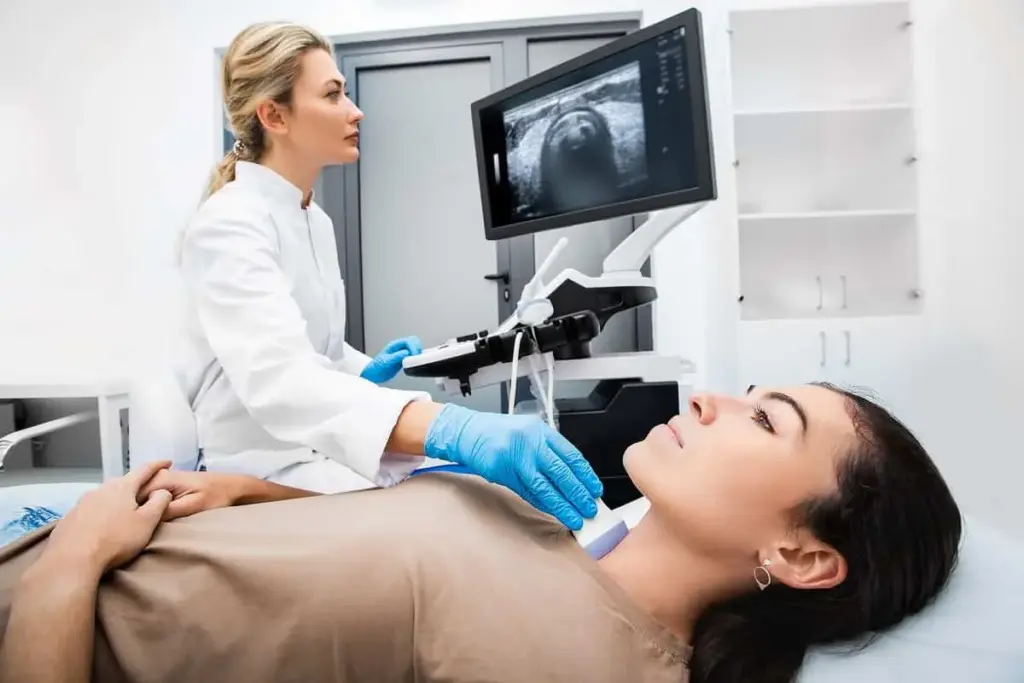
Planning for thyroid surgery can be daunting, but being informed is key to a successful outcome. Understanding the risks and complications is vital for making informed decisions about your care.
Research shows that comes with significant risks. These include a morbidity rate of 7% and a mortality rate of 3.4%. It’s important to discuss these risks with your healthcare provider and understand how to minimize them.
By asking the right questions, patients can understand their surgical options and what to expect during recovery. Clear communication with the surgical team is essential for a safe and successful thyroid removal surgery.
Key Takeaways
- Understand the risks associated with thyroidectomy, including morbidity and mortality rates.
- Discuss surgical options and possible complications with your healthcare provider.
- Learn about the measures to minimize risks during thyroid cancer surgery.
- Clarify what to expect during recovery and post-operative care.
- Ensure your surgical team is experienced in performing thyroidectomy surgery.
