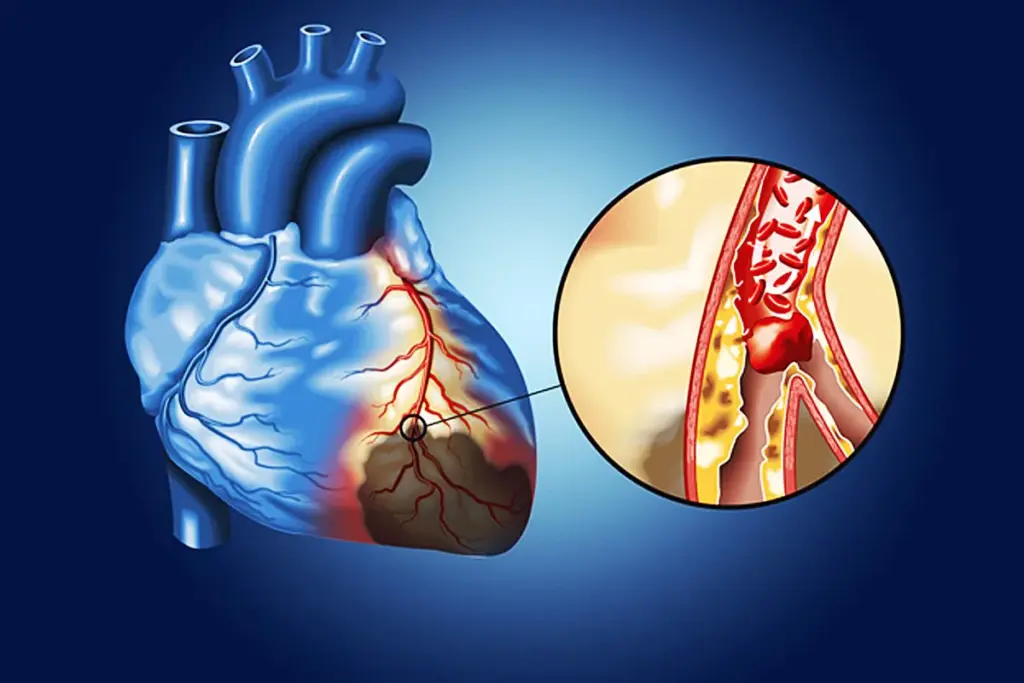
We know how vital it is to tackle cardiac ischemia with care and understanding. This condition, where the heart doesn’t get enough blood, needs quick and effective treatment. This is to stop things from getting worse.
How to treat cardiac ischemia treatment effectively? Discover the best methods and medical therapies to restore blood flow safely right now.
We see that every patient is different. So, our heart ischemia therapy methods are made just for them. We aim to give top-notch healthcare and support, including for patients from abroad looking for the best treatments.
Key Takeaways
- Comprehensive treatment approaches are key for managing cardiac ischemia.
- Effective care means tailoring it to each patient’s needs.
- We’re dedicated to providing world-class healthcare and support.
- Advanced medical treatments are available for international patients.
- Acting fast is essential to prevent further problems.
Understanding Cardiac Ischemia
It’s key to know about cardiac ischemia to help heart health. This condition happens when the heart muscle doesn’t get enough oxygen and nutrients. This is because blood flow is reduced, leading to serious health issues.
Definition and Pathophysiology
Cardiac ischemia is when the heart’s need for oxygen and nutrients doesn’t match what it gets. This can cause changes in the heart muscle. If not treated, it might lead to heart failure or a heart attack.
The reasons behind cardiac ischemia are complex. They involve blood flow, oxygen demand, and heart muscle cells. Knowing these details helps doctors find the best treatments.
Types of Cardiac Ischemia
There are different kinds of cardiac ischemia, each with its own signs and effects:
- Stable Angina: Chest pain or discomfort that comes with effort or stress, goes away with rest or medicine.
- Unstable Angina: Chest pain that happens without effort, often means a serious blockage.
- Silent Ischemia: Heart gets less blood without any symptoms.
- Acute Coronary Syndrome: Includes unstable angina and heart attacks, a medical emergency.
Common Causes and Risk Factors

Atherosclerosis, or plaque buildup in arteries, is the main cause of cardiac ischemia. Other risk factors include:
- Hypertension
- High cholesterol
- Diabetes
- Smoking
- Family history of heart disease
Understanding cardiac ischemia’s definition, types, and causes is vital. It shows why quick and right medical care is key. This includes cardiac ischemia medical treatment and heart ischemia treatment protocols to help patients.
