
Did you know over 600,000 pacemakers are implanted worldwide each year? These devices greatly improve the lives of those with heart issues. They help control the heartbeat and enhance quality of life. But, a big question comes up: what happens when a pacemaker is turned off at the end of life? Turning off pacemaker at end of life? Get best facts. Can heart stop? Yes, if muscle fails. The device is a vital helper, not a cure-all.
A pacemaker is a lifesaver for many, giving them a sense of security and normalcy. Yet, as heart disease advances, understanding the pacemaker’s role at the end of life is key. We’ll look into the personal and medical sides of pacemaker deactivation, highlighting the choices that need to be made.
Key Takeaways
- Pacemakers are vital for heart conditions but raise big questions at the end of life.
- Knowing how pacemakers work is key for patients and families facing end-of-life choices.
- Deciding to turn off a pacemaker is a significant aspect of providing care for individuals with advanced heart disease.
- These decisions involve both personal and medical factors.
- Clear talk and full care are vital for patients and families dealing with these tough choices.
Understanding Pacemakers and Their Function
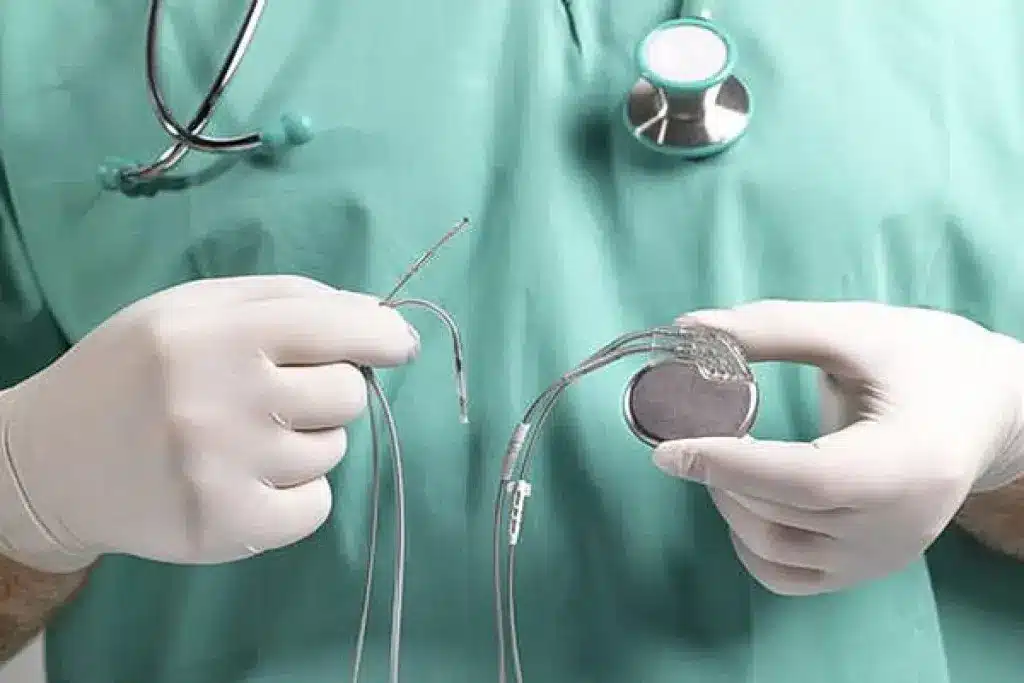
A pacemaker is a small device that helps control the heartbeat by generating electrical impulses. These devices are key for people with heart rhythm disorders. They offer a reliable way to manage irregular heartbeats.
What Is a Pacemaker and How Does It Work?
