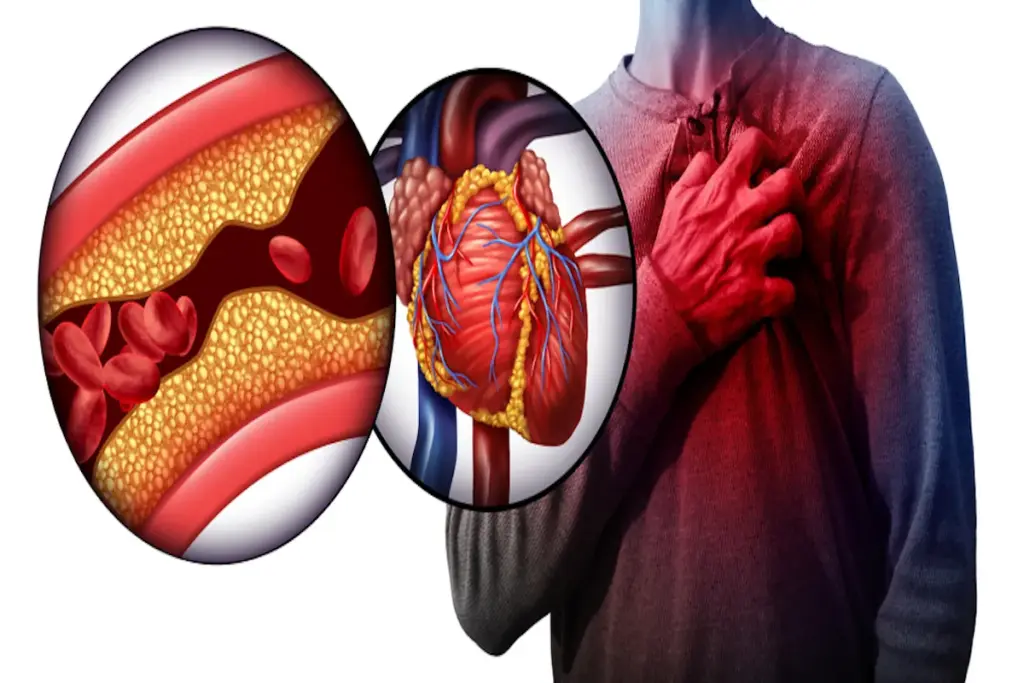
Nearly 1 in 3 adults in the United States has some form of cardiovascular disease. This is often due to clogged arteries. When plaque builds up in the arteries, it can lead to heart attacks and strokes. It’s important to know the warning signs of clogged arteries to get help early. Identify the warning signs of clogged arteries. Knowing these arterial blockage symptoms is crucial for immediate action and a positive result.
We will look at the symptoms of clogged arteries. This will help you know when to see a doctor. Spotting these signs early can help prevent bigger problems.
Key Takeaways
- Clogged arteries can lead to severe cardiovascular diseases.
- Early detection of symptoms is key for timely medical help.
- Knowing the warning signs can prevent serious health issues.
- Spotting symptoms early can save lives.
- Seeing a doctor is important when you notice symptoms of clogged arteries.
The Silent Danger of Clogged Arteries
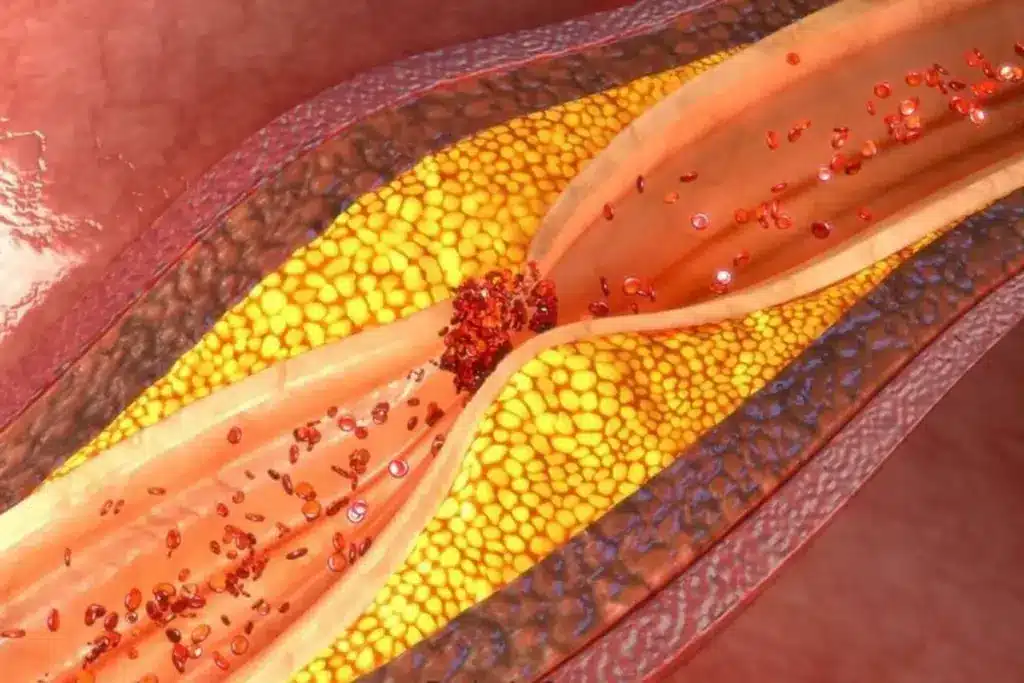
It’s important to know about the silent danger of clogged arteries. These blockages can build up over years without any symptoms. This makes them a hidden threat to our health.
