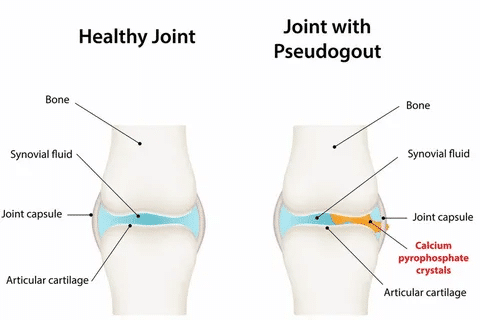
Calcium Pyrophosphate Deposition Disease (CPPD), also known as pseudogout, affects millions globally. It’s a condition where calcium pyrophosphate dihydrate crystals build up in joints. This buildup causes sudden, severe pain and swelling cppd pseudogout.
This condition can be very disabling, mainly for those over 60. If not treated, it can lead to long-term disability. It’s important for both patients and healthcare providers to know about CPPD pseudogout to manage it well.
Key Takeaways
- Calcium Pyrophosphate Deposition Disease is a common cause of inflammatory arthritis in older adults.
- The condition is characterized by the accumulation of calcium pyrophosphate dihydrate crystals in the joints.
- CPPD pseudogout can cause sudden and severe joint inflammation.
- Early diagnosis and treatment are key to prevent lasting disability.
- Understanding the condition is essential for effective management.
What Is CPPD Pseudogout and How Does It Affect the Body?
CPPD, or calcium pyrophosphate deposition disease, is a condition where calcium pyrophosphate dihydrate (CPP) crystals build up in joints. This buildup causes joint pain and swelling, similar to arthritis symptoms.
Defining Calcium Pyrophosphate Deposition Disease
Calcium pyrophosphate deposition disease (CPPD) is a type of crystal arthropathy. It happens when CPP crystals form in the cartilage and synovial tissues of joints. This can cause either acute or chronic joint inflammation.
The formation of CPP crystals is a major factor in CPPD. These crystals form when there’s an imbalance in the body’s normal crystal formation and dissolution processes. Age, metabolic disorders, and joint trauma can lead to this imbalance.
The Medical Abbreviation CPPD Explained
The medical term CPPD stands for Calcium Pyrophosphate Deposition Disease. It’s often used the same as pseudogout, but pseudogout refers to the acute inflammatory arthritis caused by CPPD.
Knowing the abbreviation is key for healthcare providers and patients. It helps in clear communication about the condition, its diagnosis, and treatment options.
How CPPD Differs from Gout and Other Arthritis Types
CPPD is different from gout because of the crystal type. Gout is caused by monosodium urate crystals, while CPPD is caused by calcium pyrophosphate dihydrate crystals. Both can cause acute arthritis but have different causes and risk factors.
- CPPD vs. Gout: Different crystal types (calcium pyrophosphate vs. monosodium urate).
- CPPD vs. Osteoarthritis: CPPD involves crystal deposition, whereas osteoarthritis is a degenerative joint disease.
It’s important to know these differences for proper diagnosis and treatment. We will look at diagnosis and treatment options in the next sections.
Essential Fact #1: CPPD Prevalence Dramatically Increases with Age
As people get older, the chance of getting CPPD goes up a lot. This makes it a big health worry for seniors. We’ll look at how age affects CPPD, why older people are more at risk, and the patterns seen in the U.S. and Europe.
Age-Related Statistics: From 3% in 60s to 50% in 90s
CPPD disease gets more common with age. It hits about 3% of people in their 60s. But by the 90s, it affects around 50% of people. This big jump shows how age is a big risk factor.
Why Older Adults Are More Susceptible to Calcium Crystal Formation
Older adults face a higher risk of calcium crystal formation. This is because of changes in their joints, metabolism, and the buildup of calcium crystals over time. These factors lead to more CPPD in older people.
Epidemiological Patterns in the United States and Europe
In Europe and the U.S., calcium crystal disease affects 4 to 7 percent of adults. Pseudogout, linked to CPPD, affects 7.0% to 13.7% of people. Age is the main risk factor. This shows why doctors need to be aware and make the right diagnosis.
|
Age Group |
Prevalence of CPPD |
|---|---|
|
60-69 years |
3% |
|
70-79 years |
15% |
|
80-89 years |
30% |
|
90+ years |
50% |
Essential Fact #2: The Biological Mechanisms of CPPD Crystal Deposition
Calcium pyrophosphate dihydrate (CPP) crystals build up in joints, causing inflammation. This buildup happens when CPPD crystals gather in the cartilage and tissues around the joints.
