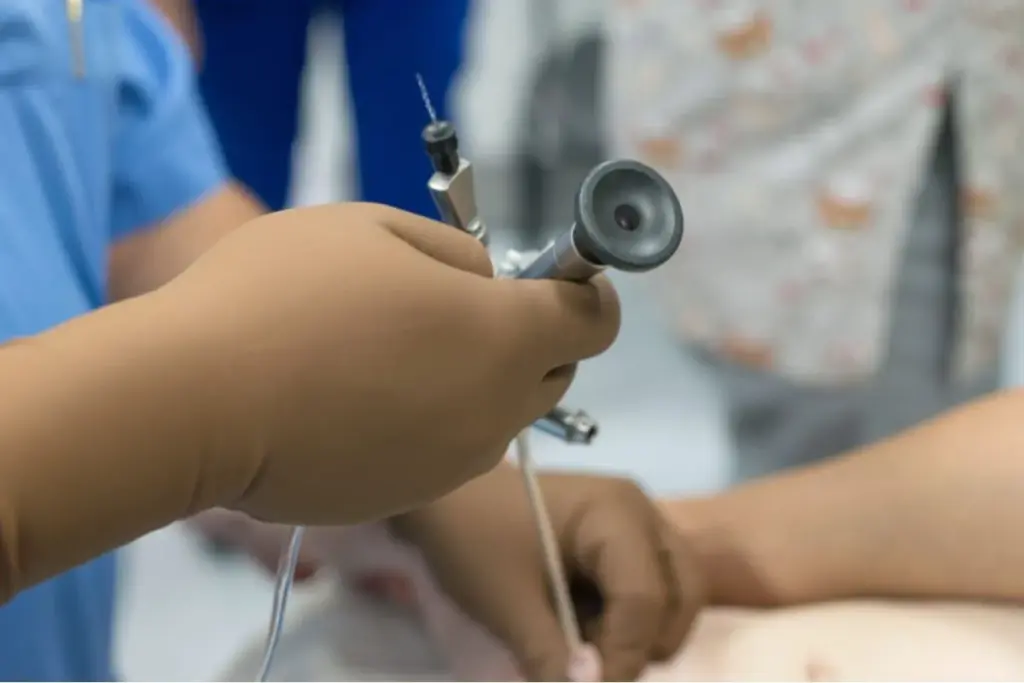
Undergoing a medical procedure can be daunting, especially when it involves sensitive areas like the bladder. A cystoscopy is a procedure that allows doctors to visually examine the inside of the bladder and urethra. For some patients, the prospect of a cystoscopy may raise concerns about pain and discomfort. In some cases, a cystoscopy may be related to more serious conditions that require a bladder removal surgery, also known as radical cystectomy.
This article aims to provide a comprehensive understanding of the cystoscopy procedure, its associated pain levels, and what patients can expect during and after the procedure. We will also touch upon the implications of bladder removal and its impact on a patient’s quality of life.
Key Takeaways
- Understanding what a cystoscopy entails and its purpose.
- Exploring the relationship between cystoscopy and bladder removal surgery.
- Learning about the levels of pain associated with cystoscopy.
- Gaining insights into the recovery process and post-procedure care.
- Understanding the implications of radical cystectomy on life expectancy.