How Arterial Blockages Develop
Arterial blockages happen because of high cholesterol, smoking, and high blood pressure. These issues cause the arteries to narrow and harden. This restricts blood flow to important organs. The problem grows slowly, and symptoms may not show until it’s too late.
Several factors lead to arterial blockages, including:
- High levels of low-density lipoprotein (LDL) cholesterol
- Smoking and tobacco use
- Hypertension (high blood pressure)
- Diabetes
- Obesity and lack of physical activity
Why Early Detection Matters
Finding arterial blockages early is key. It lets us act fast to prevent serious heart problems. If caught early, we can make lifestyle changes and use medicine to slow the blockage.
|
Benefits of Early Detection |
Description |
|---|---|
|
Prevention of Cardiovascular Events |
Early detection can prevent heart attacks and strokes by addressing blockages before they become severe. |
|
Lifestyle and Medical Interventions |
Timely intervention allows for lifestyle changes and medical treatments to be implemented, slowing or stopping blockage progression. |
|
Improved Quality of Life |
By managing arterial blockages, individuals can maintain better overall health and quality of life. |
Recognizing Arterial Blockage Symptoms: A Guide
Spotting artery blockage signs early can greatly improve treatment results. Arterial blockages can cause serious health problems if not treated quickly. We’ll look at the symptoms of arterial blockages, helping you know when to get medical help.
Early Warning Signs
The early signs of artery blockage are subtle but important for early detection. Common symptoms include:
- Chest pain, known as angina, which may feel like pressure or tightness in the chest
- Shortness of breath, specially during physical activity
- Leg pain when walking, known as intermittent claudication
- Fatigue and weakness, which can be a sign of reduced blood flow
These symptoms can vary in intensity and frequency. It’s key to notice any changes in your body. If you experience any of these signs, see a healthcare professional.
|
Symptom |
Description |
|---|---|
|
Chest Pain (Angina) |
Pressure or tightness in the chest, often triggered by physical exertion or emotional stress |
|
Shortness of Breath |
Difficulty breathing during physical activity or at rest, indicating possible heart issues |
|
Leg Pain (Intermittent Claudication) |
Pain or cramping in the legs when walking, which may improve with rest |
Advanced Symptoms Requiring Immediate Attention
Advanced symptoms of artery blockage are more severe and need immediate medical help. These include:
- Severe chest pain that persists or worsens
- Difficulty breathing or shortness of breath at rest
- Severe leg pain or cramping that does not improve with rest
If you or someone you know has these advanced symptoms, get emergency medical care right away. As a medical expert said,
“Time is muscle when it comes to heart health. The sooner you act, the better the outcomes.”
Knowing and recognizing artery blockage symptoms is the first step in managing and treating them. By being aware of early and advanced symptoms, you can take steps to protect your heart health.
Coronary Artery Disease: Heart-Related Warning Signs

Coronary artery disease affects millions worldwide. It shows through specific heart-related warning signs. Early detection is key to effective treatment.
Chest Pain (Angina)
Chest pain, or angina, is a common symptom. It happens when the heart doesn’t get enough oxygen-rich blood. Angina feels like pressure or squeezing in the chest.