Recognizing the Signs and Symptoms
Knowing the warning signs of cardiac ischemia is key to better treatment. This condition, where the heart gets less blood, shows clear signs that need quick action.
Classic Symptoms of Cardiac Ischemia
The main signs include chest pain or discomfort. This can feel like a squeeze or pressure. It might spread to the arms, back, neck, jaw, or stomach.
Other symptoms are shortness of breath, feeling lightheaded, and being very tired.
It’s important to note that these symptoms can differ in how bad they are and how long they last. Some people might feel only a little discomfort, while others might have very severe pain.
|
Symptom |
Description |
|---|---|
|
Chest Pain |
Squeezing or pressure sensation in the chest |
|
Radiating Pain |
Pain that spreads to the arms, back, neck, jaw, or stomach |
|
Shortness of Breath |
Difficulty breathing or feeling winded |
|
Lightheadedness |
Feeling dizzy or faint |
|
Fatigue |
Unusual tiredness or weakness |
Atypical Presentations
Not everyone shows the usual signs of cardiac ischemia. Women, older adults, and people with diabetes might have different symptoms. These can include nausea, vomiting, stomach pain, or irregular heartbeats.
When to Seek Emergency Care
If you or someone else has symptoms of cardiac ischemia, get emergency help right away. Waiting too long can cause serious problems, like a heart attack.
Call emergency services or go to the nearest emergency room if symptoms get worse or don’t go away.
Diagnostic Approaches for Cardiac Ischemia
To find out if someone has cardiac ischemia, doctors use many methods. These range from first checks to detailed scans.
Initial Assessment and Physical Examination
The first step is a detailed check-up and physical exam. We look at the patient’s past health, searching for things like high blood pressure, diabetes, and smoking. We also listen for heart problems and check for swelling in the legs.
Laboratory Tests and Biomarkers
Lab tests are key in spotting cardiac ischemia. We check for heart damage with tests like troponin and creatine kinase. We also test for cholesterol and blood sugar to see heart risk.
Electrocardiogram (ECG) Findings
An electrocardiogram (ECG) is very important for diagnosing cardiac ischemia. We look for signs like ST-segment changes or Q-waves. These signs tell us how bad and where the heart problem is.
Advanced Imaging Techniques
More detailed scans give us even more info. We might use stress tests, echocardiograms, or cardiac MRI to see how the heart works and where it’s not getting enough blood.
Advanced Imaging Modalities
- Stress Testing: Helps assess cardiac function under stress.
- Echocardiography: Provides information on cardiac structure and function.
- Cardiac MRI: Offers detailed images of the heart, helping identify areas of ischemia or scarring.
By using all these methods, we can accurately find out if someone has cardiac ischemia. Then, we can make a good plan to help them.
Emergency Management of Acute Cardiac Ischemia
When someone shows signs of acute cardiac ischemia, quick action is key. The first steps are critical in saving a life. We need to act fast to keep the heart safe and prevent damage.
First Response and Stabilization
The first thing to do is check if the patient’s airway, breathing, and circulation (ABCs) are okay. Prompt assessment is vital. We watch the patient’s vital signs and give oxygen if needed.
- Check the patient’s ABCs.
- Keep an eye on vital signs.
- Give oxygen if the patient is not getting enough.
Oxygen Therapy and Pain Management
Oxygen is very important for patients with acute cardiac ischemia. Supplemental oxygen helps the heart by giving it more oxygen. We also focus on pain management to reduce stress and heart strain.
Initial Medication Administration
Starting medications is a big step in treating acute cardiac ischemia. Antiplatelet therapy and nitrates are often used. Antiplatelets stop clots, and nitrates help the heart by widening blood vessels.
- Give antiplatelet therapy (like aspirin).
- Use nitrates (like nitroglycerin) for pain and to ease heart work.
- Think about beta-blockers to lower heart oxygen need.
Emergency Department Protocols
In the emergency department, a full check-up is done. This includes lab tests and ECGs. Rapid diagnosis is key to making the right treatment choices. The emergency department has special plans for quick and effective care.
- Do a quick ECG to spot ischemia.
- Run lab tests to check heart markers.
- Call for the cardiac cath lab if needed.
How to Treat Cardiac Ischemia Treatment Effectively
Effective treatment for cardiac ischemia needs a plan made just for you. It’s about knowing your unique situation and working together as a team. Every patient is different, so we tailor our approach to fit your needs.
