Plastic surgery restores form and function through reconstructive procedures, cosmetic enhancements, and body contouring.
Send us all your questions or requests, and our expert team will assist you.
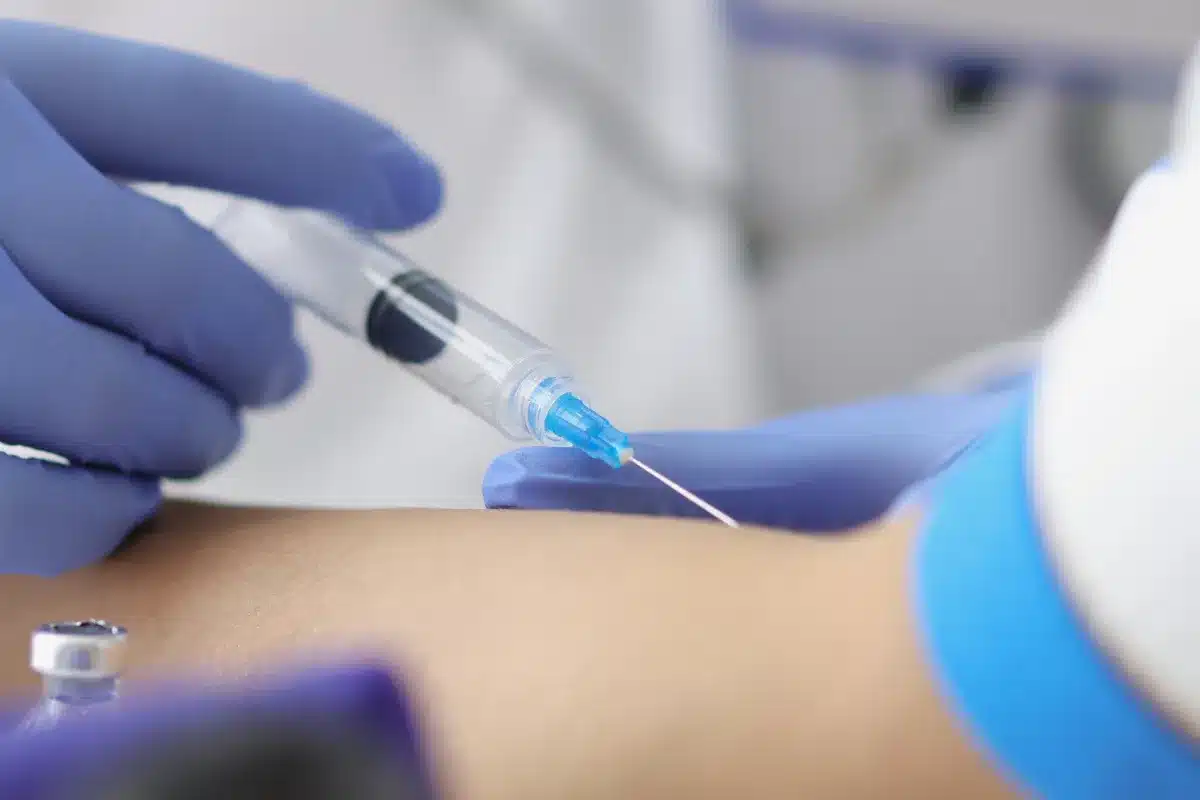
For moderate to severe cellulitis or when oral antibiotics have failed, intravenous (IV) antibiotic therapy is the standard of care. This procedure involves administering potent antimicrobial agents directly into the bloodstream, ensuring rapid, high tissue concentrations of the drug. The choice of antibiotic is often empiric initially, covering the most likely pathogens, such as Streptococcus and Staphylococcus.
This medical procedure is typically initiated in a hospital setting or an infusion center. It requires the placement of a peripheral IV line. In cases requiring long-term therapy, a peripherally inserted central catheter (PICC) may be placed to spare the peripheral veins. The response to IV therapy is closely monitored to determine when a transition to oral medication is safe.
When cellulitis is accompanied by a pus collection, known as an abscess, antibiotics alone are insufficient. The gold standard procedure is Incision and Drainage (I&D). This surgical intervention involves making an incision over the fluctuant area to allow purulent material to escape, thereby reducing bacterial load and tissue pressure.
The procedure is performed under local anesthesia. After the incision, the surgeon breaks up loculations (internal pockets) to ensure complete drainage. The cavity may be packed with sterile gauze to prevent premature closure and allow continued drainage. This mechanical removal of infection is critical for resolution.