It can also cause pain in the arms, back, neck, jaw, or stomach. If you have recurring chest pain, see a doctor.
Shortness of Breath During Activity
Shortness of breath during activity is another sign. It happens when the heart can’t pump enough blood. This symptom is noticeable during activities you used to handle easily.
If you’re short of breath, talk to a healthcare provider. It could mean your heart needs attention.
Unusual Fatigue and Weakness
Feeling unusually tired or weak can be a sign. When the heart isn’t pumping well, energy levels drop. Feeling tired or weak without a reason might be heart-related.
|
Symptom |
Description |
|---|---|
|
Chest Pain (Angina) |
Pressure or squeezing in the chest, potentially radiating to arms, back, neck, jaw, or stomach |
|
Shortness of Breath |
Feeling breathless during physical activity due to the heart’s reduced ability to pump blood |
|
Unusual Fatigue and Weakness |
Feeling tired or weak without a clear reason, potentially due to reduced heart efficiency |
Heart Palpitations and Irregular Heartbeat
Heart palpitations and irregular heartbeat are symptoms too. They feel like fluttering, pounding, or an irregular heartbeat. Not all palpitations are serious, but persistent ones need a doctor’s check.
Watch these symptoms and get medical help if they don’t go away or get worse.
Cerebrovascular Disease: Brain-Related Symptoms
It’s important to know the brain symptoms of cerebrovascular disease to get help fast. This disease harms the blood vessels that feed the brain. It can cause strokes or TIAs. We’ll look at the main symptoms.
Transient Ischemic Attacks (Mini-Strokes)
A TIA, or “mini-stroke,” is when the brain’s blood supply stops for a short time. Its symptoms are like a stroke’s. They can include:
- Sudden weakness or numbness in the face, arm, or leg, on one side.
- Difficulty speaking or understanding speech, like slurred words or confusion.
- Vision disturbances, such as sudden blurred vision or loss of vision in one or both eyes.
TIAs are a warning that a bigger stroke might happen. So, getting medical help right away is key.
Speech and Cognitive Changes
Cerebrovascular disease can change how we speak and think. Symptoms include:
- Difficulty finding the right words or following conversations.
- Memory problems, like forgetting recent events or learning new info.
- Confusion or disorientation, which can happen suddenly or over time.
These signs mean the brain is not working right. A doctor should check them out.
Vision Disturbances
Vision can be affected by cerebrovascular disease. Symptoms include:
- Sudden loss of vision in one or both eyes.
- Blurred or double vision, which can happen suddenly.
- Difficulty seeing on one side or in both eyes.
These vision problems can mean a TIA or stroke. They need quick medical help.
Balance and Coordination Problems
Cerebrovascular disease can also mess with balance and coordination. Symptoms include:
- Dizziness or lightheadedness, making it hard to stand or walk.
- Loss of balance or coordination, raising the risk of falls.
- Trouble walking, which can start suddenly or over time.
These symptoms can make daily life hard. A doctor should check them out.
Peripheral Artery Disease: Extremity Symptoms
Peripheral artery disease (PAD) happens when arteries to our limbs get narrowed or blocked. This condition causes various symptoms in our extremities, affecting our quality of life.
Intermittent Claudication (Leg Pain When Walking)
Intermittent claudication is a key symptom of PAD. It’s leg pain that happens when walking and goes away with rest. This pain is because of not enough blood flow to muscles when we’re active.
Cold Feet and Hands
People with PAD often feel coldness in their feet and hands. This is because of less blood flow. This symptom can last a long time and gets worse in cold weather.
Skin Changes and Hair Loss
The skin on affected limbs can change, becoming thinner, shinier, or even getting ulcers. Hair loss on legs or feet also happens because of poor blood supply.
Slow-Healing Wounds on Extremities
PAD can cause slow-healing wounds on our extremities. Poor blood flow makes it hard for our bodies to heal cuts or sores. This can lead to infections or more serious problems.
It’s important to recognize these symptoms early for PAD diagnosis and treatment. If you or someone you know has these symptoms, seeing a healthcare professional is key for the right care.
Renal Artery Stenosis: Kidney-Related Warning Signs
The kidneys are vital for our health. When renal artery stenosis happens, it can cause serious symptoms. This condition narrows the arteries that carry blood to the kidneys.
