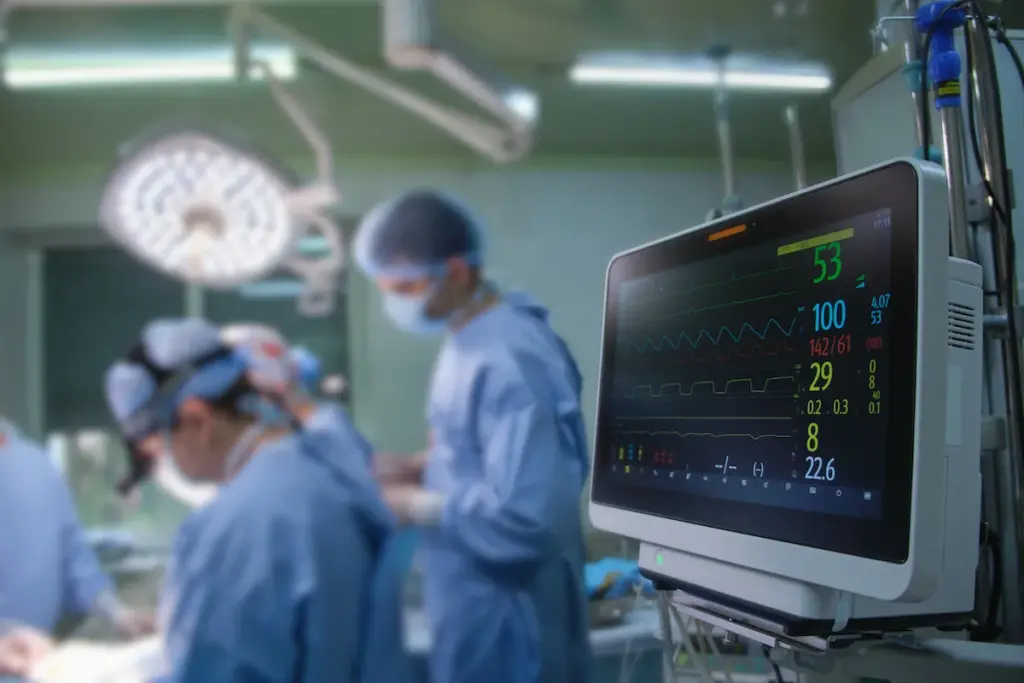
Determining heart transplant priority is a complex process. It involves looking at medical urgency, compatibility, and other key factors.
In the US, over 7,000 people are waiting for a heart transplant. But, only about 4,200 transplants are done each year. The United Network for Organ Sharing (UNOS) manages the transplant waiting list through the Organ Procurement and Transplantation Network (OPTN).
The system aims to increase survival rates and fairness. This makes heart transplant priority very important in this life-saving process.
Key Takeaways
- The heart transplant waiting list is managed by UNOS through OPTN.
- Medical urgency and compatibility are key factors in determining transplant priority.
- Over 7,000 people are awaiting heart transplantation in the US.
- Fewer than 4,200 heart transplants are performed annually.
- The system aims to maximize survival rates and fairness.
