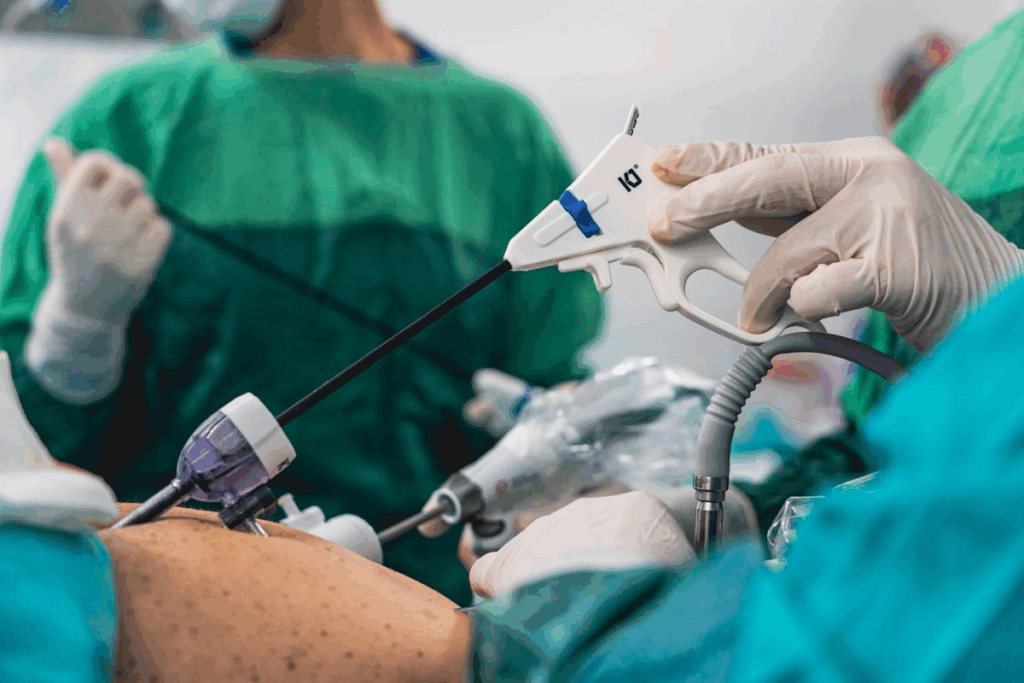
Getting gastric bypass revision surgery approved can be tough. Many bariatric surgery patients face weight regain or complications. They need revision procedures. Knowing what documents to prepare, what medical needs to show, and how to submit your case can help a lot.Explaining the different gastric bypass revision options and the steps to get insurance approval.
We’ll show you how to boost your approval chances. With the right documents and following post-op rules, you can get through the approval process. Recent data shows that revision procedures are covered in about 79% of insurance policies. This gives hope to those looking for corrective surgery.
Key Takeaways
- Understanding medical necessity criteria is key for approval.
- Having the right documents is essential for a good submission.
- Most insurance policies cover revision procedures.
- Following post-op rules can increase your approval chances.
- Smart submission strategies can help get insurance coverage.
