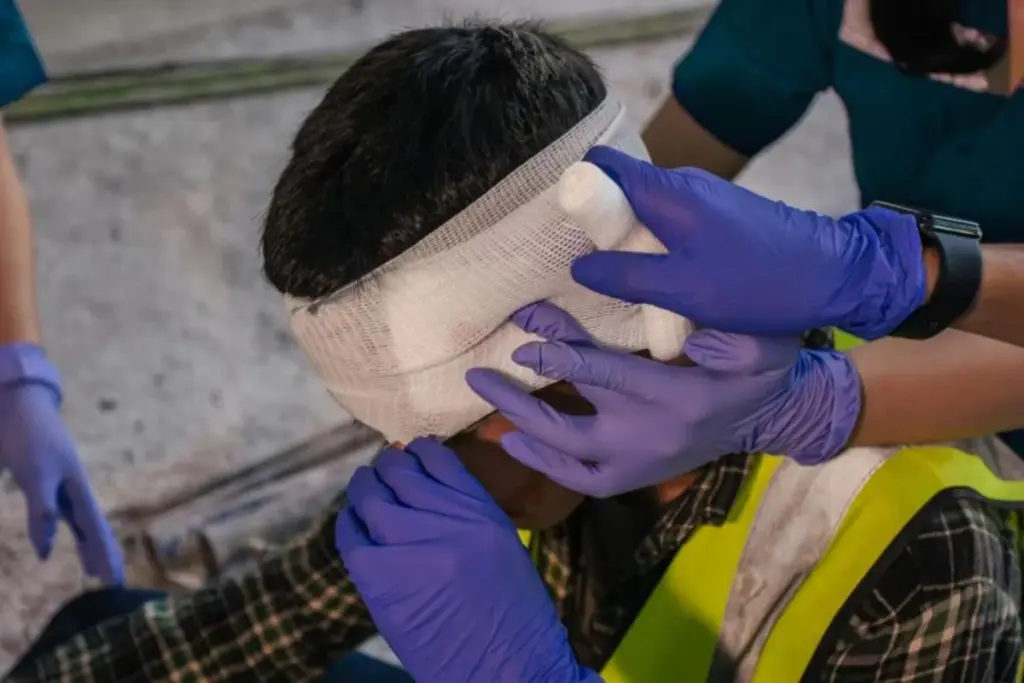
Traumatic brain injuries (TBI) affect millions worldwide, causing significant clinical concerns. It’s estimated that over 1.7 million people in the United States suffer from TBI annually. Many experience lasting impacts on their quality of life.
TBI can lead to a wide range of symptoms. These include physical disabilities, cognitive, and emotional challenges. The progressive nature of TBI is a growing concern. Research shows that long-term effects can be severe and debilitating.
Understanding whether TBI worsens over time is key. It’s important for developing effective treatment plans. It also helps in providing complete care to those affected.
Key Takeaways
- Traumatic brain injuries have significant long-term consequences.
- TBI can lead to a wide range of physical, cognitive, and emotional symptoms.
- The progressive nature of TBI is a growing clinical concern.
- Effective treatment plans require understanding the long-term effects of TBI.
- Comprehensive care is essential for individuals affected by TBI.
Understanding Traumatic Brain Injuries (TBIs)

Traumatic Brain Injuries are a major cause of illness and death. We need to understand their definition, types, causes, and how they are diagnosed. This will help us grasp this complex condition better.
Definition and Classification of TBIs
A Traumatic Brain Injury (TBI) happens when the brain changes function due to an outside force. This can range from mild concussions to severe brain damage. TBIs are divided into three levels: mild, moderate, and severe.
The Glasgow Coma Scale helps measure how conscious a person is. It scores from 3 (deep unconsciousness) to 15. This scale is used to assess the injury’s severity.
Common Causes of Traumatic Brain Injuries
TBIs can come from falls, motor vehicle accidents, sports injuries, and violence. Falls are the top reason, mainly for the elderly and young kids. Car accidents can cause severe injuries. Sports, like football and hockey, also lead to TBIs.
