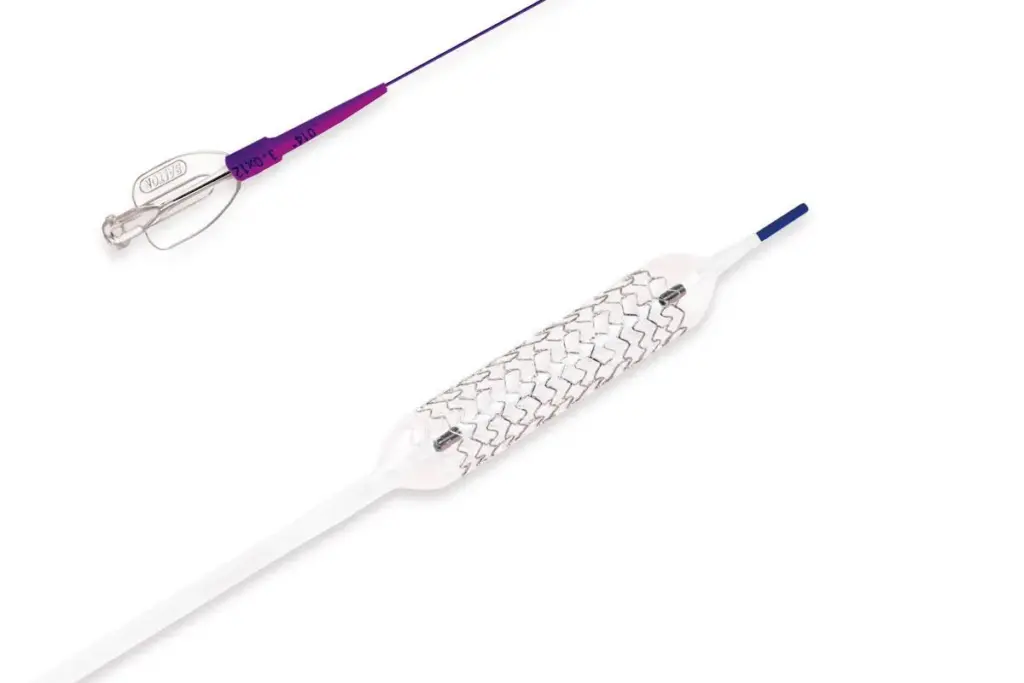
Over 3.7 million Americans have an implantable cardioverter-defibrillator (ICD). This device helps control serious heart rhythm problems. Knowing what to avoid is key for those with an ICD.
An ICD is a small device under the skin. It sends electric currents for abnormal heart rhythms, or arrhythmia symptoms. It greatly improves life for many, but there are important precautions and lifestyle changes to make.
What is a pacemaker vs defibrillator? Get best avoidance tips. Strong magnets are dangerous. Keep your vital device safe and functional.
Key Takeaways
- Learn how an ICD works and its role in managing heart rhythm.
- Know the risks and complications of ICDs.
- Understand the lifestyle changes after getting an ICD.
- See why follow-up care and device monitoring are critical.
- Know how to handle ICD discharges or shocks.
Understanding Defibrillators and Their Life-Saving Role
Defibrillators, like AEDs, ICDs, and WCDs, are key in fighting heart arrhythmias. They help fix dangerous heart rhythms that can cause sudden cardiac arrest.
Types of Defibrillators: AEDs, ICDs, and WCDs
There are many defibrillators, each with its own role in heart care. Automated External Defibrillators (AEDs) are for emergencies. They guide non-professionals through voice prompts. Implantable Cardioverter-Defibrillators (ICDs) are implanted to watch the heart and shock it when needed. Wearable Cardioverter Defibrillators (WCDs) are worn by those at risk of sudden cardiac arrest. They offer protection without surgery.
How Defibrillators Detect and Correct Dangerous Heart Rhythms
Defibrillators keep an eye on the heart’s electrical activity. If they find a bad rhythm, they send a shock to fix it. This can save lives in cardiac arrest.
