Plastic surgery restores form and function through reconstructive procedures, cosmetic enhancements, and body contouring.
Send us all your questions or requests, and our expert team will assist you.
The initial consultation is a comprehensive medical and anatomical evaluation. This is the phase in which the surgeon assesses the feasibility of the procedure and aligns the surgical plan with the patient’s goals. It is a dialogue focused on safety, anatomy, and realistic outcomes.
The surgeon reviews the patient’s weight history, specifically looking for stability. A history of “yo-yo” dieting is a red flag, as future weight fluctuations can compromise surgical outcomes. The consultation establishes the partnership required for the lengthy recovery process.

Advanced clinics use 3D imaging technology to bridge the communication gap between patients and surgeons. High-resolution scanners create a digital avatar of the patient’s lower body. The surgeon can then manipulate this model to simulate the removal of skin and fat.
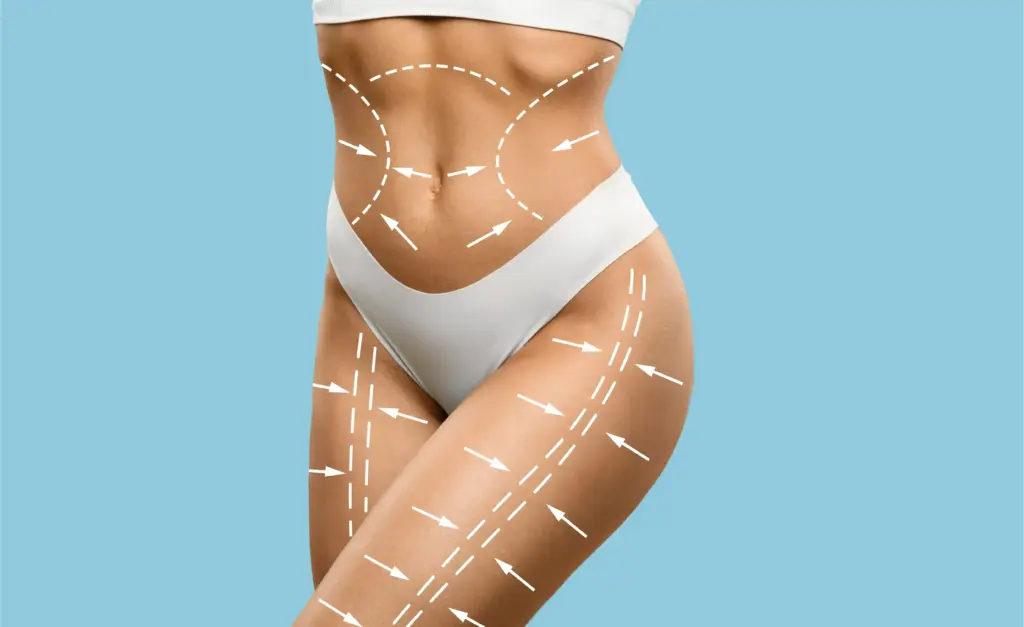
This visualization helps the patient understand the trade-off between contour improvement and scar length. Seeing the potential results on their own body helps set realistic expectations. It also assists in planning the specific lift vectors—vertical, horizontal, or oblique.

The “pinch test” is a fundamental part of the physical exam. The surgeon pinches excess tissue on the inner and outer thighs to assess the thickness of the subcutaneous fat and the laxity of the skin. This determines how much tissue can be safely removed.
By simulating the lift manually in the mirror, the surgeon demonstrates what can be achieved. They also assess the “anchoring” quality of the groin tissue. If the groin tissue is loose, additional suspension techniques will be needed to prevent the scar from migrating.
The biomechanical quality of the skin is scrutinized. The surgeon checks for striae (stretch marks) and signs of sun damage. Skin with poor elasticity requires a different tensioning approach than healthy, elastic skin to avoid complications in wound healing.
The assessment also covers the vascular status of the legs. The surgeon checks for varicose veins or signs of venous insufficiency. Good blood flow is critical for the healing of the extended skin flaps created during a thigh lift.

A significant portion of the consultation is dedicated to scar planning. Thigh lift scars are permanent and can be extensive. For a medial lift, the surgeon maps the incision to sit in the natural groin crease or along the inseam of the leg.
Patients are encouraged to bring their preferred underwear or swimwear to the consultation. The surgeon marks the proposed incision lines relative to these garments. This collaborative planning aims to conceal the scars as much as possible within the patient’s lifestyle choices.
Surgical readiness hinges on weight stability. Patients must be at or near their goal weight for at least 6 to 12 months before surgery. Operating on a patient who is still losing weight can lead to recurrent laxity. Operating on a patient who gains weight post-op can stretch the scars.
BMI (Body Mass Index) is also a safety factor. Most surgeons have a BMI cutoff (typically 30-35) above which elective body contouring is considered too risky due to increased chances of infection, wound dehiscence, and deep vein thrombosis.