Resistant Hypertension
Resistant hypertension is a key symptom. It’s high blood pressure that doesn’t get better with treatment. The kidneys help control blood pressure. If they don’t get enough blood, blood pressure can go up.
Changes in Urination Patterns
Changes in urination patterns are another sign. You might pee more often, less often, or see blood in your urine. These signs show the kidneys aren’t working right because of less blood.
Fluid Retention and Swelling
Fluid retention and swelling in the legs, ankles, and feet are also signs. If the kidneys don’t get enough blood, they can’t remove fluid. This leads to swelling.
It’s important to catch these symptoms early. Renal artery stenosis can cause serious kidney problems if not treated. If you notice these signs, see a doctor right away.
Mesenteric Ischemia: Digestive System Symptoms
When the arteries that supply blood to the intestines become narrowed or blocked, it can lead to mesenteric ischemia. This causes significant digestive issues. It’s a serious condition that needs prompt medical attention to prevent complications.
Post-Meal Abdominal Pain
One of the hallmark symptoms of mesenteric ischemia is abdominal pain after eating. This pain happens because eating increases the demand for blood flow to the intestines. In people with narrowed or blocked arteries, this demand is not met.
The pain can be severe and is often described as crampy or colicky.
Food Fear and Avoidance
Due to the association between eating and abdominal pain, individuals with mesenteric ischemia may develop a fear of eating. This fear can lead to avoidance of food. As a result, they may suffer from nutritional deficiencies and further health complications.
Unexplained Weight Loss
Weight loss is a common symptom of mesenteric ischemia, mainly due to food avoidance and malabsorption of nutrients. The reduced blood flow to the intestines impairs the ability to absorb essential nutrients. This leads to unintended weight loss.
Changes in Bowel Habits
Mesenteric ischemia can also cause changes in bowel habits, including diarrhea or constipation. These changes occur due to the compromised blood flow affecting the normal functioning of the intestines.
The symptoms of mesenteric ischemia can significantly impact an individual’s quality of life. Understanding these symptoms is key for early diagnosis and treatment.
|
Symptom |
Description |
|---|---|
|
Post-Meal Abdominal Pain |
Crampy or colicky pain after eating due to increased demand for blood flow. |
|
Food Fear and Avoidance |
Fear of eating due to associated pain, leading to nutritional deficiencies. |
|
Unexplained Weight Loss |
Weight loss due to food avoidance and malabsorption of nutrients. |
|
Changes in Bowel Habits |
Diarrhea or constipation due to compromised blood flow affecting intestinal function. |
Recognizing the symptoms of mesenteric ischemia is essential for seeking timely medical intervention. If you or someone you know is experiencing these symptoms, it is vital to consult a healthcare professional. They can provide proper diagnosis and treatment.
Gender Differences in Arterial Blockage Symptoms
It’s important to know how symptoms of arterial blockage differ by gender. Arterial blockages, or atherosclerosis, can cause serious heart problems. But, the signs often show up differently in men and women.
How Women’s Symptoms Differ
Women often have different signs than men when they have arterial blockages. While men usually feel chest pain, women might not. Instead, they might feel:
- Shortness of breath
- Fatigue
- Nausea or dizziness
- Pain in the back, neck, or jaw
This makes it harder to spot arterial blockages in women. It can lead to delays in getting the right treatment.
Unique Symptoms in Men
Men often feel chest pain, but they might also have other signs. These include:
- Discomfort or pain in one or both arms, the back, neck, jaw, or stomach
- Symptoms of a heart attack, such as lightheadedness or nausea
Men tend to have more severe symptoms that need quick medical help.
Age-Related Symptom Variations
Age affects how symptoms of arterial blockage show up. Older people, no matter their gender, might have more severe or different signs. This is because they might be less active, have other health issues, or have changes in their heart with age.
|
Age Group |
Common Symptoms |
|---|---|
|
Younger Adults |
Chest pain, shortness of breath |
|
Older Adults |
Fatigue, dizziness, confusion |
It’s key for doctors to know these differences. This helps them make the right diagnosis and treatment plan.
Silent Arterial Disease: When There Are No Symptoms
Arterial disease can sneak up on you, often without any warning signs. This is why it’s key for people at high risk to get checked regularly. Known as silent arterial disease, it can lead to serious heart problems without any signs beforehand.
