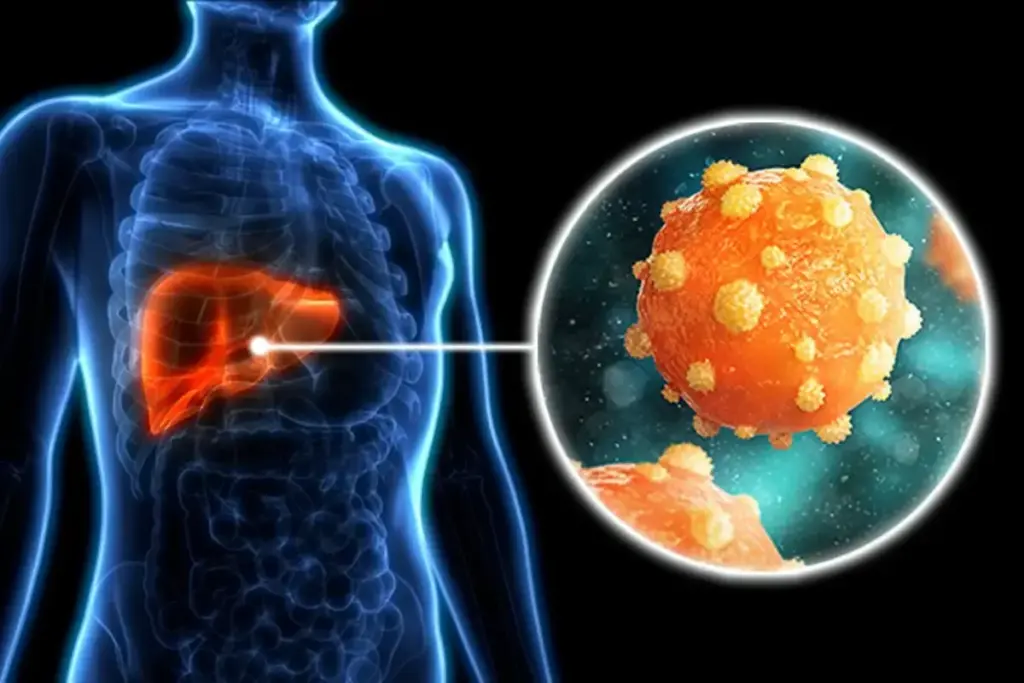
Hepatitis B is a big health problem worldwide, affecting millions. It’s important to know how the disease progresses. There are five distinct stages of hepatitis B infection that doctors need to manage well.
The disease goes through five stages, based on changes in the virus, liver function, and body’s response. The World Health Organization says it’s key to understand these stages for the right care. Each stage has different levels of virus and liver enzyme levels.
Key Takeaways
- Understanding the five stages of hepatitis B infection is key for managing the disease well.
- The stages show changes in the virus, liver function, and body’s response.
- Knowing each stage helps improve patient care and outcomes.
- If not treated, hepatitis B can become a chronic disease.
- Early detection and treatment are vital to avoid complications.
Understanding Hepatitis B Virus
It’s important to know about the Hepatitis B virus to understand its impact on health worldwide. Hepatitis B is a viral infection caused by the Hepatitis B virus (HBV). It belongs to the Hepadnaviridae family.
What is Hepatitis B?
Hepatitis B is a major health issue affecting millions globally. It’s caused by HBV, an enveloped virus leading to liver disease. The virus spreads through contact with infected blood, semen, and other fluids.
Transmission and Risk Factors
Understanding how Hepatitis B spreads is key. HBV can be transmitted through:
- Exposure to infectious blood
- Sexual contact with an infected person
- Mother-to-child transmission during birth
- Sharing needles or other equipment for injecting drugs
Risk factors for Hepatitis B include:
- Having unprotected sex with multiple partners
- Being born to a mother with Hepatitis B
- Injecting drugs and sharing equipment
- Having a history of liver disease
Acute vs. Chronic Infection
Hepatitis B can be either acute or chronic. Acute Hepatitis B is a short-term illness within the first six months after exposure. Most adults recover fully.
Chronic Hepatitis B is a long-term infection leading to serious liver disease. The risk of chronic infection is highest in young children. About 90% of infected infants and 30% of children aged 1–5 will stay infected with HBV.
Knowing the difference between acute and chronic Hepatitis B is key to managing the disease and preventing complications.
