A craniotomy is a complex surgery. It involves temporarily removing a part of the skull to reach the brain. The life expectancy after this surgery can vary a lot. This depends on the reason for the surgery. Exactly What Is A Craniotomy? Learn the vital long-term facts and amazing recovery tips that lead to a safe, healthy, and happy life.
Recent studies show that older adults face different outcomes. For example, about 64% of people over 65 who have this surgery for brain injury might not live past a year.
Many things can affect how long someone lives after a craniotomy. These include the person’s age, their health before surgery, and any complications after surgery.
Key Takeaways
- Life expectancy after craniotomy varies based on the underlying condition.
- Older adults (>65 years) have a higher mortality rate within 12 months after surgery.
- Preexisting health conditions and postoperative complications affect outcomes.
- Understanding these factors is key for making informed medical decisions.
- Recent studies provide insights into the survival rates of patients post-craniotomy.
What is a Craniotomy? A Complete Overview
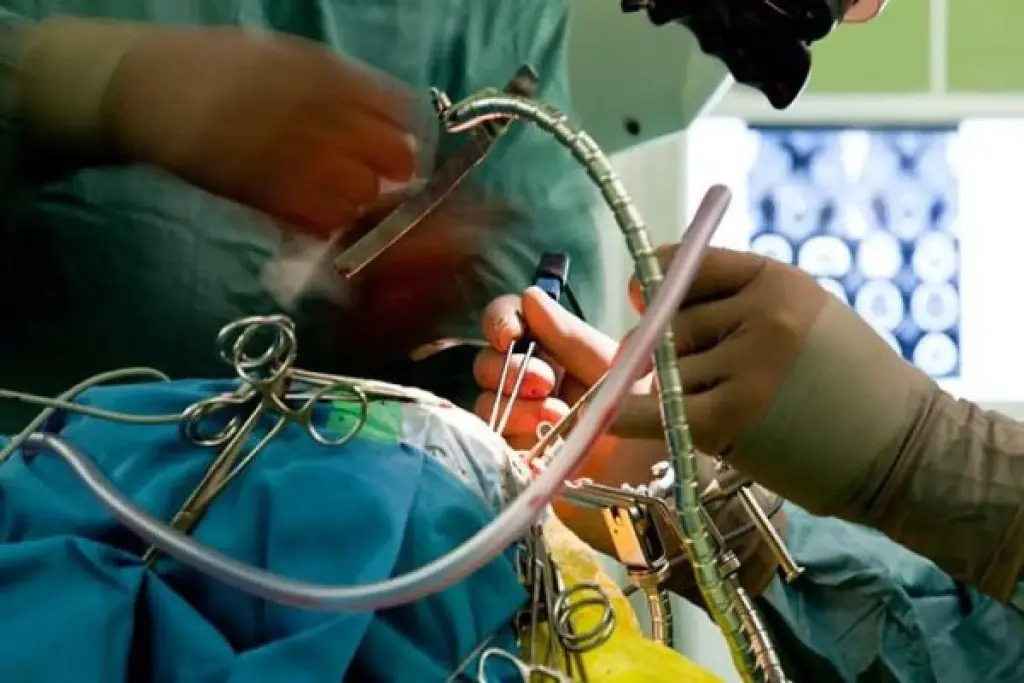
A craniotomy is a complex surgery where a part of the skull is temporarily removed to access the brain. It’s key for many neurosurgical treatments. It helps doctors diagnose and treat brain conditions.
Definition and Basic Procedure
To start, an incision is made in the scalp. Then, a section of the skull, called a bone flap, is removed to expose the brain. The surgery is done under general anesthesia for the patient’s comfort and safety.
The size and location of the craniotomy vary based on the condition being treated. This could be a tumor, aneurysm, or traumatic brain injury.
The steps of a craniotomy include:
- Making an incision in the scalp
- Retracting the scalp to expose the skull
- Drilling burr holes in the skull
- Using a craniotome to cut and remove the bone flap
- Performing the necessary surgical intervention on the brain
- Replacing the bone flap and securing it with plates or sutures
Different Types of Craniotomy Techniques
There are various craniotomy techniques, each suited for different needs:
- Standard Craniotomy: The traditional method involving a larger incision and bone flap removal.
- Keyhole Craniotomy: A minimally invasive approach using smaller incisions and a smaller bone flap.
- Decompressive Craniectomy: Removing a larger section of the skull to relieve pressure on the brain due to swelling or trauma.