Individualized Treatment Planning
Starting with a plan that’s all about you is key. We look at your health history, current status, and lifestyle. This helps us create a detailed plan to manage your cardiac ischemia.
Our method includes:
- Checking how severe your cardiac ischemia is
- Looking at any other health issues that might affect treatment
- Considering what you value and prefer
- Creating a plan that works well and improves your life
Risk Stratification Approaches
Knowing your risk level is important for choosing the right treatment. We use different tools and assessments to sort patients by risk. This helps us decide the best course of action for you.
The main parts of risk stratification are:
|
Risk Factor |
Description |
Impact on Treatment |
|---|---|---|
|
Clinical Presentation |
How bad and what kind of symptoms you have |
Tells us how quickly and strongly we need to act |
|
Electrocardiogram (ECG) Findings |
Shows if there’s ischemia or infarction |
Tells us if we need to act fast |
|
Biomarkers and Laboratory Tests |
Signs of heart damage or stress |
Helps us understand how bad your cardiac ischemia is |
Treatment Goals and Timelines
Having clear goals and timelines is key to managing cardiac ischemia. We work with you to set realistic goals and milestones. This makes sure your treatment plan is both reachable and effective.
Our goals usually include:
- Lessening symptoms and improving your life quality
- Slowing down the disease
- Preventing serious heart problems
Multidisciplinary Team Approach
Working together is essential in treating cardiac ischemia. We bring together doctors, nurses, and specialists to give you the best care. This team ensures you get all-around care that fits your needs.
By working together, we make sure you get care that covers all your needs. This team approach lets us adjust your treatment as needed. We keep up with any changes in your condition to ensure the best results.
Pharmacological Treatment Options
Managing cardiac ischemia requires a variety of treatments. Medications are key in this fight. They help improve patient health and life quality.
Antiplatelet Medications
Antiplatelet drugs are vital in treating cardiac ischemia. They stop platelets from clumping, which lowers the risk of blood clots. Aspirin is a common choice, sometimes paired with clopidogrel or prasugrel. This combo greatly improves patient outcomes.
Anticoagulants
Anticoagulants are also essential. They include heparin and warfarin, which stop blood clotting. The right one depends on the patient’s risk and symptoms.
Nitrates and Vasodilators
Nitrates and vasodilators help by boosting oxygen to the heart. Nitroglycerin is a fast-acting nitrate that widens arteries. Vasodilators help control blood pressure and heart load.
Beta-Blockers and Calcium Channel Blockers
Beta-blockers and calcium channel blockers are critical. Beta-blockers, like metoprolol and atenolol, lower heart rate and work less hard. Calcium channel blockers, such as amlodipine and diltiazem, also widen arteries and lower blood pressure.
Knowing how these treatments work helps us create better plans for patients with cardiac ischemia.
Advanced Medication Therapies
Advanced medication therapies are key in treating cardiac ischemia. They help lower the risk of complications and improve life quality. We’ll look at these therapies, their benefits, and possible side effects.
Statins and Lipid-Lowering Agents
Statins are vital in managing cardiac ischemia. They lower cholesterol by blocking a key enzyme. This helps prevent heart attacks by stabilizing plaques. Statins like atorvastatin and rosuvastatin are common. Other drugs like ezetimibe and PCSK9 inhibitors may also be used.
ACE Inhibitors and ARBs
ACE inhibitors and ARBs are important for heart health, mainly for those with high blood pressure or heart failure. ACE inhibitors reduce blood pressure by blocking a harmful substance. ARBs block the action of this substance directly. Both improve outcomes for cardiac ischemia patients.
Ranolazine and Anti-Ischemic Medications
Ranolazine helps the heart work more efficiently. It does this by reducing sodium current in heart cells. This improves heart function, making it useful for chronic angina.
Emerging Pharmacological Approaches
New treatments for cardiac ischemia are being explored. These include anti-inflammatory agents, antioxidants, and drugs targeting atherosclerosis. These are promising but need more research to be confirmed.
Interventional Procedures for Cardiac Ischemia
Interventional cardiology has changed how we treat cardiac ischemia. It offers patients effective ways to ease symptoms and improve health. These methods are less invasive and aim to improve blood flow to the heart.
Percutaneous Coronary Intervention (PCI)
Percutaneous Coronary Intervention (PCI) is a non-surgical method to treat narrowed arteries in cardiac ischemia. A thin, flexible tube called a catheter is inserted into the artery. A guide wire is then used to cross the blockage, and a balloon is inflated to expand the artery. This is called balloon angioplasty.