- Falls
- Motor vehicle accidents
- Sports injuries
- Violence
Initial Diagnosis and Assessment
Diagnosing a TBI starts with a detailed check-up. This includes a physical exam, brain tests, and scans like CT scans or MRI. The Glasgow Coma Scale helps measure injury severity. More tests might check memory and focus.
Knowing how TBIs are caused and diagnosed is key. It helps doctors give the right care. Spotting signs early can lead to better recovery.
The Immediate vs. Long-Term Effects of TBIs
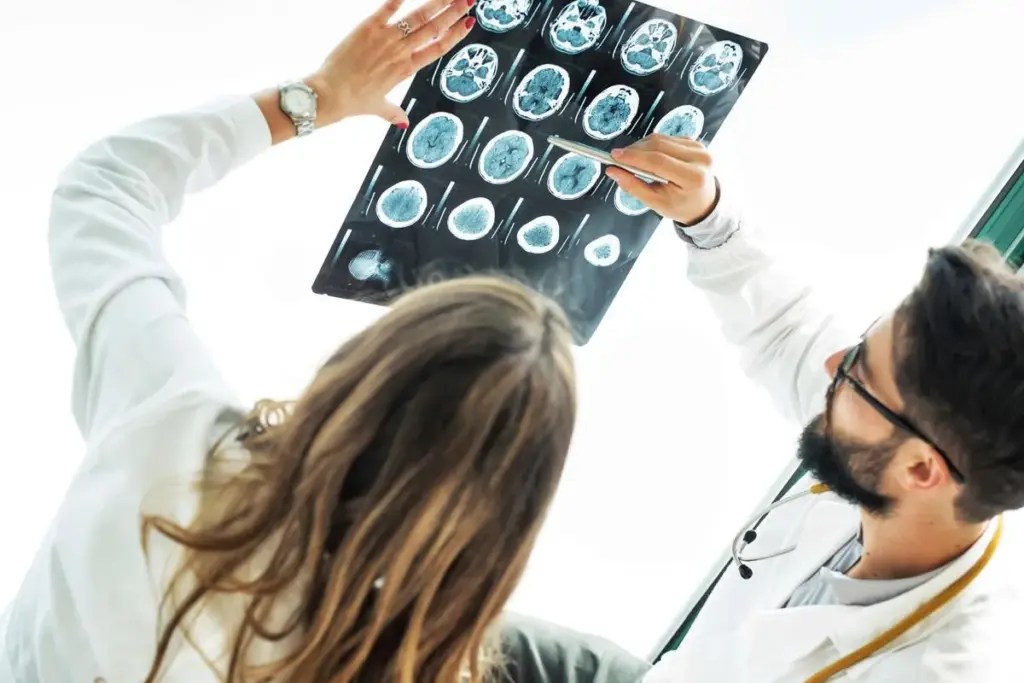
It’s important to know the effects of a TBI, from the start to long after. When someone gets a TBI, it’s tough for them and their loved ones.
Acute Symptoms and Complications
Right after a TBI, people might lose consciousness, feel confused, or have trouble speaking. These signs are the body’s first reaction to the injury. Some might also have seizures or other brain problems soon after.
Acute care for TBI focuses on keeping the patient stable, managing symptoms, and avoiding more harm. This early stage is very important and needs constant doctor attention.
The Recovery Timeline
How long it takes to recover from a TBI varies a lot. Some people get better fast, while others take longer. The recovery process depends on the injury’s severity, the person’s health, and the treatment.
Most people see big improvements in the first few months. But, some might keep getting better over time.
Transition from Acute to Chronic Effects
As the first signs of TBI go away, some people start to face chronic effects. These can include changes in thinking, feelings, and behavior. This change is a big step in the challenges they face.
Dealing with these chronic effects needs a team effort. This includes medical help, therapy, and support services. Knowing about long-term effects helps in giving the right care and support.
The Progressive Nature of Brain Injuries
It’s important to understand how brain injuries progress over time. Traumatic brain injuries (TBIs) can start a chain of changes that get worse. These changes can affect a person’s life long after the injury.
Neurodegeneration Following TBI
Neurodegeneration after TBI is a big worry. It can make brain function get worse over time. Studies show that TBI can start neurodegenerative processes. This might lead to conditions like chronic traumatic encephalopathy (CTE).