The Heart Transplant Crisis in the United States
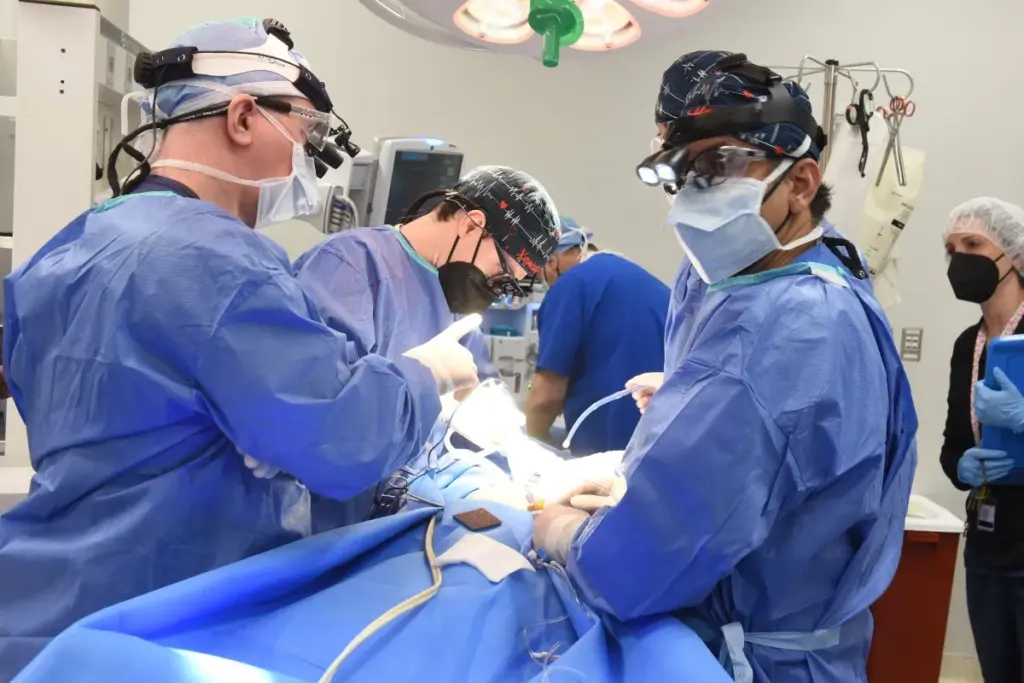
The US is facing a heart transplant crisis. There’s a big gap between the need for donor hearts and the hearts available. This gap means fewer transplants than people waiting for them.
Every year, less than 4,200 heart transplants happen in the US. Yet, over 7,000 people are waiting for a transplant. This shows how serious the crisis is and its impact on those waiting.
The waiting list mortality rate is a big worry. Patients often wait a long time, which can make their health worse.
Current Statistics on Heart Transplant Needs
The need for heart transplants is growing. This is because more people have heart failure and because transplant technology is improving. Studies show that more people are waiting for a transplant.
This trend highlights the need for better ways to allocate organs and for more organ donation rates.
The Supply-Demand Gap
The number of donor hearts is not meeting the demand for transplants. This means the waiting list keeps getting longer. The waiting times are long, and more people on the list are dying.
This situation shows we need to find ways to get more donors and to better use the organs we have.
Understanding the Heart Transplant Waiting List System
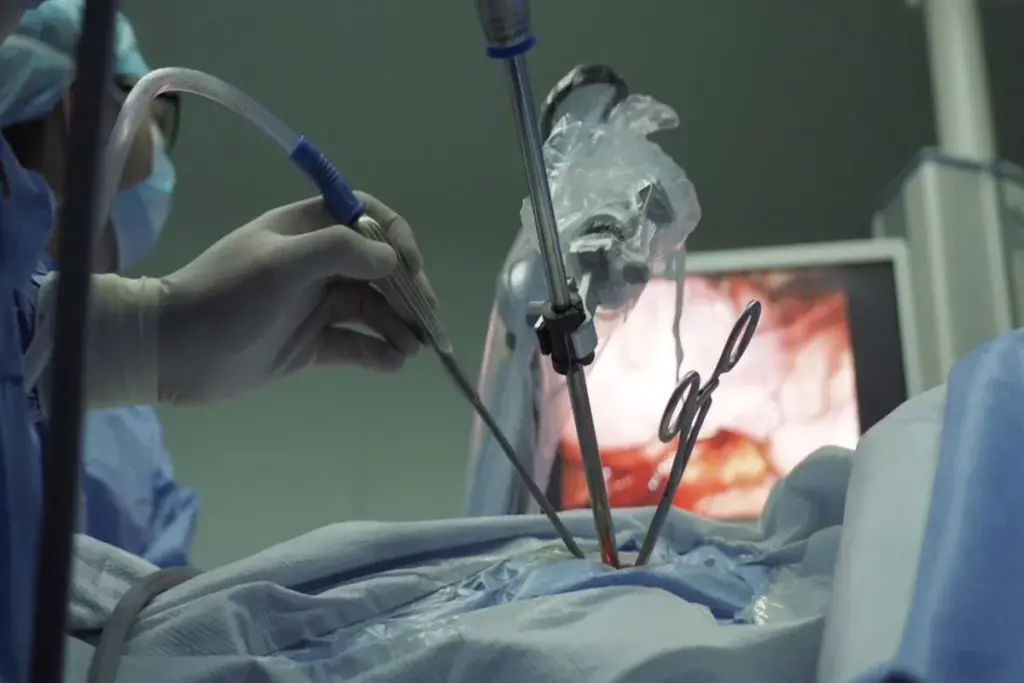
The United Network for Organ Sharing (UNOS) and the Organ Procurement and Transplantation Network (OPTN) are key players in the heart transplant waiting list. They manage the complex process of organ allocation. This ensures organs are given out fairly and efficiently across the country.