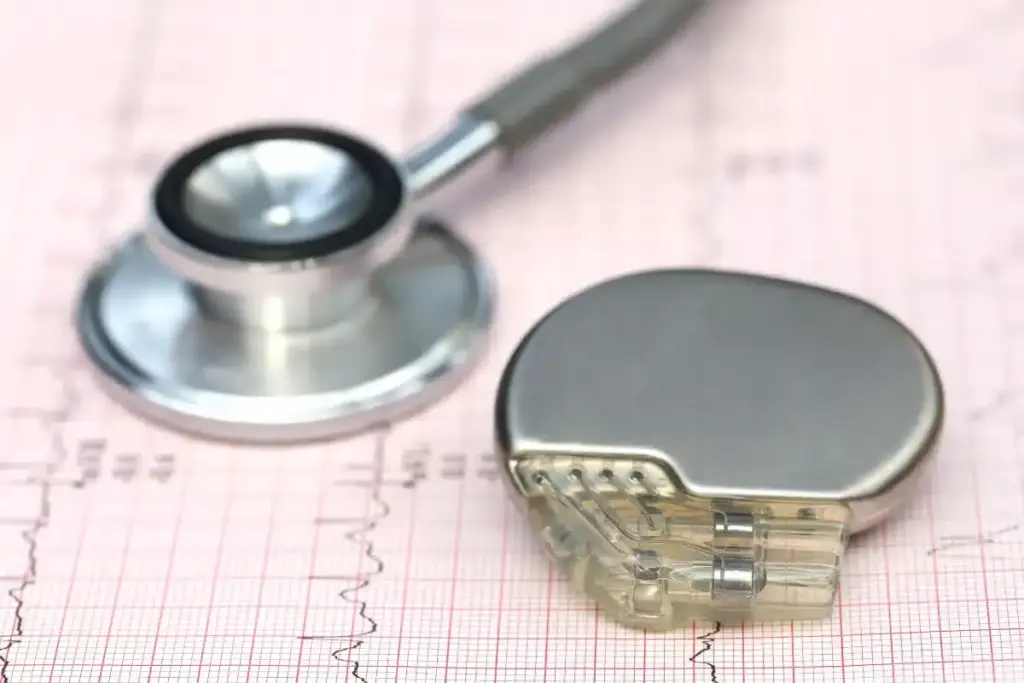
A pacemaker has two main parts: a pulse generator and leads. The pulse generator has the electronic circuitry and battery. The leads are thin wires that connect the pulse generator to the heart.
When the heart’s natural rhythm is disrupted, the pacemaker sends electrical impulses. This helps restore a normal heartbeat.
The pacemaker’s function is based on monitoring the heart’s rhythm and adjusting its pacing. Modern pacemakers are advanced. They can adapt to the patient’s needs and activity level.
Types of Pacemakers and Their Capabilities
There are several types of pacemakers, each for different heart rhythm issues. The most common types include:
- Single-chamber pacemakers: These devices use one lead to pace either the atrium or ventricle.
- Dual-chamber pacemakers: These devices use two leads, one for the atrium and one for the ventricle. They provide a more natural pacing by coordinating the contractions of both chambers.
- Biventricular pacemakers: Used in cardiac resynchronization therapy, these devices help coordinate the pumping action of the heart’s ventricles.
Cardiologists are key in managing pacemaker implantation and follow-up care. They decide if a pacemaker is needed, choose the right type, and ensure it works properly.
|
Type of Pacemaker |
Description |
Capabilities |
|---|---|---|
|
Single-Chamber |
Uses one lead to pace either the atrium or ventricle. |
Effective for certain types of arrhythmias. |
|
Dual-Chamber |
Uses two leads to pace both the atrium and ventricle. |
Provides more natural pacing, improving heart function. |
|
Biventricular |
Used in cardiac resynchronization therapy. |
Coordinates the pumping action of the ventricles. |
A cardiologist says, “The choice of pacemaker depends on the patient’s specific condition and needs. Regular follow-up care is essential to ensure the device is functioning correctly and to make any necessary adjustments.”
“Pacemakers have revolutionized the treatment of heart rhythm disorders, giving patients a new chance at life.”
The Relationship Between Your Heart and a Pacemaker
The connection between a pacemaker and the heart is quite complex. It involves how the device works and the heart’s natural beat. A pacemaker helps the heart’s electrical system, making sure it beats at the right rate.
How Pacemakers Interact With Your Natural Heartbeat
Pacemakers send electrical signals to make the heart beat at a normal pace. They are set to work with the heart’s natural rhythm. They adjust their signals based on what the heart needs.
Here are some key points about how pacemakers and the heart interact:
- Sensing: Pacemakers have sensors to catch the heart’s natural electrical signals.
- Pacing: If the heart beats too slow, the pacemaker sends signals to make it beat.
- Adaptability: Today’s pacemakers can change their beat rate based on activity or other factors.