Stent Placement Techniques
After balloon angioplasty, a stent is often placed to keep the artery open. Stents are small, mesh-like tubes that are deployed at the site of the blockage. There are two main types: bare-metal stents and drug-eluting stents. Drug-eluting stents release medication to prevent the artery from narrowing again.
Balloon Angioplasty
Balloon angioplasty is a key part of PCI. It involves inflating a balloon to widen the artery. This can greatly improve blood flow to the heart muscle.
A leading cardiologist notes, “Balloon angioplasty with stent placement has greatly improved outcomes for patients with cardiac ischemia. It allows for faster recovery and lowers the risk of complications.”
“The introduction of drug-eluting stents has been a game-changer in the treatment of cardiac ischemia, significantly reducing the rate of restenosis compared to bare-metal stents.”
An Interventional Cardiologist
Timing and Selection of Interventional Approaches
The choice of interventional approach for cardiac ischemia depends on several factors. These include the severity of symptoms, the extent of coronary artery disease, and the patient’s overall health. Guidelines suggest PCI for patients with acute coronary syndromes or significant ischemia on non-invasive tests.
We consider many factors when choosing the best procedure for a patient. These include the patient’s medical history, any comorbid conditions, and the specific characteristics of the coronary lesions.
Surgical Treatment Options
Surgery is key in treating cardiac ischemia. It offers many treatment plans based on each patient’s needs. When medicine doesn’t work or the condition is serious, surgery can greatly help.
Coronary Artery Bypass Grafting (CABG)
CABG is a common surgery for cardiac ischemia. It uses grafts to bypass blocked arteries. These grafts often come from the leg or chest.
This surgery boosts blood flow to the heart. It helps reduce symptoms and improves life quality.
The benefits of CABG include:
- Improved survival rates for patients with complex coronary artery disease
- Reduced symptoms of angina
- Enhanced quality of life through improved physical function
Minimally Invasive Cardiac Surgery
Minimally invasive cardiac surgery is a big step forward. It uses smaller cuts than traditional surgery. This leads to less damage and trauma.
Key advantages include:
- Reduced recovery time
- Less postoperative pain
- Lower risk of complications
Hybrid Revascularization Approaches
Hybrid revascularization mixes surgery and percutaneous techniques. It offers a customized treatment plan. This combines the best of both worlds.
It’s great for patients with complex disease. It provides a detailed treatment strategy to improve outcomes.
Patient Selection for Surgical Intervention
Choosing the right patients for surgery is vital. The severity of ischemia, overall health, and comorbidities are key factors. These are carefully looked at.
“The decision to proceed with surgical treatment for cardiac ischemia should be made on a case-by-case basis, taking into account the individual patient’s risk profile and possible benefits.” –
Cardiovascular Specialist
Healthcare providers evaluate these factors to find the best candidates. This helps ensure successful outcomes for patients.
Cardiac Rehabilitation Programs
Cardiac rehabilitation is key in managing heart issues. These programs aim to improve patient outcomes and quality of life after heart events.
Exercise-Based Rehabilitation
Exercise is a main part of cardiac rehab. Supervised exercise training boosts heart health and stamina. It also lessens heart ischemia symptoms. We customize exercises for each patient, making sure they’re safe and effective.
Psychological Support and Counseling
Heart issues can affect a patient’s mind too. Our programs offer psychological support and counseling for anxiety, depression, and stress. This helps with overall well-being and recovery.
Education and Self-Management Training
Learning is a big part of rehab. We teach patients about managing their condition, including diet, meds, and lifestyle changes. Self-management training helps patients take charge of their health.
Measuring Rehabilitation Outcomes
We check how well our programs work by tracking patient progress. We look at physical function, quality of life, and heart risk factors. This helps us improve our programs for better patient care.
Cardiac rehab programs are essential in heart ischemia management strategies and cardiac ischemia treatment approaches. They greatly improve patient care and outcomes.
Lifestyle Modifications for Managing Cardiac Ischemia
Healthy habits are key in treating cardiac ischemia. Making smart choices about what you eat, how much you move, managing stress, and quitting smoking can greatly improve your heart health. These actions can also boost your overall well-being.
Dietary Approaches for Heart Health
Eating a diet full of fruits, veggies, whole grains, and lean proteins is vital. Try to cut down on saturated fats, trans fats, and cholesterol. Eating foods rich in omega-3s, like salmon and walnuts, can lower inflammation. Also, watch your sodium intake and choose low-sodium foods to control blood pressure.
It’s wise to get help from a healthcare provider or a dietitian. They can help create a meal plan that fits your nutritional needs and health goals.