Role of the United Network for Organ Sharing (UNOS)
UNOS is a non-profit that oversees the national transplant waiting list. UNOS operates under contract with the federal government to match donated organs with recipients. They use a complex system that looks at medical urgency, waiting time, and biological compatibility.
The role of UNOS includes:
- Managing the national transplant waiting list
- Matching donated organs with recipients
- Coordinating organ distribution across the country
Organ Procurement and Transplantation Network (OPTN)
OPTN is in charge of the national registry of transplant candidates and the organ donation process. OPTN works closely with UNOS to make sure the organ allocation system is smooth and efficient. OPTN’s duties include:
|
Responsibility |
Description |
|---|---|
|
Managing the National Registry |
Maintaining a database of all transplant candidates |
|
Facilitating Organ Donation |
Coordinating the process of organ procurement and allocation |
|
Ensuring Compliance |
Monitoring transplant centers and organ procurement organizations for compliance with OPTN policies |
In summary, UNOS and OPTN work together to manage the heart transplant waiting list. They ensure organs are given out based on medical urgency, waiting time, and other important factors. Their teamwork is vital in saving the lives of patients waiting for heart transplants.
Medical Urgency: The Primary Factor in Heart Transplant Priority
The urgency of a patient’s condition is key in deciding their heart transplant priority. This ensures those in urgent need get the care they need quickly.
Status Classifications for Heart Transplant Candidates
Heart transplant candidates are sorted by how serious their condition is. The United Network for Organ Sharing (UNOS) has a system to rank them. This ranges from Status 1 (most urgent) to Status 3 (less urgent).
Those needing mechanical circulatory support, like VADs, get priority because they are in a critical state. This system helps organize the waiting list. It makes sure the most urgent patients are seen first.
Life Support and Mechanical Circulatory Assistance
Patients on life support or needing mechanical help are seen as high-priority. These steps are vital when a heart is failing. The level of support needed affects their spot on the waiting list.
Mechanical circulatory assistance, like VADs, helps the failing heart. It also boosts the patient’s survival chances until a donor heart is found. This is a big factor in deciding who gets a transplant first.
Assessing medical urgency is complex. It involves looking at how serious a patient’s condition is and their need for life-saving help. By focusing on urgency, the transplant system tries to give hearts to those who need them most.
The Continuous Distribution Framework Implemented in 2024
<SEP-9072_image_4>
The OPTN’s new framework, launched in 2024, changes how heart transplant candidates are ranked. It aims to make the heart allocation fairer and more efficient.
Moving Away from Status-Based Allocation
The old system focused on a patient’s status. Now, a new system looks at many factors. It gives each patient a score based on different traits.
Key Factors in Composite Score Calculation:
- Medical Urgency
- Waiting Time
- Distance from Donor Hospital
- Pediatric Status
How Composite Scores Are Calculated
A complex algorithm calculates these scores. It gives more weight to urgent cases. Waiting time and distance also play a role.
Let’s look at an example:
|
Factor |
Weightage |
Example Score |
|---|---|---|
|
Medical Urgency |
40% |
80 |
|
Waiting Time |
20% |
60 |
|
Distance from Donor Hospital |
20% |
40 |
|
Pediatric Status |
20% |
100 |
|
Composite Score |
70 |
This new system is more flexible and meets patient needs better. It looks at more factors to cut down waiting times and improve results.
