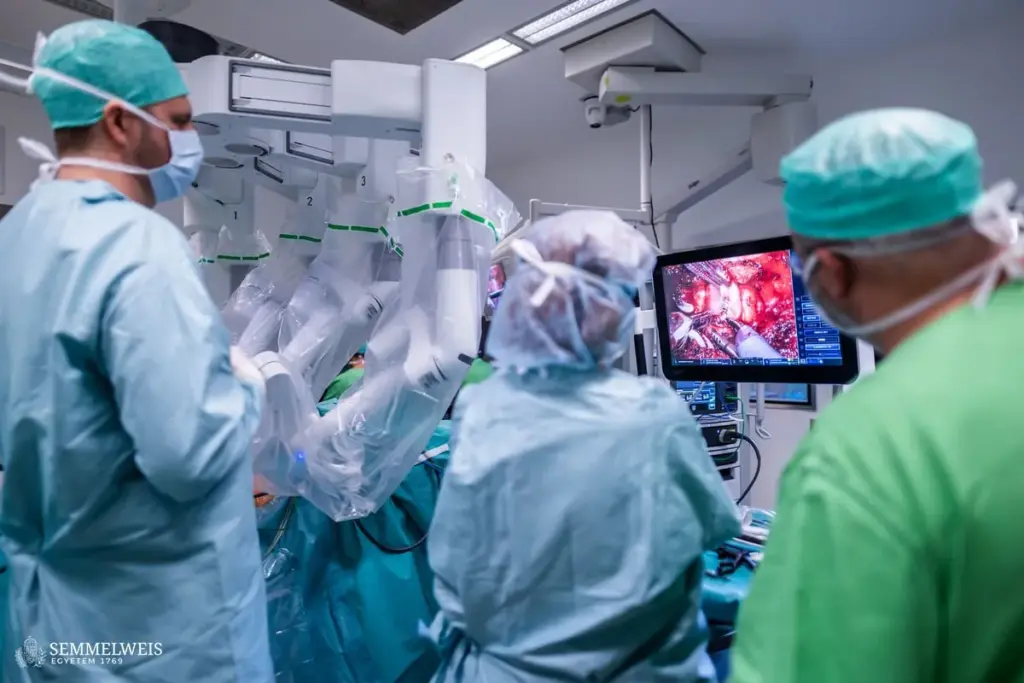
Surgical and medical oncology are two important fields in cancer treatment. They work together but have different ways of treating cancer. Their training and methods are unique.
Medical Oncology: Focus and Training
Medical oncologists use non-surgical methods to fight cancer. They use chemotherapy, targeted therapy, and immunotherapy. They focus on treating the whole body.
They get a lot of training. After finishing internal medicine, they do a fellowship in medical oncology. This helps them handle complex cancer cases.
Surgical Oncology: Focus and Training
Surgical oncologists remove tumors through surgery. They learn about the surgical techniques needed for cancer treatment. They work with other doctors for complete care.
They start with a general surgery residency. Then, they do a fellowship in surgical oncology. This prepares them for cancer surgery.
Overlapping Knowledge but Different Practices
Medical and surgical oncologists share some knowledge. But, they have different main focuses. Medical oncologists treat the whole body, while surgical oncologists focus on removing tumors.
|
Specialist |
Primary Focus |
Common Treatments |
|---|---|---|
|
Medical Oncologist |
Systemic cancer treatment |
Chemotherapy, targeted therapy, immunotherapy |
|
Surgical Oncologist |
Surgical removal of tumors |
Surgery, pre-operative and post-operative care |
Medical oncologists usually give chemotherapy. But, working together is key for full cancer care.
Who Typically Administers Chemotherapy?
Chemotherapy is a key part of cancer treatment. It’s given by many healthcare experts. It’s used to fight different cancers.
Medical Oncologists as Primary Administrators
Medical oncologists lead in giving chemotherapy. They have specialized training in using these drugs. They know how to handle cancer treatment well.
- They check the patient’s health and pick the best treatment.
- They watch how the patient is doing and change the treatment if needed.
- They help with side effects and make the patient’s life better.