Key factors contributing to neurodegeneration include:
- Inflammation and oxidative stress
- Accumulation of toxic proteins
- Disruption of normal brain function
Secondary Injury Mechanisms
Secondary injury mechanisms are key in TBI progression. They can cause more damage after the initial injury. This makes recovery harder.
|
Mechanism |
Description |
Impact |
|---|---|---|
|
Excitotoxicity |
Overactivation of glutamate receptors |
Neuronal damage and death |
|
Oxidative Stress |
Imbalance between free radicals and antioxidants |
Cellular damage and inflammation |
|
Inflammation |
Activation of immune cells and release of cytokines |
Tissue damage and edema |
Brain Injury Causing Tissue Destruction Resulting in Permanent Damage
Brain tissue damage from TBI can cause permanent harm. This harm can affect a person’s thinking, feelings, and physical health. The damage’s extent depends on the injury’s severity and the treatment’s success.
Knowing these factors helps in creating better treatments. These treatments aim to reduce long-term damage and improve patient results.
Can You Die From a Head Injury Years Later?
It’s important to know the risks of traumatic brain injuries (TBIs) years later. TBIs can cause many complications, and the risk of death is a big concern.
Delayed Mortality Risk After TBI
Studies show that people with TBIs face a higher risk of death years later. Age, health, and injury severity affect survival chances.
Several factors influence the risk of dying later, including:
- The severity of the initial injury
- The presence of comorbid health conditions
- The age of the individual at the time of injury
Research on Long-Term Survival Rates
Research aims to understand survival rates for TBI patients. It helps identify patterns and risk factors for delayed mortality.
|
Study |
Sample Size |
Follow-Up Period |
Key Findings |
|---|---|---|---|
|
Study A |
1000 |
5 years |
Increased mortality risk in the first 2 years post-injury |
|
Study B |
500 |
10 years |
Long-term cognitive decline associated with increased mortality |
Case Studies of Delayed Fatal Outcomes
Case studies show the risk of fatal outcomes years after TBIs. They highlight the need for ongoing care for head injury patients.
A documented case showed a patient died years after a severe TBI. This case stresses the importance of ongoing medical care.
While not all TBIs lead to death years later, understanding the risks is key. Taking proactive steps can improve outcomes for those with head injuries.
Encephalomalacia and Progressive Brain Damage
Encephalomalacia is a serious condition where brain tissue softens or deteriorates. It often results from traumatic brain injuries (TBIs) or cerebral infarction. The loss of brain tissue can cause various neurological deficits, depending on the damage’s location and extent.
What is Encephalomalacia?
Encephalomalacia is when brain tissue softens or is lost. This usually happens due to traumatic brain injuries or a lack of blood to the brain. It can take different forms, like cystic encephalomalacia, where brain tissue is replaced by cysts.
The causes of encephalomalacia vary, but often involve significant brain injury or disease. Knowing the cause is key to managing the condition well.
Does Encephalomalacia Get Worse Over Time?
The progression of encephalomalacia can differ greatly among people. In some, it may stop worsening after the initial injury. But in others, it can get worse.
Several factors can affect how it progresses. These include the severity of the initial injury, secondary brain injuries, and the success of management strategies.
|
Factors Influencing Progression |
Description |
Impact on Progression |
|---|---|---|
|
Severity of Initial Injury |
The extent of the initial brain damage. |
Higher severity often correlates with worse prognosis. |
|
Secondary Brain Injuries |
Additional injuries occurring after the initial trauma. |
Can exacerbate the condition and lead to further deterioration. |
|
Management Strategies |
Medical and rehabilitative interventions. |
Effective management can slow or halt progression. |
Managing Progressive Brain Softening
Managing encephalomalacia requires a multi-faceted approach. This includes medical treatment, rehabilitation, and lifestyle changes. The aim is to slow the condition’s progression and improve life quality for those affected.
Rehabilitation Strategies might include physical, occupational, and speech therapy. These are tailored to meet each person’s needs.
Monitoring and adjusting treatment plans is essential for the best management.
Life Expectancy After Brain Injuries
Traumatic brain injuries can greatly affect how long someone lives. It’s important to study this to help TBI patients. Knowing what affects survival rates is key to better care.
