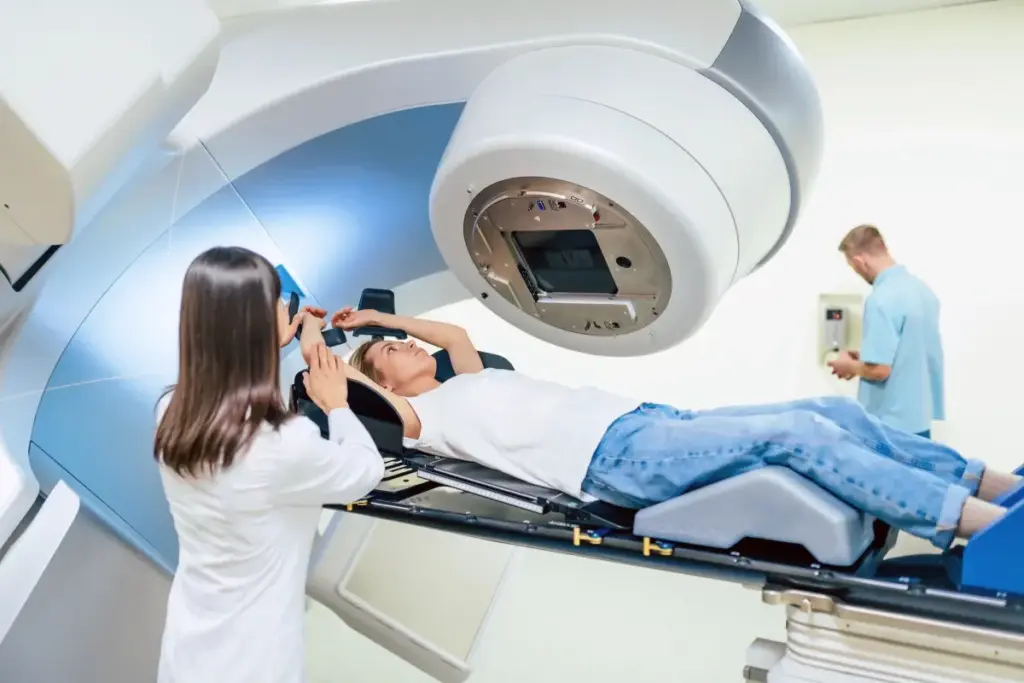
Radioembolization with Yttrium-90 (Y90) microspheres is a minimally invasive treatment for inoperable liver cancers. It sends targeted radiation straight to tumors. We look into how well this treatment works, showing great promise for liver cancer management. Explore the amazing y90 success rates for liver tumors. Learn how this vital procedure provides powerful results for cancer patients.
Recent studies show radioembolization’s success. It has a disease control rate of 78.1% and an objective response rateof 65.6% in patients with hepatocellular carcinoma. Also, the 1-year overall survival rate is about 80%.
Radioembolization sends targeted radiation to tumors, making it a valuable option for patients with inoperable liver cancers. We’ll explore this treatment’s details, its benefits, and what affects its success.
Key Takeaways
- Radioembolization is a minimally invasive treatment for inoperable liver cancers.
- The disease control rate for radioembolization is 78.1% in hepatocellular carcinoma patients.
- The 1-year overall survival rate is approximately 80%.
- Radioembolization delivers targeted radiation directly to liver tumors.
- The treatment involves the use of Yttrium-90 (Y90) microspheres.
The Fundamentals of Radioembolization Treatment
Radioembolization is changing how we treat liver cancer. It’s precise and effective. This method is key for patients with liver tumors. It targets the tumor without harming healthy tissue nearby.
We use Yttrium-90 (Y90) microspheres to send radiation to the tumor. This way, the radiation hits the tumor hard, making it more effective. It also cuts down on side effects.
What is Yttrium-90 (Y90) Radioembolization?
Y90 radioembolization means we put microspheres into the hepatic artery. This artery feeds the liver. The microspheres have Yttrium-90, a radioactive isotope that kills tumor cells. This method is minimally invasive, needing just a small cut in the groin.