Specialized Oncology Nurses
Oncology nurses are also key in giving chemotherapy. They know how to deal with chemotherapy’s challenges. They work with medical oncologists to give top-notch care.
- They give chemotherapy with a doctor’s watch.
- They teach patients about their treatment and possible side effects.
- They offer emotional support and answer patient questions.
Required Certifications for Chemotherapy Administration
Certifications are vital for those giving chemotherapy. They show that professionals know how to care for patients safely and well. Certified oncology nurses and doctors go through tough training and meet strict standards.
Why Surgical Oncologists Don’t Typically Give Chemotherapy
<SEP-7194_image_4>
Surgical oncologists are specialized surgeons who focus on the surgical aspects of cancer treatment, not on chemotherapy administration. Their expertise lies in the surgical removal of tumors and affected tissues, which is a critical component of cancer care.
Specialization and Scope of Practice
The scope of practice for surgical oncologists is defined by their training and expertise in surgical oncology. Surgical oncologists are trained to perform operations that aim to remove cancerous tissues while preserving as much normal tissue and function as possible. Their role is critical in the local control of cancer and is often used in conjunction with other treatments like chemotherapy and radiation therapy.
Administering chemotherapy, on the other hand, falls under the scope of practice of medical oncologists, who are trained to use systemic therapies to treat cancer. This distinction is based on the different skill sets and knowledge bases required for surgical versus medical treatments.
Training Differences
The training pathways for surgical and medical oncologists differ significantly. Surgical oncologists undergo extensive training in surgical techniques and the management of surgical complications. Their education and training focus on the surgical management of cancer, including pre-operative and post-operative care.
In contrast, medical oncologists are trained in the use of systemic therapies, including chemotherapy, hormone therapy, and immunotherapy. Their expertise lies in understanding the complex biology of cancer and the application of non-surgical treatments.
Legal and Liability Considerations
There are also legal and liability considerations that influence the administration of chemotherapy by surgical oncologists. Administering chemotherapy requires specific training and certification, and doing so without proper qualifications could lead to liability issues. Medical oncologists are specially trained and certified for this purpose.
Further, hospitals and cancer centers have protocols in place that dictate who can administer certain treatments based on their scope of practice and credentials. This ensures that patients receive the highest standard of care and minimizes the risk of adverse events.
In conclusion, while surgical oncologists play a vital role in cancer treatment, their specialization and training are focused on surgical interventions. The administration of chemotherapy is typically the responsibility of medical oncologists, with whom surgical oncologists collaborate as part of a multidisciplinary team to provide complete cancer care.
The Multidisciplinary Approach to Cancer Treatment
<SEP-7194_image_5>
Effective cancer treatment often needs a team effort. Many medical specialties come together to give complete care. This team approach is key to tackling cancer’s complexity and bettering patient results.
Tumor Boards and Treatment Planning
Tumor boards are a big part of cancer care. They are teams of experts from different fields who work together to plan treatments. Tumor boards include specialists in surgery, medicine, radiation, pathology, and radiology to talk about patient cases and make a detailed treatment plan.
This teamwork makes sure every part of a patient’s health is looked at. This leads to better treatment plans.
Coordination Between Specialists
It’s important for specialists to work well together in cancer treatment. Good communication among team members helps avoid mistakes and makes sure everyone is on the same page.
Regular meetings and new communication tools help with this teamwork. They make sure patient care is smooth and effective.
Patient Benefits of Integrated Care
Patients gain a lot from integrated cancer care. A team approach has been shown to increase survival rates and improve quality of life for cancer patients.
With a team of specialists, patients get care that meets their specific needs. This care goes from diagnosis to treatment and follow-up.
In conclusion, the team effort in cancer treatment is a big step forward. It offers patients a detailed and coordinated care plan that leads to better results.
Surgical Oncology Procedures and Expertise
Surgical oncology is a key part of cancer care. It uses advanced surgical techniques to remove cancerous tissues. Surgical oncologists are trained for complex surgeries, from open surgeries to minimally invasive ones.
Types of Cancer Surgeries
Surgical oncologists perform various cancer surgeries. These include:
- Tumor resections: Removing the tumor and some healthy tissue around it.