- Orbitofrontal Craniotomy: Involves removing a portion of the skull behind the eye socket, often used for tumors or aneurysms in the frontal lobe.
Common Reasons for Performing a Craniotomy
Craniotomies are done for many reasons, including:
- Removing brain tumors, either benign or malignant
- Treating aneurysms or arteriovenous malformations (AVMs)
- Relieving pressure on the brain due to traumatic injury or swelling
- Draining abscesses or cysts
- Repairing cerebral vascular abnormalities
A leading neurosurgeon says, “The decision to perform a craniotomy is based on a thorough evaluation of the patient’s condition. This includes imaging studies and clinical presentation.” This shows the importance of a personalized approach to each patient’s needs.
The Craniotomy Procedure from Preparation to Recovery
For those facing a craniotomy, knowing the steps from start to finish is key. A craniotomy is a complex surgery where part of the skull is temporarily removed. It requires careful planning and execution.
Pre-Surgical Evaluation and Preparation
The journey to a craniotomy starts with a detailed pre-surgical evaluation. This includes a review of the patient’s medical history and current health. Diagnostic tests like MRI or CT scans are used to see the brain and affected area clearly. These tests help the team plan the best surgical approach.
Patients also undergo health assessments to make sure they’re ready for surgery. This may include blood tests and cardiovascular evaluations. Patient education is also important, where the team explains the procedure, risks, and recovery.
What Happens During the Surgery
On surgery day, the patient gets anesthesia to stay comfortable. The surgical team then prepares the patient by sterilizing the area and positioning them. The surgeon makes an incision in the scalp and uses a craniotome to remove a section of the skull.
The surgery aims to remove a tumor, repair an aneurysm, or relieve pressure. The team works carefully to minimize risks and achieve the best outcome. After the surgery, the bone flap is replaced, and the scalp is closed.
Immediate Post-Operative Care
After surgery, the patient goes to the ICU for close monitoring. The post-operative period is critical for managing complications and ensuring a smooth recovery. Monitoring includes neurological checks, vital sign assessment, and pain management. The team watches for any signs of complications, such as infection or swelling.
As the patient stabilizes, they move to a regular hospital room. Here, the focus is on continued recovery and preparation for discharge. Rehabilitation may start during the hospital stay, with therapists helping the patient regain strength and functionality.
Life Expectancy Statistics: General Survival Rates After Craniotomy
Looking at survival rates after craniotomy gives us important insights. The life expectancy after this surgery varies a lot. This depends on the condition being treated, the patient’s health, and the surgery method.
Mortality Rates
Mortality rates after craniotomy show the surgery’s risks. Studies show these rates vary a lot. For example, older adults with traumatic brain injuries face higher mortality rates after decompressive craniectomy.
|
Condition |
Short-Term Mortality Rate |
Long-Term Mortality Rate |
|---|---|---|
|
Traumatic Brain Injury |
15% |
30% |
|
Brain Tumor |
5% |
20% |
|
Aneurysm/ Vascular Conditions |
10% |
25% |
Survival Rates by Condition Type
The survival rate after craniotomy depends a lot on the condition. For instance, patients with brain tumors have different survival rates than those with traumatic brain injuries or vascular conditions.
Brain Tumor: Survival rates for brain tumors depend on the tumor type and grade. Patients with benign tumors usually have better survival rates than those with malignant tumors.
Traumatic Brain Injury: TBI patients face a guarded prognosis. Their survival rates are influenced by age, initial Glasgow Coma Scale (GCS) score, and other injuries.
Short-Term Versus Long-Term Survival Considerations
It’s important to look at short-term and long-term survival rates after craniotomy. Short-term survival is up to 30 days post-surgery. Long-term survival is over a year after surgery.
Short-term survival is affected by surgery success, post-operative complications, and pre-operative health. Long-term survival depends on the condition, age, and ability to recover and rehabilitate.
Knowing these statistics helps patients and families make better care decisions and set realistic expectations.
Traumatic Brain Injury Craniotomy Outcomes and Life Expectancy
Patients who have a craniotomy for traumatic brain injury face different outcomes. These depend on the injury’s severity, the patient’s age, and the surgery type.
Decompressive Craniectomy Survival Rates
Decompressive craniectomy helps relieve brain pressure from TBI. But, survival rates vary a lot. For example, about 64% of people over 65 die within a year after this surgery.