Modern defibrillators, like ICDs, are smart. They can tell different arrhythmias apart and treat them right. They might pace or cardiovert, not just defibrillate.
Defibrillators use cool tech to spot arrhythmias. They’re set up to give the right treatment at the right time. This helps save lives in emergencies.
The Critical Differences Between Defibrillators and Pacemakers
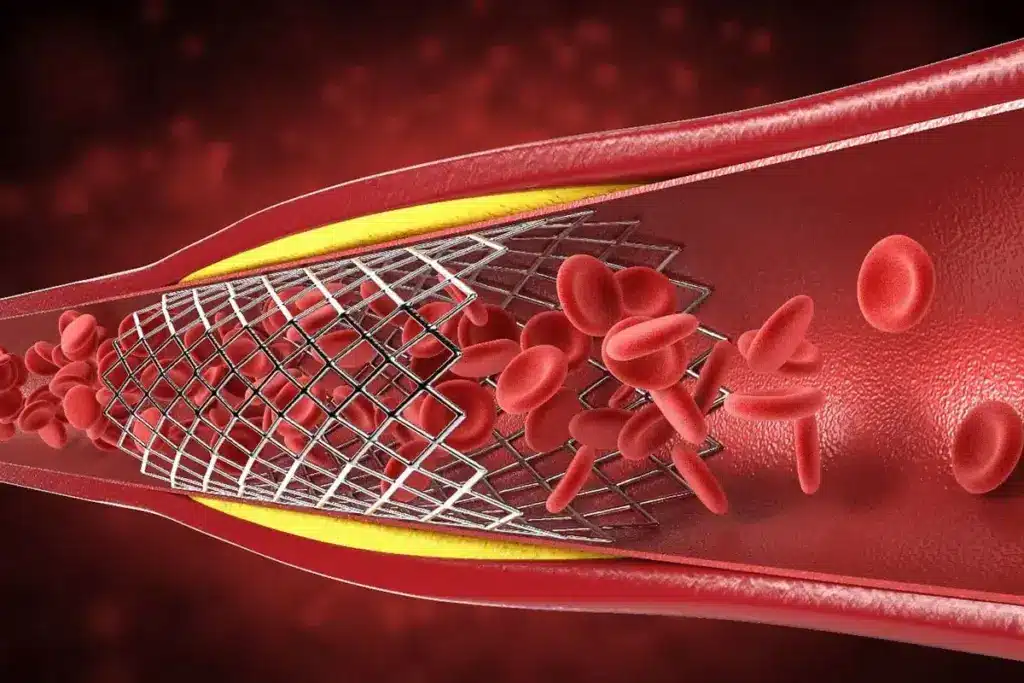
Defibrillators and pacemakers are both used for heart issues, but they work in different ways. They help manage irregular heartbeats, but they treat different conditions. Their functions and uses are unique.
Emergency Shock vs. Continuous Rhythm Regulation
Defibrillators give emergency shocks to the heart for serious arrhythmias. This shock helps get a normal heartbeat back. Pacemakers, on the other hand, keep the heart rate steady by sending electrical impulses. They help when the heart beats too slow.
Key differences in their operation include:
- Defibrillators are mainly for emergency use to fix dangerous heart rhythms.
- Pacemakers manage heart rhythm all the time to keep the heart rate right.
When Each Device Is Medically Indicated
Choosing between a defibrillator and a pacemaker depends on the heart condition. Defibrillators are for those at risk of sudden cardiac arrest. Pacemakers are for slow heart rates or heart block.
Medical indications for each device are based on:
- The type and severity of the arrhythmia.
- The patient’s overall heart health and medical history.
Patients Who May Need Both Devices
Some patients need both a defibrillator and a pacemaker. For example, someone with ventricular tachycardia might need a defibrillator. They might also need a pacemaker for a steady heart rate.
Living with cardiac devices can be tough, but knowing their roles helps. We aim to clarify the differences. This way, patients can make better choices for their heart health.
What Is a Pacemaker and How Does It Regulate Heart Rhythm?