Understanding Thyroid Disorders and When Surgery Is Necessary
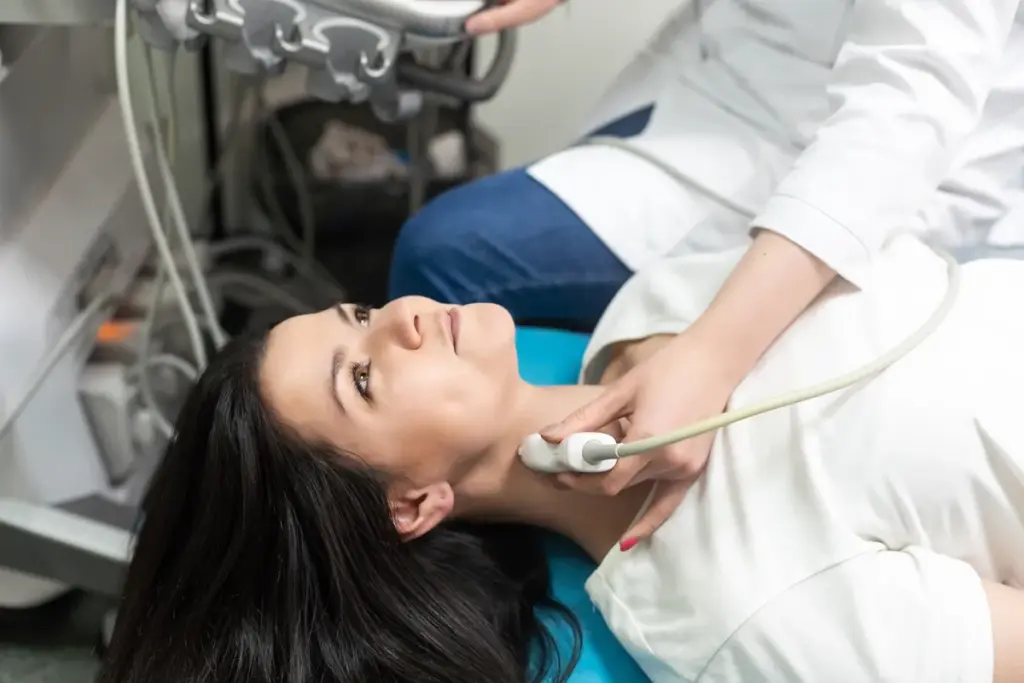
Thyroid disorders range from small nodules to serious cancers. Knowing about them helps decide if surgery is needed. The thyroid gland controls metabolism, affecting our health and well-being.
Common Thyroid Conditions That May Require Surgical Intervention
Some thyroid issues need surgery. Thyroid cancer is a big concern, affecting many people. Other problems include large goiters, uncontrolled hyperthyroidism, and unclear nodules.
It’s key to know your thyroid condition well. We’ll talk about how tests help figure out what’s going on.
Diagnostic Tests Used to Determine Surgical Necessity
Tests help decide if surgery is needed. These include:
- Ultrasound: Checks the thyroid gland for nodules or issues.
- Fine-needle aspiration biopsy: Finds out if nodules are cancerous.
- Blood tests: Looks at thyroid function and hormone levels.
- CT or MRI scans: Sees how far the disease has spread.
Non-Surgical Alternatives to Consider
For some thyroid issues, surgery isn’t the only option. Other choices include:
- Radioactive iodine therapy: Treats hyperthyroidism or some cancers.
- Thyroid hormone suppression therapy: Manages nodules or goiter.
- Medications: Helps with symptoms of thyroid problems.
Talking to your doctor is important. They can help choose the best treatment for you.
Types of Thyroid Surgery Procedures to Discuss with Your Doctor

Talking about thyroid surgery options with your doctor is key. The right surgery depends on your thyroid issue, nodule or tumor size, and your health.
Total Thyroidectomy vs. Thyroid Gland Removal
A total thyroidectomy means removing the whole thyroid gland. It’s often chosen for thyroid cancer, big goiters, or uncontrolled hyperthyroidism. Total thyroidectomy removes the gland, reducing cancer risk.
Thyroid gland removal can mean taking out part or all of the gland. The exact surgery depends on your health and the surgeon’s advice.
Partial Thyroidectomy and Thyroid Lobectomy Options
Partial thyroidectomy removes just the affected part, keeping some function. It’s for diseases in one area. Thyroid lobectomy removes one lobe for nodules or tumors in that area.
These options are less invasive than total removal. They’re good for benign nodules or early cancer. The choice depends on your condition and health.
Thyroid Nodule and Tumor Removal Approaches
Removing nodules or tumors depends on their size, location, and type. For benign nodules, a thyroid lobectomy might be enough. But for cancer, a total thyroidectomy is often needed.
Doctors use fine-needle aspiration biopsy to decide on surgery. Sometimes, intraoperative frozen section analysis is done during surgery to check for cancer, guiding the surgery.