The Dangers of Asymptomatic Progression
Asymptomatic arterial disease can quietly get worse until it’s too late. The lack of symptoms doesn’t mean the disease is not serious. It usually means the damage hasn’t shown up yet.
Several factors make arterial disease hard to notice, including:
- Gradual blockage development
- Compensatory mechanisms that mask symptoms
- Variability in individual tolerance to blockages
Who Should Be Screened Regularly
Regular checks for arterial disease are vital for some people. Spotting those at high risk early is key for catching and treating the disease. Here are some groups that should think about getting screened:
- People with a family history of heart disease
- Those with diabetes, high blood pressure, or high cholesterol
- Smokers and those who used to smoke
- Individuals over 40
- Those who don’t exercise much or eat poorly
Risk Factors That Increase Chances of Arterial Blockage
Arterial blockage risk comes from genetics and lifestyle. Knowing these factors helps prevent and manage the condition.
Modifiable Risk Factors
Some risks can be changed to lower the chance of blockage. These include:
- High Cholesterol: Too much LDL cholesterol can cause artery plaque.
- Smoking: Smoking harms blood vessel linings, making them more likely to block.
- Hypertension: High blood pressure damages blood vessels, raising blockage risk.
- Diabetes: Diabetes harms blood vessels and nerves, leading to artery disease.
Changing these risks through lifestyle and medicine can greatly lower blockage risk.
Non-Modifiable Risk Factors
Some risks can’t be changed, but knowing them helps prevent. Non-modifiable risks include:
|
Risk Factor |
Description |
|---|---|
|
Age |
Arterial blockage risk grows with age due to plaque buildup. |
|
Gender |
Men face higher blockage risk at a younger age than women. |
|
Family History |
Having a family history of heart disease increases your risk. |
Knowing both modifiable and non-modifiable risks helps us prevent and manage blockage better.
Diagnostic Tests for Detecting Clogged Arteries
Doctors use both non-invasive and invasive tests to find and check clogged arteries. These tests help spot blockages and pick the best treatment.
Non-Invasive Testing Methods
Non-invasive tests are often the first choice. They are safe and comfortable. Here are some common ones:
- Ultrasound: Uses sound waves to show artery images and find blockages.
- Computed Tomography (CT) Scan: Gives detailed images of arteries to see plaque buildup.
- Magnetic Resonance Imaging (MRI): Shows artery details without X-rays, great for disease extent.
- Stress Test: Checks the heart’s function under stress, often with ECG or echocardiography.
|
Test |
Description |
Advantages |
|---|---|---|
|
Ultrasound |
Uses sound waves to image arteries |
Non-invasive, no radiation |
|
CT Scan |
Provides detailed cross-sectional images |
Highly detailed, quick results |
|
MRI |
Detailed imaging without X-rays |
No radiation, excellent for soft tissue |
Invasive Diagnostic Procedures
When non-invasive tests don’t give clear results, doctors might use invasive tests. These include:
- Angiography: Injects dye into arteries for X-ray blockage views.
- Coronary Angiography: Looks closely at coronary arteries for blockages.
Invasive tests give detailed info on blockage location and severity. They help decide on treatments like angioplasty or stenting.
When to Seek Emergency Medical Attention
Knowing when to get emergency medical help is key to avoiding serious problems from blockages. Some symptoms mean you need to act fast. Spotting these signs can save lives.
Red Flag Symptoms That Require Immediate Care
If you or someone else has these symptoms, act quickly:
- Severe chest pain or discomfort that doesn’t go away or is with other signs like shortness of breath, nausea, or feeling dizzy.
- Sudden severe headache that’s really bad or with confusion, trouble speaking, or weakness on one side.
- Difficulty speaking or understanding speech, which could mean a stroke.
- Weakness or numbness in the face, arm, or leg on one side of the body.
- Vision disturbances, like sudden blurred vision, double vision, or losing vision in one or both eyes.
The Importance of Quick Response
Acting fast when you see these symptoms is very important. The sooner you get help, the better the chances of less damage and better results. For heart attacks or strokes, quick action can greatly lower the risk of serious harm or death.
If you’re showing these symptoms, don’t wait. Call emergency services or get someone to take you to the nearest ER. Time is of the essence in these cases.
What to Tell Emergency Responders
When you’re getting emergency medical help, give as much info as you can to the responders. This includes:
- Telling them about your symptoms and when they started.
- Listing any medicines you’re taking now.
- Talking about any health problems you already have.
