Plastic surgery restores form and function through reconstructive procedures, cosmetic enhancements, and body contouring.
Send us all your questions or requests, and our expert team will assist you.
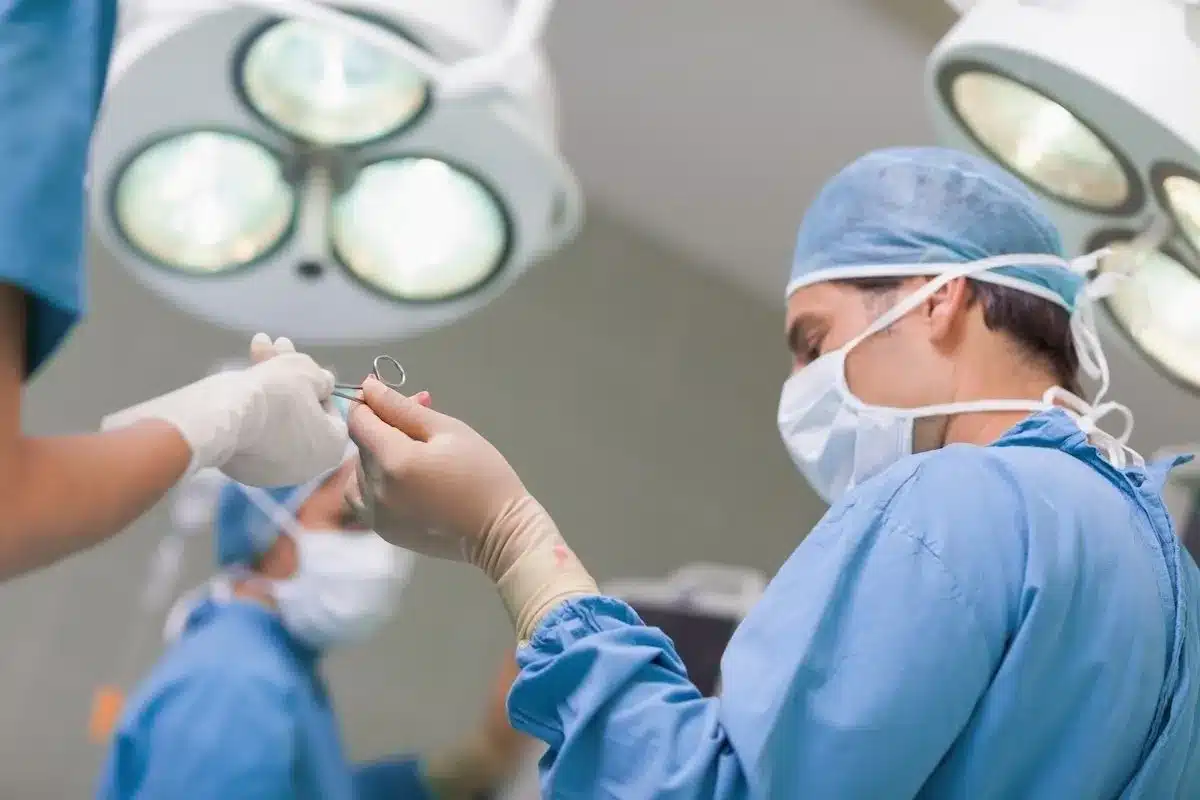
When surgery is required for severe cellulitis, necrotizing fasciitis, or extensive abscesses, it takes place in a sterile operating room. The environment is controlled to prevent secondary infections. The patient is positioned to give the surgeon optimal access to the affected limb or body part.
The room is equipped with advanced lighting and suction devices. For necrotizing cases, the setup allows for aggressive and rapid excision. The surgical team includes the lead surgeon, anesthesiologist, scrub nurses, and circulating nurses, all coordinating to manage the potentially unstable patient.