Dependency vs. Non-Dependency on Pacemakers
How much a person depends on their pacemaker can vary. Some need it to control their heartbeat because of a heart condition. Others might have it as a precaution.
Doctors check if someone needs a pacemaker and how well it works. They use tests like:
- Electrocardiograms (ECGs): To look at the heart’s electrical activity.
- Holter monitoring: A 24-hour ECG test to see the heart’s rhythm over time.
- Stress tests: To see how the heart reacts to exercise.
It’s important to know how a pacemaker and the heart work together for heart health. Regular visits to a heart specialist are key. They help make sure the pacemaker is working right and make any needed changes.
Can Your Heart Stop Despite Having a Pacemaker?
Pacemakers are key in managing heart rhythms. Yet, they have their limits. These devices help regulate heartbeats but can be affected by technical issues and medical conditions.
Technical Limitations of Pacemakers
Pacemakers are advanced, but they’re not perfect. Several factors can lead to technical limitations, including:
- Battery Life: Pacemakers run on batteries that wear out. If not replaced or recharged, they can fail.
- Lead Issues: The wires connecting the pacemaker to the heart can break or move out of place. This hampers the device’s function.
- Device Malfunction: Pacemakers, like any electronic device, can fail. This is rare but can happen.
It’s vital to have regular cardiologist appointments. These visits help check the pacemaker’s performance and fix any problems early on.
Medical Conditions That Can Override Pacemaker Function
Some medical issues can hinder a pacemaker’s effectiveness. These include:
- Heart Failure: Severe heart failure can make it hard for the pacemaker to control the heart’s rhythm.
- Electrolyte Imbalance: Big changes in electrolytes like potassium or magnesium can disrupt heart rhythm and bypass the pacemaker’s control.
- Other Cardiac Conditions: Issues like atrial fibrillation or ventricular tachycardia can sometimes resist pacemaker regulation.
A detailed cardiac workup is essential. It helps spot any conditions that might be affecting the pacemaker. This way, doctors can adjust the treatment plan as needed.
Pacemaker Failures and Malfunctions
Pacemakers are made to work well, but they can fail. It’s important to know why and how to spot the signs. These failures, though rare, can affect people who depend on pacemakers. Knowing about these problems helps in taking care of patients better.
Common Causes of Pacemaker Malfunction
Pacemaker problems can come from many sources. These include issues with the device itself, outside factors, and health conditions of the patient. Some common reasons include:
- Battery depletion
- Lead malfunction or fracture
- Device programming errors
- Electromagnetic interference
- Hardware or software defects
Seeing a cardiologist regularly is key. It helps keep the device working right and fixes problems early.
Warning Signs of Pacemaker Problems
It’s vital to know the signs of pacemaker trouble. Symptoms might be:
- Dizziness or lightheadedness
- Shortness of breath
- Palpitations or irregular heartbeats
- Fatigue or weakness
- Swelling in the legs or feet
If you notice any of these, get help right away.
|
Symptom |
Possible Cause |
Action |
|---|---|---|
|
Dizziness |
Pacemaker not pacing correctly |
Check device function |
|
Shortness of breath |
Heart failure or lead issue |
Consult cardiologist |
|
Palpitations |
Device programming issue |
Adjust device settings |
Cardiac Arrest in Patients With Pacemakers
Even with a working pacemaker, cardiac arrest can happen. This shows we need to take care of our hearts fully. It’s key to know the differences in heart problems and how they affect pacemakers.
Understanding the Difference Between Heart Failure and Cardiac Arrest
Heart failure and cardiac arrest are not the same. Heart failure means the heart can’t pump enough blood. Cardiac arrest is when the heart suddenly stops beating.
Heart failure is a long-term issue that can be managed. But cardiac arrest is an urgent emergency. Knowing this helps those with pacemakers get the right care.