Biological Compatibility Factors in Heart Transplantation
The success of a heart transplant depends on how well the donor and recipient match biologically. This matching ensures the transplanted heart is less likely to be rejected. It boosts the chances of a successful transplant.
Blood Type Matching Considerations
Blood type matching is key in heart transplantation. The donor and recipient must have the same blood type to avoid bad reactions. The main types are A, B, AB, and O, with Rh positive or negative.
Matching blood types lowers the risk of immune reactions against the new heart. A study found that mismatched blood types increase the risk of rejection and complications.
“Blood type compatibility is critical for the long-term success of heart transplants.”
|
Blood Type |
Compatible Donor Types |
|---|---|
|
A |
A, O |
|
B |
B, O |
|
AB |
AB, A, B, O |
|
O |
O |
Predicted Heart Mass and Its Importance
Predicted Heart Mass (PHM) is vital for matching donors and recipients. It considers the recipient’s body size and sex to find the ideal heart mass. This method is more accurate than just looking at body weight or blood type.
Using PHM for matching has been linked to better survival rates post-transplant. It allows for a more detailed approach to matching. It considers the complexities of heart size and the recipient’s needs.
The use of PHM is a big step forward in heart transplantation. It makes matching more precise and could lead to better outcomes for recipients.
Waiting List Checking: How Patients Monitor Their Status
Heart transplant candidates can now check their waiting list status easily. They use patient portal systems for this. These systems have changed how patients track their progress, giving them timely updates and important info.
Patient Portal Systems for Transplant Candidates
Patient portal systems offer transplant candidates secure access to their waiting list status. They can view their current status, review medical updates, and communicate with their healthcare team online. This access helps reduce anxiety and keeps patients informed about their position on the waiting list.
The United Network for Organ Sharing (UNOS) and other organ procurement organizations created these systems. They use technology to make the transplant experience better. This approach focuses more on the patient’s needs.
Understanding Your Position and Status Updates
It’s important for transplant candidates to understand their position on the waiting list. The patient portal systems provide the current status and insights into factors influencing their position. These factors include medical urgency, waiting time, and biological compatibility with donors.
Regular status updates are key in these systems. They keep patients informed about any changes in their status. This could be a change in their medical urgency score or an update on their waiting time. By staying informed, patients can prepare better for the transplant process.
To get the most out of these systems, transplant candidates should log in regularly. They should check their status and review updates from their healthcare team. This proactive approach helps patients stay on top of their waiting list status and make informed decisions about their care.
Geographical Considerations in Heart Allocation
The place where a donor hospital is located is key in deciding who gets a heart. The distance to the transplant center and regional rules affect how hearts are given out.
Regional Distribution Policies
Regional rules help make sure organs are given out fairly. They look at how many organs are available, how many people need them, and who needs them most. The United Network for Organ Sharing (UNOS) helps make and follow these rules nationwide.
It’s not just about where you live. Organs are matched with the right person based on medical needs and how well they fit. This means looking at things like blood type, organ size, and how urgent the need is.
Distance from Donor Hospital as a Factor
The distance to the transplant center is also important. Organs usually go to people close to the donor hospital. This helps keep the organ healthy for longer.
Choosing who gets an organ is a careful process. It balances keeping the organ healthy with giving it to the most urgent cases. This is done with special computer programs that look at many factors, including distance.
In short, where a donor hospital is matters a lot in heart allocation. Knowing this helps everyone involved make sure the system works well and saves lives.
Special Considerations for Pediatric Heart Transplant Candidates
Children waiting for heart transplants need special care because of their unique needs. The heart transplant waiting list is set up to help these kids. It makes sure they get the care they need.
Priority Status for Children
Pediatric heart transplant candidates get priority status on the waiting list. This is because of their age and how urgent their situation is. It’s key to make sure kids get their transplants quickly.
