Plastic surgery restores form and function through reconstructive procedures, cosmetic enhancements, and body contouring.
Send us all your questions or requests, and our expert team will assist you.
Thighplasty is a major surgical procedure performed under general anesthesia. This ensures the patient is entirely unconscious and that the muscles are relaxed, allowing precise manipulation of the tissues. A board-certified anesthesiologist monitors the patient’s vital signs, including heart rate, blood pressure, and oxygen saturation, throughout the operation.
Safety protocols are rigorous. Sequential Compression Devices (SCDs) are placed on the calves to massage the legs and prevent blood clots (Deep Vein Thrombosis). Warming blankets help maintain core body temperature, which is essential for proper blood clotting and metabolism.

The surgery typically begins with liposuction, even if the patient is thin. This step is not just for fat removal; it is used to “dissect” the tissue. By running the cannula through the subcutaneous plane, the surgeon loosens the skin from the underlying fascia while preserving the lymphatics and nerves.
This technique, often called “lipo-dissection,” preserves the blood supply better than using a knife alone. It creates a honeycomb pattern of tissue that allows the skin to be redraped smoothly. It also debulks the heavy fat that pulls on the skin, ensuring a lighter, tighter flap.

For the standard vertical thigh lift, the incision is designed along the medial line (inseam). The surgeon incises through the skin and fat down to the deep fascia. Great care is taken to stay superficial to the deep lymphatic drainage system to prevent chronic swelling.
The placement of this incision is critical. It is positioned slightly posteriorly (toward the back) so that it is not visible when the patient is standing with legs together or facing forward. The length of the incision is determined solely by the amount of skin to be removed.
The most critical technical step is anchoring the lift. Simply sewing skin to skin will fail; gravity will pull the scar down, causing a “dropped scar” deformity and widening the vaginal or scrotal opening. To prevent this, the surgeon uses high-tensile permanent sutures to anchor the deep dermis of the thigh flap to Colles’ fascia.
Colles’ fascia is a tough, fibrous band of connective tissue in the perineum. By securing the flap to this immovable structure, the surgeon creates an internal suspender. This ensures the tension is held by the deep tissues, not the skin closure, providing a stable and long-lasting lift.

Many modern surgeons utilize “drainless” techniques to improve recovery. Instead of using plastic tubes to drain fluid, the surgeon uses Progressive Tension Sutures (PTS). These are internal quilting stitches that tack the skin flap down to the underlying muscle fascia.
This quilting closes the “dead space” where fluid would otherwise collect (seroma). It also distributes the tension across the entire thigh rather than concentrating it along the incision line. This reduces pain and eliminates the hassle and infection risk associated with external drains.
In addition to sutures, fibrin sealants or tissue glues may be sprayed into the surgical pocket before closure. These biological adhesives trigger the clotting cascade, helping the tissues stick together immediately.
This technology further reduces the risk of bruising and fluid collection. It acts as an internal dressing, sealing the disrupted lymphatic channels during the dissection. This promotes faster adherence of the skin flap to its new bed.

Send us all your questions or requests, and our expert team will assist you.

Once the flap is anchored and the fat is contoured, the excess skin is measured and removed. This is a “tailoring” process. The surgeon pulls the skin up and back, marking the overlap. The excision is performed conservatively to ensure the wound can close without excessive tension.
Over-resection is a significant risk; if the closure is too tight, it can cut off the blood supply or cause the wound to pull apart (dehiscence). The goal is a snug, smooth fit that allows for normal movement, not a tight drum-like surface that restricts the legs.
The incision is closed in multiple layers. Deep absorbable sutures bring the strong fascial layers together. Subcutaneous sutures close the fat layer. Finally, the skin is closed with a running subcuticular (under the skin) stitch that dissolves on its own.
This multi-layered approach ensures strength and waterproofing. Surgical tape (Steri-Strips) and a specialized skin glue are applied over the incision to seal it from bacteria. This meticulous closure is essential for minimizing the final scar width.
It is challenging for patients to visualize the potential surgical outcomes. We use technology to create a shared vision.

