
Every year, thousands of lives are saved thanks to CPR. Knowing vital signs and how to check for life signs is key in emergencies. We offer a detailed guide on these important topics.
The SAAmplify-αSYN test shows how vital accurate diagnosis is in healthcare. It’s just as important to know when CPR is needed and how it works.
Knowing how to tell if someone needs CPR can save lives. We look at the role of vital signs in CPR. We also give a step-by-step guide on checking for life signs, making sure resuscitating life solutions work well.
Key Takeaways
- Understanding vital signs is key in emergencies.
- Knowing when CPR is needed can save lives.
- Good CPR is essential for saving lives.
- Checking for life signs is a vital skill.
- Accurate diagnosis is vital for patient care.
Understanding the Importance of Checking for Signs of Life
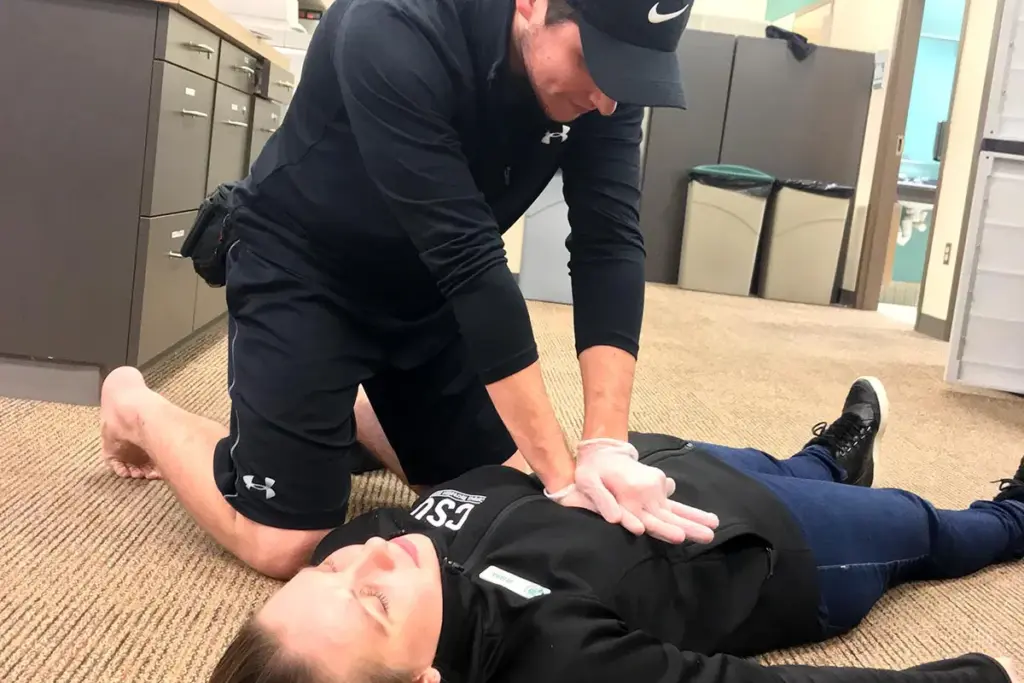
Quickly recognizing vital signs is crucial in medical emergencies. It helps decide the right action to take. Quick medical help can greatly improve survival chances and outcomes.
What Constitutes a Medical Emergency
A medical emergency happens when someone’s life is at risk fast. It’s urgent to act quickly to stop things from getting worse or to save a life. Examples include heart attacks, severe injuries, and sudden illnesses.
The Golden Minutes in Emergency Response
The first minutes after a heart stop are called the “golden minutes.” Quick action here can greatly affect survival and recovery. Studies show timely action can boost survival chances by up to 50%.
Impact of Early Recognition on Survival Rates
Spotting medical emergencies early and acting fast can greatly increase survival rates. Every minute without CPR and defibrillation cuts survival chances by 7-10%. So, knowing vital signs and acting quickly is vital.
|
Time to Intervention |
Survival Rate |
|---|---|
|
Within 1 minute |
90% |
|
Within 3 minutes |
70% |
|
Within 5 minutes |
50% |
By recognizing signs of life early and acting fast, we can greatly improve patient outcomes in emergencies.