Advanced Thyroid Surgery Techniques and Technologies
New techniques in thyroid surgery are changing the game. They aim to make surgery less invasive, speed up recovery, and improve accuracy. We’ll look at the good and bad of these new methods, helping patients understand their choices.
Minimally Invasive Thyroid Surgery Benefits
Minimally invasive thyroid surgery is a big step forward. It uses smaller incisions to reduce scarring and pain. This method also means patients can get back to their lives faster.
A study showed that this surgery leads to less pain and shorter hospital stays. It’s a great option for many patients.
|
Benefits |
Traditional Surgery |
Minimally Invasive Surgery |
|---|---|---|
|
Incision Size |
Larger |
Smaller |
|
Recovery Time |
Longer |
Shorter |
|
Post-operative Pain |
More |
Less |
Endoscopic Thyroid Surgery Procedures
Endoscopic thyroid surgery uses a small camera and tools through tiny cuts. It’s great for those worried about scars. This method lets surgeons remove thyroid tissue carefully, without harming nearby areas.
The surgery is done under general anesthesia, keeping patients comfortable. The camera technology helps surgeons see better, making the surgery easier.
Robotic Thyroid Surgery Advantages and Limitations
Robotic thyroid surgery is the latest in technology. It offers enhanced precision and improved visualization with a high-definition camera. It’s perfect for complex surgeries.
But, it has its downsides. It needs special training, and not all surgeons are skilled in it. Also, the equipment is expensive, making it hard for some to access.
Despite these challenges, robotic surgery is a big plus for the right patients. Choosing this method should be a team decision with a qualified surgeon, considering each patient’s needs.
Selecting a Qualified Thyroid Surgery Specialist
Finding a skilled thyroid surgeon is key to avoiding risks and getting the best results. Your surgeon’s experience greatly affects your surgery’s success and your overall experience.
Essential Qualifications and Certifications
A good thyroid surgeon has important qualifications and certifications. Being board certified in otolaryngology (ENT) or endocrine surgery shows they’ve had thorough training. It also means they meet high standards in their field.
Also, look for surgeons who join professional thyroid surgery groups. This shows they keep up with new techniques and research.
Questions to Ask About Surgeon Experience and Volume
When talking to thyroid surgeons, ask about their experience and how many surgeries they do. Find out how many thyroid surgeries they perform each year. Also, ask about their experience with cases like yours.
A study on shows that a surgeon’s volume matters for better results. This info helps you understand their skill level and make a better choice.
Researching Surgeon-Specific Outcomes and Complication Rates
It’s important to look into your surgeon’s past results and complication rates. This info might not always be easy to find, but it’s worth asking. Some hospitals share this data as part of their quality programs.
Knowing these details helps you choose a surgeon who can meet your needs and offer top care.
Critical Questions About Thyroid Surgery Risks and Complications
Thinking about thyroid surgery? It’s key to know the risks and complications. Thyroidectomy, like any surgery, has risks that can affect how well you do.
Understanding Morbidity and Mortality Rates
Thyroidectomy has a morbidity rate of 7% and a mortality rate of 3.4%. These numbers are important for patients to know. Morbidity is the rate of complications, and mortality is the rate of death from the surgery. We’ll dive deeper into these numbers to help you understand better.
|
Complication Type |
Rate (%) |
Description |
|---|---|---|
|
Morbidity Rate |
7% |
Rate of complications arising from thyroid surgery |
|
Mortality Rate |
3.4% |
Rate of death associated with thyroid surgery |
Improving Safety Outcomes with Surgical Checklists
Surgical checklists are vital for safer surgeries. They help teams avoid mistakes. These checklists make sure all important steps are taken and nothing is missed.
Some key parts of surgical checklists include:
- Checking the patient’s identity and the surgery site
- Looking over the patient’s medical history and allergies
- Confirming all needed equipment and supplies
Personal Risk Factors That May Increase Complication Rates
Some personal factors can raise the risk of problems during and after thyroid surgery. These include:
- Age: Older patients might face more risks
- Pre-existing medical conditions: Conditions like diabetes or heart disease can affect surgery results
- Smoking status: Smoking can slow healing and increase risks
It’s important for patients to talk to their surgeon about their personal risks. This helps understand how these might affect their surgery.