To manage post-operative pain, surgeons often inject Exparel, a long-acting liposomal anesthetic, into the surgical site. This numbs the area for up to 72 hours. It significantly reduces the need for narcotic pain medication, allowing patients to feel clearer and move sooner.
Early mobilization is key to preventing blood clots. By controlling pain at the source, patients can walk comfortably within hours of surgery. This fits into the Enhanced Recovery After Surgery (ERAS) protocols used in premium centers.
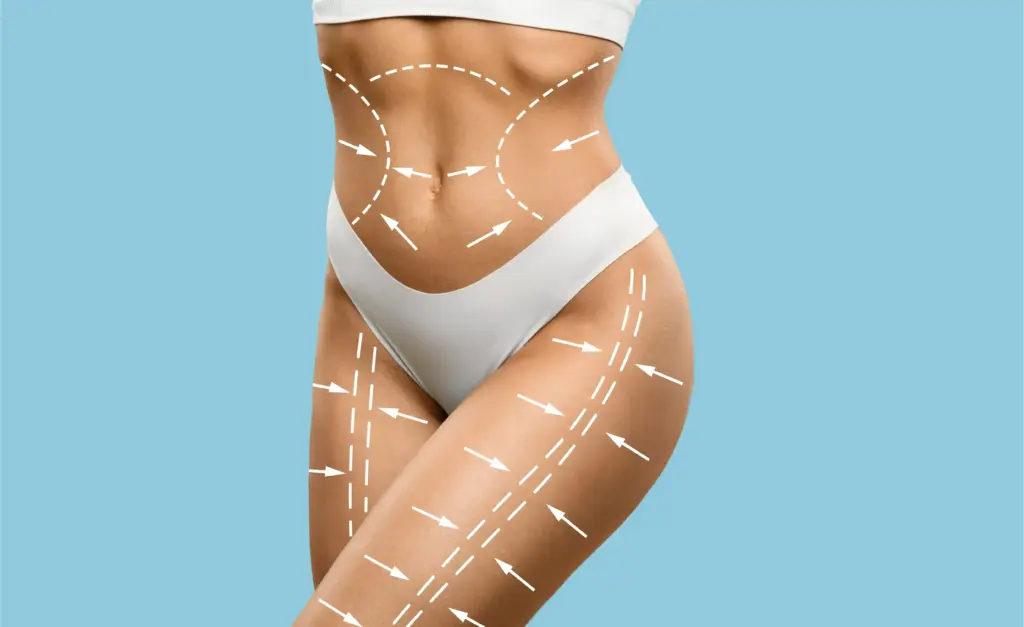
In some cases, Vaser (ultrasound-assisted lipo) or Renuvion (helium plasma) is used. Vaser uses sound waves to emulsify fat, making it easier to remove without damaging vessels. Renuvion delivers heat to the skin’s underside, shrinking collagen fibers for extra tightening.
These technologies are adjuncts that enhance the result. They are handy for patients with borderline skin elasticity or those needing significant fat reduction along with the lift. They refine the “high definition” look of the thigh muscles.
After surgery, the patient is moved to the recovery room (PACU). Nurses monitor foot circulation and the color of the thigh skin to ensure the bandages are not too tight. The patient is placed in a specific position—usually with legs slightly bent—to reduce pull on the incisions.
Immediate walking is assisted and encouraged once the anesthesia wears off. This keeps the calf muscle pump working, which is the body’s natural defense against clots. Instructions on hygiene and drain care (if used) are provided before discharge.

It depends on the technique. Many modern surgeons use “drainless” quilting sutures to close the space where fluid collects, eliminating the need for drains. However, in complex cases or in patients with massive weight loss, drains may still be used for a few days to ensure safety.
Most patients describe the pain as a deep soreness or tightness, similar to an intense leg workout, rather than sharp pain. The use of long-acting numbing injections (Exparel) significantly reduces discomfort in the first few days.
You will walk the same day as your surgery. Short, frequent walks around your home are mandatory to keep blood flowing and prevent clots. However, you must avoid spreading your legs wide or lifting heavy objects.
For a vertical thigh lift, the scar runs from the groin crease down the inner thigh toward the knee. Ideally, it is placed slightly toward the back so it is not visible when you stand facing someone.
A thigh lift typically takes between 2 and 3.5 hours, depending on whether it is a mini or full lift and whether liposuction is performed extensively. It is often shorter than a tummy tuck but requires improved precision in closure.

 Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)