How Radioembolization Targets Liver Tumors
We use a special catheter to get the Y90 microspheres to the liver tumors. This way, the radiation goes straight to the tumor. The healthy liver tissue stays safe. The microspheres block the blood vessels around the tumor, killing the cells with radiation.
|
Key Features |
Benefits |
|---|---|
|
Targeted Radiation |
Directly delivers radiation to the tumor, minimizing damage to healthy tissue |
|
Minimally Invasive |
Reduces recovery time and risk of complications |
|
Effective Tumor Control |
Provides significant control over tumor growth and progression |
Learning about radioembolization shows its promise in treating liver cancer. It’s a big step forward in cancer treatment. It gives patients new hope against liver tumors.
Understanding Y90 Radioembolization Procedure
The Y90 radioembolization procedure is a cutting-edge treatment for liver cancer. It’s a precise, step-by-step process. We’ll explain this innovative therapy, focusing on its minimally invasive nature and benefits for patients.
The Step-by-Step Process of Y90 Treatment
The Y90 radioembolization treatment has several key steps. First, we use imaging to find the hepatic artery, which feeds the liver tumors. Then, we inject Y90 microspheres into the artery, aiming for the tumor.
An interventional radiologist performs this in an angiography suite. The process starts with a detailed look at the patient’s blood vessels. This helps us find the best way to deliver the Y90 microspheres.
|
Step |
Description |
|---|---|
|
1. Pre-procedure assessment |
Evaluation of patient’s vascular anatomy |
|
2. Catheter placement |
Navigation to the hepatic artery under imaging guidance |
|
3. Y90 microsphere infusion |
Delivery of Y90 microspheres into the hepatic artery |
Minimally Invasive Approach and Patient Experience
The Y90 radioembolization procedure is minimally invasive. It only needs a small incision. This makes it less painful and reduces recovery time compared to surgery.
Patients are given conscious sedation during the procedure. It usually takes 1-2 hours, depending on the case.
After, patients are watched for a few hours before going home. Most can get back to normal in a few days. But, they should avoid hard activities for longer.
Getting a medical procedure can be scary. But, the Y90 radioembolization procedure aims to be as comfortable as possible. Our team is here to offer full care and support during treatment.
Key Success Metrics in Radioembolization Outcomes
To measure the success of radioembolization, we look at several key metrics. These metrics help us understand how well the treatment works. They also show its impact on patient outcomes.
Disease Control Rate vs. Objective Response Rate
The disease control rate and objective response rate are key indicators. The disease control rate shows how many patients’ disease is controlled. This can be through tumor shrinkage or stabilization.
Studies have found a disease control rate of 78.1% in Y90 radioembolization patients. On the other hand, the objective response rate shows how many patients see a significant tumor size reduction. An objective response rate of 65.6% has been seen in Y90 treatment patients.
Progression-Free and Overall Survival Measurements
Progression-free survival and overall survival are also important. Progression-free survival shows how long the disease doesn’t get worse. It tells us about the treatment’s ability to stop tumor growth.
Overall survival, on the other hand, shows how long patients live after treatment. By looking at these metrics, doctors can better understand the treatment’s success. This helps them make better decisions for patient care.
Success Rates for Hepatocellular Carcinoma (HCC)
Hepatocellular carcinoma (HCC) treatment has seen big improvements with Y90 radioembolization. This liver cancer type is tough, but Y90 radioembolization is proving to be a strong treatment.
Recent studies show Y90 radioembolization works well for HCC. Patients with HCC see a disease control rate of 78.1%and an objective response rate of 65.6%. These numbers show Y90 radioembolization can stop tumor growth and help patients.
78.1% Disease Control and 65.6% Objective Response Rates
The disease control rate and objective response rate are key to measuring Y90 radioembolization’s success. A disease control rate of 78.1% means many patients see their tumors stabilize or shrink. An objective response rate of 65.6% shows many patients have a strong positive reaction to the treatment. This can greatly improve their quality of life and survival chances.
The main benefits of Y90 radioembolization for HCC are:
- Effective tumor control
- Minimally invasive procedure
- Less risk of complications than traditional surgery
- Potential for better survival rates
80% One-Year Overall Survival Outcomes
Y90 radioembolization also shows promising results for HCC patients’ overall survival. Studies indicate a 1-year overall survival rate of about 80%. This is a big improvement, giving hope to both patients and doctors.