The 5 Stages of Hep B Infection
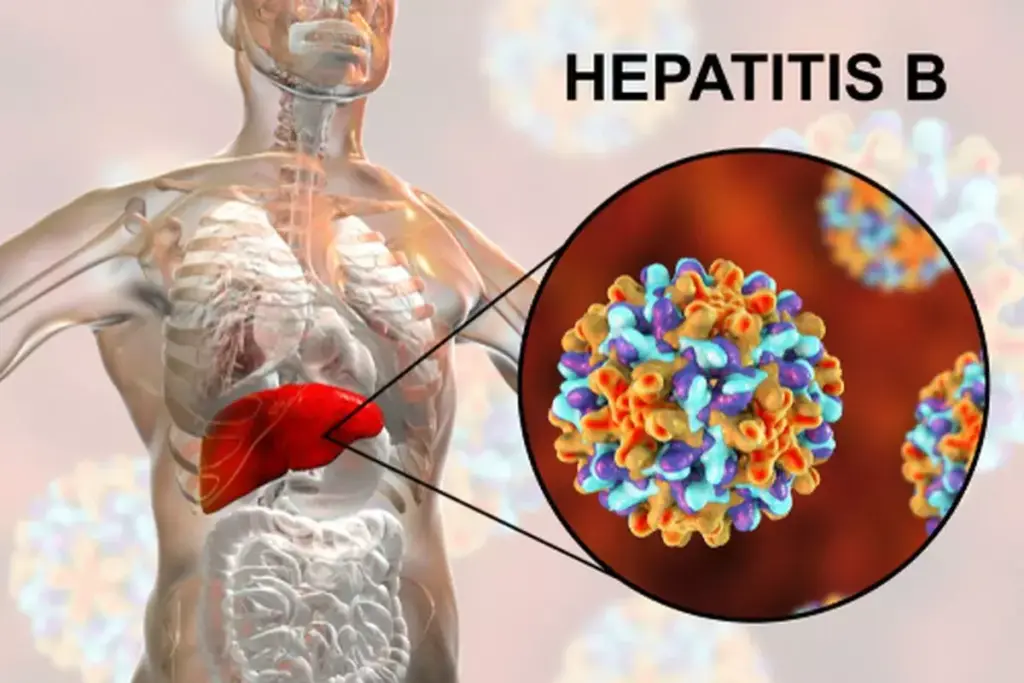
Knowing the five stages of Hepatitis B infection is key to managing the disease well. Hepatitis B virus (HBV) infection goes through different stages, each with its own traits.
Stage 1: Immune Tolerant Phase
In the immune tolerant phase, HBV DNA levels are high, and HBeAg is positive. Yet, liver enzymes are normal. Patients often don’t show symptoms, so regular checks are important.
Stage 2: Immune Response/Clearance Phase
This phase, also called the immune active phase, shows the body’s fight against the virus. Liver enzymes go up, and liver inflammation is active. It’s a critical time that can harm the liver if not handled right. The Centers for Disease Control and Prevention says it’s key to act fast.
Stage 3: Inactive Carrier State
In the inactive carrier state, viral replication drops a lot. Patients have low or no HBV DNA and are HBeAg negative. The risk of liver disease getting worse is lower, but watching closely is needed to catch any signs of getting worse.
Stage 4: Chronic HBeAg-Negative Disease
Chronic HBeAg-negative disease can start from the immune clearance phase or the inactive carrier state. It’s marked by HBV genome mutations that stop HBeAg production. Patients may see ups and downs in viral loads and liver inflammation, needing constant care to stop the disease from getting worse.
By knowing these stages, doctors can make treatment plans that fit each patient’s needs. This helps improve health outcomes and lowers the chance of serious problems.
Conclusion
Knowing the 5 stages of Hepatitis B infection is key for good disease care. It helps in giving top-notch healthcare to patients from around the world. Each stage has its own signs and what it means for health.
Chronic Hepatitis B can cause big health problems like liver damage and cancer. It’s important to spot the symptoms of chronic hepatitis b infection early. Knowing the difference between chronic and acute hepatitis b helps in acting fast.
The hepatitis b classification into stages lets doctors create the right treatment for each patient. Those with chronic hbv infection symptoms need constant check-ups and care to avoid serious issues later.
We stress the need to know about Hepatitis B infection stages. When patients and doctors understand these stages, they can better manage the disease. This leads to better health outcomes for everyone.
FAQ
What are the five stages of Hepatitis B infection?
Hepatitis B infection goes through five stages. These are the immune tolerant phase, immune clearance phase, inactive carrier state, chronic HBeAg-negative disease, and reactivation phase. Knowing these stages helps manage the disease well.
What characterizes the immune tolerant phase of Hepatitis B?
In the immune tolerant phase, HBV DNA and HBeAg levels are high. This shows the virus is actively replicating. Liver inflammation is minimal, and liver enzymes are usually normal.
How does the immune clearance phase differ from the immune tolerant phase?
The immune clearance phase is when the body fights the virus. This leads to higher liver enzymes and more inflammation. It’s a sign the body is trying to get rid of the virus.
What is the inactive carrier state in Hepatitis B infection?
The inactive carrier state means the virus is not actively replicating. HBV DNA levels are low or undetectable, and HBeAg is negative. Liver enzymes are normal, showing little inflammation.
What is chronic HBeAg-negative disease?
Chronic HBeAg-negative disease can start from the immune clearance phase or the inactive carrier state. It’s marked by HBV DNA in the blood, but HBeAg is negative. This stage needs careful management because it can cause ongoing liver inflammation.
How does the risk of chronic Hepatitis B infection vary with age?
Young children are at the highest risk of chronic infection. About 90% of infected babies and 30% of kids aged 1–5 will stay infected. Early treatment and prevention are key.
What is the difference between acute and chronic Hepatitis B infection?
Acute Hepatitis B is a short illness that happens when you first get infected. Chronic Hepatitis B is a long-term condition that can damage the liver. Knowing the difference is important for choosing the right treatment.
What are the implications of having low Hepatitis B virus levels?
Low HBV levels, often seen in the inactive carrier state, mean a lower risk of liver damage. But, regular checks are needed to catch any signs of reactivation or worsening.
What are the symptoms of chronic Hepatitis B infection?
Symptoms of chronic Hepatitis B can include fatigue, jaundice, and stomach pain. Many people with chronic HBV don’t show symptoms. Regular screening and monitoring are essential.
Hepatitis B. In StatPearls (Internet). StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK555945/



































