Urology treats urinary tract diseases in all genders and male reproductive issues, covering the kidneys, bladder, prostate, urethra, from infections to complex cancers.
Send us all your questions or requests, and our expert team will assist you.

Diagnosing conditions of the female bladder requires a systematic approach that moves from non invasive clinical assessment to advanced imaging and functional testing. Because bladder symptoms often overlap, a precise diagnosis is essential to guide effective treatment. For instance, urgency caused by infection requires antibiotics, while urgency caused by overactive bladder requires muscle relaxants or behavioral therapy.
The diagnostic pathway begins with a detailed history and physical examination. Urologists and urogynecologists utilize specific questionnaires to quantify symptoms and their impact on quality of life. From there, objective data is gathered through laboratory tests and specialized bladder function tests.
Modern diagnostics focus on understanding both the anatomy and the physiology of the lower urinary tract. This ensures that structural defects (like prolapse) and functional defects (like muscle weakness) are both identified and addressed in the management plan.

The most valuable diagnostic tool is often the patient’s own report. The clinician gathers a detailed history regarding the onset, duration, and triggers of symptoms. Validated questionnaires provide a standardized score for symptom severity.
A bladder diary is a crucial diagnostic record kept by the patient for 2 to 3 days. The patient records the time and volume of every void, fluid intake, and episodes of leakage or urgency. This diary provides objective data on functional capacity and voiding patterns that memory often fails to capture accurately.

A focused physical exam assesses the abdomen, pelvis, and neurological function. The clinician palpates the abdomen for a distended bladder or masses. A pelvic exam is performed to evaluate the health of the vaginal tissues (checking for atrophy) and to assess pelvic floor muscle strength.
The exam specifically looks for pelvic organ prolapse. The patient may be asked to cough or bear down (Valsalva maneuver) while the clinician observes the urethra for leakage, a test known as the cough stress test. This provides immediate confirmation of stress incontinence.

