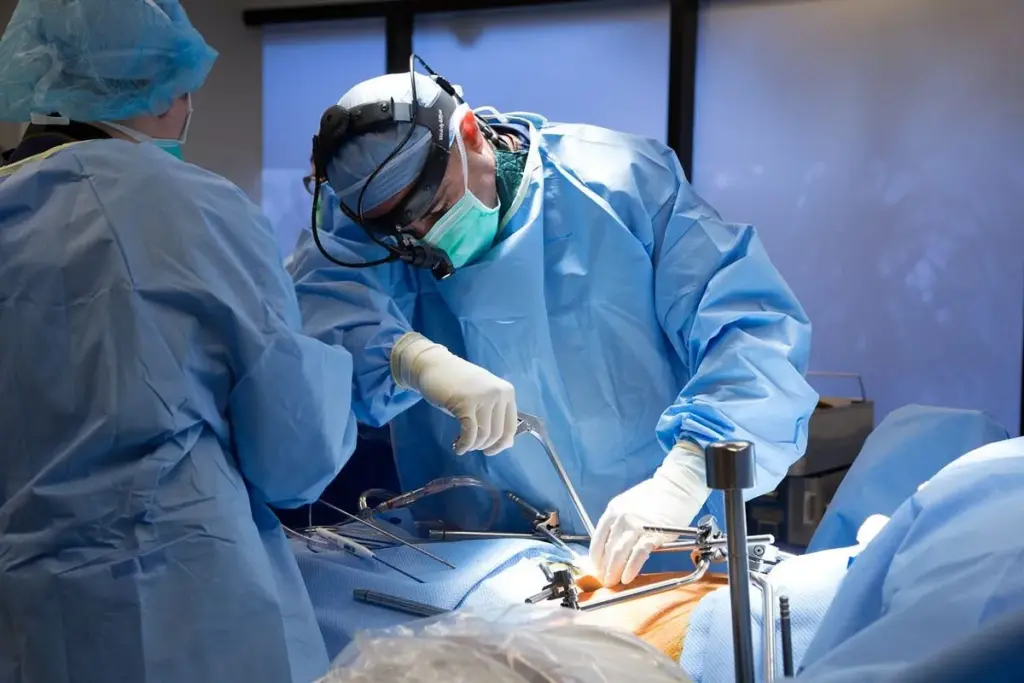
Did you know that patients having minimally invasive spine surgery often stay in the hospital less than those with open surgery? This shows how MIS can lead to quicker recovery times. It’s a great choice for many.
When we talk about Medicare coverage for MIS, knowing the age limit for spinal surgery is key. We’ll look into what Medicare pays for and what to expect with spinal surgery.
Key Takeaways
- Understanding Medicare coverage for minimally invasive spine surgery.
- The importance of age considerations for spinal surgery.
- Benefits of minimally invasive spine surgery.
- What to expect from Medicare coverage for spinal procedures.
- Factors influencing Medicare coverage decisions.
Understanding Minimally Invasive Spine Surgery
Minimally invasive spine surgery is a new way to treat spinal problems. It’s less invasive than traditional surgery. We’ll look at what makes it different, its benefits, and how it stacks up against old methods.
Definition and Basic Concepts
This surgery uses new tech and methods to make small cuts. It causes less damage and helps you heal faster. It’s made to disturb your body less, cutting down on pain and speeding up recovery.
Key aspects of minimally invasive spine surgery include:
- Smaller incisions, reducing tissue trauma
- Less blood loss during surgery
- Reduced risk of infection
- Shorter hospital stays
- Faster recovery and return to normal activities
Comparison to Traditional Open Spine Surgery
Traditional surgery needs a bigger cut for better access. It works well but can hurt more, cause more bleeding, and take longer to get better.
|
Aspect |
Minimally Invasive Spine Surgery |
Traditional Open Spine Surgery |
|---|---|---|
|
Incision Size |
Smaller (typically 1-2 cm) |
Larger (often 5-10 cm or more) |
|
Tissue Damage |
Less damage due to smaller incisions |
More extensive damage due to larger incisions |
|
Recovery Time |
Faster recovery, often within weeks |
Longer recovery, potentially several months |
Knowing the differences helps patients choose better. We’ll dive into Medicare coverage for these surgeries next.