Discussing Possible Voice Changes and Nerve Damage
When thinking about thyroid surgery, it’s important to talk about nerve damage and voice changes. Thyroid surgery is good for treating thyroid issues but is risky because it’s near important neck nerves. These nerves help us speak.
One big risk is hurting the recurrent laryngeal nerve. This can cause voice problems. Knowing the risks is key for making smart choices.
Recurrent Laryngeal Nerve Injury Statistics
About 5% of people get temporary nerve damage from thyroid surgery. This can make your voice sound hoarse or breathy. The chance of this happening depends on the surgery type and the surgeon’s skill.
|
Type of Thyroid Surgery |
Temporary Nerve Injury Rate |
Permanent Nerve Injury Rate |
|---|---|---|
|
Total Thyroidectomy |
5% |
1-2% |
|
Partial Thyroidectomy |
3% |
0.5-1% |
Voice Assessment Before and After Thyroidectomy
Checking your voice before and after surgery is very important. A good voice check can spot problems early and help fix them. This check includes talking about your voice, a physical exam, and sometimes looking at your vocal cords.
Treatment Options for Voice Complications
If your voice changes after surgery, there are ways to help. You might see a speech therapist, get vocal cord injections, or need surgery. These options can improve your voice.
Talking about voice and nerve risks with your surgeon is vital before surgery. Being informed helps you understand what might happen. This way, you can prepare for your surgery’s outcomes.
Questions About Calcium Levels and Parathyroid Function
Thyroid surgery can affect more than just the thyroid gland. It’s important to think about its impact on calcium levels and parathyroid function. The parathyroid glands, near the thyroid, help control calcium in the body. During surgery, they might get damaged or removed, causing calcium problems.
Understanding Hypoparathyroidism Risk
Thyroid surgery can lead to hypoparathyroidism. This is when the parathyroid glands don’t make enough hormone, causing low calcium levels. Up to 10% of patients might face this issue temporarily after surgery. In some cases, it can last forever.
Key statistics on hypoparathyroidism risk include:
- Temporary hypoparathyroidism: up to 10% of patients after thyroidectomy
- Permanent hypoparathyroidism: 1-3% of patients
Symptoms of Post-Thyroidectomy Calcium Deficiency
After thyroid surgery, calcium deficiency can cause various symptoms. It’s important for patients to know these signs to get help quickly. Common symptoms include:
- Numbness or tingling in the fingers, toes, or around the mouth
- Muscle cramps or spasms
- Fatigue or weakness
If you notice any of these symptoms, reach out to your healthcare provider right away. They can help evaluate and manage your condition.
Long-term Management of Parathyroid Issues
Managing parathyroid issues after thyroidectomy requires a detailed plan. For those with hypoparathyroidism, treatment usually includes calcium and vitamin D supplements. Regular check-ups with an endocrinologist are key to keep calcium levels right and adjust treatment as needed.
“The goal of managing hypoparathyroidism is to maintain serum calcium levels within a normal range, alleviate symptoms, and prevent long-term complications.”
Following your treatment plan and attending regular check-ups is vital. This ensures the best care for patients with parathyroid issues after thyroid surgery.
Preparing for Thyroid Surgery: Pre-operative Considerations
Before thyroid surgery, it’s key to know what to do to get ready. This includes several important steps that can affect your surgery and recovery. We’ll help you understand what you need to do to prepare for a successful surgery.
Medication Adjustments Before Thyroid Excision Surgery
Adjusting your medications is a big part of getting ready for surgery. Some medicines can make surgery harder or slow healing. It is crucial to discuss your medications with your physician. They might tell you to stop taking certain ones or adjust others.
For example, if you take blood thinners, you might need to stop them a few days before. This is to lower the risk of bleeding during surgery. Thyroid medicines might also need to be changed to keep your hormone levels stable.