Urinalysis is the fundamental screening test. It detects blood, protein, glucose, and signs of infection like nitrites and leukocytes. It helps rule out common conditions like diabetes (sugar in urine) or kidney disease (protein in urine).
If infection is suspected, a urine culture is performed. This identifies the specific bacteria causing the infection and determines which antibiotics will be effective. This is critical for managing recurrent UTIs and ensuring the correct treatment is prescribed.
PVR measures the amount of urine left in the bladder immediately after the patient urinates. This is typically done using a portable bladder scanner (ultrasound) or by passing a small catheter.
A high PVR indicates incomplete emptying, which can be caused by obstruction or a weak bladder muscle. It is a critical finding because retaining urine predisposes the patient to infections and overflow incontinence. Normal PVR is generally considered less than 50 100 milliliters.
Urodynamics is the gold standard for assessing bladder function. It is a series of tests that evaluate how the bladder stores and releases urine. Small catheters are placed in the bladder and rectum to measure pressures during filling and voiding.
This test can diagnose conditions like detrusor overactivity (bladder spasms), stress incontinence (sphincter weakness), and bladder outlet obstruction. It is often required before surgery to ensure the diagnosis is correct and to predict surgical outcomes.
Cystoscopy allows direct visualization of the lower urinary tract. A thin, lighted tube with a camera (cystoscope) is inserted through the urethra into the bladder. It can be performed with a rigid or flexible scope, usually under local anesthesia.
This procedure is essential for evaluating hematuria, recurrent infections, or suspected structural abnormalities. The clinician can see tumors, stones, inflammation (like in interstitial cystitis), or anatomical defects like diverticula or fistulas.
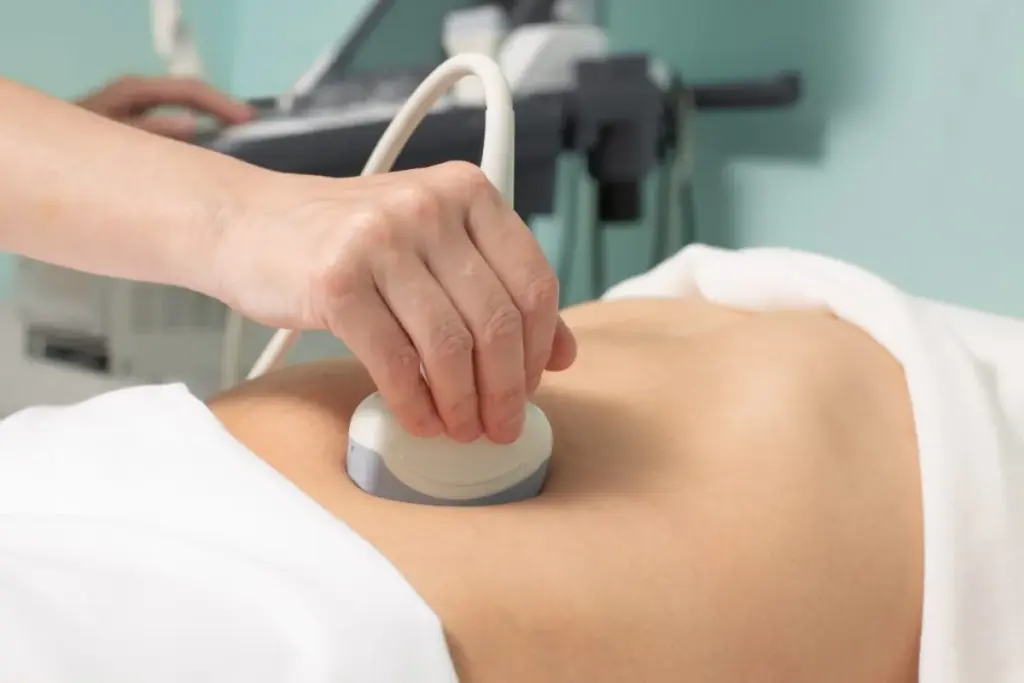
Radiological imaging provides a view of the bladder and surrounding structures. Ultrasound is non invasive and excellent for assessing bladder volume, wall thickness, and the presence of stones or masses. Renal ultrasound often accompanies bladder assessment to ensure the kidneys are protected.
CT scans offer detailed cross sectional images. A CT Urogram is the definitive test for evaluating blood in the urine, visualizing the entire tract from kidneys to urethra to rule out cancer or stones with high sensitivity.
For patients with incontinence, quantifying the leakage is important. A pad test involves wearing a pre weighed absorbent pad for a set period (e.g., 1 hour or 24 hours). The pad is weighed again after the test.
The increase in weight objectively measures the volume of urine lost. This helps classify the severity of incontinence (mild, moderate, severe) and provides a baseline to measure the effectiveness of treatments over time.
Dye tests are used to diagnose fistulas (abnormal connections) between the bladder and the vagina. The patient may take a pill (pyridium) that turns urine orange, or dye may be instilled into the bladder.
If the dye appears on a tampon placed in the vagina, it confirms a fistula. This is a critical diagnostic step for women experiencing continuous, uncontrolled leakage, often following pelvic surgery or obstructed labor.

Though less common now, this test was historically used for Interstitial Cystitis. A potassium solution is instilled into the bladder. In a healthy bladder, the lining protects the nerves, and no pain is felt.
In a bladder with a compromised lining (as in IC), the potassium penetrates the wall and stimulates nerves, causing pain or urgency. While not definitive, a positive test supports the diagnosis of bladder pain syndrome when other causes are ruled out.

Send us all your questions or requests, and our expert team will assist you.
Urodynamics involves placing very small catheters, which can be slightly uncomfortable or embarrassing, but it is generally not painful. The sensation is similar to having a full bladder and needing to urinate. Local anesthetic gel is used to numb the urethra.
Ultrasound is great for seeing the shape and size of the bladder, but it cannot see the inner lining detail. Cystoscopy allows the doctor to see small tumors, inflammation, or stones that ultrasound misses. It is the only way to visually verify the health of the mucosal surface.
A bladder scanner is a portable 3D ultrasound device used specifically to measure the amount of urine in the bladder. It is placed on the lower tummy and gives a quick reading of the volume. It is painless and helps doctors know if you are emptying your bladder completely.
For most office based tests like urodynamics, cystoscopy, or ultrasound, you can eat and drink normally. You do not need to fast unless you are having a procedure under sedation or general anesthesia.
Patients often underestimate or overestimate how often they go or how much they drink. A written diary provides factual data. It helps the doctor see patterns, such as if you drink too much caffeine or if you only leak at certain times, which guides the treatment plan.

 Female Bladder
Female Bladder Female Bladder
Female Bladder Female Bladder
Female Bladder Female Bladder
Female Bladder Female Bladder
Female Bladder Female Bladder
Female Bladder
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)