How Cardiac Arrest Can Occur Even With a Functioning Pacemaker
A working pacemaker helps control the heartbeat. But it can’t prevent all cardiac arrests. Heart disease, electrical heart problems, and severe illnesses can cause it.
|
Factors Contributing to Cardiac Arrest |
Description |
|---|---|
|
Underlying Heart Disease |
Pre-existing heart conditions that can lead to cardiac arrest despite pacemaker functionality. |
|
Electrical Disturbances |
Abnormal heart rhythms that can cause cardiac arrest, potentially due to issues not addressed by the pacemaker. |
|
Severe Medical Conditions |
Serious health issues, such as severe infections or electrolyte imbalances, that can precipitate cardiac arrest. |
A cardiologist plays a big role in managing these issues. Regular check-ups and monitoring can spot problems early. A cardiologist also helps manage heart conditions with pacemaker therapy.
End-of-Life Considerations for Pacemaker Patients
When it comes to pacemakers, end-of-life care is filled with tough choices. We must think about deactivating pacemakers and what it means. It’s key to know how pacemakers work in end-of-life situations.
Natural Death Process With a Pacemaker
A pacemaker can change how someone dies. It helps control heart rhythm but can’t stop the heart from stopping. Sometimes, it keeps working even when the heart is failing, making death seem longer.
Thinking about deactivating a pacemaker is complex. It might let the natural dying process happen. But, this choice needs careful thought and advice from doctors.
How Pacemakers Affect the Dying Process
Pacemakers can impact dying in different ways. For some, they keep the heart going even as other parts of the body stop. This can make dying take longer.
It’s important to know how pacemakers affect dying. Patients and their families should talk to cardiologists. This way, they can make choices about end-of-life care that are right for them.
|
Consideration |
Description |
Impact on Dying Process |
|---|---|---|
|
Pacemaker Functionality |
Regulates heart rhythm |
May prolong dying process |
|
Pacemaker Deactivation |
Allows natural heart rhythm |
Can facilitate natural dying process |
|
Cardiologist Consultation |
Provides medical guidance |
Essential for informed decisions |
By understanding these points, patients and families can make better choices about end-of-life care. This way, they can ensure their wishes are followed and comfort is the top priority.
Turning Off Pacemaker at End of Life: The Process
When patients are close to the end, doctors and families must think about pacemakers. Deciding to turn off a pacemaker is tough. It requires knowing the medical steps and possible changes in the body.
Medical Procedures for Deactivating a Pacemaker
Turning off a pacemaker is a serious step that needs careful thought and skill. Doctors, often cardiologists or palliative care specialists, do this. They use a programmer to talk to the pacemaker and stop it from beating the heart.
This can happen in a hospital or at home, depending on the situation and the device type.
Key Steps in Pacemaker Deactivation:
- Assessing the patient’s health and wishes about the pacemaker.
- Talking with the patient and their family about what deactivating the pacemaker means.
- Adjusting the pacemaker settings with a programmer device.
- Watching the patient closely after to make sure they’re comfortable and manage any symptoms.
What Happens Physically After Pacemaker Deactivation
After a pacemaker is turned off, the body can change in different ways. This depends on the heart condition and overall health. Some people might not feel a big change right away. Others might see their condition get worse as their heart goes back to its natural beat.
|
Physical Changes |
Possible Outcomes |
|---|---|
|
Heart Rate |
May slow down or become more irregular. |
|
Breathing |
Could become more labored or irregular. |
|
Consciousness |
May decrease as the patient’s condition progresses. |
Healthcare teams should support patients and their families during this time. They need to manage symptoms and ensure comfort. The choice to stop a pacemaker is personal. It should be made with careful thought about the patient’s wishes and health.
Ethical Considerations in Pacemaker Deactivation
When patients near the end of life, deciding on their pacemaker becomes a big ethical issue. This choice needs careful thought from doctors, patients, and their families.
Is Turning Off a Pacemaker Considered Euthanasia?
Whether deactivating a pacemaker is seen as euthanasia is a topic of debate. We must make a clear difference between stopping life-saving treatments and euthanasia. Euthanasia is when someone actively ends a life. But, turning off a pacemaker is seen as stopping a treatment that’s no longer needed or wanted.
It’s important to know that deactivating a pacemaker is a medical choice. It’s based on the patient’s right to decide about their care. This is key in the rules that guide care at the end of life.
Medical Ethics Surrounding Device Deactivation
The ethics of deactivating pacemakers involve respecting the patient’s choices, doing good, avoiding harm, and fairness. Patient autonomy is central, as it honors the patient’s right to decide their care, including deactivating a pacemaker.