Medicare Coverage Basics for Surgical Procedures
Understanding Medicare coverage for surgeries is key. Medicare has different parts, each covering various healthcare needs. This includes surgeries.
Medicare Parts and Their Coverage Scope
Medicare Part A and Part B mainly cover surgeries. Medicare Part A pays for inpatient care, like hospital stays and skilled nursing. It also covers some home health care.
Medicare Part B covers outpatient services. This includes doctor visits and some surgeries done outside the hospital. It also pays for physical therapy and certain medical equipment.
|
Medicare Part |
Coverage Scope |
|---|---|
|
Medicare Part A |
Inpatient hospital stays, skilled nursing facility care, some home health care |
|
Medicare Part B |
Outpatient services, doctor visits, diagnostic tests, outpatient surgeries |
General Requirements for Surgical Coverage
For Medicare to cover surgeries, some rules must be followed. The surgery must be medically necessary. This means it’s needed to diagnose or treat a health issue.
The surgery also needs to be done by a Medicare-approved provider. This includes hospitals, surgical centers, and certain healthcare professionals.
Knowing these basics helps patients understand Medicare’s coverage for surgeries better.
Age Limit for Spinal Surgery: Facts and Considerations
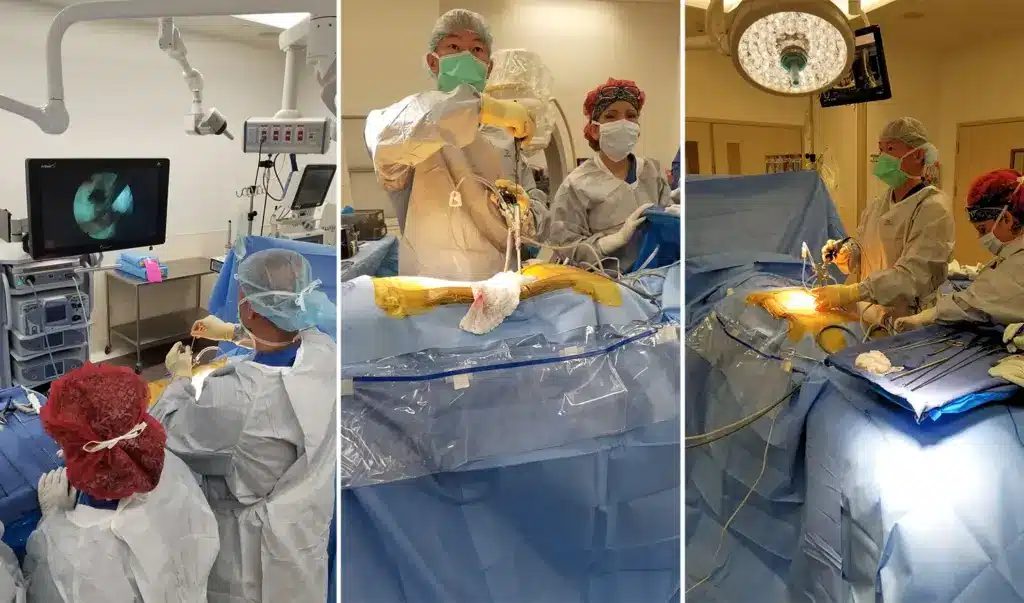
Age is a big factor in deciding if someone needs spinal surgery. As we get older, our bodies change. These changes can make surgery more complicated and risky.
Is There a Maximum Age for Spine Surgery?
Whether there’s a maximum age for spine surgery is not simple. It depends on the patient’s health, any other health issues, and the type of surgery needed.
Age is important, but it’s not the only thing. Many older people have successful surgeries. This is thanks to better surgery methods and care after surgery.