The Primary Vital Signs in CPR Assessment
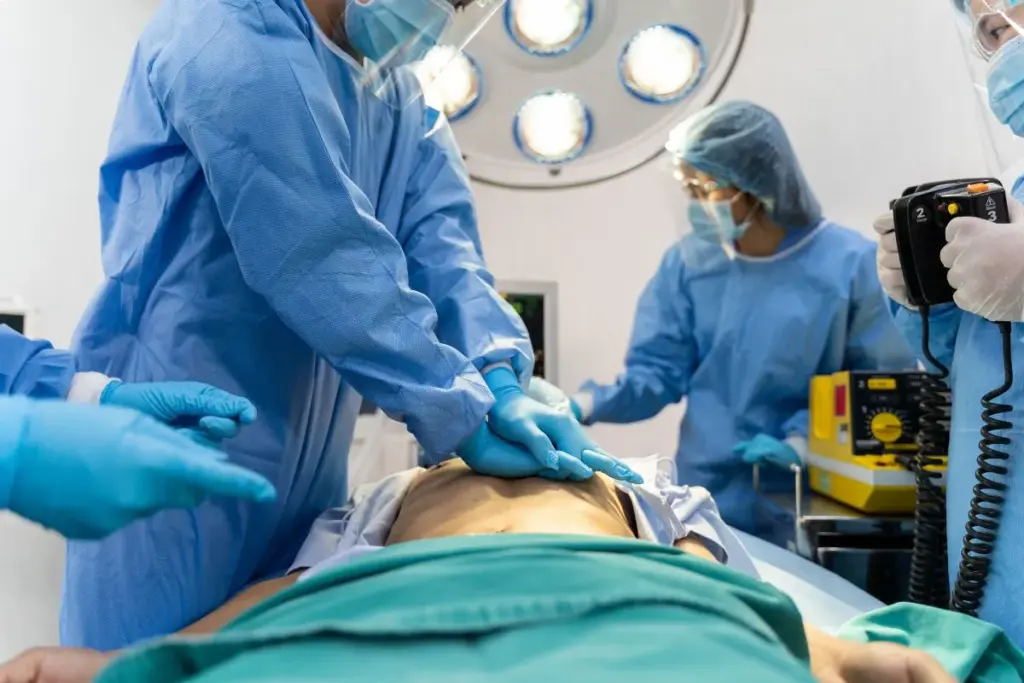
When doing CPR, checking primary vital signs is key. It helps us understand the patient’s health and if CPR is working. We look at consciousness, breathing, pulse, and other important signs.
Consciousness Assessment Techniques
We check how awake a patient is by using words and touch. If they don’t react or only respond to pain, they’re not fully awake.
Breathing Evaluation Methods
Checking how a patient breathes is very important. We look for normal breathing and check for airway blockages. We use the “look, listen, feel” method to see if the chest moves, listen for sounds, and feel for air.
Pulse Detection Locations and Procedures
Finding a pulse is a big part of CPR. We usually check the pulse in the neck. To do this, we feel the carotid artery with our fingers.
Body Temperature and Skin Color Assessment
Looking at body temperature and skin color tells us a lot. We watch for signs of too hot or too cold and check the skin color. This helps us see if blood is flowing well.
|
Vital Sign |
Assessment Method |
Normal Finding |
|---|---|---|
|
Consciousness |
Verbal commands and physical stimuli |
Responsive to verbal commands |
|
Breathing |
“Look, listen, feel” approach |
Normal rate and depth of breaths |
|
Pulse |
Checking carotid pulse |
Regular pulsations |
|
Body Temperature and Skin Color |
Observation and palpation |
Normal body temperature, normal skin color |
Step-by-Step Guide to Checking for Signs of Life
In emergency situations, knowing if someone is alive can save lives. When someone is not responding, it’s key to check their condition carefully. This helps us give the right care.
Initial Scene Assessment for Safety
First, we make sure the area is safe before we get close to the victim. We look out for dangers like cars, falling things, or electrical risks. Keeping the scene safe is very important to avoid more harm.
Ensuring Your Safety First
Our safety is the first thing we think about so we can help others well. We need to know what’s around us and any dangers. This way, we can help without getting hurt.
Approaching the Victim Properly
After checking the area is safe, we go to the victim calmly. We introduce ourselves and try to wake them up by speaking loudly and gently shaking their shoulders. This helps us see if they are awake or not.
The “Look, Listen, Feel” Approach
To check if the victim is okay, we use the “look, listen, feel” method. We look for their chest to rise, listen for breathing sounds, and feel for air on our cheek. This tells us a lot about their health.
By following these steps, we can figure out if CPR is needed. We can then help the victim until doctors get there.