Understanding Cystoscopy: What to Expect
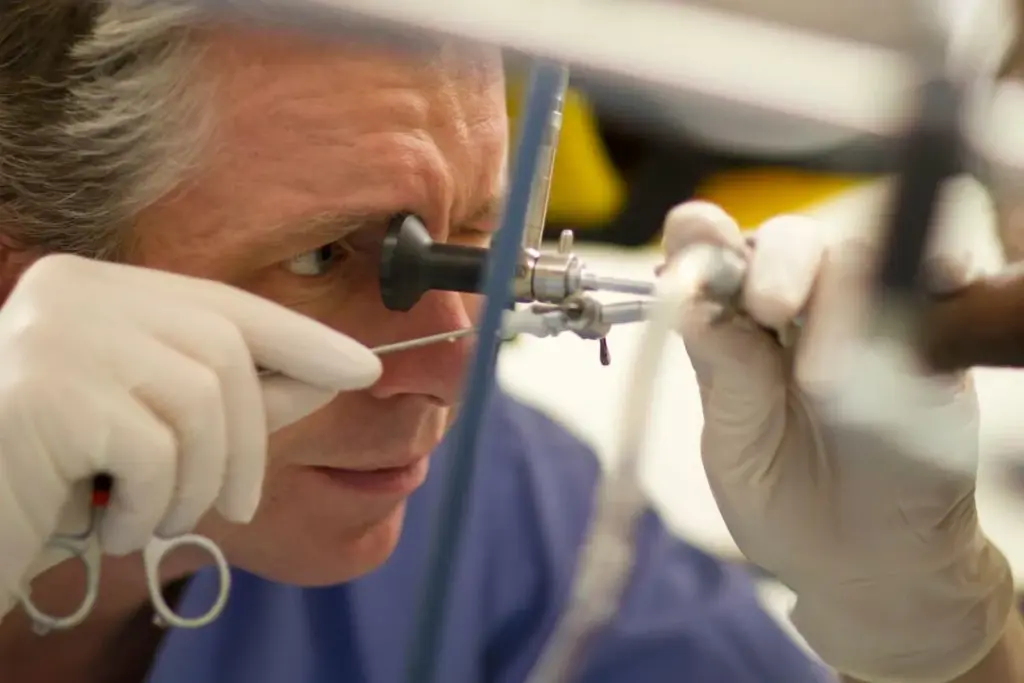
When preparing for a cystoscopy, it’s essential to understand what the procedure entails and its significance in diagnosing urological issues. This understanding can help alleviate anxiety and make the experience less daunting.
Definition and Purpose
Cystoscopy is a medical procedure that involves the use of a cystoscope—a thin, flexible or rigid tube with a camera and light on the end—to visually examine the inside of the bladder and urethra. The primary purpose of a cystoscopy is to diagnose and sometimes treat conditions affecting the urinary tract, much like a cystectomy is the surgical procedure for removing the bladder in cases of severe disease.
The procedure is crucial for identifying abnormalities such as bladder stones, tumors, and inflammation. It allows urologists to directly visualize the inside of the urinary tract, which can be more accurate than imaging tests alone.
The Procedure Explained
During a cystoscopy, the patient is typically positioned on an examination table, often on their back with their legs raised. The urologist then inserts the cystoscope into the urethra and guides it into the bladder. The procedure can be performed under local anesthesia, sedation, or general anesthesia, depending on the patient’s needs and the complexity of the procedure. In some cases, a more extensive bladder operation might be required, but cystoscopy is generally less invasive.
A cystoscopy can be either flexible or rigid. A flexible cystoscopy uses a thinner, more flexible scope, often under local anesthesia, making it a quicker procedure. A rigid cystoscopy might be used for more complex procedures or when a biopsy is required. While it’s different from a radical cystoprostatectomy, which involves removing the bladder, prostate, and surrounding tissues, understanding the differences can help patients appreciate the specific benefits of cystoscopy.
|
Procedure Type |
Characteristics |
Anesthesia Used |
|---|---|---|
|
Flexible Cystoscopy |
Thin, flexible scope; quicker procedure |
Local anesthesia |
|
Rigid Cystoscopy |
Thicker, rigid scope; used for complex procedures or biopsies |
Local anesthesia, sedation, or general anesthesia |
Understanding these aspects of cystoscopy can help patients feel more prepared and less anxious about undergoing the procedure.
Why a Urologist Recommends Cystoscopy
Urologists often recommend cystoscopy as it provides a direct visual examination of the urinary tract, aiding in the diagnosis and treatment of various conditions. This procedure is crucial for patients with urinary tract issues, as it allows for a detailed inspection of the bladder and urethra.