How Age Affects Surgical Decisions and Outcomes
Age can affect if someone gets surgery and how well it goes. Older people might face more risks. This is because they might not be as strong, have other health issues, and could have problems with anesthesia.
|
Age Factor |
Impact on Surgery |
Considerations |
|---|---|---|
|
Physical Condition |
Older patients may have reduced physical reserve. |
Preoperative assessment is critical. |
|
Comorbidities |
Presence of other health conditions can increase surgical risks. |
Managing comorbidities is key to successful outcomes. |
|
Recovery Time |
Older patients may require longer recovery times. |
Postoperative care and rehabilitation are vital. |
Even with these challenges, many older adults have good results from spinal surgery. The choice to have surgery depends on many things. These include the person’s health, how bad their spinal problem is, and what they want.
Medicare Coverage Criteria for Minimally Invasive Spine Surgery
To get Medicare to cover minimally invasive spine surgery, it must meet certain criteria. We will look at these requirements and how to get coverage.
Medical Necessity Requirements
Medicare says the surgery must be medically necessary. This means it’s a needed treatment for the patient’s condition. This decision is based on the patient’s medical history, symptoms, and test results.
Each case is judged on its own, considering how severe the condition is and if the surgery will help. We need to document the patient’s condition well. This includes any treatments they’ve tried before.
Prior Authorization and Documentation Needs
Before Medicare will cover the surgery, they often need prior authorization. This means asking Medicare for approval before doing the surgery.
To get approval, doctors must send in detailed information. This includes the patient’s medical records, test results, and why the surgery is needed. Here’s what’s usually needed:
|
Documentation Type |
Description |
Importance |
|---|---|---|
|
Medical Records |
Detailed patient history and previous treatments |
High |
|
Diagnostic Test Results |
Results of imaging studies (e.g., MRI, CT scans) |
High |
|
Physician’s Letter |
Justification for the procedure and expected outcomes |
High |
It’s important to send in all the needed documents correctly and on time. This helps with a successful request for prior authorization.
Types of Minimally Invasive Spine Procedures Covered by Medicare
We will look at the types of minimally invasive spine procedures Medicare covers. These include decompression and spinal fusion. They help reduce back pain and improve life quality.
Decompression Procedures
Decompression procedures are a type of surgery that relieve pressure on the spinal cord or nerves. They are used for conditions like spinal stenosis, herniated discs, and degenerative disc disease.
Common Decompression Procedures:
- Laminectomy: A procedure that involves removing a portion of the vertebra to relieve pressure on the spinal cord or nerves.
- Discectomy: A procedure that involves removing a herniated or damaged disc to relieve pressure on the spinal cord or nerves.
- Foraminotomy: A procedure that involves enlarging the opening through which the nerve roots exit the spinal canal.
Minimally Invasive Spinal Fusion
Minimally invasive spinal fusion is a surgery that fuses two or more vertebrae together. This stabilizes the spine and relieves pain. It’s used for conditions like degenerative disc disease, scoliosis, and spondylolisthesis.
|
Procedure |
Description |
Benefits |
|---|---|---|
|
Minimally Invasive Transforaminal Lumbar Interbody Fusion (TLIF) |
A procedure that involves fusing the vertebrae through a small incision. |
Less tissue damage, reduced blood loss, and faster recovery. |
|
Minimally Invasive Posterior Lumbar Interbody Fusion (PLIF) |
A procedure that involves fusing the vertebrae through a small incision in the back. |
Reduced risk of nerve damage, less postoperative pain. |
Knowing about the minimally invasive spine procedures Medicare covers helps patients make better choices. They can understand their treatment options better.
Who Is a Candidate for Minimally Invasive Spine Surgery?
To find out if someone is right for minimally invasive spine surgery, we do a detailed check-up. We look at many things to see if the surgery is a good fit.
Medical Conditions That Qualify
Some spinal problems might make someone a good candidate for this surgery. These include:
- Herniated discs
- Spinal stenosis
- Spondylolisthesis
- Degenerative disc disease
People with these issues might do well with minimally invasive surgery. It can heal faster and cause less damage than regular surgery.
|
Condition |
Description |
Minimally Invasive Treatment Option |
|---|---|---|
|
Herniated Disc |
A condition where the disc material bulges out, pressing on nerves. |
Discectomy |
|
Spinal Stenosis |
Narrowing of the spinal canal, causing nerve compression. |
Laminectomy or decompression |
|
Spondylolisthesis |
A vertebra slips out of place, potentially compressing nerves. |
Spinal fusion or stabilization |
Evaluation Process and Criteria
We check a patient’s medical history, do a physical exam, and look at scans like MRI or CT. We see how bad the problem is, the patient’s health, and what treatments they’ve tried before.