The CAB Protocol: Circulation, Airway, Breathing
Effective CPR uses the CAB protocol to check circulation, airway, and breathing. This method is key in CPR, focusing on these areas one by one. It ensures victims get the best care in cardiac emergencies.
Checking Circulation: Finding the Carotid Pulse
First, we check circulation by finding the carotid pulse. This is a vital step to see if the heart is pumping blood. To find it, we place the victim on their back on a firm surface.
Then, we locate the larynx (Adam’s apple) with our fingers. We slide our fingers into the groove between the larynx and the neck muscles. Here, we can feel the carotid pulse. It’s important to check for no more than 10 seconds to avoid delaying CPR.
Assessing Airway Patency and Clearing Obstructions
After checking circulation, we check the airway. We tilt the victim’s head back and lift the chin to open the airway. Then, we look in the mouth for any obstructions and remove them if we find any.
If the victim is not breathing, we start CPR. It’s vital to make sure the airway is clear for effective ventilation.
Evaluating Breathing Patterns and Depth
We then check for normal breathing patterns and depth. We listen for breath sounds and feel for air on our cheek. If the victim is not breathing or breathing abnormally, we start CPR.
Normal breathing is regular and unlabored. Abnormal breathing can be a sign of cardiac distress.
Updated Guidelines vs. Traditional ABC Approach
The CAB protocol is a change from the traditional ABC approach. The updated guidelines put circulation first because cardiac arrest is often the main cause of emergencies needing CPR. By starting with chest compressions, we aim to keep blood flowing and increase the chances of successful resuscitation.
|
Aspect |
CAB Protocol |
Traditional ABC Approach |
|---|---|---|
|
Sequence |
Circulation, Airway, Breathing |
Airway, Breathing, Circulation |
|
Priority |
Starts with chest compressions |
Starts with airway management |
|
Rationale |
Prioritizes circulation to address cardiac arrest |
Focuses on airway management first |
Vital Signs CPR: Monitoring During Resuscitation
During CPR, it’s important to keep an eye on vital signs. This helps ensure the best results. We stress the need to check the patient’s vital signs regularly.
Pulse Checks During CPR: Timing and Technique
Pulse checks are a key part of CPR monitoring. We suggest checking the carotid pulse every 2 minutes, following the latest guidelines. To do this, find the carotid pulse on the neck side closest to you. Use your index and middle fingers to feel for it. Getting the pulse right is key to knowing if CPR is working.
Assessing Breathing During Compression Pauses
Checking breathing during CPR is important. Look for chest rise and fall during pauses. Also, listen for breath sounds and feel for air on your cheek. Good ventilation is essential for keeping oxygen levels up.
Signs of Circulation Return
Signs that CPR is working include a palpable pulse, better skin color, and sometimes regaining consciousness. We say that spotting these signs is vital. They help us adjust CPR and might mean we can stop CPR if the patient gets better.
Team Communication During Vital Signs Monitoring
Good team communication is key during CPR. It’s important to share clearly about the patient’s vital signs, CPR success, and any changes.
“Clear and concise communication among team members is the backbone of effective CPR,”
as studies on CPR best practices show.
By paying attention to these monitoring aspects, we can boost the chances of successful CPR. This leads to better outcomes for patients.
How to Recognize When CPR is Needed
Knowing when to start CPR can save lives. CPR is a lifesaving technique for emergencies like heart attacks or near drowning. It’s used when someone’s breathing or heartbeat stops.
Identifying Cardiac Arrest vs. Heart Attack
It’s important to know the difference between cardiac arrest and heart attack. Both need quick medical help but have different treatments. A heart attack blocks blood flow to the heart, damaging the muscle. On the other hand, cardiac arrest is when the heart suddenly stops beating.
A heart attack may cause chest pain and shortness of breath. But the person is usually awake. Cardiac arrest, though, makes someone lose consciousness and stop breathing.
Differentiating from Seizures and Fainting
Seizures and fainting can look like cardiac arrest because they both cause loss of consciousness. But they have different causes and treatments. Seizures are brain electrical activity issues, while fainting is a temporary loss of consciousness from lack of blood flow.
Seizures cause convulsions, but fainting doesn’t. Always check for a pulse and breathing, as they can lead to cardiac arrest.
Decision-Making Process for Initiating CPR
Deciding to start CPR depends on the victim’s condition. If someone is unresponsive, not breathing, or breathing abnormally, and has no pulse, start CPR right away.