Physical Activity Recommendations
Staying active is key in managing cardiac ischemia. Aim for 150 minutes of moderate-intensity aerobic exercise, or 75 minutes of vigorous-intensity aerobic exercise, or a mix of both, each week. Good choices include brisk walking, cycling, or swimming. Don’t forget to include strength training exercises at least twice a week.
Always talk to a healthcare provider before starting any new exercise. They can help pick the best and safest activities for you based on your health and fitness level.
Stress Management Techniques
Too much stress can worsen cardiac ischemia. Try stress-reducing activities like meditation, yoga, or deep breathing exercises. Hobbies and time with loved ones can also offer emotional support and help manage stress.
We suggest trying different stress management techniques to find what works for you. Make it a regular part of your daily life.
Smoking Cessation Strategies
Quitting smoking is a big step in managing cardiac ischemia. Nicotine replacement therapy, counseling, and support groups can help you quit. It’s also important to avoid triggers that might make you want to smoke.
We offer support and resources to help you quit smoking. We’re here to guide you through the process.
Prevention Strategies and Risk Reduction
To prevent cardiac ischemia, we need to change our lifestyles and get medical help. We must also keep an eye on our health. By knowing the risks and taking action, we can lower the chances of getting cardiac ischemia.
Primary Prevention Approaches
Primary prevention aims to stop cardiac ischemia before it starts. It’s about living healthy, eating right, and staying active. It also means avoiding tobacco and managing stress with meditation or yoga.
Dietary recommendations include eating lots of fruits, veggies, whole grains, and lean meats. We should also cut down on bad fats and cholesterol. Regular physical activity, like walking or swimming, is key for heart health.
Modifying Cardiovascular Risk Factors
It’s important to tackle risk factors like high blood pressure, high cholesterol, diabetes, and obesity. We can do this with lifestyle changes and sometimes with medicine. This can greatly lower the risk of cardiac ischemia.
- Hypertension management involves lifestyle changes and, if necessary, antihypertensive medications.
- Hyperlipidemia management includes dietary changes, exercise, and lipid-lowering medications.
- Diabetes management involves maintaining blood glucose levels within target ranges through diet, exercise, and medication.
Preventive Medications
Some medicines can help prevent cardiac ischemia in people at high risk. These include drugs that prevent blood clots, lower cholesterol, and slow the heart rate. The right medicine depends on the person’s health and risk factors.
Regular Screening for High-Risk Individuals
Screening is key to finding people at risk of cardiac ischemia. It looks at family history, lifestyle, and health. Catching problems early can stop cardiac ischemia or make it less severe.
People with a family history of heart disease or many risk factors should get screened often. This might include tests like electrocardiograms, stress tests, and scans for calcium in the arteries.
By using these prevention strategies, we can lower the number of cases of cardiac ischemia. This improves heart health for everyone.
Special Considerations for High-Risk Populations
Managing cardiac ischemia needs special care for certain groups. The elderly, diabetic patients, women, and those with kidney problems face unique challenges. They need treatment plans that fit their specific needs.
Treatment Approaches for Elderly Patients
Elderly patients with heart issues often have other health problems too. Their treatment plans must consider their overall health and how well they can function. It’s also important to watch for side effects from medicines.
Key considerations for elderly patients include:
- Careful dose adjustment of medications to minimize adverse effects
- Close monitoring for signs of heart failure or other complications
- Consideration of non-pharmacological interventions, such as lifestyle modifications
Managing Cardiac Ischemia in Diabetic Patients
Diabetes increases the risk of heart problems. Treating diabetes and heart issues together is key.
|
Management Strategy |
Description |
|---|---|
|
Glycemic control |
Tight blood glucose control to reduce cardiovascular risk |
|
Lipid management |
Aggressive management of dyslipidemia to reduce cardiac risk |
|
Antiplatelet therapy |
Use of antiplatelet agents to prevent ischemic events |
Women and Cardiac Ischemia Treatment
Women with heart problems often have different symptoms and risks than men. Their treatment plans should reflect these differences for the best care.
“The management of cardiac ischemia in women requires a nuanced understanding of their unique risk factors and presentation, which can differ significantly from those in men.” – A Cardiologist
Patients with Renal Impairment
People with kidney problems are at higher risk for heart issues. They need careful management to avoid kidney damage and heart problems.
Managing heart problems in those with kidney issues involves adjusting medicine doses and watching electrolyte levels. It’s also important to use safe tests to avoid harming the kidneys further.
