
Did you know that nearly one in four women in the United States will face pelvic floor disorders? Pelvic floor disorders can really affect a woman’s life, causing pain and discomfort. A urogynecologist is a specialist who deals with these issues. They use their knowledge of urology and gynecology to help.
Talking about pelvic health might feel hard, but getting the right care is key. A urogynecologist can handle many problems, like urinary incontinence and pelvic organ prolapse. They offer care that’s both personal and caring.
Key Takeaways
- A urogynecologist specializes in the diagnosis and treatment of female pelvic floor disorders.
- Conditions treated include urinary incontinence, pelvic organ prolapse, and fecal incontinence.
- Urogynecologists combine expertise from urology and gynecology to provide complete care.
- Treatment plans are tailored to the individual, focusing on both surgical and non-surgical options.
- Seeking care from a urogynecologist can greatly improve a woman’s quality of life.
Introduction to Urogynecology
Urogynecology is a key part of women’s healthcare. It deals with complex pelvic floor issues, common during and after pregnancy and menopause. This field combines gynecology and urology for a full care approach.
Understanding urogynecology is vital for appreciating the advanced care for pelvic floor conditions. As a distinct medical specialty, it plays a big role in diagnosing and treating pelvic floor disorders. This improves the quality of life for many women.
Definition and Scope of Urogynecology
Urogynecology is a subspecialty of gynecology. It focuses on diagnosing, treating, and managing disorders of the female pelvic floor. This includes pelvic organ prolapse and urinary incontinence. Urogynecology offers both surgical and non-surgical treatments for a holistic approach to women’s pelvic health.
- Diagnosis of pelvic floor disorders
- Treatment options including lifestyle modifications, physical therapy, and surgery
- Management of conditions such as pelvic organ prolapse and urinary incontinence
Knowing the definition and scope of urogynecology helps us see the full care urogynecologists provide. They address the complex needs of women with pelvic floor disorders.
Importance of Urogynecologists in Women’s Health
Urogynecologists play a critical role in women’s health by specializing in the treatment of pelvic floor disorders. These conditions can greatly affect a woman’s quality of life, causing discomfort, pain, and emotional distress. Urogynecologists are trained to diagnose and treat these conditions with personalized care.
The American Urogynecologic Society says, “Urogynecologists are dedicated to providing the highest level of care for women with pelvic floor disorders, improving their quality of life and overall well-being.” We agree, highlighting the critical role of urogynecologists in addressing women’s complex health needs.
“The care provided by urogynecologists is not just about treating a condition; it’s about restoring a woman’s confidence and improving her overall quality of life.”
— A leading urogynecologist
The role of urogynecologists is essential. They provide critical care that addresses both the physical and emotional aspects of pelvic floor disorders. This empowers women to take control of their health.
Common Conditions Treated by Urogynecologists