Diagnostic Uses
Cystoscopy is invaluable for diagnosing a range of urinary tract problems. It enables urologists to visually inspect the inside of the bladder and urethra for abnormalities such as bladder stones, tumors, or inflammation. For instance, in cases of suspected bladder cancer, a cystoscopy can help in early detection and assessment of the disease’s extent. Moreover, it aids in understanding the cause of symptoms like hematuria (blood in the urine) or recurrent infections.
During a cystoscopy, the urologist can also perform biopsies if suspicious areas are found. This diagnostic capability is critical for creating an effective treatment plan tailored to the patient’s specific condition.
Therapeutic Uses
Beyond diagnostics, cystoscopy has several therapeutic applications. It can be used to remove bladder stones or tumors, dilate narrowed areas in the urethra (strictures), and inject medications directly into the bladder wall. For patients with bladder cancer, cystoscopy is a key component of surgery for bladder cancer, allowing for the removal of cancerous tissues.
In more severe cases, such as when a patient undergoes a cystoprostatectomy (removal of the bladder and prostate), cystoscopy can be part of the follow-up care to ensure the urethra remains healthy. Understanding that some patients might eventually require a urinary bladder removal, urologists use cystoscopy to monitor the condition and plan accordingly. For those wondering if you can live without a bladder, cystoscopy is part of the broader treatment plan that includes creating a new way for urine to exit the body.
Pain Levels Associated with Cystoscopy
While cystoscopy is generally considered a safe and relatively painless procedure, some discomfort is possible. The level of discomfort or pain experienced can vary based on several factors.
Mild Discomfort vs. Pain
It’s essential to differentiate between mild discomfort and outright pain. Most patients undergo cystoscopy without significant pain, though some may experience a sensation of discomfort or a strong urge to urinate during the procedure. Mild discomfort is common, but severe pain is not typical.
The distinction between discomfort and pain can be attributed to individual pain thresholds and the specific conditions under which the cystoscopy is performed. For instance, the use of local anesthesia can significantly reduce discomfort.
Factors Influencing Pain Perception
Several factors can influence an individual’s perception of pain during cystoscopy. These include:
- Anxiety and Stress Levels: Higher levels of anxiety can heighten the perception of pain.
- Previous Experiences: Past experiences with medical procedures can condition a patient’s response to cystoscopy.
- Use of Anesthesia: The application of local anesthesia can minimize discomfort.
- Individual Pain Threshold: People’s sensitivity to pain varies significantly.
Understanding these factors can help in managing expectations and potentially reducing the discomfort associated with cystoscopy. For some, the fear of pain after bladder surgery or concerns about living without a urinary bladder may add to their anxiety, but these are separate considerations from the procedure itself. For individuals who may eventually require an ostomy bag due to complications, knowing where to find ostomy bag supplies near them can be a relief.
By acknowledging these aspects, healthcare providers can better support their patients through the process, ensuring a more comfortable experience.
Preparing for Your Cystoscopy
Your urologist will provide specific instructions to help you prepare for your cystoscopy. Understanding these guidelines is crucial for a smooth and successful procedure.
Instructions from Your Urologist
Before your cystoscopy, your urologist may give you several instructions to follow. These might include dietary restrictions, adjustments to your medication, and information about arrival times. For instance, if you’re undergoing a cystectomy, a surgical procedure related to your cystoscopy, you may be advised on how to prepare your bowel or adjust your diet accordingly.
Dietary Restrictions: You may be asked to avoid certain foods or drinks for a specified period before the procedure. It’s essential to follow these instructions carefully to ensure your bladder is ready for the examination.
Medication Adjustments: Inform your urologist about all medications you’re currently taking. Some may need to be adjusted or stopped temporarily to avoid complications during the urine bladder operation.
What to Bring to Your Appointment
On the day of your cystoscopy, it’s vital to bring several important items to your appointment. These include your insurance cards, a list of your current medications, and any relevant medical history. Being prepared will help the procedure go as smoothly as possible.
- Insurance Cards: Ensure you have all necessary insurance information readily available.
- List of Medications: A comprehensive list of your medications will help your urologist understand your current regimen.