Statistical Data on Longevity Post-TBI
Studies show TBI can shorten life expectancy. People with severe TBI might live less than others.
|
Severity of TBI |
Average Life Expectancy Reduction |
|---|---|
|
Mild TBI |
1-2 years |
|
Moderate TBI |
2-5 years |
|
Severe TBI |
5-10 years |
The table shows life expectancy can be reduced by 1-10 years, depending on TBI severity. But, these are just averages. Outcomes can differ for each person.
Life Expectancy After Anoxic Brain Injury
Anoxic brain injuries have a tough prognosis. Life expectancy depends on how long the brain lacked oxygen and the damage.
Anoxia duration is very important. Longer without oxygen means more damage and a worse outlook.
Factors That Influence Survival Rates
Many things affect survival after TBI. These include injury severity, age, and other health issues. Good management and rehab can also help.
- Age: Older people often face tougher challenges due to less health reserve and other conditions.
- Injury Severity: Severe injuries lead to higher death rates and shorter lives.
- Comorbidities: Other health problems can make recovery harder and affect survival.
Healthcare providers need to understand these factors. This helps them give better care and support. It can improve survival chances and quality of life for TBI patients.
Long-Term Physical Effects of Traumatic Brain Injury
It’s important to know the long-term physical effects of TBI to help those affected. Traumatic brain injuries can lead to many physical challenges that last a lifetime.
Persistent Motor and Sensory Impairments
One big effect of TBI is lasting motor and sensory problems. These can make it hard to move around and balance. They can also make everyday sounds or lights feel too intense.
These motor issues can make daily tasks tough. People might need ongoing physical therapy to stay functional. Sensory problems can change how someone interacts with their world, needing special ways to cope.
Headaches and Chronic Pain
Many TBI survivors deal with headaches and chronic pain. These issues can really lower their quality of life. Finding good ways to manage pain is key.
Chronic pain is hard to handle and might need a team effort. This could include medicine, physical therapy, and even things like acupuncture or therapy to change how you think about pain.
Sleep Disturbances and Fatigue
People with TBI often have trouble sleeping and feel very tired. These problems can make other physical and mental challenges worse.
Fixing sleep issues might mean setting a regular sleep schedule and possibly medical help. Fighting fatigue is also critical. It helps people do daily tasks and join in on rehabilitation programs.
The lasting physical effects of TBI are complex and varied. Understanding these effects helps healthcare providers create better care plans. This can improve the lives of TBI survivors.
|
Physical Effect |
Description |
Potential Interventions |
|---|---|---|
|
Motor Impairments |
Difficulties with coordination, balance, and movement |
Physical therapy, occupational therapy |
|
Sensory Impairments |
Heightened sensitivity to light or sound |
Sensory integration therapy, protective gear |
|
Chronic Pain |
Ongoing pain that can impact daily activities |
Pain management clinics, medication, alternative therapies |
|
Sleep Disturbances |
Insomnia, excessive sleepiness |
Behavioral therapy, sleep regulation medication |
Cognitive Decline Following Severe Craniocerebral Injury
Severe craniocerebral injuries can cause big changes in how we think and act. These changes can affect our daily lives and how happy we are. We’ll look at how these injuries can harm our minds and what it means for people.
Memory and Attention Problems
People with severe brain injuries often have trouble remembering things. This can be anything from forgetting where they put things to not being able to learn new stuff. They might also have trouble focusing or switching between tasks.
Executive Function Impairment
Executive function is about making plans, making decisions, and solving problems. Those with severe TBI might find it hard to organize, manage time, or control their impulses.
Processing Speed and Learning Difficulties
Processing speed and learning can also be tough. It might take longer to think or learn new things. This makes it hard to do tasks that need quick thinking.
To get a clearer picture of what happens after a severe brain injury, here’s a summary table:
|
Cognitive Domain |
Common Issues |
Impact on Daily Life |
|---|---|---|
|
Memory |
Forgetfulness, difficulty forming new memories |
Forgetting appointments, tasks, or important information |
|
Attention |
Trouble focusing, sustaining attention |
Difficulty completing tasks, following conversations |
|
Executive Function |
Planning, decision-making, problem-solving challenges |
Struggling with organization, time management, impulse control |
|
Processing Speed |
Slowing of cognitive processing |
Difficulty learning new information, performing tasks quickly |
Emotional and Behavioral Changes Over Time
TBI can lead to many emotional and behavioral changes. It’s important to understand and tackle these issues fully. These changes can affect not just the person but also their family and friends.