Understanding Gastric Bypass Revision Surgery
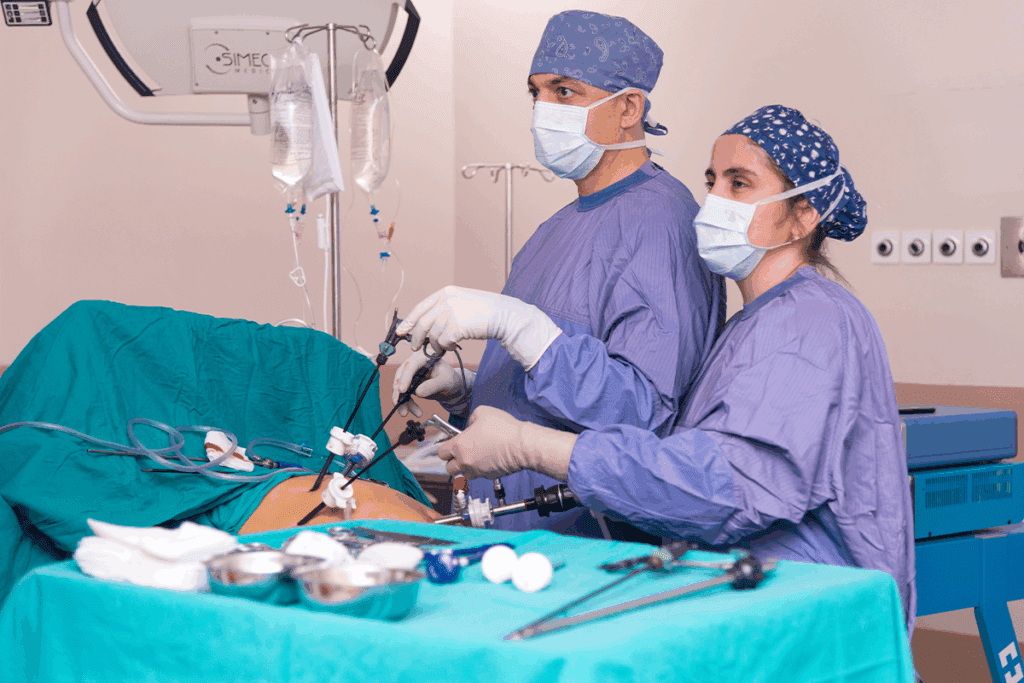
For many, gastric bypass revision surgery is needed when the first surgery doesn’t work as hoped. This second surgery aims to fix problems or help with weight loss that didn’t happen after the first surgery.
What Constitutes Revision Bariatric Surgery
Revision bariatric surgery is any surgery done after a first bariatric surgery. It can be to fix, repair, or change the first surgery. The main goal is to make the first surgery better, like fixing weight gain, fixing body problems, or solving metabolic issues.
A 2024 study in the International Journal of Surgery shows bariatric surgery’s benefits. It can even cure type 2 diabetes with early care and follow-up. This shows why revision surgery is key for lasting health benefits.
Common Reasons for Seeking Revision
People get revision surgery for many reasons. Some common ones are:
- Weight regain after losing weight
- Body problems like stricture or ulcers
- Metabolic issues not fixed or new ones
- Not losing enough weight, even with diet
Knowing these reasons helps figure out the best surgery plan. It’s important for patients to talk with their doctors to find the right solution.
Reason for Revision | Description | Potential Solution |
Weight Regain | Regaining weight after losing it | Revision surgery to adjust or modify the initial procedure |
Anatomical Complications | Issues such as stricture or ulcer formation | Corrective surgery to repair or adjust the anatomy |
Metabolic Issues | Unresolved or developed metabolic problems | Revision surgery to improve metabolic outcomes |
Patients looking for revision surgery often face insurance rules. They need to prove they really need the surgery. It’s important for them to work with their doctors to show why they need it.