The Biochemistry Behind Calcium Pyrophosphate Crystal Development
CPP crystals form when calcium and pyrophosphate ions concentrate in the joint fluid. Abnormal ion homeostasis is key in their creation. We’ll look into how this happens and its effects on CPPD arthropathy.
Several biochemical factors influence CPP crystal development, including:
- Elevated levels of inorganic pyrophosphate
- Abnormalities in calcium metabolism
- Presence of cartilage and synovial tissue degradation products
Why Crystals Form in Joint Cartilage and Synovial Tissues
Crystals form in joint cartilage and synovial tissues because of their unique chemistry. The cartilage matrix is perfect for crystal growth. We’ll talk about what makes these tissues ideal for crystal formation.
Important factors include:
- Local ion concentrations
- Presence of nucleating agents
- Degradation of cartilage components
The Inflammatory Cascade Following Crystal Deposition
When CPP crystals deposit, they start an inflammatory cascade. This cascade is what causes the symptoms of CPPD pseudogout. It involves immune cells and pro-inflammatory mediators. We’ll dive into the steps of this inflammatory process.
The inflammatory response includes:
- Activation of macrophages and neutrophils
- Release of cytokines and chemokines
- Increased vascular permeability
Essential Fact #3: Recognizing CPPD Pseudogout Symptoms and Attack Patterns
Knowing the symptoms of CPPD pseudogout is key for quick diagnosis and treatment. We’ll look at the signs of an acute flare, the joints most often affected, and the differences between acute and chronic forms.
Classic Signs of an Acute CPPD Flare
An acute CPPD flare starts suddenly with joint pain, swelling, redness, and warmth. The pain is often severe and makes moving the joint hard. These symptoms can look like other types of arthritis, making it hard to diagnose.
Some people may also feel feverish and tired. CPPD is more common in people over 60, with 30 to 50 percent of cases happening after age 85.
Most Commonly Affected Joints in CPPD Arthropathy
The knee is the most common joint affected by CPPD. But it can also affect other joints like the wrist, toe, shoulder, and hip. The joints affected can vary from person to person.
|
Joint |
Frequency of Involvement |
|---|---|
|
Knee |
Most common |
|
Wrist |
Common |
|
Toe |
Less common |
|
Shoulder |
Less common |
|
Hip |
Less common |
Acute vs. Chronic Manifestations of Calcium Crystal Disease
CPPD can show up as sudden attacks or as chronic joint pain. Acute attacks start suddenly, while chronic CPPD causes ongoing pain and stiffness. The chronic form can also cause degenerative changes in the joints.
It’s important to know the difference between acute and chronic CPPD to choose the right treatment. We’ll talk about treatment options next.
Essential Fact #4: Medical Conditions and Risk Factors Associated with CPPD
Knowing the risk factors for CPPD is key for early diagnosis and treatment. Certain health conditions make it more likely to get calcium pyrophosphate deposition arthropathy. It’s important to manage these factors well.
Metabolic Disorders Linked to Calcium Pyrophosphate Arthropathy
Metabolic disorders are a big deal in CPPD. Conditions like hyperparathyroidism, hypomagnesemia, and hemochromatosis raise the risk of CPPD. These disorders mess with the body’s mineral balance, causing crystals to form in joints.
For example, hyperparathyroidism can upset calcium levels, leading to crystal formation. Low magnesium, or hypomagnesemia, also increases CPPD risk. And iron overload from hemochromatosis is another factor.
Genetic Predisposition and Familial CPPD
Genetics also matter in CPPD. Familial CPPD is a rare condition passed down through families. Certain genetic mutations can make someone more likely to get CPPD.
Families with CPPD history often see symptoms early and in many joints. Knowing the genetic link can help spot at-risk individuals and prevent CPPD.
Joint Trauma and Its Relationship to Crystal Formation
Joint trauma is a big risk factor for CPPD. Injury can start an inflammatory response, making it easier for crystals to form. Studies show injured joints are more likely to get CPPD.
The exact way trauma leads to CPPD isn’t clear. But, it’s thought that the inflammation after injury helps crystals form.
Other Medical Conditions That Increase CPPD Risk
Other health issues can also raise CPPD risk. These include osteoarthritis, hypothyroidism, and diabetes mellitus. These conditions can make diagnosing and treating CPPD harder.