Survival Rates After Decompressive Craniectomy
|
Age Group |
Survival Rate at 6 Months |
Survival Rate at 12 Months |
|---|---|---|
|
<40 years |
70% |
60% |
|
40-65 years |
50% |
40% |
|
>65 years |
36% |
24% |
Age-Related Outcomes in TBI Patients
Age is key in TBI outcomes. Older patients often do worse because of less health reserve and more health issues. Younger patients usually recover better, but it depends on the injury’s severity.
Functional Recovery and Quality of Life After TBI Craniotomy
Recovery and quality of life are important for patients and their families. Some patients recover well, while others face lasting disabilities. Rehabilitation helps a lot, focusing on getting back cognitive and physical skills.
Rehabilitation Strategies include physical, occupational, and speech therapy. These are customized for each patient. The aim is to increase independence and improve life quality.
Brain Tumor Craniotomy: Survival Rates and Prognosis
Patients with brain tumors who have surgery are worried about their future. The surgery’s success depends on many things. These include the tumor’s type and how much of it was removed, and the patient’s health.
Outcomes for Benign Versus Malignant Tumors
The type of tumor greatly affects the patient’s chances. Benign tumors grow slower and are less likely to spread. On the other hand, malignant tumors grow faster and can shorten life if not treated well.
- Patients with benign tumors usually live longer and have a better life after surgery.
- Those with malignant tumors face tougher challenges, with survival rates depending on the tumor’s grade and other factors.
Survival Rates by Tumor Type and Grade
Survival rates after surgery depend on the tumor’s type and grade. For example, people with low-grade gliomas tend to do better than those with high-grade gliomas. Knowing this helps set realistic hopes and plan for after surgery.
|
Tumor Type |
Typical Survival Rate |
|---|---|
|
Low-Grade Glioma |
5-10 years or more |
|
High-Grade Glioma |
1-3 years |
|
Meningioma (Benign) |
High survival rate, often cured with surgery |
Impact of Complete Versus Partial Tumor Resection
How much of the tumor is removed affects the outcome. Complete resection leads to better survival chances and less chance of the tumor coming back. Partial resection might be needed for tumors near important brain areas, leaving some tumor cells behind.
Role of Adjuvant Therapies in Extending Life Expectancy
Adjuvant therapies like radiation and chemotherapy are key in fighting remaining tumor cells. These treatments are chosen based on the tumor’s type, grade, and how much was removed. Surgery plus these therapies can give patients a better chance at living longer and enjoying life more.
Aneurysm and Vascular Condition Craniotomy Outcomes
Outcomes for aneurysm surgery vary a lot. This depends on if the aneurysm has ruptured or not. Doctors carefully consider the patient’s health, the aneurysm’s details, and the risks and benefits of surgery before deciding on a craniotomy.
Survival Rates for Ruptured Versus Unruptured Aneurysms
Patients with ruptured aneurysms face a tougher road. Those with unruptured aneurysms tend to have better chances of survival. This is because unruptured aneurysms are less urgent and often easier to treat.
For unruptured aneurysms, surgery is usually successful, with a low death rate of 1% to 5%. But, ruptured aneurysms are more deadly, with a 20% to 40% chance of death within 30 days.
|
Aneurysm Status |
Mortality Rate |
Survival Rate |
|---|---|---|
|
Unruptured |
1-5% |
95-99% |
|
Ruptured |
20-40% |
60-80% |
Long-Term Prognosis After Successful Repair
After a successful surgery, patients face a mixed bag of outcomes. The patient’s age, health, and any other diseases play big roles. The aneurysm’s size and location also matter.
Patients who get their aneurysms treated can see a big drop in rupture risk. This improves their chances of living longer. But, other health issues can affect how long they live.
Risk of Recurrence and Its Impact on Life Expectancy
How likely an aneurysm is to come back is a big worry. The risk depends on the treatment used. Some treatments might have a higher chance of failure.
For those with ruptured aneurysms, the risk of it happening again is a big concern. This can shorten their life. Regular check-ups are key to catching any problems early.
Key Factors Influencing Life Expectancy After Aneurysm Surgery:
- Initial aneurysm rupture status
- Presence of comorbid conditions
- Age and overall health of the patient
- Effectiveness of the initial treatment
- Risk of recurrence
How Age Impacts Craniotomy Outcomes and Survival
Craniotomy results change a lot with age because of health differences. The success of a craniotomy and how long a patient lives depend on many things. Age is a big factor.