Doctors must weigh these ethical values against the facts of pacemaker use and the effects of turning it off. This requires care that is both compassionate and complete. It must meet the physical, emotional, and spiritual needs of patients and their families.
In summary, the ethics of pacemaker deactivation are complex and need careful thought. By understanding these ethics and valuing patient autonomy, we can make these tough choices with kindness and integrity.
Legal Framework for Pacemaker Deactivation in the United States
It’s important to know the legal rules for turning off pacemakers. This choice is complex, involving legal, ethical, and medical aspects.
Patient Rights and Autonomy
Patient choice is key in deciding to turn off a pacemaker. Patients have the right to decide on their medical care, including devices like pacemakers. Advance directives and healthcare proxies help patients share their end-of-life care wishes.
The Patient Self-Determination Act of 1990 makes sure patients know about advance directives. This law helps patients make choices about their care, like turning off medical devices.
State-by-State Variations in End-of-Life Laws
End-of-life laws differ across states, affecting pacemaker deactivation. Some states have laws or court decisions on deactivating life-saving devices. For example, some states let doctors follow a patient’s advance directive to turn off a pacemaker, while others might not.
Patients and their families need to know the laws in their state. Talking to a healthcare provider or legal expert can help understand these laws. Doctors and other healthcare workers are key in making sure patients get care that matches their wishes.
The Role of Advance Directives in Pacemaker Management
It’s key for patients with pacemakers to know about advance directives. These documents outline a patient’s medical treatment wishes, including pacemaker management, if they can’t speak for themselves.
Having an advance directive helps healthcare providers and family members. It ensures the patient’s wishes are followed, even when they can’t speak for themselves.
Creating Specific Instructions for Your Cardiac Device
When making an advance directive, include pacemaker details. You might want to say when you’d like your pacemaker turned off or specific settings for end-of-life care.
Talking to your cardiologist or heart specialist is important. They can help understand pacemaker settings and guide your care choices.
Communicating Your Wishes to Healthcare Providers
After making an advance directive, share it with your healthcare team. This way, your cardiologist and others know your pacemaker wishes.
Good communication means giving your healthcare team copies of your advance directive. Discuss your wishes with them and make sure they’re in your medical records. This way, your autonomy is respected in your care.
We suggest reviewing and updating your advance directive often. This ensures your wishes reflect any changes in your preferences or health.
The Cardiologist’s Role in End-of-Life Care
Cardiologists do more than just treat hearts. They also offer compassionate care at the end of life. As heart specialists, they support patients with serious heart conditions.
Approaching End-of-Life Discussions
Cardiologists handle end-of-life talks with care and skill. These talks help understand what patients want for their care. They make sure patients and families know all their options, like managing pacemakers.
Good end-of-life talks include:
- Clear talks about the patient’s future
- Explaining treatment choices and their effects
- Knowing the patient’s values and wishes
- Supporting the patient and family in making decisions
Collaboration Between Cardiology and Palliative Care
Working together, cardiology and palliative care teams offer full end-of-life care. This teamwork ensures patients get the medical help they need. It also addresses their physical, emotional, and spiritual needs.
“Palliative care teams bring expertise in symptom management and supportive care, which complements the medical treatment provided by cardiologists.”
— Expert in Palliative Care
Key parts of this teamwork are:
- Planning care together to meet the patient’s needs
- Working together on decisions with the patient
- Coordinating care for smooth support for the patient
By combining cardiology and palliative care, we aim to give patients the best quality of life they can have.
Family Considerations and Emotional Impact
Deciding to turn off a pacemaker at the end of life is not just about medical choices. It also involves family and emotional factors. It’s important to think about how this affects both the patient and their loved ones.
Supporting Loved Ones Through Pacemaker Deactivation Decisions
Helping family members decide on pacemaker deactivation needs empathy and clear talk. It’s key to get a cardiologist’s opinion to help make the right choice.
- Encourage open talks about what the patient wants.
- Offer emotional support and clear up any wrong ideas about deactivation.
- Help the patient, family, and doctors talk to each other to make sure everyone agrees.
This way, families can make choices that respect the patient’s wishes and help them feel supported.
Addressing Common Fears and Misconceptions
There are often wrong ideas about turning off a pacemaker, like thinking it will make someone die right away. Clearing up these wrong ideas with the right facts can ease worries.