The United Network for Organ Sharing (UNOS) and the Organ Procurement and Transplantation Network (OPTN) manage the waiting list. They make sure hearts are given based on who needs them most, including kids.
Size Matching for Pediatric Recipients
Size matching is very important for kids needing heart transplants. The donor heart must fit the child’s body size for a successful transplant. This is even more critical for kids because their hearts are smaller and they grow and develop differently.
When matching sizes, doctors look at the donor heart and the child’s body surface area. This makes sure the heart works right and helps the child grow.
By focusing on kids first and matching sizes carefully, the transplant community works to help children waiting for heart transplants.
Ethical Dimensions of Heart Transplant Allocation
Heart transplant allocation is a delicate balance of urgency and ethics. It’s not just about who needs a heart the most. It also involves ethical considerations that guide who gets a transplant.
Balancing Urgency and Utility
One big ethical challenge is balancing urgency and utility. Urgency is about the medical need of the patient, with those in dire need first. Utility looks at the chance of a successful transplant and the patient’s long-term survival.
Choosing patients based on urgency can sometimes not be the best for utility. For example, a patient with a better chance of survival might be passed over for a sicker one. This dilemma is about saving lives now versus the best long-term outcomes.
“The allocation of scarce organs like hearts for transplantation requires a nuanced approach that balances competing ethical demands.”
Addressing Disparities in Access
Another key ethical issue is making sure everyone has equal access to heart transplants. Things like where you live, how much money you make, and your healthcare access can affect your chances.
- Geographical disparities come from uneven donor heart distribution and transplant centers.
- Socioeconomic status can impact a patient’s ability to get evaluated and listed for a transplant.
- Healthcare access can affect pre-transplant care and post-transplant follow-up.
To fix these disparities, we need policy changes and better healthcare infrastructure. Making sure everyone has equal access to heart transplants is not just right; it’s also key to keeping public trust in the system.
Looking into the ethical sides of heart transplant allocation helps us understand its complexities. This way, we can work towards a fairer and more effective system.
Expanding the Donor Pool: Alternative Approaches
To tackle the heart transplant shortage, new ways to find donors are being explored. The goal is to increase the number of donor hearts. This is essential to meet the growing demand for heart transplants.
Accepting Hepatitis C-Positive Hearts
One approach is to use hepatitis C-positive hearts for transplants. Before, these hearts were often not used because of the virus risk. But, new treatments have changed this.
Direct-acting antivirals (DAAs) have greatly improved treatment for hepatitis C. This makes it possible to use these hearts for transplants.
- Studies show that people who get these hearts and take DAAs do very well.
- Using these hearts can greatly increase the donor pool. This could shorten wait times for those needing transplants.
- Guidelines are being made to ensure safe transplant and care for these recipients.
Extended Criteria Donors
Another strategy is using extended criteria donors (ECDs). ECDs are donors who don’t fit the usual criteria but can give viable organs. This includes older donors or those with certain health issues.
Using ECDs can add more donor hearts. But, it’s important to weigh the risks and benefits. The donor’s health, the heart’s condition, and the recipient’s urgency are all considered.
By exploring these new methods, we can help reduce the waiting list for heart transplants. This will improve care for those in need of a transplant.
Survival Rates and Waiting List Mortality
It’s key to know about survival rates and waiting list mortality for heart transplant patients. The waiting list sorts patients by how urgent they need a transplant, how well they match with a donor, and more.
Waiting for a heart transplant is tough, with many patients dying before getting one. About 50,000 people are waiting for an organ transplant, and sadly, many don’t make it.
Statistics on Waiting List Outcomes
Outcomes for heart transplant patients on the waiting list differ a lot. These outcomes depend on the patient’s health when they’re listed, if a matching donor heart is found, and their overall health.
Patients who need a transplant quickly tend to have higher death rates on the list. But, those who get a transplant often live longer after it.
- Patients with Status 1A need a transplant the most and get priority.
- Many patients on the list die before they can get a transplant.