Mood Disorders and Emotional Regulation
Mood disorders like depression and anxiety are common after TBI. This is because the injury can harm brain areas that control emotions. Treatment often involves medicine and therapy.
A study in the Journal of Neurotrauma showed TBI survivors are more likely to have mood disorders. This is true compared to the general population.
“The presence of mood disorders post-TBI is a significant concern, necessitating early identification and intervention to mitigate long-term effects.”
Personality Changes
Personality changes after TBI can be hard for everyone involved. These changes might include acting impulsively, feeling less motivated, or lacking empathy. Knowing what causes these changes is key to finding the right help.
- Impulsivity can lead to reckless decisions or actions.
- Apathy may result in a lack of motivation or interest in activities.
- Reduced empathy can strain personal relationships.
Social Functioning Challenges
TBI can make it hard to socialize, work, or enjoy activities. Programs that teach social skills can help with these issues.
|
Challenge |
Description |
Potential Intervention |
|---|---|---|
|
Social Isolation |
Difficulty maintaining social connections. |
Social skills training, support groups. |
|
Employment Issues |
Challenges in maintaining employment due to cognitive or behavioral changes. |
Vocational rehabilitation, workplace accommodations. |
Dealing with emotional and behavioral changes after TBI needs a wide approach. This includes medical care, therapy, and support for the person and their family.
Neurodegenerative Diseases Linked to TBI
Traumatic Brain Injuries (TBIs) are linked to many neurodegenerative diseases. Studies show TBIs can cause long-term brain damage. We’ll look at how TBIs might lead to Chronic Traumatic Encephalopathy (CTE), Alzheimer’s disease, and Parkinson’s disease.
Chronic Traumatic Encephalopathy (CTE)
CTE is a brain disorder caused by repeated head injuries, common in athletes. Symptoms include memory loss, confusion, and depression. It’s not just athletes who are at risk, but anyone who has had repeated head trauma.
CTE is diagnosed after death by examining the brain. It’s caused by tau protein buildup. Learning about CTE helps us find ways to prevent and treat it.
Alzheimer’s Disease and TBI Connection
Research shows a link between TBI and Alzheimer’s disease. Alzheimer’s is marked by amyloid-beta plaques and tau tangles in the brain. People with TBI are more likely to get Alzheimer’s, if the injury was severe.
We’re trying to understand how TBI leads to Alzheimer’s. It’s thought that TBI starts a chain of events that can cause Alzheimer’s symptoms.
Parkinson’s Disease Risk After Head Trauma
Parkinson’s disease is also linked to TBI. It causes tremors, stiffness, and movement problems. Head injuries may raise the risk of Parkinson’s, but we don’t know how.
- Key findings include:
- The impact of TBI on starting or speeding up neurodegenerative diseases.
- The need to watch people with TBI over time.
- More research is needed to fully understand the TBI and neurodegenerative disease link.
It’s important to understand how TBI affects neurodegenerative diseases. This knowledge helps us prevent and treat these conditions. As we learn more, we can better help those with TBI and reduce long-term risks.
Monitoring and Managing Progressive TBI Symptoms
It’s key to watch and manage TBI symptoms to better life quality for those with traumatic brain injuries. A good plan includes regular doctor visits, knowing when things get worse, and acting fast.
Regular Medical Assessment Protocols
Regular doctor visits are a must to track TBI symptoms and catch problems early. These visits include doctor checks, scans, and tests of brain function. It’s best for TBI patients to stick to a plan made just for them.
How often and what these visits include can change based on the injury and health. A common plan might include:
- Doctor checks to see how the brain is doing and if symptoms are getting worse.
- Scans like MRI or CT to see if the brain is changing.
- Tests to check how well the brain is working, including thinking, feelings, and behavior.
Warning Signs of Worsening Condition
People with TBI and their helpers need to know the signs that things might be getting worse. Look out for more confusion, trouble speaking or swallowing, big mood swings, or losing physical skills. Spotting these signs early can lead to quick help.