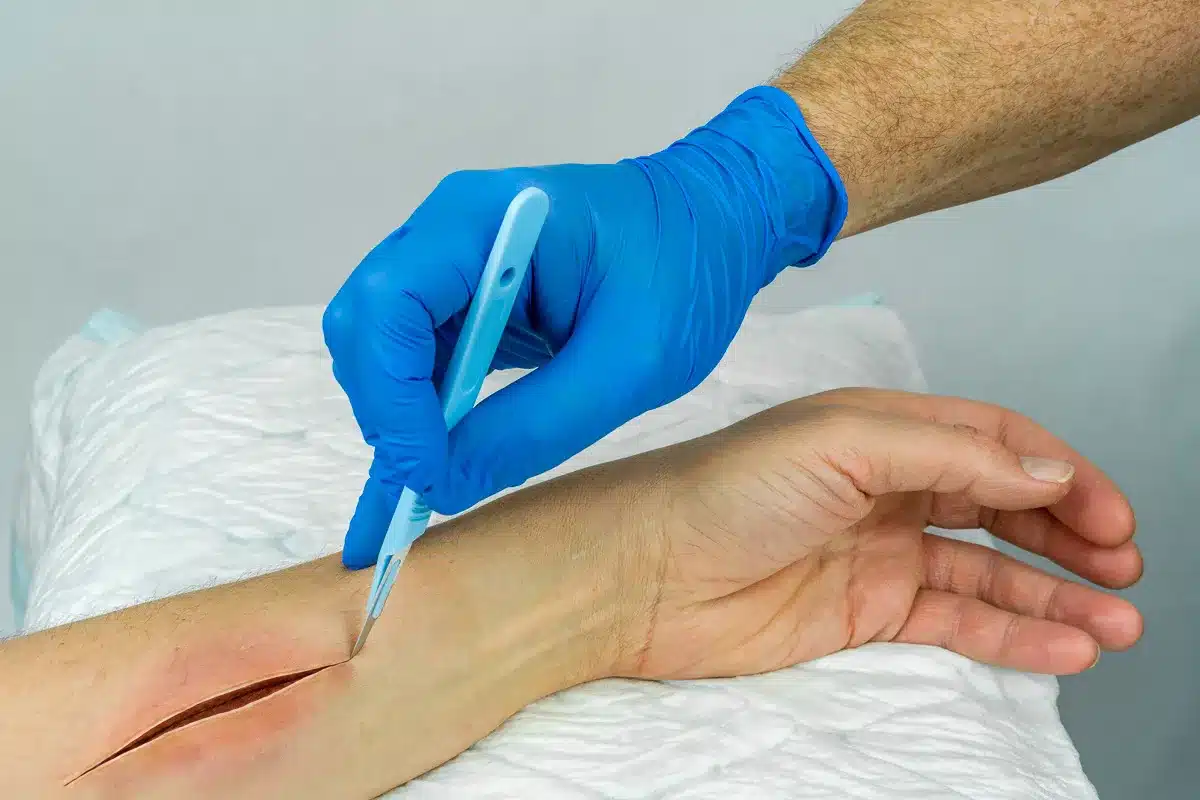
In severe cases where the infection has caused tissue death (necrosis), surgical debridement is required. This procedure involves the sharp excision of dead, infected, or nonviable tissue. Removing this necrotic burden is essential because dead tissue has no blood supply and antibiotics cannot reach it, making it a haven for bacteria.
Debridement is often performed in an operating room under general or regional anesthesia. The surgeon cuts away tissue until healthy, bleeding tissue is reached. This process may need to be repeated (serial debridement) to ensure all infection is cleared before the wound can be closed or grafted.
Rarely, the swelling from severe cellulitis can increase pressure within a muscle compartment to dangerous levels, cutting off blood flow. This emergency condition requires a fasciotomy. The surgeon makes long incisions through the skin and the fascia (the connective tissue covering the muscle) to relieve the pressure.
This limb-saving procedure restores circulation to the muscles and nerves. The wounds are typically left open initially to accommodate swelling and are closed or grafted later, once the swelling has subsided and the infection is controlled.

Diagnostic clarity is often needed to distinguish between uncomplicated cellulitis and a deep abscess that isn’t visible on the surface. Ultrasound-guided aspiration is a procedure in which a radiologist or surgeon uses real-time imaging to guide a needle into a suspected fluid collection.
If fluid is found, it is aspirated (drawn out) and sent for culture to identify the specific bacteria. This procedure can be both diagnostic and therapeutic, as removing the fluid can relieve pressure and pain while providing crucial data for targeted antibiotic selection.