- Lymph node dissections: Taking out lymph nodes to check for cancer spread.
- Reconstructive surgeries: Fixing the affected area after tumor removal.
Minimally Invasive Techniques
Minimally invasive surgery has changed cancer treatment. It cuts down recovery time and scarring. Techniques like laparoscopic and robotic surgeries remove tumors with less damage.
Post-Surgical Care and Recovery
Post-surgical care is vital for recovery. It includes managing pain, watching for complications, and supporting nutrition. Surgical oncologists work with other healthcare teams for complete care.
Good post-surgical care can greatly improve patient outcomes. It lowers the risk of complications and boosts quality of life.
How Surgical Oncologists Understand Chemotherapy
<SEP-7194_image_6>
Understanding chemotherapy is key for better cancer treatment. As healthcare professionals, we see how surgery and chemotherapy work together. This teamwork is vital for good cancer care.
Knowledge of Treatment Protocols
Surgical oncologists need to know about chemotherapy protocols. They must understand the different types of chemotherapy. This includes neoadjuvant and adjuvant therapies for various cancers.
In breast cancer, neoadjuvant chemotherapy makes tumors smaller before surgery. This makes surgery easier. So, knowing these protocols is important for planning surgery.
Awareness of Side Effects and Complications
It’s also important for surgical oncologists to know about side effects and complications of chemotherapy. These can range from nausea and fatigue to serious issues like neutropenia and thrombocytopenia.
|
Side Effect |
Complication |
Management Strategy |
|---|---|---|
|
Nausea |
Dehydration |
Antiemetic medication, hydration |
|
Neutropenia |
Infection |
Granulocyte-colony stimulating factor (G-CSF), antibiotics |
|
Fatigue |
Reduced quality of life |
Rest, physical therapy, nutritional support |
Neoadjuvant and Adjuvant Therapies: Improving Survival Rates
Neoadjuvant and adjuvant therapies have changed cancer treatment a lot. They include chemotherapy, hormone therapy, and radiation therapy. These treatments are used at different times to work best.
Pre-Surgical (Neoadjuvant) Chemotherapy Benefits
Neoadjuvant chemotherapy is given before surgery. It makes the tumor smaller. This makes surgery easier and can lead to better results.
Post-Surgical (Adjuvant) Chemotherapy Outcomes
Adjuvant chemotherapy is given after surgery. It kills any cancer cells left behind. This lowers the chance of cancer coming back and boosts survival chances.
It works well for cancers like breast, colon, and lung cancer.
- Reduces the risk of cancer recurrence
- Improves long-term survival rates
- Effective in treating various types of cancer
Statistical Improvements in Patient Survival
Many studies prove neoadjuvant and adjuvant therapies improve survival. For example, they show neoadjuvant chemotherapy can greatly increase survival in gastric cancer patients. These therapies are now a key part of cancer treatment plans.
|
Therapy Type |
Cancer Type |
Survival Rate Improvement |
|---|---|---|
|
Neoadjuvant Chemotherapy |
Gastric Cancer |
25% |
|
Adjuvant Chemotherapy |
Breast Cancer |
30% |
Case Studies: Successful Integrated Cancer Treatment
World-renowned cancer centers stress the value of integrated care in fighting cancer. We’ll look at several case studies. They show how combining treatments can lead to better outcomes for different cancers.
Gastric Cancer Treatment Protocols
Gastric cancer treatment has made big strides with the mix of surgery, chemotherapy, and radiation. A study in a top oncology journal found that adding chemotherapy before surgery boosted survival rates for advanced gastric cancer patients.
The treatment plan included FLOT chemotherapy (docetaxel, oxaliplatin, leucovorin, and fluorouracil) and surgery. It showed a big jump in survival rates compared to surgery alone.
|
Treatment Protocol |
Survival Rate Improvement |
|---|---|
|
Neoadjuvant FLOT Chemotherapy + Surgery |
30% increase in 5-year survival rate |
|
Surgery Alone |
Baseline |
Breast Cancer Multimodal Approaches
Breast cancer treatment has also seen big improvements with integrated care. A mix of surgery, chemotherapy, and targeted therapy has led to better results for HER2-positive breast cancer patients.
