Plastic surgery restores form and function through reconstructive procedures, cosmetic enhancements, and body contouring.
Send us all your questions or requests, and our expert team will assist you.
For the vast majority of cases, local anesthesia is used. The surgeon injects a mixture of lidocaine (numbing agent) and epinephrine (vasoconstrictor) around and under the tattoo. Epinephrine reduces bleeding, allowing a clear visual field.
The injection is done slowly to minimize discomfort. Bicarbonate is often added to the solution to buffer the acidity, reducing the “sting” of the injection. Once the area is verified to be completely numb, the surgery begins.

Using a scalpel, the surgeon incises along the marked lines, cutting through the full thickness of the dermis and into the subcutaneous fat. The goal is to remove the entire block of tissue containing the tattoo pigment.
The excision must be deep enough to remove all ink, which usually resides in the mid-to-deep dermis, but superficial enough to spare deep nerves and large blood vessels. The tissue is removed in one piece, ensuring no pigment is left behind at the margins.

To close the gap left by the tattoo, the surgeon must loosen the surrounding skin. This process is called undermining. The scalpel or scissors are used to separate the skin and fat from the underlying muscle fascia for several centimeters around the wound.
Undermining releases the skin from its attachments, allowing it to slide forward and cover the defect with less tension. This step is critical for preventing the scar from stretching or widening later.
Once the tissue is removed, the surgeon controls any bleeding using electrocautery. This device uses heat to seal small blood vessels. Meticulous hemostasis is vital to prevent a hematoma (collection of blood) from forming under the closed incision.
A hematoma can put pressure on the wound, causing pain and increasing the risk of infection or wound separation. The surgeon ensures the bed is arid before beginning the closure.

Closing the wound is an architectural process. It is done in layers to distribute the tension. First, deep absorbable sutures are placed in the dermis and fascia. These stitches hold the strength of the closure and bring the edges together.
By taking the tension off the surface with deep sutures, the outer skin can be closed gently. This prevents “track marks” from the stitches and ensures a fine line scar. The deep sutures dissolve on their own over several months.
The final layer is the skin surface. The surgeon uses fine, non-absorbable sutures (like nylon) or a running absorbable stitch just under the skin surface (subcuticular). The goal is precise alignment of the skin edges to ensure a flat scar.
In some cases, surgical glue or adhesive strips (Steri-Strips) are used to reinforce the closure. The choice of surface closure depends on the location; areas under high tension, like the back, typically get external stitches, while the face may get subcuticular closure.

Send us all your questions or requests, and our expert team will assist you.

A sterile dressing is applied to the wound. This typically consists of a non-stick layer, gauze for absorption, and tape. In areas prone to swelling or movement (like the legs), a compression bandage (Coban or Ace wrap) is applied.
Compression helps to minimize swelling and supports the soft tissues during the initial healing phase. It also serves as a reminder to the patient to protect the area and restrict movement.
After the procedure, patients are monitored briefly to ensure they are feeling well and that there is no immediate bleeding. Since local anesthesia is used, recovery is rapid. Patients remain awake and alert throughout.
Pain is typically minimal once the anesthesia wears off, often manageable with over-the-counter acetaminophen or ibuprofen. Patients are given verbal and written instructions on wound care and activity restrictions before discharge.
For the first 48 hours, keeping the wound elevated and dry is crucial. Activity restrictions depend on location. An arm excision may require avoiding heavy lifting for 2 weeks. A leg excision usually requires strict elevation and limited walking to prevent throbbing and bleeding.
Patients are instructed to avoid submerging the wound in water (e.g., baths or pools) until the sutures are removed and the wound is fully sealed. Showers are usually permitted after 24-48 hours, provided the wound is patted dry immediately.

If tissue expansion is used, the surgery involves placing the expander. The surgeon creates a pocket under the normal skin, inserts the silicone balloon, and places the inflation port. The incision is closed, and the expansion process begins weeks later.
This is a more invasive surgery requiring strict sterile technique to prevent infection of the implant. The recovery involves managing the drains (if used) and caring for the port site during the expansion weeks.
Surgeons use specific scales to grade the severity of defects, which dictates the surgical approach.
For skin grafts, two sites are managed: the tattoo removal site and the donor site (usually the thigh). The tattoo is excised, and the graft is stapled or sewn into place. A bolster dressing is sewn over the graft to press it firmly against the wound bed.
The bolster must remain dry and undisturbed for roughly 5 to 7 days to allow the graft to “take” (grow new blood vessels). Recovery is more involved due to the pain associated with the donor site, which feels like a severe scrape or burn.

The surgery itself is painless because of the local anesthesia. You will feel pressure and movement, but no sharp pain. After the numbing wears off (3-4 hours later), you will feel soreness similar to that of a deep cut or scrape, which is usually managed with Tylenol.
Yes, almost all surgical tattoo removals require stitches. There are usually dissolving stitches deep under the skin and non-dissolving stitches on the surface that need to be removed in 10 to 14 days.
Usually, yes, after the first 24 to 48 hours. You can let soapy water run over the wound, but do not scrub it. Afterward, pat it dry gently and apply a fresh bandage. Do not soak in a bath or pool for at least 2 weeks.
If the wound opens (dehiscence), it is usually small. Do not panic. Contact your surgeon. Small openings often heal on their own with ointment and dressing changes. Large openings may need to be re-stitched, but this is rare if you follow activity restrictions.
A typical simple excision takes about 30 to 60 minutes. Complex cases involving flaps or skin grafts may take 1 to 2 hours. It is an outpatient procedure, meaning you go home the same day.

 Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery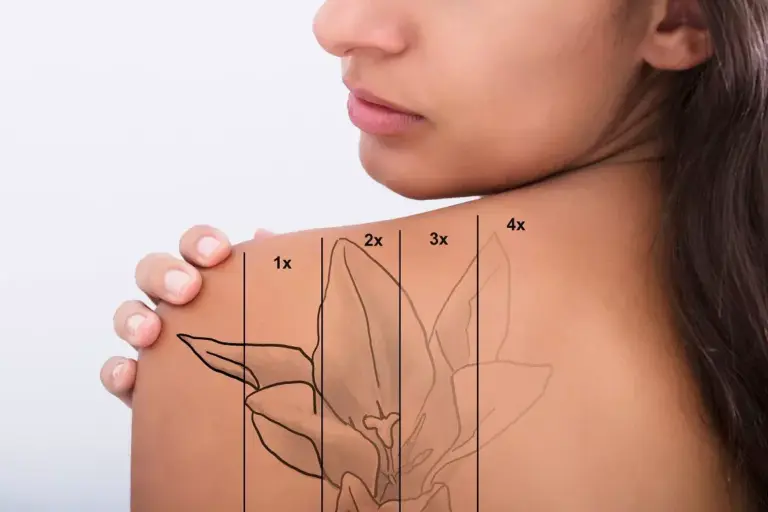 Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery Plastic Surgery
Plastic Surgery
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)