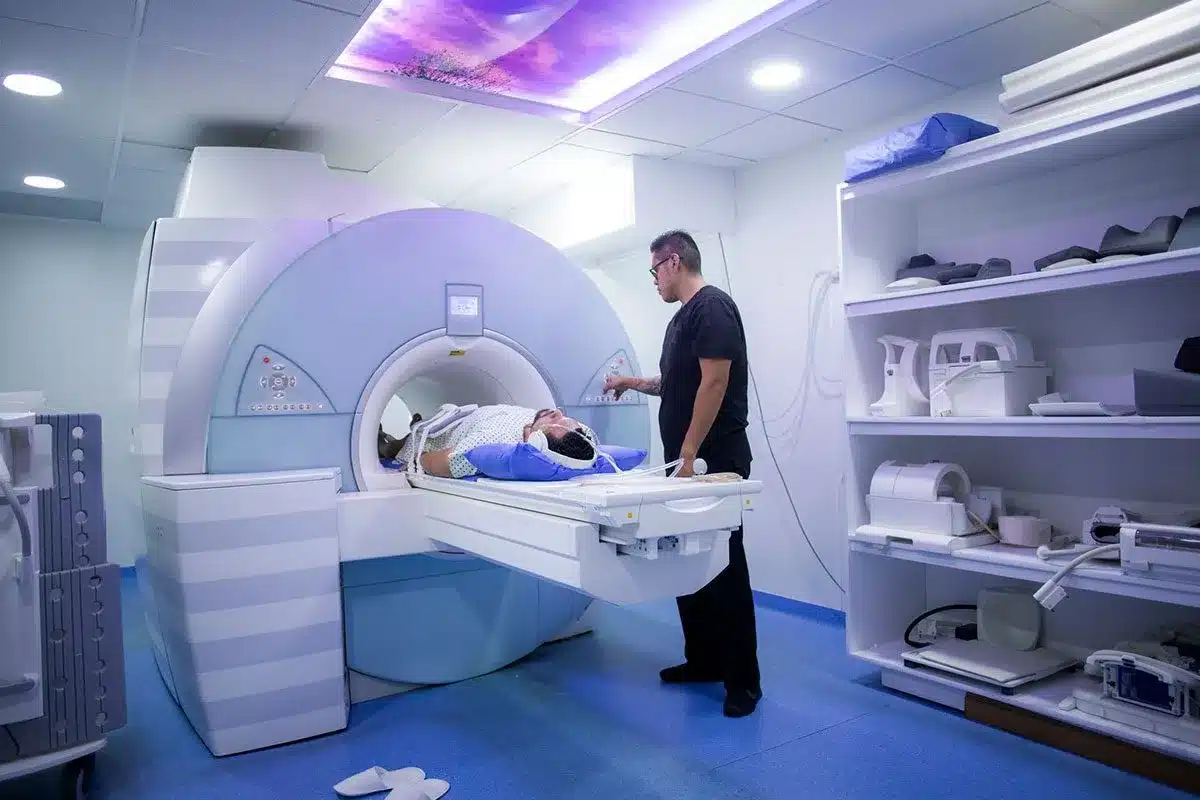
Advanced imaging procedures are vital when the extent of the infection is unclear or deep-structure involvement is suspected. Magnetic Resonance Imaging (MRI) is the gold standard for visualizing soft tissue and distinguishing cellulitis from osteomyelitis (bone infection) or necrotizing fasciitis.
Computed Tomography (CT) scans are faster and are often used in the emergency setting to detect gas in tissues or deep abscesses. These diagnostic procedures dictate the surgical or medical management plan by providing a detailed map of the infection’s anatomy.
To determine whether bacteria have spread to the bloodstream (bacteremia), blood cultures are drawn. This procedure involves collecting blood samples from two different venipuncture sites to maximize accuracy and prevent contamination. The blood is incubated to see if bacteria grow.
While often negative in uncomplicated cellulitis, this procedure is critical in patients with high fevers or signs of sepsis. Identifying the specific organism in the blood allows for the de-escaon of antibiotics to a targeted, narrow-specnarrow-spectrumoving efficacy and reducing side effects.