A case study from a top cancer center showed the power of combining neoadjuvant chemotherapy with targeted therapy (trastuzumab and pertuzumab) and surgery. This method greatly reduced tumor size and improved looks.
Colorectal Cancer Management
Colorectal cancer treatment has grown with the blend of surgery, medical oncology, and radiation oncology. A team effort has shown to better patient results.
A study on colorectal cancer treatment found that mixing surgical resection, adjuvant chemotherapy, and radiation therapy improved control and survival for stage III colorectal cancer patients.
International Standards in Comprehensive Cancer Centers
Globally, comprehensive cancer centers meet high standards. These standards ensure patients get top-notch care. They make sure treatment is complete and well-coordinated.
Multidisciplinary Team Requirements
Comprehensive cancer care needs a multidisciplinary team. This team includes surgical, medical, and radiation oncologists. They also have support staff.
This team works together to create personalized treatment plans. Having a team is not just good; it’s required for these centers. Effective communication among team members is key for smooth care.
Accreditation Standards
Accreditation for comprehensive cancer centers is strict. It ensures care quality. The Commission on Cancer gives accreditation based on these standards.
To get accredited, centers must show they follow care, treatment, and follow-up standards. They go through regular checks and keep improving.
Best Practices in Comprehensive Cancer Care
Best practices in cancer care go beyond just treating the disease. They focus on the patient’s overall well-being. This includes psychosocial support, nutrition advice, and rehab services.
By following these practices, centers can better patient outcomes. They can also improve the quality of life for cancer survivors.
Navigating Cancer Treatment: The Patient Perspective
Knowing who does what in cancer treatment can really help a patient. It’s key to understand your treatment team and how each specialist helps. This knowledge can make a big difference in your care and results.
Understanding Your Treatment Team
Your treatment team includes many specialists, each with their own role. You’ll work with surgical oncologists, medical oncologists, radiation oncologists, and oncology nurses. Knowing their roles helps you understand your treatment better.
A surgical oncologist removes tumors, while a medical oncologist handles chemotherapy. Knowing this can make you feel more in charge of your care.
Questions to Ask About Who Administers Your Treatment
Being proactive means asking the right questions. Here are some important ones:
- Who will be my main contact during treatment?
- What does each specialist on my team do?
- How will my treatment plan be coordinated?
- What are my treatment team’s qualifications and experience?
These questions help you understand your treatment and ensure you get the best care.
Coordinating Care Between Multiple Specialists
It’s vital to coordinate care among specialists for effective treatment. Tumor boards are a way to do this. As a patient, you can help by:
|
Coordination Method |
Description |
Benefit |
|---|---|---|
|
Keeping a Personal Health Record |
Maintain a record of your treatments, test results, and appointments. |
Ensures all specialists have access to your complete medical history. |
|
Using a Care Coordinator |
Many cancer centers offer care coordinators to help manage your care. |
Helps navigate the healthcare system and schedule appointments. |
|
Regular Communication |
Ensure that all members of your treatment team are informed about your progress. |
Enhances the overall quality of care by ensuring everyone is on the same page. |
By understanding your treatment team, asking the right questions, and coordinating care, you can navigate your cancer treatment with confidence.
Exceptions to Standard Practice: When Roles May Overlap
While there are set roles for oncologists, there are exceptions. Cancer treatment’s complexity often calls for teamwork among healthcare pros.
Rural and Underserved Healthcare Settings
In rural and underserved areas, finding specialized oncologists can be tough. Surgical oncologists might give chemotherapy, even though it’s not their usual job.
“In some rural settings, surgical oncologists may be required to provide chemotherapy due to the lack of medical oncologists.”
This isn’t the best situation, but it’s needed. It ensures patients get care without long travel times.
Integrated Practice Models
Some places, like cancer centers, use a team approach. Here, surgical and medical oncologists work closely together. Their roles start to blend.
|
Model |
Description |
Benefits |
|---|---|---|
|
Multidisciplinary Clinics |
Various specialists see patients together |
Comprehensive care, improved coordination |
|
Shared Decision-Making |
Specialists collaborate on treatment plans |
Enhanced patient outcomes, better resource utilization |
International Variations in Oncology Practice
Oncology practices differ worldwide. In some places, surgical oncologists are trained to give chemotherapy. This is not the norm everywhere.