Post-Transplant Survival Statistics
Thanks to better technology and care, survival rates after transplant have gone up. The post-transplant survival numbers are good, with many patients living five years or more after their transplant.
|
Time Frame |
Survival Rate |
|---|---|
|
1 Year |
85-90% |
|
5 Years |
70-75% |
|
10 Years |
50-60% |
These numbers show why we need to keep improving transplant care. We aim to boost survival rates and cut waiting list mortality.
The Patient Journey: From Listing to Transplantation
Patients waiting for a heart transplant go through a journey filled with careful steps. This path includes several key moments from the start to the transplant itself.
Initial Evaluation and Listing Process
The first part of the journey is the initial evaluation for a heart transplant. This step looks at the patient’s health history and current condition. A team of doctors checks if the patient is a good match for a transplant.
After checking, patients who can get a transplant are put on a waiting list. The listing process adds the patient’s info to the United Network for Organ Sharing (UNOS) database. This database manages the national transplant list.
Maintaining Transplant Candidacy
Patients on the list must keep meeting the transplant criteria. They need regular check-ups to see if they’re ready for a transplant.
Staying on the list also means following a treatment plan. This plan might include medicines, lifestyle changes, and devices like Ventricular Assist Devices (VADs). These steps help keep the patient stable and increase their transplant success chances.
The journey from listing to transplant is complex. It needs teamwork from the patient, their family, and healthcare team. Knowing the steps and the importance of staying on the list helps patients through this tough time.
Living with a VAD While Waiting for a Heart
Ventricular assist devices (VADs) are more than just medical tools. They are lifelines for those waiting for a heart transplant. These devices help the heart work better and improve health until a donor heart is found.
For many, VADs greatly improve life while waiting for a transplant. They help patients move more and live more independently. This is because VADs make the heart function better.
Types of Ventricular Assist Devices
There are many types of VADs, each with its own benefits. The right device depends on the patient’s health needs and how long they’ll need support.
- Left ventricular assist devices (LVADs) help the left ventricle, which pumps blood to the body.
- Right ventricular assist devices (RVADs) help the right ventricle, which sends blood to the lungs.
- Biventricular assist devices (BiVADs) support both ventricles, giving full heart support.
Quality of Life Considerations
Life with a VAD means big changes. Patients must follow a strict care plan, including medication and regular doctor visits.
Yet, many patients say VADs have made their lives better. These devices help them live longer and do things they love. They also let patients stay close to family and friends, and keep some independence.
Key things for VAD patients to remember include:
- Watching for and dealing with device alarms and problems.
- Keeping a healthy lifestyle with good food and exercise.
- Staying up-to-date on their health and treatment choices.
Future Directions in Heart Transplant Allocation
The future of heart transplant allocation is set to see big changes. This is thanks to new technologies and policy updates. As we move forward, it’s key to think about what’s coming next in this field.
Technological Innovations in Matching
New tech will be a big help in making heart transplants better. Some exciting developments include:
- Artificial Intelligence (AI) and Machine Learning (ML) to find the best matches for donors and recipients.
- Advanced Data Analytics to guess how well patients will do and make better organ choices.
- Blockchain Technology to make the organ donation and transplant process more open and safe.
These new technologies could make heart transplant allocation much better.
Policy Changes on the Horizon
Policy updates are also on the way to change heart transplant allocation. Some changes could be:
- Revised Allocation Criteria to focus on who needs a transplant the most, based on urgency and waiting time.
- Expanded Donor Pool by using organs from donors who might not have been considered before.
- Increased Transparency by sharing more data and results publicly.
These policy changes aim to make heart transplant allocation fairer and more efficient.
Conclusion: Navigating the Heart Transplant Waiting List
Getting a heart transplant is a complex journey. It depends on how urgent the need is, how well the donor’s heart matches, and the rules for sharing organs.
It’s key for patients and their families to understand these points while waiting. The United Network for Organ Sharing (UNOS) and the Organ Procurement and Transplantation Network (OPTN) help manage the list. They make sure organs are given out fairly and quickly.
The list is always changing, with updates on patient status happening all the time. It’s important for patients to stay updated on their place on the list and why their priority might change.