Physiological Factors Affecting Recovery in Different Age Groups
How well someone recovers from a craniotomy varies with age. Young people usually do better because they are healthier. Older adults might face more problems like less energy to heal and other health issues.
Key physiological factors influencing recovery include:
- Cardiovascular health: Older people are more likely to have heart problems, making surgery and recovery harder.
- Neurological resilience: Younger brains might recover better from brain surgery.
- Immune system function: Both very young and older patients might have weaker immune systems, making it harder to fight off infections.
Special Considerations for Pediatric Craniotomy Patients
Pediatric patients face special challenges with craniotomy. Their growing brains and bodies need careful handling to avoid lasting effects.
Key considerations for pediatric craniotomy include:
- Developmental stage: The child’s age at surgery can affect how they do.
- Surgical technique: Neurosurgeons need to adjust their methods for the child’s size and shape.
- Post-operative care: Kids need special care after surgery that fits their needs.
Geriatric Craniotomy Outcomes and Life Expectancy
Geriatric patients, those over 65, often have more health issues. Age is a factor, but it’s not the only thing that decides survival or quality of life after surgery.
Factors influencing geriatric craniotomy outcomes include:
- Comorbid conditions: Older adults often have many health problems that can affect recovery.
- Pre-operative health status: The patient’s health before surgery is very important for outcomes.
- Surgical and anesthetic techniques: Newer methods have helped improve results for older patients.
In conclusion, age greatly affects how well someone does after a craniotomy and how long they live. Each age group has its own challenges and needs. Knowing these helps doctors give better care and improve long-term results.
Pre-Existing Health Conditions and Their Effect on Post-Craniotomy Survival
Having pre-existing health conditions can greatly affect survival rates after a craniotomy. People with health issues are more likely to face complications during and after surgery.
Cardiovascular Comorbidities
Heart diseases like high blood pressure and coronary artery disease are common. They can make surgery outcomes worse. These conditions raise the risk of heart problems during the operation.
Table 1: Impact of Cardiovascular Comorbidities on Craniotomy Outcomes
|
Comorbidity |
Risk Level |
Management Strategy |
|---|---|---|
|
Hypertension |
High |
Pre-operative blood pressure control |
|
Coronary Artery Disease |
High |
Pre-operative cardiac evaluation |
Diabetes and Metabolic Disorders
Diabetes can also impact recovery after a craniotomy. Uncontrolled blood sugar can cause infections and slow healing.
- Pre-operative optimization of blood glucose levels is key.
- It’s important to watch for complications after surgery.
Immunocompromised States and Infection Risk
Those with weakened immune systems, like HIV/AIDS patients or those on long-term immunosuppressants, face a higher risk of infections after surgery.
Neurological Comorbidities
Existing neurological conditions, such as past strokes or neurodegenerative diseases, can also impact outcomes. These conditions may make post-operative care and rehabilitation more challenging.
Managing these conditions is vital to improve survival rates after a craniotomy. A thorough pre-operative check-up and a detailed post-operative care plan can help reduce risks related to pre-existing health conditions.
Post-Operative Complications Affecting Life Expectancy
Complications after a craniotomy can greatly affect a patient’s life. These issues come from the surgery, the patient’s health before surgery, and care after surgery.
Infection Risks and Management
Infections are a big risk after a craniotomy. They can lead to serious problems if not treated quickly. Meningitis and surgical site infections are common types.
To manage these infections, doctors often use antibiotic therapy. Sometimes, they need to do more surgery to fix the infection.
|
Type of Infection |
Common Causes |
Management Strategies |
|---|---|---|
|
Meningitis |
Bacterial contamination during surgery |
Antibiotic therapy, supportive care |
|
Surgical Site Infections |
Contamination of the surgical site |
Antibiotics, possible surgical debridement |
Neurological Complications
Neurological problems can greatly affect a craniotomy’s outcome. Issues like stroke, cerebral edema, and seizures can happen.
It’s important to quickly spot and treat these problems. This might mean watching the patient’s brain health, controlling swelling, and giving drugs to stop seizures.
Systemic Complications
Systemic problems, like deep vein thrombosis (DVT) and pulmonary embolism, can also occur. These usually happen because the patient is not moving much.