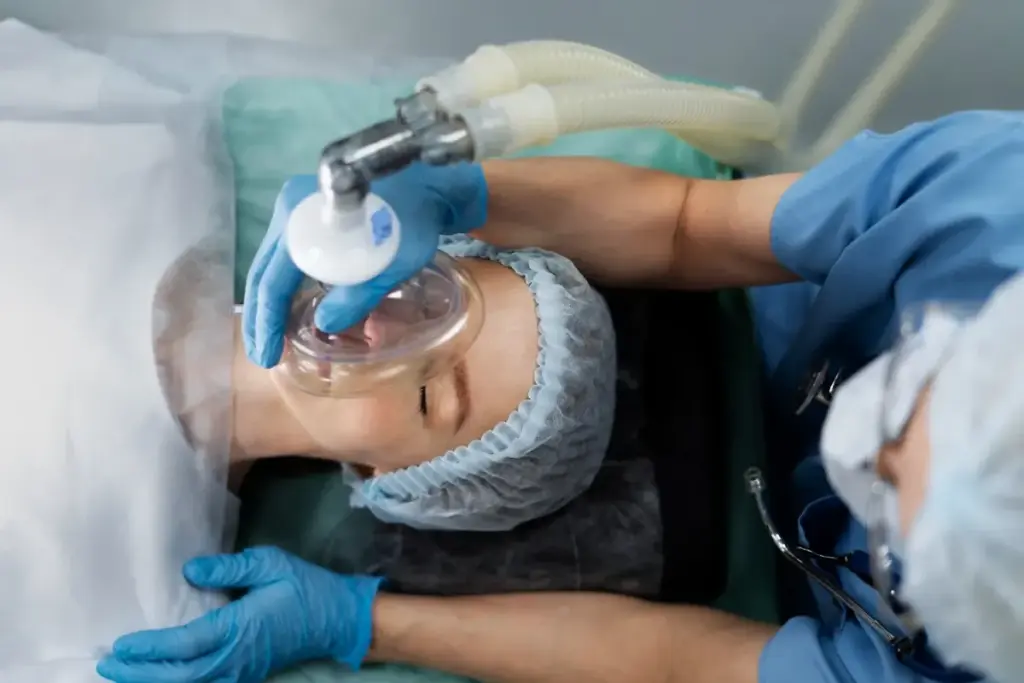
The type of anesthesia depends on the severity of the procedure. For simple bedside Incision and Drainage (I&D), local anesthesia (lidocaine) injected around the site is sufficient. However, the acidic environment of infected tissue can reduce the effectiveness of regional anesthesia.
For extensive debridement or deep abscesses in the operating room, general anesthesia or regional blocks (like a spinal block for leg infections) are used. This ensures the patient is unconscious or completely numb, allowing the surgeon to thoroughly explore and clean the wound without causing pain.

The surgeon makes a decisive incision over the point of maximal fluctuation (the softest, most fluid-filled area). The incision is large enough to allow complete evacuation of pus and to insert instruments for breaking up internal pockets (loculations).
Once opened, the cavity is irrigated copiously with saline to wash out bacteria and debris. The surgeon explores the depth of the cavity to ensure no tracts are missed. The goal is to convert a complex, infected pocket into a clean, open wound that can heal from the inside out.
In cases of necrosis, the surgeon excises tissue until healthy, bleeding margins are observed. This is often described as “cutting until it bleeds,” as bleeding indicates viable tissue with a blood supply. The appearance of the tissue (grey, dull, non-contractile muscle) guides the excision.
This can be a disfiguring procedure that requires the removal of skin, fat, and fascia. The priority is life over limb, and limb over appearance. Samples are sent to pathology and microbiology for guidance on further treatment.
Surgical wounds from cellulitis interventions are rarely stitched closed immediately. Closing an infected wound would trap bacteria inside, leading to a new abscess. Instead, the wound is left open to drain.
The cavity is packed with sterile materials, such as iodoform gauze or alginate, which absorb exudate and keep the wound edges apart. This technique, known as healing by secondary intention, allows the wound to fill in with granulation tissue from the bottom up.
Pain management after surgery is a priority. The inflammatory nature of cellulitis, combined with surgical trauma, creates significant pain. A multimodal approach is used, combining opioid analgesics, acetaminophen, and NSAIDs (if not contraindicated).
Elevation of the limb is strictly enforced to reduce throbbing and swelling. Nerve blocks administered during surgery can provide relief for 12 to 24 hours post op. The goal is to keep pain at a manageable level to allow for rest and eventual mobilization.
For large, open surgical wounds, a wound vac (Negative Pressure Wound Therapy) is often applied in the recovery phase. A sponge is fitted into the wound, sealed with film, and connected to a pump.
This device draws out infected fluid, reduces swelling, and pulls the wound edges together. It significantly speeds up the formation of granulation tissue (the red, vascular tissue that heals wounds) and reduces the number of dressing changes required, improving patient comfort.
Post surgery, patients remain on IV antibiotics. The specific drug may be adjusted based on the results of the cultures taken during surgery. This targeted therapy is more effective and reduces the risk of developing resistance.
As the patient’s fever resolves and the wound shows signs of healing, the medical team plans the transition to oral antibiotics. This switch is a key milestone for hospital discharge. The duration of antibiotic treatment depends on the severity of the initial infection.
Recovery in the hospital involves monitoring for signs of sepsis resolution. Nurses frequently check vital signs and assess the wound for signs of necrosis. Blood work is repeated to ensure white blood cell counts are normalizing.