- Check the scene for safety
- Check the victim for responsiveness
- Call for emergency medical help
- Begin CPR with 30 chest compressions followed by two rescue breaths
When to Call for Advanced Medical Help
After starting CPR, call for advanced medical help. If alone, call after starting CPR. If with someone, one person calls while the other does CPR.
Advanced medical help is needed because CPR is only a temporary fix. It keeps blood flowing until medical professionals can provide more care, like defibrillation.
Signs of Effective CPR Performance
Effective CPR is key to saving lives. It’s important to watch how the victim reacts to CPR.
Chest Compression Quality Indicators
Good chest compressions are vital in CPR. We check for several things to make sure they’re done right. These include:
- Depth and Rate: Compressions should be at least 2 inches deep and at a rate of 100-120 compressions per minute.
- Complete Chest Recoil: Allowing the chest to return to its normal position after each compression.
- Minimal Interruptions: Minimizing pauses in chest compressions to ensure continuous blood circulation.
Victim Response Signs During Resuscitation
We watch for signs of response during CPR. These signs can include:
- Return of Spontaneous Circulation (ROSC): Indicated by a palpable pulse or improved hemodynamic stability.
- Improved Breathing: The victim may start showing signs of normal or spontaneous breathing.
- Consciousness: The victim may regain consciousness or show signs of responsiveness.
Using Feedback Devices for Quality CPR
Feedback devices are key for quality CPR. They give real-time feedback on:
- Compression Depth and Rate: Ensuring that compressions meet the recommended guidelines.
- Chest Recoil: Monitoring whether the chest is fully recoiling after each compression.
Capillary Refill and Other Circulation Indicators
We also watch other signs of circulation. These include:
- Capillary Refill: Checking the time it takes for color to return to the skin after applying pressure.
- Color and Temperature: Observing improvements in skin color and temperature, indicating better circulation.
By monitoring these signs and using feedback devices, we can make sure CPR is done right. This increases the chances of a successful resuscitation.
When to Stop CPR: Recognizing Signs of Life Return
Knowing when to stop CPR is key to saving lives. It’s all about paying close attention to the patient’s vital signs. This is a critical part of emergency care.
Spontaneous Breathing: What to Look For
Spontaneous breathing is a big sign of recovery. Look for regular, easy breaths. If the patient is breathing normally, they might be getting better.
It’s important to tell the difference between agonal respirations and real breathing. Agonal respirations are gasping breaths that happen during cardiac arrest. Real breathing is steady and effective.
- Observe the chest for rise and fall.
- Listen for breath sounds.
- Feel for air on your cheek.
Pulse Return: Assessment Locations
Another important sign is a palpable pulse. We check for a pulse in the carotid artery. This is on either side of the neck.
- Position your fingers on the patient’s Adam’s apple.
- Slide your fingers toward you, into the groove between the trachea and the sternocleidomastoid muscle.
- Feel for a pulse for at least 5 seconds but no more than 10 seconds.
Other Signs of Circulation and Consciousness
Other signs can also show recovery. These include:
- Return of consciousness or responsiveness.
- Movement or spontaneous limb movement.
- Normal skin color and temperature.
These signs together mean CPR can stop.
When to Continue Despite Apparent Recovery
Even if it seems like the patient is recovering, CPR might need to keep going. If the patient stays unresponsive or shows distress, keep doing CPR until medical help arrives.
Always stay alert and don’t stop CPR unless you see clear, lasting signs of life.
Age-Specific Considerations for Checking Vital Signs
Checking vital signs changes a lot with age. This means CPR and vital sign checks need to be different for each age group.
Age-specific CPR is key for saving lives. From babies to the elderly, each age needs its own CPR method.
Infants (Under 1 Year): Special Techniques
Infants need gentle but firm checks of vital signs. Instead of the carotid pulse, check the brachial pulse. Watch the chest for breathing.
“The key to successful infant CPR lies in the subtleties of the technique,” as emphasized by pediatric CPR guidelines. The rate and depth of compressions, as well as the method of giving breaths, are adapted to the infant’s physiology.
Children (1-8 Years): Adaptation of Adult Methods
Children’s CPR is a mix of infant and adult methods. Use one-hand or two-hand compressions based on the child’s size and the rescuer’s ability.
Checking vital signs in children needs a careful balance. Adjust the compression rate and breath ratio based on the child’s age and size.