- Medical History: Bring any relevant medical records or history that could impact your cystoscopy or related procedures like a cystectomy.
For patients who may be undergoing additional treatments or surgeries related to their bladder health, such as a urine bladder operation, understanding the preparation process is crucial. It’s also worth noting that while a cystoscopy is a diagnostic tool, conditions diagnosed through this procedure might require further treatment, such as a cystectomy in cases of bladder cancer. Knowing how long you can live with bladder cancer largely depends on early detection and treatment, which a cystoscopy can facilitate.
|
Preparation Step |
Description |
|---|---|
|
Dietary Adjustments |
Avoid certain foods and drinks as instructed by your urologist. |
|
Medication Management |
Inform your urologist about your medications and follow their guidance on adjustments. |
|
Arrival and Documents |
Arrive on time with all necessary documents, including insurance cards and medical history. |
While preparing for your cystoscopy, you might also want to consider other related needs, such as colostomy bag supplies if you’re undergoing a more extensive surgical procedure. However, for a cystoscopy, the preparation is generally straightforward.
During the Cystoscopy: Step-by-Step
Undergoing a cystoscopy can be a daunting experience, but understanding the procedure can help alleviate anxiety. A cystoscopy involves the insertion of a cystoscope (a thin, flexible or rigid tube with a camera and light) into the bladder to diagnose or treat certain conditions related to the urinary system, including issues that might require the removal of bladder operation or surgical removal of the urinary bladder in severe cases.
Anesthesia Options
There are different anesthesia options available to minimize discomfort during the procedure. These include:
- Local Anesthesia: Numbs the urethra and surrounding area.
- General Anesthesia: Puts the patient to sleep, used for more complex procedures or patient preference.
- Sedation: Helps the patient relax, often used in conjunction with local anesthesia.
For patients with conditions like interstitial cystitis, certain supplements for interstitial cystitis may be recommended before or after the procedure to help manage symptoms.
Length of the Procedure
The length of a cystoscopy can vary depending on its purpose and whether any additional procedures are performed. Generally, it can take anywhere from 15 to 45 minutes. In some cases, if the procedure involves more complex interventions, such as preparing for a remove bladder surgery, the duration may be longer.
Understanding the steps involved and the options available for anesthesia can help patients feel more prepared and less anxious about the procedure.
Post-Procedure Symptoms
Following a cystoscopy, it’s essential to distinguish between normal and abnormal symptoms to ensure proper care. Patients may experience a range of reactions after the procedure, and being aware of what is considered normal can help alleviate concerns.
Normal vs. Abnormal Reactions
Some discomfort after a cystoscopy is normal. Patients may experience mild burning during urination or a frequent urge to urinate. These symptoms are typically temporary and resolve on their own within a few days. However, it’s crucial to monitor the severity of these symptoms. Severe pain, heavy bleeding, or difficulty urinating are not normal and require immediate medical attention.
In some cases, patients may experience more severe reactions, such as infection or significant bleeding. If you notice any signs of infection, such as fever, chills, or unusual discharge, it’s vital to contact your urologist promptly. Understanding the difference between normal and abnormal reactions can help you seek the necessary care in a timely manner.
When to Contact Your Urologist
If you experience any of the following symptoms after a cystoscopy, it’s essential to reach out to your urologist:
- Severe pain that doesn’t improve with medication
- Heavy bleeding or clots in the urine
- Difficulty urinating or inability to urinate
- Fever or chills
- Persistent or severe symptoms
In the context of more extensive surgical procedures, such as partial cystectomy or surgeries involving the removal of the bladder, post-operative care instructions may vary significantly. It’s crucial to follow your urologist’s specific guidance, as these procedures can have different recovery requirements. For instance, patients undergoing a procedure that involves the use of a colostomy pouch will need to follow specific instructions regarding its care and management.
Being informed about what to expect after a cystoscopy and knowing when to seek medical help can make a significant difference in your recovery process. If you’re unsure about any aspect of your post-procedure symptoms or have concerns about your care, don’t hesitate to contact your urologist for guidance.