- The idea that turning off a pacemaker means dying right away.
- Thinking it’s like ending someone’s life.
- Worries about pain or comfort after the pacemaker is turned off.
Talking to doctors can help calm fears and offer support to both the patient and their family.
In short, choosing to turn off a pacemaker is a big decision that affects many areas. Understanding these and getting advice from experts can help families get through this tough time more easily.
Palliative Care Approaches for Pacemaker Patients
Understanding both the pacemaker and the patient’s health is key for effective palliative care. As we face end-of-life care, we must tailor our approach for pacemaker patients. This ensures their unique needs are met.
Managing Symptoms After Pacemaker Deactivation
After a pacemaker is turned off, patients may face various symptoms. Symptom management is vital for their comfort. Symptoms like shortness of breath, pain, and anxiety need attention.
Medicines are important in managing these symptoms. Opioids can help with pain and breathing issues. Anxiolytics are used for anxiety. Personalized care plans help control symptoms for each patient.
Ensuring Comfort During the End-of-Life Transition
Comfort during the end-of-life transition goes beyond physical symptoms. It includes emotional and spiritual support. Cardiologists and palliative care specialists work together for this.
Making the patient’s environment comfortable is essential. Adjusting their surroundings can reduce stress. Family support is also key, with open communication helping to clear fears.
Conclusion
Understanding pacemakers and their role in end-of-life care is key for patients and their families. A pacemaker helps control the heartbeat but doesn’t prevent cardiac arrest or heart failure. Deciding to turn off a pacemaker at the end of life is a personal choice, considering medical, ethical, and legal aspects.
Cardiologists are essential in helping patients make these decisions. They offer expert care and support during tough times. Knowing about pacemakers in end-of-life care helps patients make informed choices. It ensures their wishes are honored. Good end-of-life care goes beyond managing medical devices. It also meets the emotional and spiritual needs of patients and their families.
FAQ
What is a pacemaker and how does it work?
A pacemaker is a small device implanted under the skin. It helps control the heartbeat. It sends electrical impulses to keep the heart beating at a normal rate.
Can a heart stop beating with a pacemaker?
Yes, a heart can stop beating even with a pacemaker. A pacemaker can regulate the heartbeat but can’t prevent all heart problems.
What happens when a pacemaker is turned off at the end of life?
When a pacemaker is turned off, it stops sending impulses to the heart. This can lead to different outcomes based on the heart condition and other factors.
Is turning off a pacemaker considered euthanasia?
No, turning off a pacemaker is not euthanasia. It’s a medical choice made to ease suffering, not to end life.
How do cardiologists approach end-of-life discussions with patients who have pacemakers?
Cardiologists talk about end-of-life with care and understanding. They consider the patient’s wishes and medical situation. They help make decisions about pacemaker management and care.
What is the role of advance directives in managing pacemakers?
Advance directives are key in managing pacemakers. They let patients state their wishes about device deactivation and care. This ensures care matches their values and preferences.
Can a pacemaker be deactivated without a patient’s consent?
No, a pacemaker can’t be turned off without consent. Patients have the right to decide about their care, including deactivation.
What are the symptoms of pacemaker malfunction?
Symptoms of malfunction include dizziness, fainting, and irregular heartbeats. If you notice these, seek medical help right away.
How do cardiologists manage symptoms after pacemaker deactivation?
Cardiologists work with palliative care to manage symptoms after deactivation. They use various methods to comfort patients.
What is the difference between heart failure and cardiac arrest?
Heart failure means the heart can’t pump enough blood. Cardiac arrest is when the heart suddenly stops. Both are serious but different conditions.
Can cardiac arrest occur even with a functioning pacemaker?
Yes, cardiac arrest can happen even with a working pacemaker. A pacemaker can’t prevent all heart emergencies.
How do I create specific instructions for my cardiac device?
To make instructions for your device, talk to your cardiologist. Include them in your advance directive. This ensures your wishes are followed by healthcare providers.
What is the legal framework for pacemaker deactivation in the United States?
The laws for pacemaker deactivation vary by state in the U.S. Cardiologists follow these laws to ensure care matches patient wishes and values.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/PMC9982664/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