It’s key to know these differences. This helps in giving care that meets local standards and patient needs.
The Future of Collaborative Cancer Care
The future of cancer care will rely more on teamwork. Different medical specialties will come together. This is because cancer treatment is complex and needs many experts.
Emerging Integrated Treatment Models
Integrated treatment models are leading the way in cancer care. A team of doctors, including surgeons and oncologists, work together. They create treatment plans that fit each patient’s needs.
These models offer many benefits. They improve communication, make treatment plans more personal, and coordinate care better. This leads to better patient outcomes.
Experts say, “Integrated care models have shown promise in improving patient outcomes and quality of life.”
Technology Facilitating Specialist Coordination
Technology is key in helping specialists work together. Electronic health records (EHRs) and telemedicine platforms let doctors share information easily. This is true even if they are far apart.
Technology in cancer care has many benefits. It makes data sharing better, improves communication, and lets patients get involved through patient portals.
Training Programs for Comprehensivie Cancer Care
To support collaborative cancer care, we need training programs. These programs should teach healthcare professionals about teamwork and communication. They should focus on delivering top-notch patient care.
Conclusion
Cancer care needs a team effort from many experts, including surgical oncologists. They focus mainly on surgery, not on giving chemotherapy.
Medical oncologists are the ones who usually give chemotherapy. They have special training in cancer treatment and managing side effects. But, surgical oncologists also need to know about chemotherapy to work well together and help patients get better.
Working together, doctors make sure patients get the best care for their cancer. This team effort is key as cancer treatment keeps getting better.
By teaming up, we can help more people live longer and better lives with cancer. Surgical oncologists play a big part in this team effort. Their work is very important for taking care of cancer patients.
FAQ
What is the role of a surgical oncologist in cancer treatment?
Surgical oncologists focus on the surgical side of cancer treatment. They remove tumors and surrounding tissues. They work with a team that includes medical oncologists and other specialists.
Can surgical oncologists administer chemotherapy?
No, surgical oncologists usually don’t give chemotherapy. Their main job is surgery. But, they know a lot about different cancer treatments, including chemotherapy.
Who typically administers chemotherapy?
Medical oncologists are the ones who give chemotherapy. They are experts in treating cancer with medicine. They work with surgical oncologists and others to plan treatment.
What is the difference between a surgical oncologist and a medical oncologist?
Surgical oncologists do surgeries to remove tumors. Medical oncologists use medicine, like chemotherapy, to manage cancer. Both are key in cancer treatment.
Why don’t surgical oncologists typically give chemotherapy?
Surgical oncologists focus on surgery, not chemotherapy. Their training and legal rules keep them from giving chemotherapy.
What is the importance of a multidisciplinary approach in cancer treatment?
A team approach, with specialists like surgical and medical oncologists, is vital. It ensures patients get the best care, leading to better outcomes and survival rates.
What types of cancer surgeries do surgical oncologists perform?
Surgical oncologists do many surgeries, like removing tumors. They use new techniques when they can. They handle complex surgeries for various cancers.
How do surgical oncologists understand chemotherapy?
Surgical oncologists know a lot about chemotherapy. They understand how to time surgery with chemotherapy and manage side effects. This helps them work well with medical oncologists.
What are neoadjuvant and adjuvant therapies?
Neoadjuvant therapy is given before surgery to shrink tumors. Adjuvant therapy is after surgery to kill any remaining cancer cells. Both can improve survival rates.
How can patients navigate cancer treatment effectively?
Patients should know their treatment team and ask questions. They should also make sure their care is well-coordinated among specialists.
Are there exceptions to the standard practice of who administers chemotherapy?
Yes, in some places, like rural areas or certain international settings, roles can overlap. Surgical oncologists might give chemotherapy or other treatments.
What is the future of collaborative cancer care?
The future of cancer care will be more integrated, thanks to technology and training. This will help ensure patients get the best care possible.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from

