- Giving them your emergency contact info.
Having this info ready can help responders give the best care on the way to the hospital.
Treatment Approaches for Arterial Blockages
Treating arterial blockages involves different methods based on the blockage’s severity and location.
We look at several factors to choose the right treatment. These include the person’s health and how bad the blockage is. Our goal is to improve blood flow, ease symptoms, and avoid more problems.
Medication-Based Therapies
Medicines are key in managing arterial blockages. They help in many ways, such as:
- Lowering cholesterol levels
- Controlling blood pressure
- Stopping blood clots
- Reducing inflammation
Some common medicines include:
|
Medication Type |
Purpose |
Examples |
|---|---|---|
|
Statins |
Lower cholesterol |
Atorvastatin, Simvastatin |
|
Antiplatelet agents |
Prevent blood clots |
Aspirin, Clopidogrel |
|
Beta blockers |
Control blood pressure |
Metoprolol, Atenolol |
Interventional Procedures
For serious blockages, we might need to use interventional procedures. These aim to get blood flowing again.
Some common procedures are:
- Angioplasty: a small procedure to open up the blocked artery
- Stenting: using a stent to keep the artery open
- Atherectomy: removing plaque from the artery
Surgical Options
Sometimes, surgery is needed to bypass or remove the blockage.
Surgical options include:
- Bypass surgery: making a new path around the blocked artery
- Endarterectomy: removing plaque and fixing the artery
We work with patients to find the best treatment plan. We consider their health and specific needs.
Lifestyle Modifications to Prevent and Manage Arterial Disease
We can lower the risk of blockages in arteries by making smart lifestyle choices. A complete approach to lifestyle changes is essential for preventing and managing arterial disease.
Heart-Healthy Diet Recommendations
Eating a heart-healthy diet is key. It should include lots of fruits, vegetables, whole grains, and lean proteins. Try to avoid foods high in saturated fats, trans fats, and cholesterol.
Adding foods rich in omega-3 fatty acids, like salmon and walnuts, is also beneficial.
|
Food Group |
Recommended Foods |
Foods to Limit |
|---|---|---|
|
Fruits and Vegetables |
Berries, leafy greens, citrus fruits |
Fruits canned in syrup, vegetables cooked in butter |
|
Grains |
Whole wheat bread, brown rice, quinoa |
White bread, refined pasta, sugary cereals |
|
Protein |
Lean meats, fish, legumes, nuts |
Processed meats, fried foods, high-fat dairy |
Exercise Guidelines for Arterial Health
Regular exercise is vital for keeping arteries healthy. Aim for 150 minutes of moderate-intensity aerobic exercise or 75 minutes of vigorous-intensity aerobic exercise each week. Also, adding strength training to your routine can boost your heart health.
Stress Management Techniques
Too much stress can harm your arteries. Using stress management techniques like meditation, deep breathing, or yoga can help. Make sure to take time each day to relax and manage stress.
- Meditation and mindfulness practices
- Deep breathing exercises
- Yoga and tai chi
- Progressive muscle relaxation
Smoking Cessation Strategies
Smoking greatly increases the risk of arterial disease. Quitting can significantly lower this risk. Use a mix of counseling and medication to help quit smoking. Also, avoid secondhand smoke to keep your arteries healthy.
Effective smoking cessation strategies include:
- Nicotine replacement therapy
- Prescription medications
- Counseling and support groups
- Alternative methods such as acupuncture
The Connection Between Arterial Blockages and Other Health Conditions
It’s important to know how arterial health connects to other health issues. Arterial blockages often link to many other health problems. This creates a complex situation that needs a full approach to manage.
Diabetes and Vascular Health
Diabetes can harm blood vessels, making them more likely to block. High blood sugar damages the blood vessel lining. Managing diabetes well is key to avoiding vascular problems.
Hypertension’s Impact on Arteries
Hypertension, or high blood pressure, strains arterial walls. This speeds up blockage. Controlling blood pressure through lifestyle and medicine can lower blockage risk.
Obesity and Metabolic Syndrome
Being overweight, and metabolic syndrome, raise artery disease risk. Belly fat leads to insulin resistance, high blood pressure, and bad cholesterol. Changing lifestyle, like diet and exercise, helps manage these risks.
Chronic Kidney Disease
Chronic kidney disease (CKD) affects blood vessels. The kidneys help keep blood vessels healthy. CKD increases blockage risk. Treating CKD with medicine and lifestyle changes is vital for artery health.