Nutrition plays a huge role here; high-protein diets or supplements are ordered to fuel tissue repair. Physical therapy may be initiated early to maintain the affected limb’s range of motion without compromising the wound.
If cellulitis progresses to sepsis, recovery is prolonged. Patients may experience “post-sepsis syndrome,” characterized by fatigue, muscle weakness, and cognitive fog. Recovery involves rebuilding stamina.
The body has undergone a massive metabolic stress event. Rehydration and electrolyte balance are maintained. Patients are educated that feeling “wiped out” is a regular part of recovering from a systemic infection and that full energy levels may take weeks to return.
Discharge occurs when the patient is stable, afebrile (no fever) for 24 hours, and able to tolerate oral antibiotics. The wound must be clean or have a manageable care plan (like home health nurse visits).
Pain must be controlled with oral medication. The skin redness should be receding. The patient receives detailed instructions on wound care, antibiotic adherence, and when to follow up.

For patients with wound vacs, PICC lines, or complex dressings, home health nursing is arranged. A nurse visits the home to change dressings, draw blood, or administer IV antibiotics.
This allows patients to recover in the comfort of their homes while maintaining medical oversight. Regular outpatient clinic visits with the surgeon are scheduled to monitor the wound’s progress and decide when to stop antibiotics or remove the wound vac.

Send us all your questions or requests, and our expert team will assist you.
If you have a packed open wound, the packing is usually changed once or twice a day. This keeps the wound clean and allows it to heal from the bottom up. It can be uncomfortable, so taking pain medicine beforehand is recommended.
It depends on the location and severity. Generally, you should minimize walking to keep swelling down. Short trips to the bathroom are okay, but you should keep the leg elevated most of the time. Crutches or a walker might be prescribed.
Healthy granulation tissue looks like bright red, bumpy flesh, similar to a raspberry. This is a good sign! It means the wound is getting good blood flow and is healing. If it looks grey or yellow, tell your doctor.
As the swelling goes down and the infection heals, the stretched skin often dies and peels off. This is called desquamation. It is a regular part of the recovery process and reveals new, healed skin underneath.
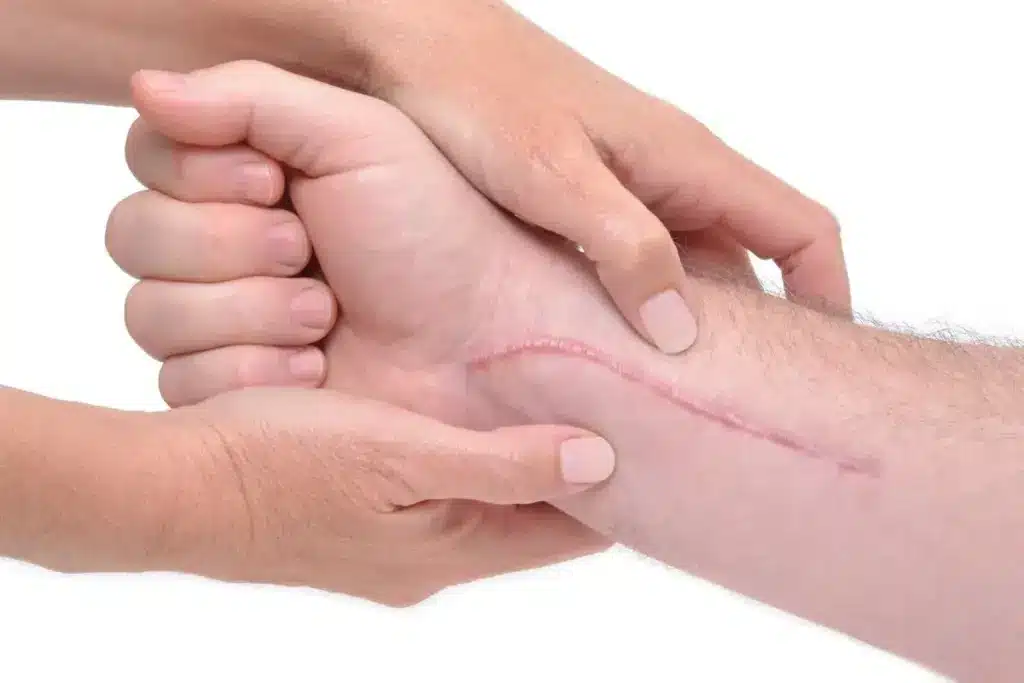
If you had surgery, yes, there will be a scar. Initially, it might look indented or wide. Over time (6-12 months), it will flatten and fade. Surgical scars from abscesses can be revised later if they are cosmetically bothersome.



Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)