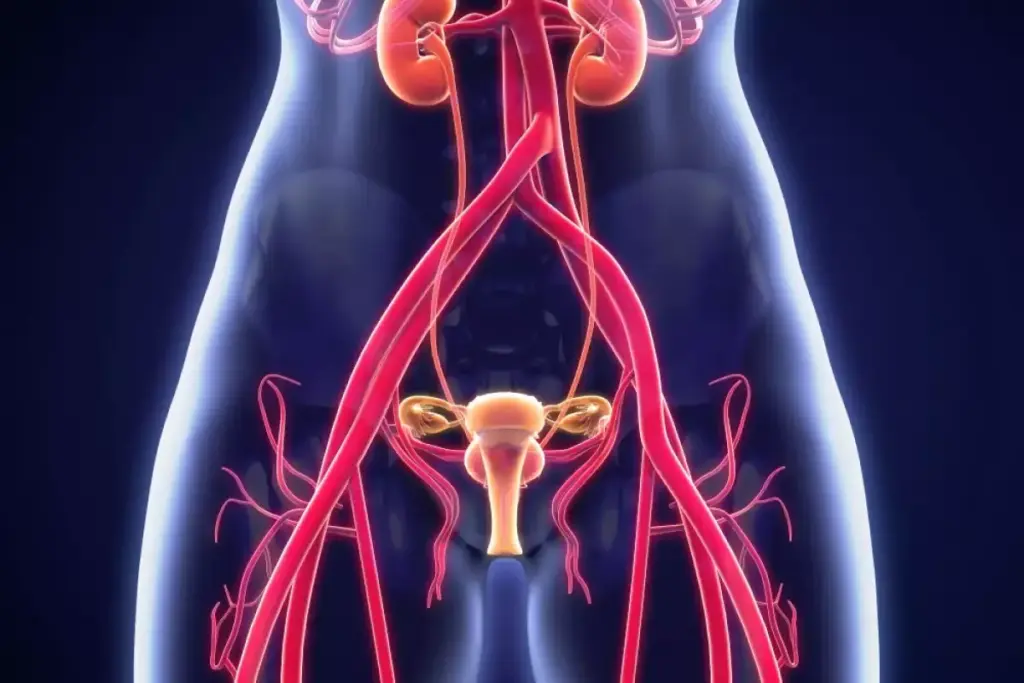
Many women face pelvic floor disorders, urinary incontinence, or prolapse. Urogynecologists are specialists who effectively address these issues. These problems can really change a woman’s life, affecting her comfort, mood, and social life.
Pelvic Floor Disorders
Pelvic floor disorders affect the muscles and tissues around the pelvic organs. Symptoms include pelvic pain, trouble with urination or bowel movements, and discomfort during sex. We understand how upsetting these symptoms can be and how they can mess up daily life.
- Pelvic organ prolapse
- Urinary incontinence
- Fecal incontinence
- Chronic pelvic pain
Dealing with pelvic floor disorders often means making lifestyle changes, physical therapy, and sometimes surgery. Urogynecologists are skilled at finding the cause and creating a treatment plan.
Urinary Incontinence
Urinary incontinence means losing bladder control and leaking urine. It’s common, often after childbirth or during menopause. We recognize how embarrassing and confidence-shaking it can be.
There are different kinds of urinary incontinence, like:
- Stress incontinence: happens when coughing, sneezing, or lifting
- Urge incontinence: sudden, intense need to urinate
- Mixed incontinence: a mix of stress and urge incontinence
Treatments include pelvic floor exercises, lifestyle changes, medicines, and sometimes surgery like sling surgery.
Prolapse and Its Types
Pelvic organ prolapse happens when the muscles and tissues around the pelvic organs weaken. This causes the organs to drop or bulge into the vagina. There are several types, like:
- Cystocele: bladder prolapse
- Rectocele: rectal prolapse
- Uterine prolapse: uterus prolapse
- Vaginal vault prolapse: vaginal apex prolapse
Urogynecologists use different methods to treat prolapse, like pessary placement, physical therapy, and surgery. We are committed to helping women understand their condition and find the best treatment.
Diagnostic Procedures in Urogynecology
Getting a correct diagnosis is key to treating urogynecology issues. We use many diagnostic tools to check pelvic floor disorders. These tools help us understand the problem and choose the right treatment.
Physical Examination Techniques
A detailed physical exam is the first step in diagnosing pelvic floor disorders. We check the pelvic organs and muscles during this exam. This helps us find the best tests to do next.
Imaging Tests: Ultrasound and MRI
Imaging tests are very important in diagnosis. Ultrasound helps us see the pelvic organs and their movement. It spots problems like pelvic organ prolapse or bladder issues.
MRI (Magnetic Resonance Imaging) gives detailed pictures of the pelvic area. It’s great for complex cases or when we need detailed images for surgery.
Urodynamic Testing
Urodynamic testing checks how well the bladder and urethra work. It helps find issues like urinary incontinence. This test shows how the lower urinary tract works, helping us find the right treatment.
Surgical Procedures Performed by Urogynecologists
Urogynecologists use surgery when other treatments don’t work. They aim to fix complex pelvic floor issues. This helps patients feel better and live better lives.
Pelvic Organ Prolapse Surgery
Pelvic organ prolapse happens when pelvic muscles weaken. This causes organs to drop into the vagina. Symptoms include pain, trouble peeing, and bowel issues.