A pacemaker is a small device that helps control the heart’s rhythm. It manages irregular heartbeats, keeping the heart rate steady and right.
Pacemaker Components and Functionality
A pacemaker has two key parts: the pulse generator and the leads. The pulse generator is a small metal box with a battery and electronics. It sends electrical impulses to the heart.
The leads are insulated wires that connect the pulse generator to the heart. They deliver the impulses to the right chambers.
The pacemaker works by checking the heart’s rhythm and stepping in when it’s off. If the heart beats too slow or irregularly, it sends signals to fix it. Modern pacemakers can even adjust the heart rate during exercise.
Single-Chamber, Dual-Chamber, and Biventricular Pacemakers
There are different types of pacemakers for various heart issues. Single-chamber pacemakers have one lead in the right atrium or ventricle. Dual-chamber pacemakers have two leads, one in each chamber, for better pacing.
Biventricular pacemakers, or CRT devices, have three leads. They pace both ventricles and the atrium, helping with heart failure.
|
Type of Pacemaker |
Description |
Primary Use |
|---|---|---|
|
Single-Chamber |
One lead in either atrium or ventricle |
Basic pacing needs |
|
Dual-Chamber |
Two leads, one in atrium and one in ventricle |
More coordinated pacing |
|
Biventricular |
Three leads, pacing both ventricles and atrium |
Heart failure treatment |
The Implantation Procedure and Recovery Process
The pacemaker implantation involves a small chest incision. The device and leads are inserted through this incision. The procedure is done under local anesthesia, and the device is set to meet the patient’s needs.
After the procedure, patients are watched for any immediate issues. The recovery is usually easy. Some discomfort or bruising at the site may occur but it fades in a few days.
Most people can go back to their usual activities in a week. But, they should avoid hard activities for a bit longer.
“The implantation of a pacemaker is a relatively minor surgical procedure that can significantly improve the quality of life for individuals with certain heart conditions.”
A Cardiologist
It’s important to have follow-up care to make sure the pacemaker works right. Regular visits to a cardiologist help monitor the device and make any needed adjustments.
Cardiac Arrhythmias That May Require Defibrillator Intervention
Cardiac arrhythmias are conditions that might need a defibrillator to fix the heart’s rhythm. These happen when the heart’s electrical system goes wrong. This can cause heartbeats that are too fast, too slow, or irregular.
Ventricular Fibrillation and Ventricular Tachycardia
Ventricular fibrillation (VF) and ventricular tachycardia (VT) are serious arrhythmias that might need a defibrillator. VF makes the heart’s ventricles quiver fast and erratically. VT causes a fast, regular heartbeat from the ventricles. Both can lead to sudden cardiac arrest if not treated quickly.
“Using an implantable cardioverter-defibrillator (ICD) can greatly lower death rates in those at high risk of VF and VT,” studies show.
Atrial Fibrillation With Rapid Ventricular Response
Atrial fibrillation (AFib) with rapid ventricular response (RVR) is another arrhythmia that needs careful management. AFib is the most common sustained cardiac arrhythmia, with rapid and irregular heart rhythms. When it has RVR, it can cause symptoms like palpitations, shortness of breath, and fatigue.
AFib with RVR isn’t usually treated with a defibrillator directly. But, patients with this condition might be at higher risk for other arrhythmias that could need a defibrillator.
Sudden Cardiac Arrest Risk Factors
Sudden cardiac arrest (SCA) is a sudden loss of heart function, often due to VF or VT. Several factors increase SCA risk, including heart disease, previous heart attack, family history of SCA, and certain genetic conditions.
Knowing these risk factors is key to deciding if a defibrillator is needed. Patients at high risk of SCA may benefit from an ICD to prevent fatal outcomes.
As we learn more about cardiac arrhythmias and their treatment, defibrillators play a vital role in saving lives and improving patient outcomes.
Strong Electromagnetic Fields: Primary Hazards to Avoid
Strong electromagnetic fields can mess with implantable defibrillators, which is a big risk. These fields come from things like high-voltage power lines, industrial gear, and MRI machines.