It’s important for doctors to know about these connections. This way, they can better care for patients with CPPD.
Essential Fact #5: Diagnostic Approaches for Calcium Crystal Disease
Diagnosing calcium pyrophosphate deposition disease needs advanced methods. It involves clinical checks, imaging, and lab tests. These steps help spot CPPD pseudogout and rule out other causes of symptoms.
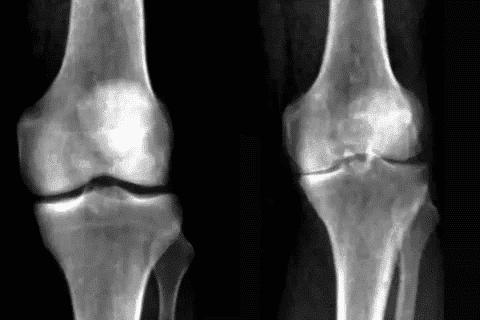
Imaging Techniques for Identifying CPPD Deposits
Imaging is key in diagnosing CPPD. The main imaging methods are:
- X-rays: To find calcification in cartilage, known as chondrocalcinosis.
- Ultrasound: To spot calcium pyrophosphate crystals in joints.
- CT scans: To see detailed images of joint calcification.
- MRI: To check soft tissue and joint damage.
Joint Fluid Analysis and Crystal Identification
The best way to diagnose CPPD is finding CPP crystals in joint fluid. This process includes:
- Collecting synovial fluid from the joint.
- Looking at it under a microscope to find CPP crystals.
Testing the joint fluid is key to confirm CPPD crystals. It helps tell CPPD apart from other arthritis types.
Laboratory Tests and Their Significance
Labs help confirm the diagnosis and rule out other conditions. Tests might include:
|
Test |
Significance |
|---|---|
|
Serum calcium and phosphate levels |
To check for metabolic disorders linked to CPPD. |
|
Inflammatory markers (e.g., ESR, CRP) |
To see how much inflammation there is. |
|
Synovial fluid analysis |
To confirm CPP crystals are present. |
By using imaging, joint fluid tests, and lab tests, doctors can accurately diagnose CPPD. They can then create a good treatment plan.
Comprehensive Treatment Options for CPPD Arthropathy
CPPD arthropathy treatment aims to ease symptoms and lower inflammation. It combines medicine and non-medical ways to manage CPPD pseudogout.
Medications for Managing Acute CPPD Flares
Medicines are key in treating acute CPPD flares. Nonsteroidal anti-inflammatory drugs (NSAIDs) help reduce inflammation and pain. Colchicine is used when NSAIDs can’t be taken.
Corticosteroids are an option for those who can’t use NSAIDs or colchicine. They can be taken by mouth or injected into the joint. This gives quick relief from inflammation and pain.
|
Medication |
Use in CPPD |
Benefits |
|---|---|---|
|
NSAIDs |
First-line treatment for acute flares |
Reduces inflammation and pain |
|
Colchicine |
Alternative for NSAID-intolerant patients |
Effective for acute CPPD attacks |
|
Corticosteroids |
Oral or intra-articular for severe cases |
Rapid relief from inflammation and pain |
Long-term Therapeutic Strategies
Long-term CPPD management includes preventing future flares and slowing disease growth. Magnesium supplements are recommended to reduce calcium pyrophosphate crystals.
It’s also important to manage underlying conditions like hyperparathyroidism or hemochromatosis. Treating these can lessen CPPD symptoms.
Joint Aspiration and Injection Therapies
Joint aspiration removes fluid from the affected joint. This can lessen pain and swelling. Intra-articular corticosteroid injections are given after aspiration to treat the joint directly.
When Surgical Intervention May Be Necessary
In severe cases, surgery might be needed. Joint replacement surgery is considered for those with chronic CPPD damage.
Arthroscopic surgery can remove crystals and damaged tissue. This can improve joint function and reduce symptoms.
Living with CPPD: Practical Management and Self-Care Approaches
Managing Calcium Pyrophosphate Deposition Disease (CPPD) needs a full plan. This includes practical steps and self-care. Living with CPPD can be tough, but the right methods can greatly improve life quality.
Joint Protection Techniques for Daily Activities
Protecting joints is key for CPPD patients. Simple changes in daily life can help a lot. For instance, using ergonomic tools, resting joints often, and keeping a healthy weight can ease joint stress.