Understanding and tackling these health links helps prevent and manage blockages. This approach improves blood vessel health and overall well-being.
Emerging Research and Future Directions in Arterial Disease Management
Arterial disease management is changing fast. New medical research and technology are leading the way. This research is uncovering more about arterial disease, helping us find better ways to manage it.
New Diagnostic Technologies
Recently, we’ve seen big steps forward in diagnosing arterial disease. Non-invasive imaging and biomarker testing are getting better. They help find blockages in arteries sooner and more accurately.
- Advanced ultrasound techniques
- High-resolution CT angiography
- MR angiography without contrast
These new tools are making diagnosis more precise. They also lower the risks of older, more invasive tests.
Innovative Treatment Approaches
New treatments for arterial disease are being explored. Personalized medicine is becoming more common. It means treatments are tailored to each patient’s needs. This includes:
- Targeted drug therapies
- Gene therapy for vascular diseases
- Advanced stent technologies
These new treatments offer hope for those with severe arterial disease.
Preventive Strategies on the Horizon
Prevention is key in managing arterial disease. New research is looking into new risk factors and ways to prevent them. This includes:
- Lifestyle interventions tailored to genetic predispositions
- Novel pharmacological agents for primary prevention
- Public health initiatives aimed at reducing cardiovascular risk factors
By focusing on prevention, we might see fewer cases of arterial disease.
As research keeps improving, the future for managing arterial disease looks bright. New diagnostic tools, treatments, and prevention strategies will help. Together, we can make a big difference in patient care and reduce the impact of arterial disease.
Conclusion: Taking Proactive Steps for Arterial Health
Keeping our arteries healthy is key to avoiding heart diseases. By living a healthy lifestyle and managing risks, we can lower the chance of blockages. Staying informed about the latest in managing arterial disease also helps.
Regular exercise, a balanced diet, and managing stress are important for our arteries. Knowing the signs of blockages lets us get medical help fast. This can prevent serious problems.
To stop blockages, we need a full plan. This includes controlling risks like high blood pressure and diabetes. Regular medical check-ups are also essential. By taking these steps, we can have a healthier future and lessen heart disease’s impact.
FAQ
What are the common symptoms of clogged arteries?
Symptoms include chest pain (angina), shortness of breath, and leg pain when walking. In severe cases, symptoms can be more serious and need immediate help.
How do arterial blockages develop?
Over many years, blockages form due to high cholesterol, smoking, and high blood pressure. This causes arteries to narrow and harden.
What is the difference between coronary artery disease and peripheral artery disease?
Coronary artery disease affects the heart’s arteries, causing heart symptoms. Peripheral artery disease affects the limbs, leading to leg pain when walking.
Can arterial blockages occur without noticeable symptoms?
Yes, they can happen without symptoms, known as silent arterial disease. This is risky because it can progress unnoticed until a serious event.
What are the risk factors for arterial blockage?
Risk factors include high cholesterol, smoking, and diabetes. Non-modifiable factors are age, gender, and family history.
How are clogged arteries diagnosed?
Tests include ultrasound, CT scans, and MRI. Angiography is used for more detailed views. The choice depends on the individual’s condition and history.
What are the treatment options for arterial blockages?
Treatments include medications, angioplasty, and stenting. Surgery like bypass surgery is also an option.
How can arterial disease be prevented and managed?
A healthy lifestyle is key. This includes a heart-healthy diet, exercise, stress management, and quitting smoking.
What are the symptoms of renal artery stenosis?
Symptoms include resistant hypertension, changes in urination, and fluid retention. These need prompt medical attention.
How do symptoms of arterial blockage vary between men and women?
Symptoms differ in men and women and change with age. Understanding these differences is important for diagnosis and treatment.
What are the red flag symptoms that require immediate medical attention?
Severe chest pain, sudden severe headache, difficulty speaking, and weakness on one side are red flags. They need immediate medical care.
Are there any new developments in the management of arterial disease?
Yes, research is ongoing. New diagnostic technologies, treatments, and preventive strategies are being developed.
Can managing other health conditions help in maintaining arterial health?
Yes, managing diabetes, hypertension, obesity, and chronic kidney disease is important. It helps prevent arterial blockages.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/30879355/




