Emerging Treatments and Future Directions
The future of treating cardiac ischemia is looking bright. New therapies are showing great promise. As we learn more about cardiac ischemia, we’re finding new ways to help patients.
Novel Therapeutic Targets
Scientists are working hard to find new ways to treat cardiac ischemia. They’re looking at inflammation, oxidative stress, and how to protect cells. This could lead to treatments that really make a difference.
Regenerative Medicine Approaches
Regenerative medicine is a field that’s growing fast. It includes using stem cells and gene therapy to fix damaged heart tissue. This could be a game-changer for treating cardiac ischemia.
Advances in Interventional Techniques
Interventional cardiology is getting better all the time. New techniques and technologies are being developed. This includes better stents and ways to open blocked arteries.
Personalized Medicine in Cardiac Ischemia
Personalized medicine is becoming more important. It means treatments are tailored to each patient. This can lead to better results and fewer complications.
|
Treatment Approach |
Description |
Potential Benefits |
|---|---|---|
|
Novel Therapeutic Targets |
Targeting pathways involved in inflammation and oxidative stress |
More effective symptom alleviation and addressing underlying causes |
|
Regenerative Medicine |
Stem cell therapy and gene therapy for tissue repair |
Potential for cardiac tissue regeneration and improved heart function |
|
Advances in Interventional Techniques |
New PCI techniques and stent technologies |
Improved outcomes in cardiac ischemia management |
|
Personalized Medicine |
Tailoring treatment to individual patient characteristics |
Improved patient outcomes and reduced risk of adverse events |
In conclusion, the future of treating cardiac ischemia is very promising. With new treatments and strategies coming, we can help more patients. We’re making great strides in improving heart health.
Conclusion
Effective treatment for cardiac ischemia needs a team effort. We’ve looked at many ways to treat heart ischemia, from medicines to changes in lifestyle and procedures. Healthcare providers can make a big difference by tailoring treatment plans. We’re dedicated to top-notch healthcare, helping international patients every step of the way. We use the latest medical treatments and care to help those with cardiac ischemia. Our goal is to give each patient the best care possible, meeting their specific needs.
FAQ
What are the primary treatment options for cardiac ischemia?
Treatments for cardiac ischemia include medicines, lifestyle changes, and procedures. These include percutaneous coronary intervention (PCI) and coronary artery bypass grafting (CABG).
How do antiplatelet medications help in managing cardiac ischemia?
Antiplatelet drugs stop blood clots from forming. This helps prevent heart attacks and manage cardiac ischemia well.
What lifestyle changes can help manage cardiac ischemia?
Eating healthy, exercising regularly, managing stress, and quitting smoking can help manage cardiac ischemia.
What is the role of cardiac rehabilitation in treating cardiac ischemia?
Cardiac rehab programs improve outcomes and quality of life. They include exercise, psychological support, and education.
How is cardiac ischemia diagnosed?
Diagnosing cardiac ischemia involves initial assessment, physical exam, and tests. It also includes electrocardiogram (ECG) findings and imaging techniques.
What are the emergency management steps for acute cardiac ischemia?
Treating acute cardiac ischemia starts with first response and stabilization. It includes oxygen, pain management, and initial meds. Then, patients are moved to a medical facility for further care.
Can cardiac ischemia be prevented?
Yes, preventing cardiac ischemia is possible. It involves managing risk factors, using preventive meds, and regular screenings for high-risk individuals.
What are the advanced medication therapies available for cardiac ischemia?
Advanced treatments include statins, ACE inhibitors, ARBs, and ranolazine. These help manage the condition and reduce risks.
How do interventional procedures like PCI help in treating cardiac ischemia?
PCI opens blocked arteries, restoring blood flow. This reduces symptoms and improves outcomes for patients with cardiac ischemia.
What are the benefits of surgical treatment options for cardiac ischemia?
Surgical options like CABG improve blood flow and reduce symptoms. They also enhance long-term survival for selected patients.
Are there special considerations for treating cardiac ischemia in high-risk populations?
Yes, high-risk groups need tailored treatments. This includes elderly, diabetic, women, and those with renal impairment.
What are the emerging treatments and future directions in cardiac ischemia management?
New treatments include novel targets, regenerative medicine, and personalized medicine. These aim to improve cardiac ischemia management.
Reference
Centers for Disease Control and Prevention. Evidence-Based Medical Insight. Retrieved from https://www.cdc.gov/heartdisease/treatment.htm





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