We suggest patients work with an occupational therapist. They can create joint protection plans tailored to each person. This might include learning new ways to do tasks, like using devices for opening jars or holding things.
|
Joint Protection Technique |
Benefit |
|---|---|
|
Using ergonomic tools |
Reduces strain on joints |
|
Taking regular breaks |
Prevents fatigue and pain |
|
Maintaining a healthy weight |
Decreases pressure on joints |
Dietary Considerations for CPPD Patients
Diet is important for CPPD management. There’s no special “CPPD diet,” but eating well is key. Focus on fruits, veggies, and whole grains for better health.
“A well-balanced diet is essential for managing CPPD. Foods rich in omega-3 fatty acids, such as salmon and sardines, can help reduce inflammation.”
Some foods might make symptoms worse. Keeping a food diary can help find these foods.
Appropriate Exercise Recommendations and Limitations
Exercise is vital for CPPD management. Gentle activities like swimming or cycling keep joints moving without too much strain.
It’s important to balance activity with rest. Too much activity can lead to flares. So, listen to your body and adjust your exercise plan.
- Gentle exercises like yoga or tai chi can improve flexibility and balance.
- High-impact activities should be avoided to prevent joint damage.
- Regular exercise can help maintain a healthy weight, reducing pressure on joints.
Pain Management Strategies Between Flares
Managing pain between flares is key for a good life. This might include medicine, lifestyle changes, and alternative therapies.
Some find relief in alternative therapies like acupuncture or physical therapy. These can help with chronic pain and improve well-being.
By using these practical and self-care methods, CPPD patients can better handle their symptoms. This can greatly improve their life quality.
Conclusion: Navigating Life with CPPD and Future Research Directions
Understanding CPPD, or calcium pyrophosphate deposition disease, is key to managing it well. This condition, also known as CPPD pseudogout, is marked by calcium pyrophosphate crystals in joints. These crystals cause various symptoms and problems.
Research is ongoing to understand CPPD better and find new treatments. By studying how these crystals form and identifying risk factors, we can tackle this condition more effectively. New treatments could improve life for those with CPPD pseudogout.
As we learn more about CPPD, both healthcare providers and patients will benefit. Keeping up with the latest CPPD research and treatments is important. This way, we can offer the best care to those with CPPD.
FAQ
What is CPPD pseudogout?
CPPD pseudogout, also known as calcium pyrophosphate deposition disease (CPPD), is a type of arthritis. It happens when calcium pyrophosphate (CPP) crystals build up in the joints. This leads to inflammation and symptoms similar to gout.
What does CPPD stand for in medical terms?
CPPD stands for Calcium Pyrophosphate Deposition disease. It’s a condition where calcium pyrophosphate crystals deposit in the cartilage and synovial tissues of joints.
How does CPPD differ from gout?
CPPD differs from gout in the type of crystals that accumulate in the joints. Gout is caused by monosodium urate crystals. CPPD is caused by calcium pyrophosphate crystals.
What are the symptoms of CPPD pseudogout?
Symptoms of CPPD pseudogout include sudden onset of joint pain, swelling, redness, and warmth. These symptoms typically affect the knee, wrist, or other joints.
How is CPPD diagnosed?
CPPD is diagnosed through a combination of imaging techniques, such as X-rays or ultrasound. Joint fluid analysis to identify CPP crystals is also used. Laboratory tests help rule out other conditions.
What are the treatment options for CPPD arthropathy?
Treatment options for CPPD arthropathy include medications to manage pain and inflammation. Joint aspiration and injection therapies are also used. In some cases, surgical intervention is necessary.
Can CPPD be managed through lifestyle changes?
Yes, CPPD can be managed through lifestyle changes. This includes joint protection techniques, dietary considerations, and appropriate exercise recommendations.
Is CPPD associated with other medical conditions?
Yes, CPPD is associated with various medical conditions. These include metabolic disorders, genetic predisposition, and joint trauma.
How does age affect the prevalence of CPPD?
The prevalence of CPPD increases significantly with age. It affects up to 50% of individuals in their 90s.
What is the role of genetics in CPPD?
Genetic predisposition plays a role in CPPD. Some families show a higher incidence of the condition.
Can CPPD be treated with medication?
Yes, medications such as NSAIDs, colchicine, and corticosteroids can help manage acute CPPD flares. They reduce inflammation.
References
Valuable 5 Essential Facts About CPPD Pseudogout https://www.ncbi.nlm.nih.gov/books/NBK540151



