Send us all your questions or requests, and our expert team will assist you.

A full battery of pre-operative tests is ordered to ensure the patient can withstand the metabolic stress of surgery. This includes a Complete Blood Count (CBC) to check for anemia and infection, and a coagulation profile to ensure normal clotting.
Nutritional markers such as albumin and prealbumin are checked, especially in post-bariatric patients who may have absorption issues. Adequate protein levels are non-negotiable for wound healing. Uncontrolled diabetes or high blood pressure must be managed before a date is set.
Nicotine is a potent vasoconstrictor, meaning it constricts blood vessels and reduces oxygen flow to tissues. In a thigh lift, where long flaps of skin rely on a delicate blood supply, nicotine use is a recipe for disaster (tissue necrosis).
A strict zero-tolerance policy is enforced. Patients must cease all nicotine products—including vapes, gum, and patches—for at least 4 to 6 weeks before and after surgery. Cotinine tests (urine tests for nicotine metabolites) may be administered to verify compliance.
The groin is a hub for lymphatic drainage from the legs. The surgeon evaluates the patient’s history for any swelling or lymphedema. Previous groin surgeries (e.g., hernia repairs) are noted, as they may have altered lymphatic pathways.
Understanding the lymphatic anatomy is crucial to avoiding post-operative complications like lymphoceles (fluid collections) or chronic swelling. In high-risk patients, a specialized surgical plan sparing the deep lymphatic bundles is developed.

The consultation assesses the patient’s mental readiness for the recovery. A thigh lift recovery can be physically restrictive and emotionally taxing. Patients must be prepared for a period of limited mobility and dependency on others.
Realistic expectations are reinforced. The surgery improves contour but does not produce “perfection.” Patients with body dysmorphic disorder (BDD) or unrealistic expectations are counseled that surgery may not be the appropriate path for them.
Patients are advised to prepare their home environment (“nesting”) before the surgery date. This involves setting up a recovery station where they can lie comfortably with their legs elevated. They need to arrange help with daily tasks such as cooking, cleaning, and pet care.
Mobility aids, such as a raised toilet seat or a walker, may be recommended for the first week. Having these logistics sorted in advance reduces anxiety and allows the patient to focus entirely on healing during the critical early days.

You should be within 10 to 15 pounds of your goal weight. More importantly, your weight should be stable. Losing a significant amount of weight after the surgery will cause the skin to loosen again, potentially requiring a second surgery.
Vaping contains nicotine, which constricts blood vessels. This cuts off the oxygen supply to the skin borders that are trying to heal. Using nicotine before or after a thigh lift significantly increases the risk of the wound opening up or the skin turning black and dying.
You will stand in front of a specialized camera that takes a 360-degree scan of your body. The software creates a 3D model on a screen. The surgeon then digitally edits the model to show you how your legs might look after the skin is removed and tightened.
Yes, most surgeons require a medical clearance from your primary care physician. This ensures that your heart, lungs, and general health are strong enough for general anesthesia and the recovery process.
Scar placement is planned to be hidden by swimwear, but this depends on the extent of the lift. A mini thigh lift scar is hidden in the groin. A vertical thigh lift scar runs down the inner leg and will be visible in shorts or a bikini, though it fades over time.

 Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery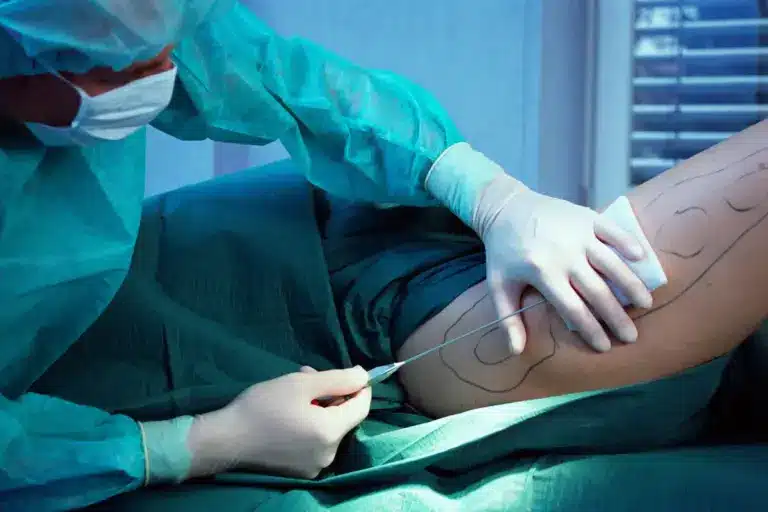 Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)