To show how effective Y90 radioembolization is, look at this data:
|
Treatment Outcome |
Percentage |
|---|---|
|
Disease Control Rate |
78.1% |
|
Objective Response Rate |
65.6% |
|
1-Year Overall Survival |
80% |
In conclusion, Y90 radioembolization is a big step forward in treating HCC. It offers better disease control, response, and survival rates. As we keep improving this treatment, we expect even better results for HCC patients.
Y90 Treatment Success for Metastatic Colorectal Cancer
Y90 radioembolization is becoming a key treatment for metastatic colorectal cancer. This condition is hard to treat, but Y90 radioembolization is showing great promise.
15-Month Median Overall Survival Data
Research shows a median overall survival of 15 months for patients with metastatic colorectal cancer treated with Y90 radioembolization. This is a big win for those undergoing this treatment.
The median overall survival rate is a key measure of a cancer treatment’s success. For metastatic colorectal cancer, reaching a median overall survival of 15 months with Y90 radioembolization is a big deal.
60% Progression-Free Survival at 12 Months
Y90 radioembolization also improves progression-free survival. About 60% of patients with metastatic colorectal cancer stay progression-free at 12 months after treatment.
Progression-free survival is a key sign of a treatment’s success. A 60% progression-free survival rate at 12 months shows Y90 radioembolization’s effectiveness in treating metastatic colorectal cancer.
|
Treatment Outcome |
Y90 Radioembolization |
|---|---|
|
Median Overall Survival |
15 months |
|
Progression-Free Survival at 12 Months |
60% |
These results show Y90 radioembolization’s value as a treatment for metastatic colorectal cancer. Remember, results can vary, and who gets treated matters a lot.
Radioembolization Outcomes for Neuroendocrine Tumor Metastases
Y90 radioembolization is a big step forward in cancer treatment. It brings great benefits to those with neuroendocrine tumor metastases.
27.2-Month Median Survival Advantage
Research shows that Y90 radioembolization can extend life by 27.2 months. This is a big win for patients, giving them more time with family and a better life quality.
The 27.2-month survival boost is key to measuring Y90 therapy’s success. It lets patients live longer, try more treatments, and feel better overall.
Quality of Life Improvements After Y90 Therapy
Y90 radioembolization also boosts life quality for patients with neuroendocrine tumor metastases. It lessens tumor sizeand eases symptoms, helping patients stay independent.
Patients who get Y90 therapy often see a big drop in symptoms. This shows Y90 therapy’s power in handling this tough condition.
With Y90 radioembolization, patients with neuroendocrine tumor metastases get a longer life and better life quality. We’re dedicated to giving our patients the best care, and Y90 therapy is a key part of it.
Downstaging Success: From Y90 to Curative Options
Y90 radioembolization is a promising way to treat liver tumors. It helps patients become candidates for surgery or liver transplant. This is key in treating liver cancer, as it can make tumors that were once too big to remove now operable.
34% Achievement Rate for Surgery or Transplant Eligibility
Y90 radioembolization has a big advantage: it can downstage tumors. This makes patients eligible for treatments that could cure them. Studies show that 34% of patients become eligible for surgery or liver transplant after Y90 therapy.
100% Two-Year Survival in Downstaged Patients
Downstaging tumors not only makes patients eligible for curative treatments. It also greatly improves their chances of survival. Research shows that downstaged patients have a 100% two-year survival rate. This highlights Y90 radioembolization’s role in improving long-term survival.
The success of Y90 radioembolization in downstaging tumors is significant. It shows how important Y90 therapy is for patients with liver cancer. It’s a key option for those who were not initially candidates for curative treatments.
The main benefits of downstaging success are:
- More patients become eligible for surgery or liver transplant
- Downstaged patients have better survival rates
- Patients undergoing Y90 radioembolization enjoy a better quality of life
In summary, Y90 radioembolization is a valuable treatment. It can downstage liver tumors, making patients eligible for curative treatments. With its high success rate and impressive survival outcomes, Y90 therapy is a key part of treating liver cancer.
Is Y90 a Last Resort? Understanding Treatment Timing
Y90 radioembolization isn’t always a last resort. Its timing depends on many factors. The best time for Y90 treatment varies based on the patient’s health and past treatments. We’ll look at how Y90 fits into liver cancer treatment and when it works best.