Some key signs to watch for are:
|
Symptom Category |
Warning Signs |
|---|---|
|
Cognitive Decline |
More confusion, memory loss, trouble solving problems. |
|
Emotional and Behavioral Changes |
Big mood swings, being irritable, feeling sad or anxious. |
|
Physical Symptoms |
Headaches, feeling dizzy, seizures, or trouble with balance and coordination. |
Intervention Strategies for Emerging Problems
When new problems show up, there are many ways to help. This can include medicines, therapy, and changes in daily life. The aim is to lessen TBI symptoms and make life better.
Some ways to help include:
- Medicines for things like seizures, depression, or anxiety.
- Therapy to boost memory, attention, and planning skills.
- Physical therapy to improve movement, strength, and balance.
- Changes in diet, exercise, and sleep to help overall health.
By being proactive and taking a full approach to TBI symptoms, we can greatly improve life for those with traumatic brain injuries.
Treatment Approaches for Long-Term TBI Management
Managing TBI long-term needs a detailed plan. This plan includes medical care, rehabilitation, and ongoing support. It’s made to fit each person’s needs.
Pharmacological Interventions
Medications are key in managing TBI symptoms. They help with depression, anxiety, and sleep problems. For example, SSRIs treat depression, and anticonvulsants manage seizures.
It’s important to watch how these medicines work. Doctors need to check for side effects and adjust treatments as needed.
Cognitive and Physical Rehabilitation
Cognitive rehabilitation helps improve memory and attention. It uses training and tools to help people be more independent.
Physical rehabilitation works on getting people moving again. It includes physical, occupational, and speech therapy. The goal is to help with daily tasks and improve life quality.
Emerging Therapies and Research
New treatments for TBI are being researched. This includes stem cell therapy and neurostimulation. These new methods show promise but need more study.
As we learn more about TBI, our treatments must keep up. Adding new therapies to care plans can help people recover better.
Conclusion
It’s key to understand the long-term effects of traumatic brain injuries (TBI) to help those affected. We’ve looked at how TBI impacts people, from the first effects to long-term issues. These include problems with thinking, mood changes, and a higher risk of diseases like Alzheimer’s.
Handling TBI needs a team effort. This includes regular doctor visits, strategies for new challenges, and ongoing support. By recognizing TBI’s long-term effects and managing them, we can make life better for those with TBI.
As we learn more about TBI, we must keep researching and supporting those affected. This way, we can offer top-notch care and support. It’s all about improving their health and happiness.
FAQ
What are the long-term effects of traumatic brain injuries?
Traumatic brain injuries can cause lasting problems. These include motor and sensory issues, headaches, and chronic pain. Sleep troubles and fatigue are also common.
Cognitive decline is another issue. This includes memory and attention problems. Mood disorders and social challenges are also seen.
Can traumatic brain injuries worsen over time?
Yes, they can. Secondary injury mechanisms and neurodegeneration can cause further damage. Encephalomalacia, a softening of brain tissue, can also worsen over time.
Does encephalomalacia get worse over time?
Yes, it can. Encephalomalacia can lead to more brain damage. Medical treatment is key to slow its progression.
Can you die from a head injury years later?
Yes, it’s possible. Head injuries can increase the risk of long-term complications. This includes neurodegenerative diseases like Alzheimer’s and Parkinson’s.
What is the life expectancy after anoxic brain injury?
Life expectancy varies. It depends on injury severity and individual factors. Survival rates can be influenced by brain damage extent and medical care quality.
What are the treatment approaches for long-term TBI management?
Treatment includes pharmacological interventions and rehabilitation. Cognitive and physical therapy are also used. A multidisciplinary care plan is essential.
How can progressive TBI symptoms be monitored and managed?
Regular medical checks and early intervention are key. Warning signs and treatment strategies help manage symptoms. Early action can reduce long-term effects.
Is there a link between TBI and neurodegenerative diseases?
Yes, research shows a link. TBI can increase the risk of diseases like CTE, Alzheimer’s, and Parkinson’s.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC4677116/


