Managing Pain Post-Cystoscopy
Understanding how to manage pain after a cystoscopy can significantly enhance your recovery experience. While the procedure is generally well-tolerated, some discomfort is common afterward.
Recommended Over-the-Counter Medications
For managing post-cystoscopy pain, over-the-counter (OTC) medications are often recommended. Ibuprofen and acetaminophen are commonly used to alleviate discomfort. It’s essential to follow the dosage instructions provided by your healthcare provider or the medication’s packaging. For instance, men who have undergone bladder surgery might be advised on the suitability of taking Aleve (naproxen) for pain relief.
When considering OTC medications, it’s also crucial to be aware of any potential interactions with other medications you’re currently taking. Consulting with your urologist or pharmacist can provide personalized guidance.
Home Remedies for Comfort
In addition to OTC medications, several home remedies can help alleviate discomfort post-cystoscopy. Drinking plenty of water can help flush out your system, potentially reducing irritation. Applying a warm heating pad to the lower abdomen may also provide relief, though it’s advisable to consult with your healthcare provider first.
Some individuals find that taking a warm bath can be soothing, helping to relax the muscles and reduce discomfort. However, it’s recommended to avoid submerging the genital area in water until your healthcare provider advises it’s safe to do so.
Emotional and Psychological Considerations
It’s natural to feel apprehensive about a cystoscopy, a procedure that examines the bladder. The emotional and psychological aspects of undergoing this procedure are significant, and understanding these factors can help patients prepare better.
Anxiety Before the Procedure
Many patients experience anxiety before a cystoscopy. This anxiety can stem from various sources, including fear of the unknown, concerns about potential pain, or worries about the outcome. As one patient noted,
“I was nervous about what they might find during the procedure.”
Such feelings are common and can be addressed by discussing them with a healthcare provider.
For individuals who have undergone urinary bladder removal or are facing surgery for bladder cancer, the anxiety can be even more pronounced. Understanding the procedure and its implications can help alleviate some of this anxiety.
Coping Strategies
There are several coping strategies that can help manage pre-procedure anxiety. These include:
- Seeking support from family and friends
- Engaging in relaxation techniques, such as deep breathing or meditation
- Visiting resources like the Reservoir Center for Health & Rehabilitation for additional guidance
Moreover, understanding how to manage everyday tasks, such as adjusting the water level in a toilet tank, can provide a sense of normalcy and control. While this may seem unrelated, it’s these small aspects of life that can become significant when facing a medical procedure.
By acknowledging and addressing these emotional and psychological considerations, patients can better cope with the cystoscopy process. It’s about taking control and being prepared, both physically and mentally.
Frequently Asked Questions about Cystoscopy
Clarifying common myths and misunderstandings about cystoscopy can help patients feel more at ease with the procedure. Many individuals have questions about what to expect before, during, and after the examination.
Common Myths and Misunderstandings
One common misconception is that cystoscopy is an extremely painful procedure. While it’s true that some discomfort may be experienced, the use of anesthesia and modern medical techniques have significantly reduced the pain associated with cystoscopy.
Another myth is that cystoscopy is only used for diagnostic purposes. In reality, cystoscopy can also be used for therapeutic interventions, such as removing bladder stones or tumors.
Clarifications from Urologists
Urologists often field questions about the difference between cystoscopy and other procedures like cystectomy, which involves the surgical removal of the bladder. Cystoscopy, on the other hand, is a less invasive procedure that allows for the examination of the inside of the bladder and urethra.
Patients also frequently ask, “What is cystectomy?” Cystectomy is a major surgical procedure where the bladder is removed, often performed to treat bladder cancer. It’s distinct from cystoscopy, which is typically an outpatient procedure.