High-Voltage Power Lines and Electrical Substations
High-voltage power lines and substations are big sources of strong electromagnetic fields. The risk is higher near them, but it depends on several things. This includes the voltage and how close you are to the source.
To stay safe, patients with defibrillators should:
- Avoid hanging out near high-voltage power lines or substations.
- Keep a safe distance when walking or standing near these spots.
Industrial Equipment and Welding Machinery
Places with industrial equipment, like welding machines and big motors, have strong electromagnetic fields. People with defibrillators should be careful in these areas.
Here are some safety tips:
- Talk to your doctor about safe work practices.
- Let your employer know about your condition and what precautions you need.
- Wear personal protective gear if it’s recommended.
MRI Machines and Compatibility Considerations
MRI machines have very strong magnetic fields. These can mess with or even damage an implantable defibrillator. If you have a defibrillator, tell your doctor and the MRI place before you go.
Here are some important things to think about for MRI safety:
|
Consideration |
Description |
|---|---|
|
Device Compatibility |
Not all defibrillators can go near MRI machines. Check your device’s specs. |
|
Pre-MRI Checks |
Your doctor might need to do checks or adjust your device before the MRI. |
|
Monitoring During MRI |
You might need to be watched closely during the MRI. |
By knowing these risks and taking the right steps, people with implantable defibrillators can avoid problems with strong electromagnetic fields.
Everyday Electronics and Appliances: Safe Usage Guidelines
Having a defibrillator means knowing how to use common household devices safely. These devices are usually safe, but some precautions are needed. This ensures your defibrillator works right.
Cell Phones, Tablets, and Wireless Devices
Mobile devices are everywhere today and are mostly safe for defibrillator users. But, it’s wise to:
- Keep your cell phone at least 6 inches away from your defibrillator implant site.
- Avoid carrying your phone in a breast pocket over the device.
- Use the ear on the opposite side of your body from the implant when on a call.
These steps help avoid electromagnetic interference (EMI) from your phone affecting your defibrillator.
Household Appliances and Power Tools
Most household appliances and power tools are safe when used as usual. But, to avoid EMI:
- Maintain a safe distance from appliances like microwaves and induction cooktops.
- Use power tools as intended, and avoid direct contact with the device’s electrical components.
- Be cautious with high-powered devices like electric drills and saws.
If you feel unusual symptoms or your device malfunctions while using these appliances, turn them off. Then, talk to your healthcare provider.
Smart Home Devices and Wireless Charging Systems
Smart home technology and wireless charging systems are becoming more common. They are usually safe when used correctly. But, remember:
- Be aware of the possible EMI from devices like smart speakers and wireless charging pads.
- Follow the manufacturer’s guidelines for safe use.
- If you notice any issues with your defibrillator, report them to your healthcare provider.
By being careful with how you use these devices, you can avoid risks. This way, you can enjoy the benefits of modern technology.
Physical Activities and Sports Restrictions After Implantation
People with defibrillators can stay active, but they need to be careful with some sports and activities. It’s important to know how these activities affect defibrillator patients. This ensures their safety and well-being.
Contact Sports and High-Impact Activities to Avoid
Contact sports and high-impact activities can be risky for those with defibrillators. These activities might harm the device or cause unnecessary shocks. Here are some activities to avoid:
- Contact sports like football, rugby, or hockey
- High-impact aerobics or gymnastics
- Activities with a high risk of collision or falls
It’s key for patients to talk to their healthcare provider about their activities. This helps understand the risks.
Safe Exercise Options and Cardiac Rehabilitation
While some activities are not recommended, many patients can do safe exercises. Cardiac rehabilitation programs also help. These programs improve strength, heart health, and adjust to the condition.
Safe exercises include:
- Brisk walking or jogging
- Swimming or water aerobics
- Cycling or using a stationary bike
Cardiac rehabilitation offers exercise, heart-healthy education, and stress management. It’s made for each person’s needs and abilities.