Adults and Adolescents: Standard Procedures
Adults and teens follow standard CPR. Check the carotid pulse and listen for breath sounds and feel for air on the cheek.
The focus is on high-quality CPR. Aim for the right compression depth and rate, and proper ventilation.
Elderly Patients: Accounting for Physical Differences
Elderly patients have unique needs for CPR. Consider their frailty and rib fragility. Make necessary adjustments to avoid injury.
When checking vital signs in the elderly, think about their health and any conditions that might affect CPR response.
Technology and Tools for Vital Signs Assessment
Technology has changed how we check vital signs during CPR. New tools make checking vital signs more accurate and effective.
AEDs and Their Role in Assessment and Treatment
Automated External Defibrillators (AEDs) are key in heart emergencies. They check the heart’s rhythm and give a shock if needed. AEDs help assess the heart and guide treatment.
AEDs are easy to use. Even those with little training can operate them. They guide users with voice prompts and visual instructions during emergencies.
Pulse Oximetry and Oxygen Saturation Monitoring
Pulse oximetry checks blood oxygen levels and pulse rate without needles. It’s key for checking breathing and oxygen levels.
Pulse oximeters are used in clinics and during CPR. They show oxygen levels in real-time. This helps see if CPR is working and guides treatment.
Advanced Monitoring Equipment in Professional Settings
In hospitals, advanced tools track vital signs in detail. They monitor heart rate, blood pressure, and breathing. This gives a full picture of a patient’s health.
These tools are great in hospitals where constant monitoring is needed. They connect to central stations. This lets doctors quickly respond to changes in a patient’s health.
Smartphone Apps and Consumer Technology for Vital Signs
Smartphone apps and devices let people check vital signs at home. Apps track heart rate and rhythm using phone sensors or devices.
These tools aren’t a full replacement for medical gear. But they offer useful info and encourage seeking medical help if needed. Always use them wisely and talk to doctors for accurate care.
Common Mistakes When Checking for Signs of Life
Knowing and avoiding common mistakes in CPR can greatly improve outcomes. The accuracy of vital sign assessment is key in CPR. It helps decide the right action to take.
Pulse Check Errors: Too Brief or Wrong Location
One major error in CPR is wrong pulse assessment. Checking for a pulse for too short a duration or in the wrong location can lead to wrong conclusions. The carotid pulse is best for pulse checks because it’s easy to find and reliable.
Breathing Assessment Pitfalls: Missing Subtle Signs
Checking breathing during CPR can be tough, and missing subtle signs of breathing is common. It’s important to look, listen, and feel for breathing. Agonal respirations can look like normal breathing.
Misinterpreting Agonal Respirations as Normal Breathing
Agonal respirations are abnormal breathing in cardiac arrest. Misinterpreting these as normal breathing can delay CPR. It’s key to know agonal respirations are a sign of cardiac distress, not normal breathing.
Delaying CPR Due to Assessment Hesitation
Delaying CPR because of hesitation can be deadly. Prompt action is essential in cardiac arrest. Any hesitation can lower the chances of successful resuscitation.
By understanding these common mistakes, CPR performers can improve their skills. This can increase the victim’s chances of survival.
Legal and Psychological Aspects of Emergency Response
When we do CPR, we face legal and psychological challenges. We use our medical skills and also think about legal and mental health issues.
Good Samaritan Laws and Legal Protection
Good Samaritan laws protect those who help in emergencies. These laws vary but usually shield from lawsuits unless there’s clear negligence. Knowing these laws can help people act in emergencies without fear.
In the U.S., all states have Good Samaritan laws, but they’re not all the same. It’s key for responders to know their local laws to understand their protection.
Mental Preparation for Emergency Situations
Being mentally ready is key for emergency response. It’s not just about knowing CPR but also being ready to act under stress. Training with simulations can boost confidence. Regular practice is vital for staying ready.
Knowing CPR’s mental toll can also help. This knowledge helps responders seek help if they need it after an event.
Dealing with Psychological Impact After Performing CPR
Doing CPR can affect responders’ minds, from feeling good to feeling anxious or guilty. Recognizing these effects is the first step to handling them. Responders should talk to peers, professionals, or support groups if they’re struggling.
More organizations are now focusing on mental support for responders. They offer debriefing and counseling after big incidents.
Documentation and Reporting Requirements
After CPR, it’s important to document and report what happened. This includes the incident details, CPR steps, and any other actions. Good documentation is key for legal protection and to improve future responses. Reporting should be accurate and on time.