For female patients, a common question is “what to expect after a catheter is removed.” After a catheter is removed following a cystoscopy, some patients may experience minor discomfort or difficulty urinating initially, but these symptoms usually resolve on their own.
|
Common Questions |
Clarifications |
|---|---|
|
Is cystoscopy painful? |
While some discomfort may occur, anesthesia helps minimize pain. |
|
What is the difference between cystoscopy and cystectomy? |
Cystoscopy is a diagnostic/procedural examination, whereas cystectomy involves surgical removal of the bladder. |
|
What to expect after catheter removal? |
Minor discomfort or difficulty urinating may occur but typically resolves quickly. |
By understanding the answers to these frequently asked questions, patients can better prepare themselves for a cystoscopy and reduce their anxiety about the procedure.
Alternatives to Cystoscopy
While cystoscopy is a valuable diagnostic tool, several alternative methods can be employed to diagnose and monitor urological conditions. These alternatives can be particularly useful for patients who may be anxious about undergoing a cystoscopy or have conditions that make the procedure challenging.
Imaging Techniques
Imaging techniques offer a non-invasive or minimally invasive way to visualize the urinary tract. Ultrasound is one such method that uses high-frequency sound waves to create images of the bladder and kidneys. It’s particularly useful for detecting stones, tumors, or other abnormalities. Another imaging technique is Computed Tomography (CT) scans, which provide detailed cross-sectional images of the urinary tract, helping to identify issues such as blockages or structural anomalies.
Magnetic Resonance Imaging (MRI) is also utilized in some cases, offering a detailed view of the soft tissues within the urinary tract without the need for ionizing radiation. MRI can be especially helpful in staging cancers or assessing complex anatomical issues.
Other Diagnostic Methods
Beyond imaging, other diagnostic approaches can be used depending on the patient’s condition. Urodynamic tests, for example, assess how well the bladder and urethra are performing their job of storing and releasing urine. These tests can help diagnose issues related to incontinence or difficulty urinating.
For patients who have undergone significant urinary tract surgery, such as general surgery bladder removal, understanding the function of any created reservoir is crucial. A reservoir, in this context, refers to a surgically created pouch or container that holds urine. Managing and understanding the implications of such procedures can be complex, and patients often have questions about their quality of life post-surgery, including concerns about activities such as sex with a colostomy bag, although this is more related to ostomy surgery.
“The advancement in diagnostic techniques has significantly improved our ability to manage urological conditions effectively, offering patients a range of options tailored to their specific needs.”
— A leading urologist’s perspective
It’s essential for patients to discuss these alternatives with their healthcare provider to determine the most appropriate diagnostic approach for their specific condition. Factors such as the patient’s overall health, the nature of the suspected condition, and previous medical history will influence this decision.
Patient Experiences: Real Stories
The experience of undergoing a cystoscopy is multifaceted, and patient testimonials shed light on various aspects, including pain levels. By sharing their stories, patients can provide valuable insights into what others might expect during and after the procedure.
Testimonials on Pain Levels
Many patients report that their experience with cystoscopy was less painful than anticipated. For instance, some describe the sensation as a mild discomfort, similar to a urinary tract infection. Others, however, have noted more significant pain, often attributing it to the specific technique used or their individual pain threshold.
A patient who underwent an open cystectomy prior to their cystoscopy noted that the latter was far less invasive and painful in comparison. “The cystoscopy was a breeze,” they said. “I was back to normal in no time, unlike after my surgery.”
Different Perspectives
Patient experiences with cystoscopy can vary widely, influenced by factors such as the reason for the procedure, the urologist’s technique, and the patient’s overall health. For some, the procedure is a straightforward diagnostic tool that provides clarity on their condition. For others, it’s a more complex experience that requires emotional preparation.
One patient likened the experience to “living without a certain level of comfort,” stating that while the procedure was not pleasant, it was necessary for their health. This sentiment is echoed by many who view cystoscopy as a crucial step in addressing their urological issues.