Fasting and Other Pre-operative Instructions
Fasting is another key thing to do before surgery. Most people need to fast for at least 8 hours before surgery. This is to avoid problems with anesthesia. Your healthcare team will tell you exactly how long to fast.
There are other things you might need to avoid before surgery. Your doctor might tell you not to eat certain foods or drinks. They might also ask you to shower with a special soap to lower infection risk.
|
Pre-operative Instruction |
Purpose |
|---|---|
|
Fasting |
Prevent complications related to anesthesia |
|
Medication Adjustment |
Minimize risks during and after surgery |
|
Special Soap Shower |
Reduce the risk of infection |
What to Bring to the Hospital for Your Thyroid Operation
On surgery day, bring things that make you comfortable and help your recovery. Bring comfy clothes, insurance cards, ID, and any needed papers. You might also want to bring your medicines, a charger, and something to read.
Having someone with you at the hospital is a good idea. They can help with instructions and care after surgery.
Anesthesia Considerations for Thyroid Surgery
Thyroid surgery needs careful thought about anesthesia to keep patients comfortable and safe. Anesthesia is key in thyroid surgery. Knowing about the types of anesthesia, talking about risks, and understanding recovery can ease worries and make the surgery go smoothly.
Types of Anesthesia
Several anesthesia types are used in thyroid surgery. General anesthesia is the most common, making patients sleep through the surgery. Local anesthesia with sedation is used less often but might be an option for some patients.
Discussing Risks
Talking about anesthesia risks with your doctor is very important. Though rare, risks include allergic reactions, breathing problems, and bad reactions to anesthesia. Your doctor will look at your health and past to pick the safest anesthesia for you.
Recovery from Anesthesia
Recovery from anesthesia happens in a special unit where doctors watch your health and manage any pain or side effects. Pain management is a big part of recovery. Your healthcare team will try to keep you as comfortable as possible.
|
Anesthesia Type |
Description |
Risks |
|---|---|---|
|
General Anesthesia |
Patient is completely asleep during the procedure |
Respiratory complications, allergic reactions |
|
Local Anesthesia with Sedation |
Patient is sedated and has local numbing |
Less risk of respiratory complications, but possible for not enough sedation |
Understanding anesthesia types and talking about risks with your doctor can prepare you for thyroid surgery. A smooth recovery also depends on the anesthesia choice.
Hospital Stay and Immediate Post-operative Care
Understanding what to expect after thyroid surgery is key to a smooth recovery. We’re here to guide you through this important time. We want to make sure you get the best care and support.
Expected Length of Hospitalization After Thyroidectomy
The time you spend in the hospital after surgery can change based on several things. These include how complex the surgery was and your health. Usually, most people stay for 1-2 days after surgery.
A study on thyroid surgery risk management shows the need for careful monitoring after surgery. This is done during your hospital stay .
|
Factor |
Typical Hospital Stay |
Extended Stay Criteria |
|---|---|---|
|
Simple Thyroidectomy |
1 day |
Complications or comorbidity |
|
Complex Thyroidectomy |
2 days |
Significant comorbidity or complications |
Pain Management After Thyroid Gland Surgery
Managing pain well is very important after surgery. We use different methods to help you feel less pain and recover better.
Some ways we manage pain include:
- Giving you pain medicines when you need them
- Using cold compresses to help with swelling
- Helping you find comfortable positions
Initial Wound Care and Drainage Management
Good wound care is key to avoiding infection and helping your wound heal. Our team will teach you how to take care of your surgical site. This includes how to change dressings and watch for infection signs.
In some cases, a drain is used to remove extra fluid. We’ll show you how to handle the drain and watch its output.
Recovery Timeline After Thyroid Surgery
Knowing the recovery timeline after thyroid surgery helps manage expectations and reduces anxiety. Each person’s recovery is unique, based on the surgery’s extent and their health.
First Week After Thyroid Removal Surgery
The first week is key for healing. You might feel pain, swelling, and discomfort in your neck. Effective pain management is very important. Follow your healthcare team’s post-operative instructions, which may include pain relief medication and wound care guidelines.