Medical Necessity Criteria for Revision Surgery
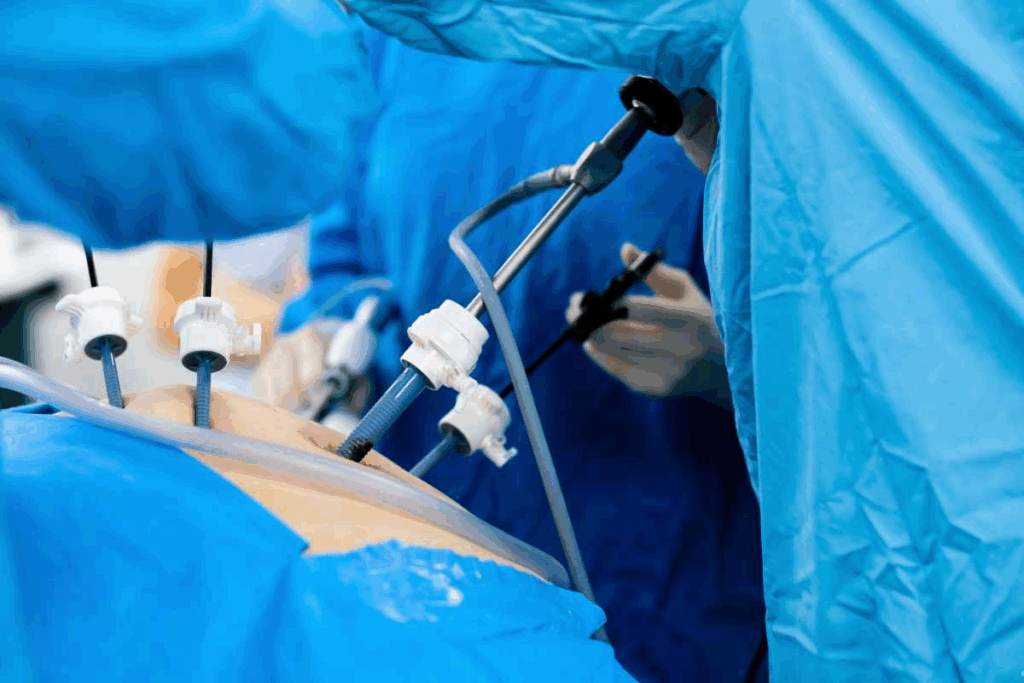
Medical necessity criteria are key in deciding if a patient needs gastric bypass revision surgery. These rules make sure revision surgery is only for those who really need it.
To be eligible, patients must meet certain requirements. These include weight regain, complications from the first surgery, and following the timeline after the first surgery.
Documented Weight Regain Thresholds
Insurance companies look at how much weight patients regain after the first surgery. They check if patients lose less than 50% of excess weight or regain most of it within 12 to 24 months. This helps them see if the first surgery worked and if a revision is needed.
For example, if a patient lost 60% of excess weight in the first year but gained 20% back by the second year, they might get approved for revision surgery.
Complications That Qualify for Medical Necessity
Some complications after gastric bypass surgery can also qualify patients for revision. These include:
- Ulcers or erosion
- Fistulas
- Malnutrition
- Other serious health issues directly related to the initial surgery
These complications need to be well-documented. Their impact on the patient’s health must be shown clearly to the insurance provider.
Timeline Requirements After Initial Surgery
Insurance companies also look at how long it’s been after the first surgery before approving a revision. This time is usually 12 to 24 months. It gives enough time to see if the first surgery was successful.
Criteria | Description | Timeline |
Weight Regain | Losing less than 50% of excess weight or regaining most of the weight | 12 to 24 months |
Complications | Presence of ulcers, fistulas, malnutrition, or other serious health issues | Variable, depending on complication onset |
Revision Approval | Meeting weight regain thresholds or having significant complications | After initial surgery timeline requirements are met |
Understanding these criteria is key for patients going through the approval process for gastric bypass revision surgery. By meeting these criteria, patients can make a stronger case for insurance approval.
Insurance Coverage Landscape for Revision Procedures
Insurance for gastric bypass revision varies a lot. Some pay a lot, while others are harder to get approval from.
Current Coverage Statistics and Trends
About 79% of insurance plans cover revision procedures. But, the rules are strict. Around 67% of plans pay for a second surgery if the first one didn’t work.
It’s key to know what your insurance says. Check your policy well to see what you can get covered for.
Variations Among Major Insurance Providers
Insurance companies have different rules for gastric bypass revision. Some might cover it under certain conditions. Others might ask for more proof or have special rules.
- Some insurance companies need proof you’ve gained weight back or had problems after the first surgery.
- Others might make you try to lose weight without surgery first before they’ll cover the revision.
Medicare Coverage for Revision Surgery
Medicare covers bariatric surgery, including revisions, under certain rules. You need to have a high BMI or health problems to qualify.