Responders need to know their local reporting rules. Reports should cover the incident time, victim’s state, CPR method, and any tools used.
Training and Certification for Proper Vital Signs Assessment
Learning to assess vital signs well needs the right training and certification. This is key for doing CPR right. We’ll look at BLS certification, ACLS training, why refresher courses are important, and compare online and in-person learning.
Basic Life Support (BLS) Certification Options
BLS certification is a must for healthcare workers. It teaches the basics of CPR, including checking vital signs. We have many BLS courses to fit your needs and schedule. They mix hands-on practice with theory.
- Course formats: in-person, online, and blended
- Certification validity: typically 2 years
- Target audience: healthcare professionals, including nurses and doctors
Advanced Cardiovascular Life Support (ACLS) Training
ACLS training goes beyond BLS. It teaches advanced ways to handle heart emergencies. ACLS also covers detailed vital signs checks during CPR.
Key components of ACLS training:
- Advanced airway management
- Cardiac rhythm interpretation
- Pharmacological interventions
- Team dynamics and communication
Refresher Training Importance and Frequency
Refresher training keeps CPR and vital signs skills sharp. The American Heart Association says update CPR skills every 2 years. It helps by:
- Reinforcing what you know
- Keeping skills up to date
- Boosting confidence in emergencies
Online vs. In-Person Training Effectiveness
Online and in-person training each have their own perks. Online is flexible and easy, while in-person gives hands-on practice. We suggest a mix of both for the best learning.
In summary, getting the right training and certification is key for good vital signs checks during CPR. By picking the right courses and keeping up with refresher training, healthcare pros can be ready for emergencies.
Conclusion: The Critical Role of Accurate Life Signs Assessment
Getting vital signs right is key in CPR and emergency care. It helps save lives and improve patient care. We’ve talked about why checking vital signs matters, CPR steps, and how to act in emergencies.
Spotting cardiac arrest early and starting CPR fast can really help. Knowing the CAB steps and CPR signs can make a big difference in emergencies.
It’s vital to get trained and certified in CPR and vital signs. Keeping up with CPR rules and emergency tips helps us all respond better in urgent situations.
The role of accurate vital signs checking is huge. By using what we’ve learned, we can help improve care and save lives in emergencies.
FAQ
What are the primary vital signs assessed during CPR?
During CPR, we check for consciousness, breathing, and pulse. We also look at body temperature and skin color.
How do you check for signs of life in a victim?
First, make sure the scene is safe. Then, approach the victim carefully. Use the “look, listen, feel” method to check for consciousness, breathing, and pulse.
What is the CAB protocol in CPR, and how does it differ from the traditional ABC approach?
The CAB protocol focuses on Circulation, Airway, Breathing. It checks for pulse first, then airway, and breathing. This is different from ABC, which focuses on Airway, Breathing, Circulation.
How often should pulse checks be performed during CPR, and what is the correct technique?
Pulse checks should happen every 2 minutes. Use the carotid pulse location. Check for 5 to 10 seconds.
What are the signs that CPR is effective, and how can you assess them?
Effective CPR shows proper chest compression and victim response. Look for capillary refill and use CPR quality feedback devices.
When should CPR be stopped, and what signs indicate the return of spontaneous circulation?
Stop CPR when the victim shows signs of life. This includes breathing, pulse, or consciousness. Make this decision based on a thorough assessment and medical guidelines.
Are there age-specific considerations for CPR and vital sign assessment?
Yes, CPR and vital sign assessment vary by age. Infants, children, adults, and the elderly need different approaches due to their unique physiology.
What role does technology play in enhanced vital signs assessment and CPR?
Technology, like AEDs and pulse oximetry, improves CPR and vital signs assessment. It also includes advanced monitoring and smartphone apps.
What are common mistakes made when checking for signs of life, and how can they be avoided?
Mistakes include pulse check errors and misinterpreting breathing. Avoid these with proper training and awareness of these common errors.
What are the legal and psychological considerations for individuals performing CPR?
CPR performers should know Good Samaritan laws for legal protection. They must also prepare mentally for emergencies and understand the psychological impact.
What training and certification options are available for CPR and vital sign assessment?
Options include BLS, ACLS, and refresher training. Both online and in-person training are available, each with its own benefits.
References
