To prevent these, doctors might start moving the patient early. They also use anticoagulant prophylaxis for those at high risk.
|
Systemic Complication |
Risk Factors |
Prevention Strategies |
|---|---|---|
|
DVT |
Prolonged immobilization, surgery |
Early mobilization, anticoagulant prophylaxis |
|
Pulmonary Embolism |
DVT, immobilization |
Early mobilization, anticoagulant prophylaxis |
Recovery Timeline and Rehabilitation Impact on Long-Term Survival
The path to recovery after a craniotomy has key milestones for long-term survival. Knowing these milestones and the importance of rehabilitation can greatly affect patient results.
Typical Recovery Milestones After Craniotomy
Recovery from a craniotomy is a slow process that differs for everyone. First, patients are watched closely in the ICU for any immediate problems. Once they get better, they move to a regular ward for more care.
Important recovery milestones include:
- Regaining consciousness and initial neurological recovery
- Gradual improvement in cognitive functions
- Physical rehabilitation to regain strength and mobility
- Follow-up appointments to monitor healing and address any complications
Importance of Rehabilitation for Optimal Outcomes
Rehabilitation is key in the recovery after a craniotomy. A good rehabilitation plan can help patients get back lost functions, improve their life quality, and increase long-term survival chances.
Rehabilitation after craniotomy involves a team of healthcare experts. This team includes physical, occupational, and speech therapists. Their goal is to help patients reach their highest level of independence and function.
|
Rehabilitation Component |
Description |
Benefits |
|---|---|---|
|
Physical Therapy |
Helps patients regain strength, mobility, and balance |
Improves overall physical function and reduces the risk of falls |
|
Occupational Therapy |
Assists patients in performing daily activities and tasks |
Enhances independence and quality of life |
|
Speech Therapy |
Addresses communication and swallowing disorders |
Improves communication skills and reduces the risk of aspiration |
Signs of Favorable Versus Concerning Recovery
It’s important to watch how recovery is going to spot any issues early. Good signs include steady improvements in brain function, thinking, and physical strength.
Bad signs might be:
- Worsening neurological deficits
- Increased confusion or decreased level of consciousness
- Signs of infection, such as fever or redness around the surgical site
Long-Term Follow-Up Requirements
Long-term care after a craniotomy is vital. Regular visits with healthcare providers help catch late problems, manage ongoing conditions, and adjust rehab plans as needed.
Long-term follow-up includes office visits, imaging, and lab tests. These help make sure the patient stays on the right recovery path.
Quality of Life Considerations After Craniotomy
Life after a craniotomy is complex. It involves physical, cognitive, and emotional recovery. It’s important to know what affects a person’s quality of life.
Cognitive and Functional Outcomes
Outcomes after a craniotomy can differ a lot. Some people might fully recover, while others face challenges. These can include memory problems, trouble concentrating, or physical disabilities.
- Cognitive Challenges: Patients might struggle with memory, attention, or processing information.
- Functional Recovery: The ability to regain strength and do daily tasks can vary.
Many factors influence these outcomes. These include why the craniotomy was needed, the patient’s health, and any complications after surgery.
Return to Daily Activities and Work
Going back to daily life and work is a big step in recovery. The time it takes can vary a lot. It depends on the person’s condition and their job.
- Some people might get back to normal in a few weeks.
- Others might need more time, like if their job is physically demanding or stressful.
Psychological Impact and Adjustment
The psychological effects of a craniotomy are significant. Patients can feel a range of emotions. These can include anxiety, depression, relief, or gratitude.
Adjusting to life after a craniotomy is more than just physical recovery. It also involves emotional and psychological healing.
Social Support and Its Role in Recovery
Social support is key in recovery. A strong network of family, friends, and healthcare professionals can greatly help. They can improve a patient’s outcomes.
- Emotional support helps patients deal with the surgery’s psychological effects.
- Practical support, like help with daily tasks, can ease the recovery burden.
Understanding these aspects helps patients and their families face the challenges and opportunities of life after a craniotomy.
Modern Advances Improving Craniotomy Outcomes and Survival
New medical technologies have greatly improved craniotomy results. These advancements have made surgeries more precise and helped patients recover faster. They have also led to higher survival rates.
Minimally Invasive Techniques
Minimally invasive craniotomy has changed neurosurgery. It uses smaller incisions and less tissue damage. This means less pain for patients and quicker healing times.
Research shows that minimally invasive craniotomy leads to fewer complications. It’s good for patients with certain brain tumors or vascular issues.