It’s important to talk to your doctor and insurance to know what Medicare needs for coverage.
Gastric Bypass Revision Options and Their Approval Rates
Gastric bypass revision surgery includes many procedures, like conversions and corrective surgeries. Each has its own insurance approval rate. It’s important for patients to know about these options and how insurance works for them.
Conversion Procedures (RNY to Sleeve, Band to Bypass)
Conversion procedures change one bariatric surgery to another. For example, some might switch from Roux-en-Y (RNY) gastric bypass to a gastric sleeve. Or, they might change from an adjustable gastric band to a gastric bypass. These changes are often made because of complications or not losing enough weight.
Conversion Procedure Typical Reasons Insurance Approval Rate RNY to Sleeve Insufficient weight loss, complications 60-70% Band to Bypass Complications, inadequate weight loss 70-80%
Conversion Procedure | Typical Reasons | Insurance Approval Rate |
RNY to Sleeve | Insufficient weight loss, complications | 60-70% |
Band to Bypass | Complications, inadequate weight loss | 70-80% |
Corrective Procedures for Complications
Corrective procedures fix problems from the first bariatric surgery. They can fix anatomical issues, address nutritional problems, or solve other surgery-related issues.
Procedures with Highest Insurance Approval Rates
Some revision procedures get approved by insurance more often. This is because they are medically necessary. For example, surgeries for severe complications usually get approved more than less severe reasons for conversion.
Endoscopic revision procedures are less invasive. They cost between $5,000 and $15,000. Insurance might see them as more favorable because they are less invasive.
Dealing with insurance can be tough. Our team helps patients through this. We make sure they get the care they need.
Preparing Your Case for Insurance Approval
Getting insurance to approve your gastric bypass revision surgery starts with careful preparation. We know it can be tough to deal with insurance rules. But with the right steps, you can make your case stronger and boost your approval chances.
Essential Medical Documentation
Insurance companies need solid documentation to decide if you need gastric bypass revision surgery. Here are the key documents to get:
- Operative reports from your first surgery
- Medical records about your care after surgery and any issues
- Follow-up notes from your doctors
- Proof of weight gain and health problems that followed
These documents show your medical history and why you need the surgery. A top bariatric surgeon says, “Good documentation is key to showing you really need the surgery.”
“The importance of detailed medical records cannot be overstated. They are the cornerstone of a successful insurance claim for gastric bypass revision surgery.”
Required Specialist Evaluations
Along with medical records, specialist opinions are also important. We suggest getting checks from:
- A bariatric surgeon to see if you need the surgery
- A nutritionist to look at your diet and health
- A psychologist or psychiatrist to check your mental health
These checks give a full view of your health and if you’re ready for surgery. As shown in the image below, a detailed evaluation is essential for a good insurance claim.
By getting the right medical documents and specialist opinions, you can make a strong case for insurance approval. We’re here to help you through this and support you all the way.
The Pre-Approval Process Step-by-Step
To get ready for gastric bypass revision surgery, knowing the pre-approval process is key. This process has several important steps. Patients must follow these steps to get their surgery approved.
Initial Consultation with Bariatric Surgeon
The first step is an initial consultation with a bariatric surgeon. The surgeon will look at your medical history and current health. They will also check why you want the surgery.
Be ready to talk about your past weight loss tries and any problems you faced. This is also a chance to learn about the surgery’s risks and benefits.
Insurance Verification and Benefits Check
Next, you need to do insurance verification and benefits check. Your insurance company will tell you what they cover. This is important to know what you’ll pay out of pocket.
You’ll get a detailed report on your insurance coverage. Make sure to work with your surgeon’s office to get all the needed info.
Submitting the Pre-Authorization Request
After checking your insurance, it’s time to submit the pre-authorization request. You’ll need to prepare a package for your insurance. This includes your medical records and why you need the surgery.
Make sure your request is complete and well-documented. This will help increase your chances of approval. Your healthcare team can help make sure you have everything needed.