Returning to Physical Activity: Timeline and Precautions
The time to start physical activities after a defibrillator implant varies. It depends on the person’s health and the procedure details. Usually, patients are told to avoid hard activities for a few weeks.
Before starting activities, patients should:
- Consult with their healthcare provider for advice
- Slowly increase activity to avoid sudden strain
- Watch their body’s reaction to exercise and report any unusual symptoms
By following these steps and being cautious, patients with defibrillators can enjoy an active life safely.
Travel Considerations for Defibrillator Patients
Traveling with a defibrillator needs careful planning and knowing possible risks. We know travel is a big part of life. With the right steps, people with a defibrillator can travel safely.
Airport Security Procedures and Body Scanners
When going through airport security, tell the staff about your defibrillator. Carry your device ID card and be ready to explain your device. Some security scanners might affect your device. If worried, ask for a hand search or other screening.
Tips for Airport Security:
- Notify security personnel about your defibrillator before screening.
- Carry your device ID card and medical documentation.
- Be prepared for possible extra screening.
Air Travel Safety and High Altitude Concerns
Air travel is usually safe for defibrillator users. But, check with your airline for any special rules. High altitudes might affect your device, but most flights are safe. Talk to your doctor before going to high places.
International Travel: Medical Documentation and Device ID Card
For international trips, having the right medical papers is key. Carry a device ID card, a letter from your doctor, and medical records. This helps in emergencies abroad. Also, look up local healthcare and register with your country’s travel service.
Before you travel, ensure you have:
- A valid device ID card.
- A letter from your healthcare provider.
- Relevant medical records and contact information.
Medical and Dental Procedures Requiring Special Precautions
People with implantable defibrillators need to be careful during some medical and dental treatments. This is to keep the device working right and keep them safe.
Radiation Therapy and Imaging Studies
Radiation therapy can mess with implantable defibrillators. It’s key to tell your radiation oncologist about your defibrillator.
- Talk to your cardiologist and radiation oncologist about your treatment plan to lower risks.
- Make sure the radiation therapy team knows about your defibrillator.
- Some imaging studies, like MRI, might need special care or different methods.
Electrocautery During Surgical Procedures
Electrocautery is used in surgeries to cut or stop bleeding. But it can mess with a defibrillator’s work.
Precautions include:
- Use bipolar electrocautery instead of monopolar to cut down on interference.
- Avoid long or strong electrocautery near the defibrillator.
- Check the defibrillator’s work before and after surgery.
Dental Equipment and Electromagnetic Interference
Some dental tools can make electromagnetic fields that might affect defibrillators.
- Tell your dentist about your defibrillator and its type.
- Talk about risks and what to do with your dentist.
- Some dental work might need changes to the defibrillator’s settings or extra watching.
By being careful and talking to your healthcare team, people with implantable defibrillators can stay safe during medical and dental visits.
Warning Signs of Defibrillator Malfunction or Complications
Having an implantable defibrillator means you need to watch for problems. These devices save lives but can sometimes have issues. We’ll talk about the signs that might mean your defibrillator is not working right.
Unexpected Shocks or Failure to Deliver Therapy
Getting an unexpected shock is a big warning sign. Or not getting a shock when you need it is also a problem. If this happens, you should see a doctor right away.
Here are some examples to help you understand:
- Getting many shocks in a row
- Feeling a shock that feels different
- Not getting a shock when your heart is in danger
Infection Symptoms Around the Implant Site
Infections can happen where the device is implanted. It’s important to catch the signs early. Look for redness, swelling, warmth, or discharge. You might also feel feverish, have chills, or just not feel well.
If you see any of these signs, call your doctor fast. Catching an infection early can stop it from getting worse.
|
Symptom |
Description |
Action |
|---|---|---|
|
Redness and Swelling |
Increased redness or swelling around the implant site |
Contact healthcare provider |
|
Fever |
Elevated body temperature |
Seek medical attention |
|
Drainage |
Unusual discharge or fluid around the implant site |
Consult doctor immediately |
When to Seek Emergency Medical Attention
Knowing when to go to the emergency room is key. If you have any of these issues, don’t wait:
- Many shocks that shouldn’t happen
- Severe symptoms like chest pain, dizziness, or trouble breathing
- Signs of infection like we talked about
Being quick to notice and act on these signs can help a lot. Always talk to your doctor if you’re worried about your device or notice anything odd.