Y90 in the Treatment Sequence for Liver Cancer
Y90 radioembolization can be used at different stages of liver cancer treatment. Its place in the treatment plan depends on the patient’s health, tumor type, and past treatments.
Liver cancer treatment often combines surgery, chemotherapy, and targeted therapies. Y90 radioembolization is effective for patients with liver cancer that can’t be removed or those who have tried other treatments. Doctors consider each patient’s needs and history to decide when to use Y90 therapy.
When Radioembolization Offers Maximum Benefit
Y90 radioembolization works best for patients with liver-dominant disease. This means the cancer mainly affects the liver. In these cases, Y90 can slow tumor growth, improve survival, and enhance quality of life. It’s also good for patients who can’t have surgery or other local treatments.
By choosing the right patients and timing Y90 therapy, doctors can get the most out of it. This tailored approach ensures patients get the best care for their condition.
Factors Influencing Y90 Radioembolization Success
Y90 radioembolization success depends on many patient and tumor traits. Knowing these traits is key to better treatment results and care.
Tumor Size and Stage
The size and stage of the tumor greatly affect Y90 radioembolization success. Larger tumors or those at an advanced stage are harder to treat. Research shows better results for patients with smaller, earlier-stage tumors.
Starting treatment early can improve control over the disease and survival rates. So, checking tumor size and stage is essential in choosing patients for Y90 radioembolization.
Liver Function and Patient Selection Criteria
Liver function is also key to Y90 radioembolization success. Patients with poor liver function might not be good candidates. This is because they could face higher risks and lower treatment success.
Picking the right patients is critical. This means looking at liver function, overall health, and past treatments. Multidisciplinary teams evaluate these to find the best treatment for each patient.
Prior Treatments and Their Effect on Outcomes
Prior treatments can change how well Y90 radioembolization works. Patients who have had other treatments might not respond the same way as those getting Y90 first.
It’s important for doctors to understand how past treatments affect Y90 outcomes. Customizing treatment plans based on each patient’s history can make Y90 more effective.
By focusing on these factors, doctors can make Y90 radioembolization better. This leads to better results and a better life for patients.
Comparing Radioembolization to Alternative Liver Cancer Treatments
Understanding how different treatments work for liver cancer is key. As we learn more, we can make better choices for patients. This helps both patients and doctors decide the best course of action.
Y90 vs. Transarterial Chemoembolization (TACE)
Transarterial chemoembolization (TACE) is a treatment that delivers chemotherapy directly to tumors. It then blocks the blood supply to the tumor. Y90 radioembolization also targets tumors but in a different way.
Y90 radioembolization might need fewer sessions than TACE. A study in the Journal of Clinical Oncology found Y90 works better for some liver cancer patients. It showed a higher success rate than TACE in certain cases.
“The use of Y90 radioembolization has been shown to provide a significant survival benefit in patients with advanced liver cancer, comparable to or even surpassing that of TACE in certain cases.”
Radioembolization vs. Systemic Therapies
Systemic therapies use drugs to fight cancer all over the body. Choosing between radioembolization and these therapies depends on the cancer’s stage and the patient’s health.
Radioembolization is great for tumors in the liver because it targets them precisely. Systemic therapies are better for cancer that has spread beyond the liver.
A study showed Y90 radioembolization helps patients live longer without their cancer getting worse. This is more than systemic therapies alone.
Choosing between treatments depends on many factors. These include the patient’s condition, cancer stage, and treatment goals. Knowing how each treatment works helps doctors create the best plan for each patient.
Managing Side Effects and Complications After Y90 Procedure
Managing side effects is key after Y90 radioembolization treatment. Knowing and reducing possible complications is vital for better patient results.
Common Side Effects and Their Duration
Patients may face fatigue, nausea, and abdominal pain after Y90 radioembolization. These issues usually go away in a few days to weeks. Using medicines for nausea and pain can make patients feel better.
Some might also get mild fever or chills. These are usually short-term. It’s important to watch these symptoms and tell doctors if they worry you.