Timeline Expectations for Approval Decision
After you send in your request, know the timeline for the approval decision. Insurance companies usually take weeks to review. The time can vary based on how complex your case is and how busy they are.
It’s important to keep in touch with your insurance to make sure they’re working on your request. Below is a general timeline for the pre-approval process.
Step | Timeline | Responsibility |
Initial Consultation | 1-2 weeks | Patient & Surgeon |
Insurance Verification | 1-3 weeks | Surgeon’s Office |
Pre-Authorization Request | 2-4 weeks | Patient & Surgeon’s Office |
Approval Decision | 4-6 weeks | Insurance Provider |
By following these steps, patients can better navigate the pre-approval process. This increases their chances of getting their surgery approved.
Demonstrating Conservative Measure Exhaustion
Before getting approval for gastric bypass revision surgery, you must show you’ve tried non-surgical weight loss methods. This can be tough, but it’s key for insurance to see if surgery is needed.
Required Non-Surgical Interventions
Insurance wants to see you’ve tried many non-surgical ways to lose weight before surgery. These might include:
- Medically supervised diets: You’ll need to follow a diet plan with a doctor’s help.
- Exercise programs: You must do regular exercise and show your progress.
- Behavioral therapy: Some insurance requires therapy to change eating habits and lifestyle.
Documenting Supervised Diet Attempts
Showing you’ve tried supervised diets is very important. Work with a dietitian to make a diet plan just for you. Your records should have:
- Dietary plans and modifications: Keep track of your diet plans and any changes.
- Progress tracking: Monitor your weight and body mass index (BMI) regularly.
- Outcome assessments: Show how well your diet plans worked for weight loss.
Exercise Program Participation Evidence
Doing an exercise program is also key. You should do a workout plan that fits your needs. Your evidence might include:
- Exercise logs: Keep a log of your workouts, like type, how long, and how hard.
- Fitness assessments: Check your heart health, strength, and flexibility often.
- Progress reports: Get reports from a fitness expert or doctor on your fitness gains.
By documenting these non-surgical steps, you can make a strong case for gastric bypass revision surgery. This can help get insurance approval.
Navigating Insurance Denials and Appeals
Insurance denials for gastric bypass revision surgery happen to about 25% of patients. It’s important to know why and how to appeal. This helps patients fight for their health needs.
Common Reasons for Revision Surgery Denial
Insurance companies deny coverage for several reasons. These include:
- Insufficient documentation of medical necessity
- Lack of evidence showing exhaustion of conservative weight loss measures
- Previous denials without significant changes in the patient’s condition or new evidence
Knowing these reasons helps patients build a stronger case. They can prepare better for their application and appeal.
Crafting an Effective Appeal Letter
An effective appeal letter is key to challenging a denial. It should:
- Clearly state the reason for the appeal
- Provide additional medical evidence supporting the necessity of the revision surgery
- Include personal statements from the patient and their healthcare provider
Key elements of a successful appeal letter include: a concise summary of the patient’s medical history, specific details about complications or weight regain, and how the revision surgery will improve health outcomes.
Utilizing Peer-to-Peer Reviews
A peer-to-peer review is a direct conversation between the surgeon and the insurance company. It’s a chance to discuss the patient’s case in detail. This can help address concerns and overturn denials.
The benefits of peer-to-peer reviews include: real-time clarification of medical information, addressing specific insurance concerns, and a personal approach to advocating for the patient.
External Review Options and Patient Rights
If an internal appeal is denied, patients can request an external review. This is done by an independent third party. It’s governed by state and federal regulations, adding an extra layer of oversight.
Patients should know their rights, including:
- The right to an external review within a specified timeframe (usually 45 days)
- The right to have their case reviewed by experts in bariatric surgery
- The possibility that the external review decision could be binding on the insurance company
Understanding these options and advocating for their rights can help patients. It can improve their chances of a successful appeal and access to necessary care.