It’s common to have trouble swallowing or feel like something is stuck in your throat in the first week. These symptoms usually go away in a few days to a week. Resting your voice and avoiding hard activities can help.
Returning to Normal Activities Following Thyroidectomy
Most people can start getting back to normal in 1-2 weeks after surgery. But, it’s important to listen to your body and not rush. Light activities like walking are good, but avoid heavy lifting, bending, or hard exercises for a few weeks.
- Resume driving when you feel comfortable and safe to do so, usually within a few days to a week.
- Gradually increase your activity level based on your energy levels and comfort.
- Avoid heavy lifting or bending for at least 2-3 weeks post-surgery.
Long-term Recovery Expectations and Thyroid Removal Side Effects
Long-term recovery includes healing of the scar and adjusting to thyroid hormone level changes. Most people see big improvements, but some may face long-term side effects like voice changes or needing lifelong thyroid hormone therapy.
|
Recovery Stage |
Timeline |
Expectations |
|---|---|---|
|
Immediate Recovery |
1-2 weeks |
Pain, swelling, difficulty swallowing |
|
Returning to Normal |
1-2 weeks |
Gradual increase in activities |
|
Long-term Healing |
Several months |
Scar healing, adjustment to thyroid hormone levels |
Understanding the recovery timeline after thyroid surgery is key to managing recovery. Knowing what to expect in the first week, when to start normal activities, and long-term recovery helps patients navigate their care better.
Thyroid Hormone Replacement After Thyroidectomy
After removing the thyroid gland, a detailed plan for hormone replacement is needed. This is because the body can’t make thyroid hormones anymore, leading to hypothyroidism. A good thyroid hormone replacement therapy plan is key to managing this condition.
Who Needs Hormone Replacement After Surgery
Those who have their thyroid gland completely removed need hormone replacement for life. This is because the body can’t make thyroid hormones anymore. Even if only part of the gland is removed, hormone replacement might be needed if the remaining tissue is not enough.
Starting lifelong medication can seem overwhelming. But with the right care and monitoring, patients can live normal lives. It’s important to work with your healthcare provider to find the best treatment for you.
Finding the Right Dosage and Medication Options
There are different types of thyroid hormone replacement medication, with levothyroxine being the most common. The right dosage depends on several factors, including age, weight, and other health conditions. Finding the right dosage involves regular blood tests to check hormone levels.
Being patient and working closely with your healthcare provider is key. The goal is to get hormone levels back to normal, easing symptoms and improving your quality of life.
|
Medication Type |
Common Brand Names |
Key Characteristics |
|---|---|---|
|
Levothyroxine (T4) |
Synthroid, Levoxyl, Unithroid |
Most commonly prescribed; mimics natural thyroid hormone production |
|
Liothyronine (T3) |
Cytomel |
Used less frequently; can be used in conjunction with T4 for some patients |
|
Natural Desiccated Thyroid (NDT) |
Armour Thyroid, Nature-Throid |
Derived from animal thyroid glands; contains both T4 and T3 |
Monitoring Thyroid Levels Long-term After Thyroid Gland Removal
It’s important to regularly check thyroid hormone levels after thyroidectomy. This means taking blood tests to check TSH, free T4, and sometimes free T3 levels. These tests help adjust the medication dosage to keep hormone levels in the normal range.
Long-term care is vital to manage any side effects of hormone replacement therapy. It also helps make any needed changes to the treatment plan. By keeping thyroid hormone levels right, patients can reduce symptoms and enjoy a better life.
Scar Management and Cosmetic Outcomes
Many patients worry about how their thyroid surgery scars will look. New surgical methods have made these scars less noticeable. This is a big part of taking care of you after surgery.
Typical Incision Placement and Size for Thyroid Surgery
Doctors usually make the incision in a neck crease to hide it better. The size of the cut depends on the surgery type and your body. Minimally invasive techniques often mean smaller cuts, which can make scars less visible.