There are a few ways to fix this:
- Native tissue repair uses the patient’s own tissues to fix the problem.
- Mesh repair uses synthetic mesh for support.
- Laparoscopic and robotic surgeries are less invasive, helping patients recover faster.
A study in the Journal of Urogynecology found these surgeries work well. Most patients see big improvements in their symptoms and life quality.
|
Surgical Approach |
Description |
Recovery Time |
|---|---|---|
|
Native Tissue Repair |
Reattachment using patient’s tissues |
6-8 weeks |
|
Mesh Repair |
Use of synthetic mesh for support |
4-6 weeks |
|
Laparoscopic/Robotic Surgery |
Minimally invasive technique |
2-4 weeks |
Sling Procedures for Incontinence
Urinary incontinence is common in women. It’s often due to weak pelvic muscles or urethral issues. Sling procedures help by placing a supportive sling under the urethra.
There are a few types of sling procedures:
- Mid-urethral sling is a minimally invasive procedure using synthetic mesh.
- Autologous sling uses the patient’s own tissue.
The American Urogynecologic Society says sling procedures are very effective. They have high success rates and few complications.
Hysterectomy and Its Variants
Hysterectomy is sometimes done by urogynecologists. It’s for conditions like uterine prolapse or severe pelvic pain when other treatments fail.
There are different types of hysterectomy:
- Total hysterectomy removes the uterus and cervix.
- Supracervical hysterectomy removes only the upper uterus.
- Laparoscopic and robotic-assisted hysterectomies are less invasive.
Choosing to have a hysterectomy is a big decision. It’s made after talking it over with a healthcare provider. They consider the benefits and risks together.
“The choice of surgical procedure depends on the individual patient’s condition, medical history, and personal preferences. Urogynecologists work closely with their patients to determine the most appropriate treatment plan.”
Non-Surgical Treatment Options
There are many non-surgical ways to handle pelvic floor disorders. These non-surgical methods can be highly effective in managing symptoms. They often give a lot of relief and improve symptoms without surgery.
Lifestyle Modifications
Making lifestyle changes is often the first step. Simple adjustments can make a big difference. These include:
- Dietary changes to manage constipation and reduce pressure on the pelvic floor
- Fluid management to avoid incontinence triggers
- Weight management to reduce pressure on the pelvic organs
- Avoiding heavy lifting and bending
By making these changes, many women see a big improvement. As one patient said,
“Making dietary changes and losing a bit of weight really helped me manage my incontinence.”
Physical Therapy for Pelvic Health
Physical therapy is key in treating pelvic floor disorders. Pelvic floor physical therapy uses exercises and techniques to strengthen the muscles. This includes:
- Kegel exercises to strengthen pelvic floor muscles
- Biofeedback to improve muscle control
- Manual therapy to release tension in the pelvic area
These therapies are customized for each person. They offer a personalized approach to treatment.
Medications for Managing Symptoms
For some, medications can help manage symptoms. Medications can:
- Relax the bladder muscle to reduce urgency and frequency
- Improve bladder control
- Manage pain associated with pelvic floor disorders
We work with our patients to find the right medication and dosage. This ensures the best results.
Non-surgical treatments are a great option for pelvic floor disorders. They offer relief and improve life quality. By combining lifestyle changes, physical therapy, and medications, we create a treatment plan that meets each patient’s needs.
Advanced Procedures in Urogynecology
Urogynecology is seeing a big change thanks to new technologies and methods. These new ways are making treatments better and recovery times shorter. Now, we have robotic-assisted surgery, new techniques, and biomaterials for support.
Robotic-Assisted Surgery
Robotic-assisted surgery is a big step up in urogynecology. This technology makes procedures more precise and cuts down on recovery time. It lets us do more complex surgeries with less invasion.
Using robots for surgery means less blood loss, fewer complications, and shorter hospital stays. Patients get back to their lives faster, making it a great choice for surgery.