Serious Complications and Risk Mitigation
Though rare, serious issues like radiation-induced liver disease (REILD) or gastrointestinal ulcers can happen. REILD is a serious condition that needs close watching and quick treatment. To lower this risk, picking the right patients and planning the dose carefully are key.
Steps to reduce risks include a detailed check before the procedure, precise Y90 dosing, and watching patients closely after. Knowing what can cause these problems helps doctors lower risks and improve care.
Handling side effects and complications after Y90 radioembolization is complex. It involves teaching patients, watching them closely, and acting fast when needed. By focusing on these areas, we can make Y90 treatment more successful for patients.
International Standards in Radioembolization Treatment
International standards are key to making radioembolization treatment work well. As this treatment gets better, sticking to these standards is very important. It helps patients get the best results.
Advanced Y90 Protocols at Leading Institutions
Top hospitals around the world are using the latest Y90 protocols. These new methods make radioembolization treatments more precise and effective. For example, Yttrium-90 (Y90) microspheres are now a main part of treating liver cancer.
These advanced methods need careful planning and doing. They include detailed dosing and imaging checks. The aim is to get the best treatment effect while protecting healthy tissues.
|
Institution |
Protocol |
Key Features |
|---|---|---|
|
Leading Cancer Center |
Combination Therapy |
Integration of Y90 with other treatment modalities |
|
Advanced Research Institute |
Image-Guided Y90 Delivery |
Real-time imaging for precise microsphere delivery |
Conclusion: The Evolving Success Story of Y90 Radioembolization
Y90 radioembolization has become a top choice for treating liver cancer. It offers great benefits in controlling the disease, improving survival rates, and boosting quality of life. Studies have shown it works well for different types of liver cancer, like hepatocellular carcinoma and metastatic colorectal cancer.
As research keeps moving forward, Y90 radioembolization’s success story will likely grow. We’re seeing big steps forward, with places like ours using the latest methods to help patients from all over. This means better care for everyone.
The outlook for treating liver cancer is bright, with Y90 radioembolization leading the way. It gives hope to both patients and doctors. By making treatment even better and choosing the right patients, we can make Y90 radioembolization even more effective. This will lead to even better results for patients.
FAQ
What is Y90 radioembolization?
Y90 radioembolization is a treatment that uses tiny Yttrium-90 microspheres. These microspheres carry targeted radiation to liver tumors. This method helps protect the healthy tissue around the tumors.
How effective is Y90 radioembolization in treating liver cancer?
Research shows Y90 radioembolization is very effective. It controls liver cancer in 78.1% of patients and shows improvement in 65.6%. Patients also live about 80% longer for a year after treatment.
What are the common side effects of Y90 radioembolization?
Side effects include feeling tired, nausea, and stomach pain. These usually go away on their own. But, serious problems like liver damage or ulcers can happen.
Is Y90 radioembolization a last resort for liver cancer treatment?
Y90 radioembolization is not always a last choice. It can be used at various stages of treatment. It helps make tumors smaller, so patients might be eligible for more treatments.
How does Y90 radioembolization compare to other liver cancer treatments?
Y90 radioembolization targets the tumor directly. It’s better than some treatments like TACE for some patients. Unlike systemic treatments, Y90 focuses on the tumor site, not the whole body.
What factors influence the success of Y90 radioembolization?
Success depends on tumor size, stage, liver health, and past treatments. Patients with big tumors or poor liver function might face challenges.
Can Y90 radioembolization improve quality of life for patients with neuroendocrine tumor metastases?
Yes, it can. Y90 radioembolization can reduce symptoms and improve life quality. Patients often live 27.2 months longer after treatment.
What is the role of downstaging in Y90 radioembolization?
Downstaging makes patients eligible for treatments like surgery or liver transplant. Studies show 34% of patients can get these treatments. Downstaged patients have a 100% 2-year survival rate.
How is Y90 radioembolization performed?
The procedure involves injecting Y90 microspheres into the hepatic artery. This is done under imaging to ensure the microspheres reach the tumor. It’s less invasive than surgery, leading to less discomfort and quicker recovery.
What are the key metrics used to evaluate the success of Y90 radioembolization?
Success is measured by disease control rate, objective response rate, and survival rates. These metrics help understand how well the treatment works and patient outcomes.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from