Scar Minimization Techniques and Treatments
There are many ways to make scars less noticeable after thyroid surgery. These include:
- Using fine sutures or staples to close the incision
- Applying topical creams or gels to promote healing
- Silicone scar sheets or gel to flatten and soften the scar
- Laser treatments to reduce the appearance of the scar
Our surgeons help you choose the best way to manage your scar.
“The key to effective scar management is a combination of proper wound care and follow-up treatments. By working together with our patients, we can achieve the best possible cosmetic outcomes.”
Timeline for Scar Healing and Fading After Thyroidectomy
How long it takes for scars to heal can differ for everyone. At first, the scar will be red and raised for a few weeks. Then, it will start to flatten and fade over months. It’s essential to be patient and follow post-operative instructions to ensure optimal healing.
Knowing about incision placement, using scar treatments, and understanding healing times can help you get the best results from thyroid surgery.
Conclusion: Making an Informed Decision About Thyroid Surgery
Understanding thyroid surgery is key to making a good choice. It involves knowing the procedure’s risks and benefits, as well as other treatment options. Talking to your doctor about your concerns helps you make a decision that fits your needs.
Being well-informed about thyroid surgery options helps patients navigate their treatment. Knowing the risks, benefits, and alternatives lets them choose what’s best for their health and goals.
Grasping the complexities of thyroid surgery and its outcomes helps patients make confident decisions. This approach ensures the best results and supports a smooth recovery.
FAQ
What are the possible risks and complications of thyroid surgery?
Thyroid surgery, like any surgery, has risks. These include damage to the nerve that controls your voice, low calcium levels, and reactions to anesthesia. It’s important to talk about these risks with your doctor.
How do I know if I need thyroid surgery?
Your doctor will check your thyroid condition with tests like ultrasound and blood tests. They will tell you if surgery is needed based on these results.
What types of thyroid surgery are there?
There are several surgeries for the thyroid, like removing the whole gland or just part of it. Your doctor will choose the best one for you based on your condition and health.
What are the benefits of minimally invasive thyroid surgery?
This type of surgery has many benefits. It means smaller cuts, less pain, and a quicker recovery. But, it’s not right for everyone.
How do I choose a qualified thyroid surgery specialist?
Look for a surgeon with the right qualifications and experience. Check their success rates and complication history to make a good choice.
What is the risk of nerve damage during thyroid surgery?
There’s a 5% chance of nerve damage that’s temporary. Your voice will be checked before and after surgery. There are treatments for voice problems.
How will thyroid surgery affect my parathyroid function?
Surgery can affect your parathyroid glands, leading to low calcium levels. Knowing the risks and how to manage them is important.
What pre-operative considerations should I be aware of before thyroid surgery?
Before surgery, you’ll need to adjust your medications and fast. Knowing what to bring to the hospital helps ensure a smooth surgery and recovery.
What type of anesthesia is used for thyroid surgery?
Your doctor will decide on the anesthesia. Knowing the risks and what to expect after surgery helps make the experience better.
What can I expect during the recovery process after thyroid surgery?
Recovery time varies. Knowing what to expect in the first week and when you can return to normal activities helps plan your recovery.
Will I need thyroid hormone replacement therapy after thyroidectomy?
Some patients need hormone replacement after surgery. Understanding who needs it and how to manage it is key for good thyroid health.
How can I minimize scarring after thyroid surgery?
Knowing about incision placement and scar healing can help. Talking to your doctor about these topics can also be helpful.
References:
- Xu T, Zheng X, Wei T. Preoperative preparation for Graves’ disease. Front Endocrinol (Lausanne).2023;14:1234056. doi:10.3389/fendo.2023.1234056.
- Uludag M, et al. Preoperative Preparation in Hyperthyroidism and Surgery in the Hyperthyroid State. Med Bull Sisli Etfal Hosp. 2024;58(3):[page numbers]. doi:10.5578/mbsih-2024-0000. PMCID: PMC11472198.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/25900848/



