Learning about the heart transplant waiting list and how it works can help people deal with the wait. It’s a way to better understand the journey to a new heart.
FAQ
How is priority determined for a heart transplant?
A complex system decides who gets a heart transplant first. It looks at how urgent the need is, if the heart is a good match, how long they’ve been waiting, and other things. UNOS and the OPTN manage this process.
What is the role of UNOS in managing the heart transplant waiting list?
UNOS oversees the national transplant waiting list. They make sure organs are given out fairly. This is based on how urgent the need is and if the heart is a good match.
How long does a heart transplant surgery take?
Heart transplant surgery can take a few hours. It usually lasts between 4 to 6 hours. This depends on how complex the surgery is and the patient’s health.
What is the continuous distribution framework in heart transplantation?
In 2024, a new system was introduced. It uses scores to rank candidates. This system focuses on many factors, not just status.
How are composite scores calculated in the new allocation system?
Scores are based on several things. These include how urgent the need is, how long they’ve been waiting, if the heart is a good match, and where they are. This helps find the best match for the heart.
Why is biological compatibility important in heart transplantation?
It’s key for a successful transplant. It means the blood types match and the heart size is right. This ensures the donor heart works well for the recipient.
How can patients check their status on the heart transplant waiting list?
Patients can check their status online. Their transplant center has a patient portal. This lets them know where they are on the list and any updates.
What geographical considerations affect heart allocation?
Where the donor and recipient are matters. Policies and distance from the donor hospital are considered. This affects how quickly a heart is given to a candidate.
Are pediatric heart transplant candidates given special priority?
Yes, kids get priority. It’s important to find a heart that’s the right size for them. This ensures the best fit for the child.
What are the survival rates for heart transplant patients?
Survival rates vary. But most patients do well after the transplant. They can live active lives. Survival stats are available from transplant registries.
What is the patient journey from being listed to receiving a heart transplant?
First, patients go through an evaluation and listing. Then, they’re checked regularly to stay eligible. They wait until a suitable heart is found.
How do ventricular assist devices (VADs) support patients waiting for a heart transplant?
VADs help the heart work better. They improve life quality while waiting for a transplant. There are different types to meet individual needs.
What are the future directions in heart transplant allocation?
New technologies and policy changes are coming. They aim to make the allocation process more efficient and fair.
How long can a person live with a heart transplant?
Many live 10 to 20 years or more after a transplant. It depends on their health, the heart’s condition, and following treatment.
How do heart transplants work?
A diseased heart is replaced with a healthy one. The new heart is connected to the recipient’s blood vessels. It starts working right away.
What is the heart transplant waiting list by state?
The list is national, but centers serve patients from different states. The waiting list status can vary by region.
References
- World Population Review. (2025). Heart Transplant Waiting List by State 2025. Retrieved from https://worldpopulationreview.com/state-rankings/heart-transplant-waiting-list-by-state (World Population Review)
- Organ Procurement and Transplantation Network (OPTN) & Health Resources & Services Administration (HRSA). (n.d.). Continuous Distribution — Heart. Retrieved from https://optn.transplant.hrsa.gov/policies-bylaws/a-closer-look/continuous-distribution/continuous-distribution-heart/ (optn.transplant.hrsa.gov)
- Toro, S., & Schlendorf, K. H. (2025). Expanding the Donor Pool. Methodist DeBakey Cardiovascular Journal, 21(3), 33–39. https://doi.org/10.14797/mdcvj.1577. PMC12082461. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC12082461/ (PubMed)
- Jain, R., Kransdorf, E. P., Cowger, J., Jeevanandam, V., & Kobashigawa, J. A. (2025). Donor Selection for Heart Transplantation in 2025. JACC: Heart Failure, 13(3), 389–401. PMC12085803. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC12085803/ (PubMed)
- Centers for Disease Control and Prevention. (n.d.). Heart Transplantation. Retrieved from https://www.cdc.gov/transplantation/heart/index.htm (Mayo Clinic).
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC7738116/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