Defibrillator Maintenance and Battery Considerations
Keeping your defibrillator in good shape is key to your safety. It’s not just about checking the device. It’s about making sure it works right. There are several important steps to follow.
Battery Lifespan and Monitoring
The battery is a vital part of your defibrillator. Its life span depends on the model and how much you use it. Usually, a defibrillator battery lasts 5 to 7 years. It’s important to keep an eye on it to know when it needs to be replaced.
Your healthcare team will set up appointments to check the battery and the device. They will use the device to get info on its status. This helps them catch any problems early.
The Generator Replacement Procedure
When the battery is almost out, you’ll need to replace the generator. This is a surgery that changes the battery and the electronics. The surgery is usually done under local anesthesia and takes 1-2 hours.
While the surgery is safe, there are risks. These include infection or damage to the leads. Your healthcare team will talk to you about these risks and how they plan to avoid them.
Remote Monitoring Systems and Regular Check-ups
Many defibrillators today have remote monitoring. This lets your healthcare team check on the device from afar. This can spot problems early and alert your healthcare provider. It makes it easier for you to manage your device.
Even with remote monitoring, you’ll need to see your healthcare team in person. These visits let them check your device and health fully. They will decide how often you need to come in.
Psychological Aspects of Living With an Implantable Defibrillator
Having an implantable defibrillator can change your life, bringing relief and new challenges. The device is key to keeping your heart healthy. But it also brings emotional and psychological issues.
Coping With Shock Anxiety and Device Dependence
One big challenge is shock anxiety—the fear of getting a sudden shock. This fear can really affect your daily life and happiness. Also, you might feel like you’re always waiting for the device to act.
It’s important to find ways to deal with these feelings. Things like cognitive-behavioral therapy (CBT), relaxation, and support groups can help. Healthcare providers should also focus on these mental health aspects.
Impact on Relationships and Intimacy
An implantable defibrillator can also change how you connect with others. Family and partners might worry or feel scared about the device. Talking openly and learning about it can help everyone feel more comfortable.
Intimacy might also be affected, as you might worry about certain activities causing a shock. But, most people can do normal things with the right advice from doctors. Being open and reassuring is key to keeping relationships strong.
Support Resources and Counseling Options
It’s important for defibrillator patients to have access to support and counseling. Support groups, both in-person and online, offer a place to share and learn. Professional counseling, like CBT, can help with anxiety and other mental health issues.
|
Support Resource |
Description |
Benefits |
|---|---|---|
|
Support Groups |
In-person or online communities for sharing experiences |
Reduces feelings of isolation, provides coping strategies |
|
Cognitive-Behavioral Therapy (CBT) |
Professional counseling to address anxiety and device dependence |
Manages shock anxiety, improves mental health |
|
Educational Programs |
Programs educating patients and families about defibrillator care |
Enhances understanding, reduces fear and anxiety |
Using these support resources and counseling can help patients with implantable defibrillators. It can improve their mental health and overall quality of life.
Potential Complications and Side Effects of Defibrillators
Defibrillators save lives, but they can also have side effects. It’s important for patients to know about these risks. This knowledge helps manage expectations and ensures proper care.
Inappropriate Shocks: Causes and Prevention
Inappropriate shocks are a big worry for defibrillator users. They can happen due to electromagnetic interference, lead problems, or wrong device settings. To avoid these, patients should stay away from strong magnetic fields and tell their doctors about any changes.
- Avoid strong magnetic fields, like those from MRI machines or certain industrial equipment.
- Keep electronic devices, like cell phones and tablets, away from the defibrillator.
- Check your device regularly and report any odd shocks or behavior to your doctor.
Lead Displacement and Device Migration
Lead displacement happens when the wires connecting the defibrillator to the heart move. This can cause inappropriate shocks or prevent needed therapy. Device migration is when the defibrillator generator moves from its original spot.