Minimally Invasive Techniques
Minimally invasive techniques are key in advanced urogynecology. They use smaller cuts, causing less damage and pain. Patients heal faster because of this. We use these methods for many urogynecological issues.
These techniques have many benefits. They leave less scarring, lower the chance of infection, and help patients recover quicker. They’re great for those with health issues or who want to get back to their lives fast.
Biomaterials for Pelvic Support
Biomaterials for pelvic support are becoming more common in urogynecology. They’re used in surgeries to strengthen weak pelvic areas. These materials can be synthetic or biological and are picked based on the patient’s needs.
Biomaterials have many pluses, like lasting longer and having fewer complications. They’re used in sling surgeries for incontinence and repairs for prolapse.
Post-Operative Care and Recovery
The success of urogynecologic surgery depends on the care after the procedure. Proper post-operative care is key for a smooth recovery.
What to Expect After Surgery
After urogynecologic surgery, recovery time varies based on the procedure. It’s important to rest and avoid heavy lifting and bending. Following the surgeon’s instructions helps prevent complications and speeds up recovery.
Patients often feel discomfort, swelling, and bruising after surgery. These symptoms can be managed with pain relief medications and other measures suggested by your urogynecologist.
Follow-Up Appointments and Their Importance
Follow-up appointments are vital for post-operative care. They let your urogynecologist check on your healing, remove sutures or staples, and address any issues. Attending these appointments as scheduled is key for a successful recovery.
- Monitoring the healing process
- Removing sutures or staples
- Addressing patient concerns
- Managing possible complications
Managing Complications and Side Effects
While complications are rare, knowing the risks and how to manage them is important. Common issues include infection, bleeding, and reactions to anesthesia. Recognizing complications early and getting immediate medical help can greatly improve outcomes.
- Watch for signs of infection, such as fever or increased redness
- Report any unusual bleeding or discharge
- Follow medication instructions carefully
Understanding what to expect after surgery, the importance of follow-up appointments, and managing complications helps patients feel confident during recovery. Our team is dedicated to providing full care and support throughout your recovery journey.
The Role of Urogynecologists in Patient Education
Urogynecologists do more than treat patients; they also teach them about their health. As experts in women’s health, we know how key it is to educate patients. We help them understand their conditions and the options for treatment.
Explaining Conditions and Treatments
Urogynecologists are key in making complex health issues simple for patients. We take the time to explain the diagnosis, treatment choices, and what to expect during recovery. This approach reduces anxiety and uncertainty, enabling patients to make well-informed decisions.
For example, when talking about pelvic floor disorders, we explain the body parts involved and how the condition affects them. We discuss treatment options like lifestyle changes, physical therapy, and surgery. We highlight the benefits and risks of each.
Empowering Patients in Health Decisions
Empowering patients is our main goal. By giving them all the information about their condition and treatment options, we help them take charge of their health. This is key for making choices that fit their personal values and preferences.
We encourage patients to ask questions and share their concerns. This open talk helps us understand their needs better. For instance, when discussing urinary incontinence treatment, we consider their lifestyle, condition severity, and preferences. This way, we suggest the best treatment for them.
Through education and open communication, we work together in healthcare. This approach not only makes patients happier but also leads to better health results. When patients understand their condition and treatment options, they are more likely to follow their treatment plans and make healthy choices.
Conclusion: The Future of Urogynecology
The future of urogynecology looks bright with new research and tech. We’re getting better at treating pelvic floor issues. This shows how vital specialized care is for women’s health.
Advances in Research and Technology
Research in urogynecology is leading to better treatments. Minimally invasive surgeries and robotic-assisted surgeries are making recovery faster and more precise. New biomaterials are also helping women with prolapse and other issues.
New tech like advanced imaging and urodynamic testing is key. These tools help doctors diagnose and treat better. This leads to better care for patients.
The Growing Importance of Urogynecological Care
As more people get older, the need for urogynecology will grow. The importance of urogynecological care is huge. It greatly affects women’s lives. Urogynecologists help women stay independent and healthy.
“The future of urogynecology is bright, with ongoing research and technological advancements set to improve patient outcomes significantly.”