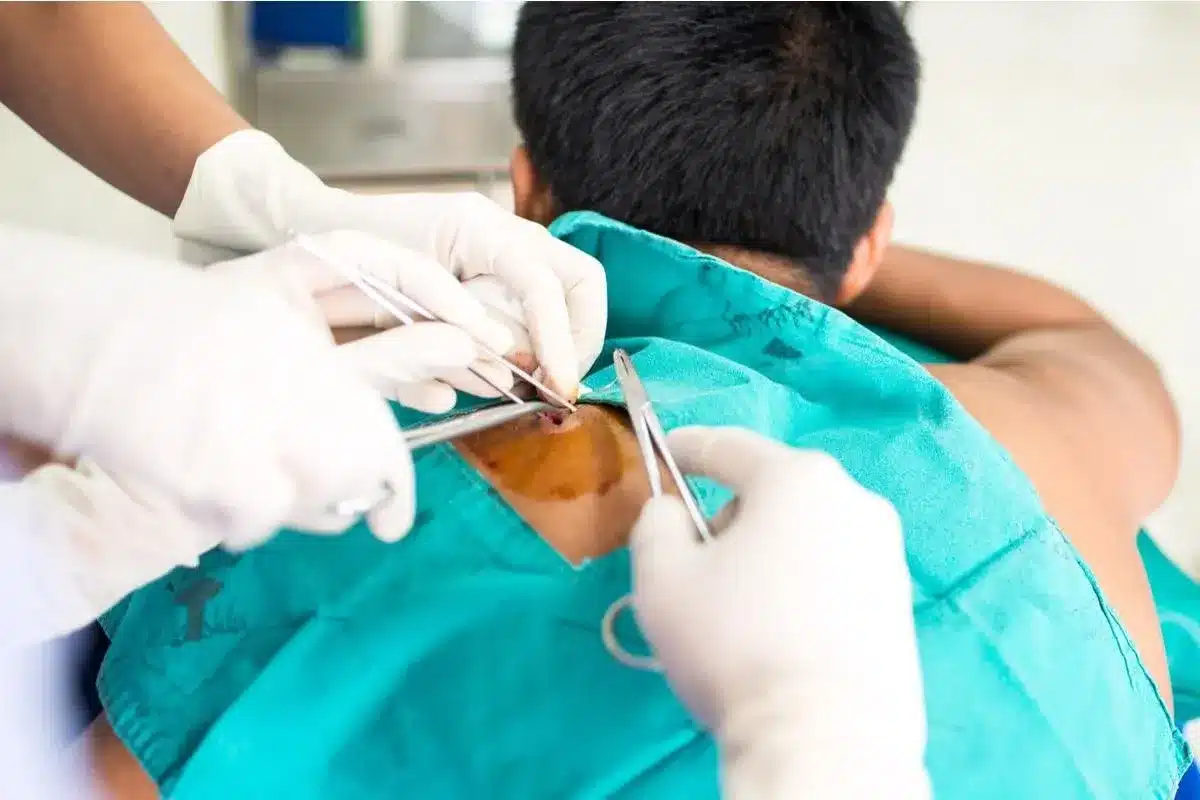
When cellulitis does not respond to standard treatment or has an unusual appearance, a skin biopsy may be performed. This involves removing a small sample of full-thickness skin for microscopic examination by a pathologist.
This procedure helps rule out conditions that mimic cellulitis, such as inflammatory dermatoses, vasculitis, or rare fungal and mycobacterial infections. It provides a histological diagnosis that can completely alter the treatment plan from antibiotics to steroids or other therapies.
Following debridement or drainage of large abscesses, Negative Pressure Wound Therapy (NPWT), often known as a wound vac, may be applied. This device consists of a foam dressing connected to a vacuum pump that applies continuous suction to the wound bed.
NPWT promotes healing by removing excess fluid, reducing bacterial load, and stimulating blood flow to the area. It also physically draws the wound edges together. This procedure accelerates granulation tissue formation, preparing the wound for final closure or grafting.
If a large area of skin is lost due to necrosis or surgical debridement, a skin graft may be necessary to close the wound. This involves harvesting a thin layer of healthy skin from a donor site (usually the thigh) and transplanting it to the clean wound bed.
This reconstructive procedure restores the skin barrier, preventing fluid loss and further infection. It is typically performed once the active cellulitis has resolved and the wound bed is healthy and vascularized enough to support the graft.
While not surgical, strict limb elevation is a fundamental therapeutic procedure in managing cellulitis. The affected limb must be elevated above the level of the heart. This mechanical action uses gravity to drain the edema fluid away from the infection site.
Reducing edema improves local microcirculation, allowing immune cells and antibiotics to reach the infection more effectively. Hospitals often use specialized ramps or slings to maintain this position continuously, thereby significantly accelerating clinical improvement.