To reduce these risks, patients should:
- Avoid heavy lifting or bending to prevent the device or leads from moving.
- Follow the activity guidelines given by their healthcare team after implantation.
- Go to regular check-ups to make sure the device and leads are in the right place.
Infection Risks and Management Strategies
Infection is a serious problem with any implanted device, including defibrillators. Signs include redness, swelling, warmth, or drainage at the implant site, along with fever or chills.
To manage infection risks:
- Keep the implant site clean and dry.
- Watch for signs of infection and tell your doctor right away if you see them.
- Follow antibiotic guidelines before dental or other surgeries.
By knowing about these risks and taking steps to prevent them, patients with defibrillators can live better lives.
Medications and Substances That May Affect Defibrillator Function
Living with a defibrillator means knowing a lot about it and how some medicines and substances can change how it works. It’s important to understand how these things can affect your heart health and your defibrillator.
Antiarrhythmic Drugs and Possible Interactions
Antiarrhythmic drugs help control irregular heartbeats in people with defibrillators. But, these drugs can also affect how the defibrillator works. For example, some drugs might change how the device detects heart problems or how it shocks the heart back to normal.
It’s key to talk to your doctor about these interactions. They can help adjust your treatment plan. Regular check-ups and device checks can spot any problems early.
Over-the-Counter Medications to Use With Caution
Most over-the-counter (OTC) medicines are safe when used right. But, some can affect your defibrillator or mix badly with other medicines. For instance, some cold medicines can make your heart beat too fast and cause your defibrillator to shock you when it shouldn’t.
- Always read the labels carefully and consult with your healthcare provider before taking any new medication.
- Inform your provider about all the medications you’re currently taking, including vitamins and supplements.
- Be cautious with medications that can affect heart rate or rhythm, such as certain cold remedies.
Alcohol and Caffeine Consumption Guidelines
Drinking alcohol and too much caffeine can mess with your heart rhythm and your defibrillator. While a little is usually okay, too much can cause heart problems or issues with your device.
- Limit alcohol to moderate levels (up to one drink a day for women and up to two for men).
- Watch how much caffeine you drink, as too much can cause heart issues.
- Pay attention to how your body reacts to these substances and adjust your use as needed.
Knowing how medicines and substances can impact your defibrillator helps you keep it working right. This way, you can take care of your heart health better.
Workplace Environments and Occupational Hazards
The workplace can be challenging for those with implantable defibrillators. It’s important to know about hazards that could affect these devices. We’ll look at risks and how to avoid them.
Jobs With High Electromagnetic Exposure
Some jobs have high electromagnetic fields. These can harm defibrillators. Jobs near power lines or electrical substations are risky. Workers should be careful and take precautions.
Heavy Machinery and Equipment Concerns
Heavy machinery can cause electromagnetic interference. Workers should protect themselves. This includes following safety rules and wearing protective gear.
Communicating With Employers About Restrictions
Talking to employers is key for safety. Defibrillator patients should tell their employers about their needs. This includes discussing job duties and emergency plans.
|
Occupational Hazard |
Potential Risk |
Precautionary Measure |
|---|---|---|
|
High-voltage power lines |
Electromagnetic interference |
Maintain safe distance, use shielding |
|
Industrial welding equipment |
Electromagnetic fields |
Limit exposure time, use protective gear |
|
Heavy machinery operation |
Physical injury, EMI |
Follow safety protocols, wear protective equipment |
Understanding hazards and taking steps can keep defibrillator patients safe at work.
Emergency Response Plan for Defibrillator Patients
Creating an emergency response plan is key for those with implantable defibrillators. It makes sure they get the right care in a medical crisis.
What to Do When Your Device Delivers a Shock
If your defibrillator shocks you, stay calm and follow these steps:
- If you’re awake, call your emergency contact or local emergency number right away.
- Tell someone nearby about the shock and ask them to call for help.
- If you’re alone, try to find a phone to call for help.