We’re dedicated to improving urogynecology. We want to make sure women get the best care. With new research and tech, we’re excited for a future where pelvic floor issues are better managed. Women’s health will greatly improve.
Resources and Support for Patients
Dealing with pelvic floor disorders can be tough. But, there are many resources and support systems available. We aim to provide full support to those facing these challenges.
Finding the right care and understanding options is key. We’re here to help patients navigate this journey.
Finding a Urogynecologist
Finding a qualified urogynecologist is vital. Start by asking your primary care doctor for a referral. Also, check out directories from groups like the American Urogynecologic Society (AUGS).
When choosing a urogynecologist, look at their experience and services. It’s important to find someone who is both skilled and supportive.
Support Groups and Educational Resources
Support groups offer emotional support and connections. They come in both in-person and online formats. This lets patients pick what works best for them.
Educational resources help patients understand their conditions. Look for peer-reviewed articles, educational websites, and patient advocacy groups. These can help patients make informed decisions about their care.
- Pelvic Floor Disorders Alliance
These organizations provide a lot of information. They cover symptom management and treatment options. This empowers patients to be active in their healthcare.
Frequently Asked Questions About Urogynecology
Women often have questions and concerns about urogynecological care. We’re here to address them. Knowing what to expect from a urogynecologist visit can help reduce anxiety. It ensures a productive consultation.
Addressing Common Concerns
Many women have common concerns about urogynecological conditions and their treatment. Our team is dedicated to providing compassionate and expert care. Some of the most frequently asked questions include:
- What are the symptoms of pelvic floor disorders?
- How is urinary incontinence treated?
- What can I expect during a urogynecologist visit?
Preparing for Your Visit
To make the most of your visit, prepare by writing down your symptoms, medical history, and any questions you have. This will help us provide you with personalized care. By being open and honest about your symptoms and medical history, we can work together to develop an effective treatment plan.
FAQ
What is a urogynecologist?
A urogynecologist is a doctor who specializes in treating problems with the female pelvic floor. This includes issues like urinary incontinence, pelvic organ prolapse, and fecal incontinence.
What conditions do urogynecologists treat?
Urogynecologists deal with a variety of conditions. These include pelvic floor disorders, urinary incontinence, and different types of prolapse. They provide detailed care for women with these complex issues.
What diagnostic procedures are used in urogynecology?
In urogynecology, doctors use several diagnostic methods. These include physical exams, imaging tests like ultrasound and MRI, and urodynamic testing. These help accurately diagnose pelvic floor disorders.
What surgical procedures do urogynecologists perform?
Urogynecologists do various surgeries. This includes fixing pelvic organ prolapse, sling procedures for incontinence, and hysterectomy. These surgeries aim to correct complex pelvic floor disorders.
Are there non-surgical treatment options available?
Yes, there are non-surgical options. These include making lifestyle changes, physical therapy for pelvic health, and medications. These help manage symptoms of pelvic floor disorders.
What advanced procedures are available in urogynecology?
Urogynecology offers advanced procedures. These include robotic-assisted surgery, minimally invasive techniques, and the use of biomaterials for support. These methods provide effective treatments for pelvic floor disorders.
What can I expect during recovery after urogynecologic surgery?
After surgery, patients need time to recover. Follow-up appointments are key, and managing any complications or side effects is important.
How do urogynecologists empower patients in their healthcare decisions?
Urogynecologists help patients by explaining complex conditions and treatment options clearly. This enables patients to make informed decisions about their healthcare.
How can I find a urogynecologist?
To find a urogynecologist, ask your primary care doctor or gynecologist for a referral. You can also search online for certified urogynecologists in your area.
What resources are available for patients with pelvic floor disorders?
There are many resources for patients. These include support groups, educational materials, and guidance on managing their conditions. These help women deal with the challenges of pelvic floor disorders.
How should I prepare for a visit to a urogynecologist?
To prepare for a visit, be ready to talk about your symptoms, medical history, and any concerns. Also, ask questions about your condition and treatment options.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/20108394/


