A study on the National Center for Biotechnology Information website talks about these benefits. It shows how these techniques can cut down recovery time and boost survival rates.
Intraoperative Monitoring and Mapping
Intraoperative monitoring and mapping are key in modern neurosurgery. They let surgeons watch brain function live during surgery. This helps them make better decisions and avoid harming important brain areas.
“The integration of intraoperative monitoring has been a game-changer in neurosurgery, allowing for more precise and safer surgeries.” – A Neurosurgeon
Post-Operative Care Improvements
Improvements in post-operative care have also helped. Better post-operative care includes better pain management and infection control. This has lowered the risk of complications and death.
Rehabilitation programs tailored to each patient have also improved survival and quality of life. They focus on helping patients recover fully.
Emerging Technologies in Cranial Surgery
New technologies like robotics and artificial intelligence are starting to impact cranial surgery. They promise to make surgeries even more precise and effective. For example, robotic-assisted surgery offers greater control and precision during complex operations.
|
Technology |
Description |
Potential Benefit |
|---|---|---|
|
Robotic-Assisted Surgery |
Utilizes robotic systems to enhance surgical precision |
Improved accuracy and control during complex procedures |
|
Artificial Intelligence |
Applies AI algorithms to analyze data and support surgical decisions |
Enhanced diagnostic capabilities and personalized treatment plans |
Conclusion: Key Factors Determining Life Expectancy After Craniotomy
Life expectancy after a craniotomy depends on many things. These include the reason for the surgery, the patient’s age, and any complications after surgery.
It’s important for patients and their families to understand these factors. The patient’s health, how severe their condition is, and how well they respond to treatment all matter. These factors help determine how long they might live after a craniotomy.
Thanks to better surgery techniques and care after surgery, outcomes have gotten much better. Healthcare providers can make treatment plans better by knowing these key factors. This helps patients get the best results from their craniotomy.
FAQ
What is a craniotomy?
A craniotomy is a surgery where a part of the skull is removed. This lets surgeons work on the brain. They can remove tumors, fix aneurysms, or ease brain pressure.
What is the purpose of a craniotomy?
The main goal of a craniotomy is to give surgeons a way to reach the brain. They can then diagnose and treat conditions like tumors, vascular issues, and injuries.
What are the different types of craniotomies?
There are several types of craniotomies. These include traditional, keyhole, and decompressive craniectomy. The choice depends on the condition and the patient’s health.
How long does a craniotomy surgery take?
The time needed for a craniotomy surgery varies. It can last from 2 to 6 hours or more. This depends on the procedure’s complexity and the condition being treated.
What is the recovery time after a craniotomy?
Recovery time after a craniotomy varies. It depends on the patient’s health, the surgery’s complexity, and any complications. Patients usually spend several days to weeks in the hospital and months recovering.
What are the risks associated with a craniotomy?
Craniotomy carries risks like infection, bleeding, stroke, and neurological damage. These risks vary based on the patient’s health and the surgery type.
How does age impact craniotomy outcomes?
Age can affect craniotomy outcomes. Older adults face higher risks and may have poorer recovery. But, individual outcomes also depend on health and comorbidities.
What is the life expectancy after a craniotomy for a brain tumor?
Life expectancy after a craniotomy for a brain tumor varies. It depends on the tumor type and grade, surgery success, and any additional treatments. Benign tumors usually have better outcomes than malignant ones.
Can pre-existing health conditions affect survival after a craniotomy?
Yes, pre-existing health conditions can impact survival after a craniotomy. Conditions like cardiovascular disease, diabetes, and weakened immune systems increase risks and affect recovery.
What are the signs of favorable versus concerning recovery after a craniotomy?
Good signs of recovery include improving neurological function, reduced symptoms, and more independence. Bad signs include worsening function, seizures, or infection signs.
How do modern advances impact craniotomy outcomes?
Modern advances have improved craniotomy outcomes. Techniques like minimally invasive surgery, intraoperative monitoring, and better care have reduced complications and increased survival rates.
What is the role of rehabilitation after a craniotomy?
Rehabilitation is key after a craniotomy. It helps patients regain functions and adapt to changes. This improves their quality of life.
How does a craniotomy affect quality of life?
A craniotomy’s impact on quality of life varies. It depends on the condition, surgery success, and any lasting effects. Many patients can return to daily activities, while others need ongoing support.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/17303538/


