Alternative Funding Options When Insurance Fails
When insurance says no to gastric bypass revision surgery, there are other ways to pay. Patients can look for financial help to cover the surgery costs.
Medical Financing Programs
Medical financing helps pay for surgeries like gastric bypass revision. These plans let you pay over time. CareCredit and Prosper Healthcare Lending offer these options.
To get financing, apply online or through your surgeon. You’ll need to share your financial info. After approval, you can use the funds for your surgery.
Hospital Charity Care Programs
Hospitals have charity care for those without insurance. These programs can lower or wipe out surgery costs. You must meet income limits and show you can’t pay.
Check with hospitals about their charity care. Financial counselors can help with the application and see if you qualify.
Clinical Trials and Research Studies
Clinical trials can also help pay for surgery. Some studies cover costs as part of their research. Look for trials on ClinicalTrials.gov.
Be sure to understand the trial’s rules and risks. This option can help financially, but know what you’re getting into.
Medical Tourism Considerations
Medical tourism is another option. Some countries offer surgery at lower costs than the U.S. But, check the surgeon’s qualifications and the facility’s standards.
Think about travel and accommodation costs, too. International Society for the Study of Obesity can help find safe surgery centers abroad.
Conclusion: Maximizing Your Chances for Revision Surgery Approval
To increase your chances for gastric bypass revision approval, it’s key to know the medical necessity criteria and insurance coverage. Follow the steps in this article to boost your approval odds.
It’s vital to document weight regain, complications, and when conservative measures fail. Providing detailed medical records and specialist evaluations can strengthen your case.
For better approval tips, navigate the pre-approval process well. This includes initial talks with bariatric surgeons and checking insurance. Being well-prepared is essential.
Maximizing your chances for revision surgery approval is a big step towards your weight loss goals and better health.
FAQ
What is gastric bypass revision surgery?
Gastric bypass revision surgery is a second surgery done after the first one. It’s to fix problems or if you didn’t lose enough weight.
Why is revision surgery necessary?
It’s needed to fix weight gain, problems with the surgery, and metabolic issues after the first surgery.
What are the medical necessity criteria for revision surgery?
To get it covered, you need to show weight gain or problems like ulcers, fistulas, or malnutrition.
How do I know if my insurance covers gastric bypass revision surgery?
Coverage varies by insurance. Check with your provider to see what they cover and their rules.
What are the common reasons for insurance denial?
Insurance might deny it if it’s not medically necessary, if you don’t have the right documents, or if you haven’t tried other treatments.
How can I prepare a strong case for insurance approval?
To strengthen your case, collect important medical records, get specialist opinions, and follow post-surgery rules.
What is the pre-approval process for gastric bypass revision surgery?
The process starts with a doctor’s visit, then checking your insurance, and asking for pre-approval.
How can I demonstrate conservative measure exhaustion?
Show you’ve tried other treatments by documenting diet and exercise plans under supervision.
What are my options if my insurance denies my claim?
You can appeal, ask for a peer-to-peer review, or look into external reviews if denied.
Are there alternative funding options available?
Yes, you can look into medical loans, hospital charity, clinical trials, or even medical tourism.
What are the most common gastric bypass revision options?
Common options include changing from one surgery to another, like RNY to sleeve, or fixing surgery problems.
How can I maximize my chances for revision surgery approval?
Understand the medical criteria, insurance rules, and the pre-approval steps to increase your chances.
What is the role of a bariatric surgeon in the pre-approval process?
A bariatric surgeon is key by providing medical records, specialist opinions, and guiding through the approval process.
Can I get insurance to cover revision bariatric surgery?
Yes, if you meet the medical criteria and follow the approval steps, insurance might cover it.
What is revisional bariatric surgery?
It’s surgery to fix or change previous bariatric surgery, like gastric bypass revision.
References
Government Health Resource. Evidence-Based Medical Guidance. Retrieved from https://apastyle.apa.org/




