A spine specialist says, “A detailed check is key to picking the best surgery for each patient.”
“The key to successful minimally invasive spine surgery lies in careful patient selection and a tailored treatment plan.”
Our criteria include:
- The severity of symptoms and their impact on quality of life
- Previous conservative treatments and their effectiveness
- Anatomical considerations that may affect the surgical approach
By looking at these things, we can decide if someone is a good fit for minimally invasive spine surgery. Then, we create a treatment plan that works.
Cost of Minimally Invasive Spine Surgery with Medicare
Minimally invasive spine surgery costs can change. Medicare helps us understand these costs. It’s key to know how Medicare covers these expenses.
Medicare Part A and B Coverage Percentages
Medicare Part A and Part B cover different medical services. For spine surgery, both parts might apply. Part A covers hospital stays, and Part B covers doctor visits and some procedures.
Medicare Part B usually covers 80% of approved costs after the deductible. The other 20% is often covered by extra insurance or paid by the patient.
|
Medicare Component |
Coverage Percentage |
Typical Coverage |
|---|---|---|
|
Medicare Part A |
Varies |
Inpatient hospital stays |
|
Medicare Part B |
80% after deductible |
Outpatient services, doctor visits |
Out-of-Pocket Expenses and Supplemental Insurance
Even with Medicare, patients face some costs for spine surgery. These include deductibles, copayments, and coinsurance.
Supplemental insurance, like Medigap, can help with these costs. Some Medigap plans cover the 20% coinsurance for Part B services, including surgeries.
“Understanding your Medicare coverage and any supplemental insurance you may have is key to managing costs for minimally invasive spine surgery,” a Medicare spokesperson advises.
Patients should talk to their healthcare provider and financial advisors. This helps understand their financial responsibilities fully.
Knowing Medicare’s coverage and possible out-of-pocket costs helps patients manage the financial side of minimally invasive spine surgery.
Minimally Invasive Spine Surgery Success Rates and Recovery
Minimally invasive spine surgery is popular for its high success rates and quick recovery times. It’s a great choice for many patients. We’ll look at the success rates and recovery times for patients with Medicare coverage.
Statistical Outcomes and Success Factors
Studies show that minimally invasive spine surgery works well for many patients. Success depends on the procedure, patient, and surgeon. Patients often see big improvements in pain and function.
Key factors for success include:
- Choosing the right patient for the surgery
- Having a skilled surgeon
- Using new imaging and navigation tools
- Following proven surgical methods
A study in a top spine journal found a 90% patient satisfaction rate with this surgery. Patients saw less pain and disability. This shows the surgery’s benefits.
Typical Recovery Timeline with Medicare Coverage
The recovery time for this surgery varies. But, patients usually have shorter hospital stays and get back to normal faster. Medicare helps a lot during recovery.
The recovery has several stages:
- Right after surgery (0-2 weeks): Focus on pain and healing
- Early recovery (2-6 weeks): Slowly start moving more
- Intermediate recovery (6-12 weeks): Get stronger and do more exercises
- Late recovery (3-6 months): Get back to normal fully
Medicare covers follow-up care and physical therapy. It’s key for patients to work with their doctors on a recovery plan.
“Quickly getting back to normal is a big plus of minimally invasive spine surgery. With the right care, many patients see great results and live better lives.”
Knowing about success rates and recovery times helps patients with Medicare make smart choices. They can prepare for a successful surgery.
Specific Procedures: Does Medicare Cover the Minuteman Procedure?
Medicare’s coverage for spinal procedures can be tricky, like with the Minuteman procedure. We’ll first look at what the Minuteman procedure is. Then, we’ll see if Medicare covers it.
Understanding the Minuteman Procedure
The Minuteman procedure is a new way to fix the spine. It’s less invasive than old methods. It’s for people with certain spine problems, like worn-out discs or slipped vertebrae.
Key Features of the Minuteman Procedure:
- It’s a minimally invasive method, which means less damage and quicker healing.