Having a plan for emergencies is vital. Know your device well and have emergency numbers ready.
Educating Family Members and Caregivers
Family and caregivers are important for defibrillator patients. Teach them about:
- The basics of your condition and how your defibrillator works.
- Signs of trouble, like dizziness or chest pain.
- Your emergency plan, including who to call and what to do.
Good communication helps your loved ones support you better.
Emergency Contact Information and Medical Alert Systems
Right emergency contacts and medical alert systems can save time in emergencies. Think about:
|
System |
Description |
Benefits |
|---|---|---|
|
Medical Alert Systems |
Wearable devices that let you call for help with a button press. |
Fast help access, peace of mind for patients and caregivers. |
|
Emergency Contact Apps |
Apps that store important medical info and emergency contacts. |
Quick access to vital info, easier communication with emergency services. |
Adding these systems to your plan helps ensure a quick and effective response to emergencies.
Conclusion: Balancing Safety With Quality of Life
Living with a defibrillator means finding a balance between safety and enjoying life. We’ve looked at how to manage a defibrillator, from knowing how it works to dealing with daily tasks and work settings.
Knowing about dangers like strong magnetic fields and taking steps during medical visits helps. Keeping the device in good shape, like checking the battery, is also key.
It’s vital to have mental support and ways to cope with having a defibrillator. Talking openly with doctors and loved ones is also important. By following these tips, people can live well and stay safe.
Managing a defibrillator well lets people live active, happy lives. By understanding the device and its effects, we can create a safer, better world for everyone.
FAQ
What is a defibrillator and how does it work?
A defibrillator is a device that helps fix abnormal heart rhythms. It sends an electric shock to get the heart beating right again. This is important to stop sudden cardiac arrest.
What are the different types of defibrillators?
There are many types of defibrillators. You have Automated External Defibrillators (AEDs), Implantable Cardioverter-Defibrillators (ICDs), and Wearable Cardioverter-Defibrillators (WCDs). Each one is used in different ways.
How do I avoid strong electromagnetic fields with a defibrillator?
To stay away from strong electromagnetic fields, avoid high-voltage power lines and electrical substations. Also, be careful around industrial equipment and welding machinery. MRI machines can also interfere with your defibrillator.
Can I use everyday electronics and appliances with a defibrillator?
Mostly, you can use everyday electronics and appliances. But, keep a safe distance from things that might mess with your defibrillator. This includes cell phones, tablets, and wireless charging systems.
Are there any physical activities or sports I should avoid with a defibrillator?
Yes, you should avoid contact sports and high-impact activities. These can damage your defibrillator or pull out its leads. Choose safe exercises and talk to your doctor about getting back into physical activities.
What precautions should I take when traveling with a defibrillator?
When traveling, be ready for airport security checks. Tell security about your defibrillator. Carry your device ID card and medical papers. Also, check with your doctor about any travel concerns.
How do I manage my defibrillator during medical and dental procedures?
Tell your healthcare provider about your defibrillator before any medical or dental procedure. Some procedures, like radiation therapy and electrocautery, need special care to avoid problems with your device.
What are the warning signs of defibrillator malfunction or complications?
Watch for signs like unexpected shocks or if your device doesn’t work right. Also, look out for infection signs around the implant site. If you see any of these, get emergency help right away.
How often should I have my defibrillator checked?
Regular check-ups are key for your defibrillator. Your doctor will tell you how often to come in. You might also use remote monitoring systems to check your device’s status.
Can I take medications and substances with a defibrillator?
Some medications and substances, like alcohol and caffeine, can affect your defibrillator. Always check with your doctor before taking anything new.
How do I create an emergency response plan with a defibrillator?
Make a plan for what to do if your device shocks you. Teach family and caregivers about it. Also, have emergency contact info ready.
What should I know about workplace environments and occupational hazards with a defibrillator?
If your job exposes you to strong electromagnetic fields or heavy machinery, talk to your employer. They can help make sure your workplace is safe.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/18364820/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