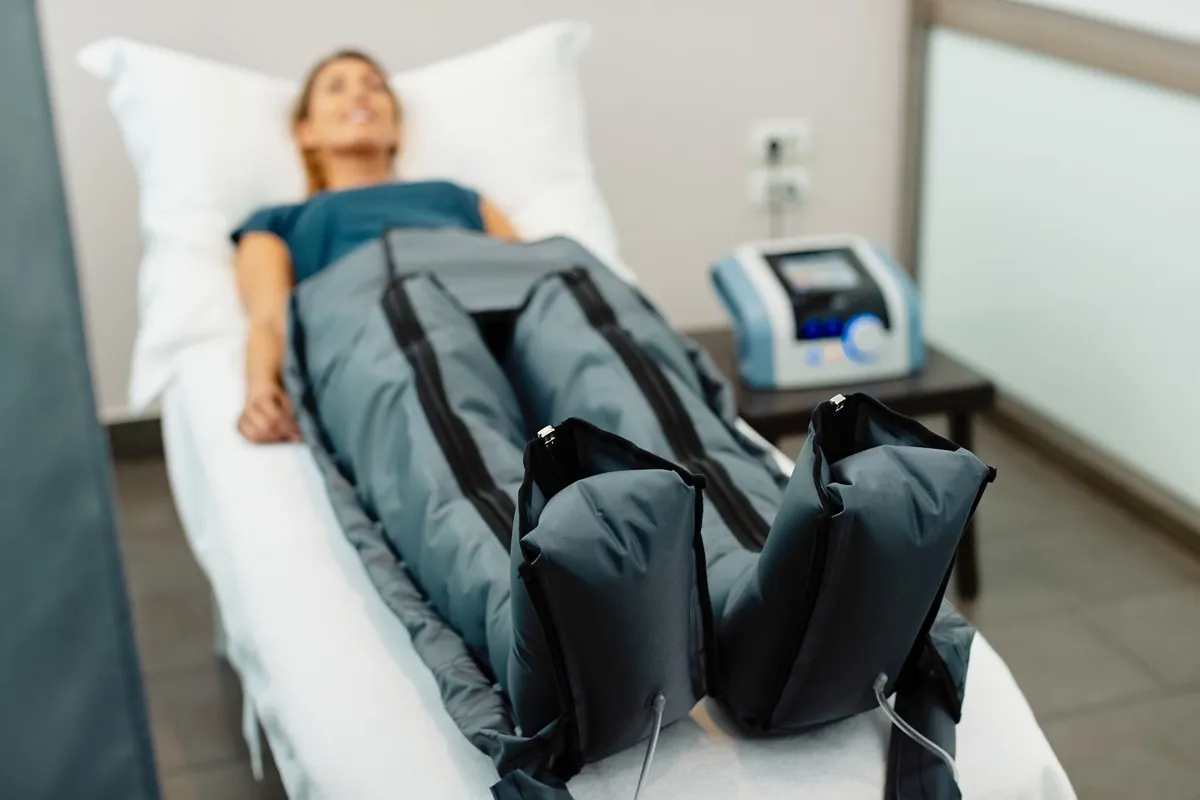
Once the acute infection has begun to subside, initiating compression therapy is a standard procedure to prevent recurrence. This involves measuring and fitting the patient with medical-grade compression stockings or wraps.
This mechanical support prevents the accumulation of lymphatic fluid, which is a breeding ground for bacteria. Proper fitting is a procedural skill that ensures the pressure is therapeutic without compromising arterial blood flow. It is a long-term maintenance strategy started in the clinical setting.

Send us all your questions or requests, and our expert team will assist you.
The doctor uses a local anesthetic to numb the skin before the incision. However, because the tissue is inflamed and acidic due to the infection, the numbing medicine might not work as perfectly as usual. You may feel some pressure or sharp sensations, but the relief from the pressure release is usually immediate.
A CT scan helps doctors see what is happening under the skin. It checks for deep pockets of pus (abscesses) that need draining or gas bubbles that indicate a flesh-eating infection. It ensures that surgery isn’t required and that antibiotics are the right choice.
A PICC (Peripherally Inserted Central Catheter) is a long, thin tube inserted into a vein in your arm that goes up to the large veins near your heart. It is used when you need antibiotics for several weeks. It saves you from getting poked with a needle every few days for a new IV.
Yes, skin grafting leaves two scars: one at the donor site (where the skin was taken) and one at the recipient site (where it was placed). The donor site usually looks like a bad sunburn that heals over time, while the grafted area may have a different texture or color than the surrounding skin.
You should keep the affected limb elevated as much as possible, ideally 23 hours a day during the acute phase. Even a brief trip to the bathroom can cause it to throb and swell. Strict elevation speeds up healing dramatically.



Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)