Understanding cystotomy definition and its relation to cystoscopy can also provide context. While the terms are related, they refer to different procedures. Cystotomy involves surgically opening the bladder, whereas cystoscopy is a less invasive examination of the bladder’s interior.
|
Aspect of Experience |
Common Feedback |
|---|---|
|
Pain Level |
Mild discomfort to moderate pain |
|
Recovery Time |
Typically quick, with most returning to normal activities within a day |
|
Emotional Impact |
Varies; some experience anxiety, while others are relieved to have the procedure behind them |
For those preparing for a cystoscopy, understanding the range of patient experiences can be reassuring. While everyone’s story is different, the common thread is that cystoscopy is a valuable diagnostic tool that, despite some discomfort, can significantly contribute to urological health.
Creating a resume of one’s medical experiences, including procedures like cystoscopy, can be helpful for patients when discussing their history with healthcare providers. Using another name for resume, such as a medical history summary, can also be beneficial.
Conclusion: The Importance of Cystoscopy in Urological Health
Cystoscopy plays a vital role in diagnosing and treating various urological conditions, including those related to bladder cancer removal and radical operations. Understanding the procedure and its implications can help alleviate concerns and prepare patients for what to expect.
For individuals dealing with urological issues, a cystoscopy can be a crucial step towards diagnosis and treatment. In some cases, patients may need to use a men’s urine bag post-procedure, and it’s reassuring to know that many individuals can lead active lives even after radical operations. Notably, some people can live without a bladder, albeit with significant lifestyle adjustments.
It’s essential to consult with a urologist to understand the specific needs and risks associated with cystoscopy. By discussing individual circumstances and concerns, patients can make informed decisions about their care. Cystoscopy, when performed by experienced professionals, is a valuable tool in maintaining urological health.
FAQ
What is a cystectomy?
A cystectomy is a surgical procedure that involves the removal of the urinary bladder, often performed to treat bladder cancer.
Can you live without a bladder?
Yes, it is possible to live without a bladder. After a cystectomy, the body will need to adapt to a new way of storing or passing urine, often through the creation of a urinary diversion or an ostomy bag.
What is the life expectancy after bladder removal?
Life expectancy after bladder removal surgery, or radical cystectomy, varies depending on the underlying reason for the surgery, the stage of cancer if applicable, and overall health. It’s best to consult with a healthcare provider for personalized information.
What are the alternatives to cystoscopy?
Alternatives to cystoscopy include various imaging techniques such as ultrasound, CT scans, and MRI, as well as other diagnostic methods like urine tests and biopsies.
How do you manage pain after a cystoscopy?
Pain after a cystoscopy can be managed with over-the-counter pain medications as recommended by a healthcare provider, as well as home remedies like warm baths or heating pads on the lower abdomen.
Can you have sex with a colostomy bag?
Yes, having a colostomy bag does not necessarily preclude sexual activity. However, it’s essential to discuss any concerns or questions with a healthcare provider.
What are the supplements for interstitial cystitis?
Supplements for interstitial cystitis may include substances like glucosamine, chondroitin, and certain herbal remedies, though it’s crucial to consult with a healthcare provider before adding any supplements to your regimen.
How do you adjust the water level in a toilet tank?
Adjusting the water level in a toilet tank typically involves turning a screw or adjusting a float to change the water level, ensuring it’s not too high or too low.
What is a radical cystectomy?
A radical cystectomy is a surgical procedure that involves the removal of the bladder and surrounding tissues, often performed to treat bladder cancer.
Where can I find ostomy bag supplies near me?
Ostomy bag supplies can be found at local pharmacies, medical supply stores, or online retailers that specialize in ostomy care products.
Can I take Aleve after bladder surgery?
It’s generally recommended to consult with a healthcare provider before taking any medication, including Aleve, after bladder surgery, as they can advise on the safest options for pain management.
What is a cystoprostatectomy?
A cystoprostatectomy is a surgical procedure that involves the removal of the bladder and prostate gland, often performed in men to treat bladder cancer or other conditions.
How long can you live with bladder cancer?
The prognosis for bladder cancer varies widely depending on the stage and grade of the cancer, as well as overall health. Early-stage bladder cancer has a more favorable prognosis, while advanced stages can be more challenging to treat.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/25251958/



