- It uses a special implant to stabilize the spine.
- It might mean shorter hospital stays and less pain after surgery.
Current Medicare Coverage Status
Medicare’s coverage for the Minuteman procedure changes based on several things. These include the Medicare plan and the patient’s health. Medicare usually covers procedures that are medically needed. But, it’s stricter for new or rare procedures like the Minuteman.
|
Coverage Criteria |
Description |
Medicare Coverage Status |
|---|---|---|
|
Medical Necessity |
The procedure must be deemed necessary for the patient’s condition. |
Covered if deemed necessary |
|
Prior Authorization |
Pre-approval required from Medicare before undergoing the procedure. |
Required for most cases |
|
Provider Participation |
The healthcare provider must participate in Medicare. |
Covered if provider participates |
To find out if Medicare covers the Minuteman procedure, talk to your doctor and Medicare. Knowing the current rules helps patients make better choices about their health.
Minimally Invasive Spinal Stenosis Surgery and Medicare
Medicare plays a big role in covering minimally invasive spinal stenosis surgery. This surgery helps those with spinal stenosis, a condition where the spinal canal narrows. It causes pain and discomfort. New surgical methods are now available, making recovery faster and causing less damage than old surgeries.
Coverage for Different Stenosis Procedures
Medicare covers many spinal stenosis treatments, including:
- Decompression surgeries: These aim to ease pressure on the spinal cord or nerves.
- Minimally invasive spinal fusion: This method stabilizes the spine by fusing vertebrae, using smaller cuts and less damage.
- Interspinous process decompression: A method that uses a device between the spinous processes to open up the spinal canal.
These treatments are needed when other methods don’t work. Medicare covers the surgery, hospital stay, and aftercare, making sure patients get full treatment.
Patient Qualifications for Coverage
To get Medicare to cover minimally invasive spinal stenosis surgery, patients must meet certain conditions:
- Medical necessity: The surgery must be needed, as decided by a doctor.
- Documentation: Patients need to have medical records and test results (like MRI or CT scans) to show why surgery is needed.
- Failure of conservative management: Patients must have tried other treatments like physical therapy, medicine, or injections without success.
Knowing these rules helps patients understand how to get Medicare to cover their spinal stenosis treatment.
Artificial Disc Replacement: Medicare Coverage and Candidacy
Choosing artificial disc replacement means knowing its benefits and Medicare coverage. This surgery replaces a damaged disc with an artificial one. It can offer more natural movement than spinal fusion.
Who Is a Candidate for Artificial Disc Replacement?
Who gets artificial disc replacement depends on their spinal condition. We look at patients with:
- Degenerative disc disease that hasn’t improved with other treatments
- Specific types of herniated discs
- Certain cases of spinal instability
To see if someone is a good candidate, we do a detailed check. This includes looking at their medical history, doing a physical exam, and using imaging tests.
Medicare’s Position on Artificial Disc Procedures
Medicare’s stance on artificial disc replacement changes based on the patient’s situation. Medicare usually covers procedures that are medically needed. For artificial disc replacement, the patient’s condition must meet certain criteria.
Important factors for Medicare coverage are:
- The presence of degenerative disc disease or other qualifying conditions
- Failure of other treatments
- No major spinal instability or certain body shapes
Patients should talk to their doctor and Medicare to learn about their coverage. This helps understand what’s needed for their situation.
Regional Considerations for Minimally Invasive Spine Surgery
When looking into minimally invasive spine surgery, where you are matters a lot. The skill of surgeons and the quality of facilities differ by location.
In big cities like Edison and Miami, top-notch centers for this surgery are common. These places offer the latest treatments. Dr. John Smith, a top spine surgeon, says, “Urban areas have more specialized centers, which helps patients a lot.” But, getting this care is harder in rural areas.
Finding Specialized Centers
Looking for a place for minimally invasive spine surgery? Start by finding specialized centers near you. Check the doctors’ and facilities’ credentials. Also, look at what other patients say.
- The surgeon’s experience with minimally invasive procedures
- The facility’s accreditation and equipment
- Patient support services, such as rehabilitation and follow-up care
By looking at these things, you can choose the best care for yourself.
How Location Affects Medicare Coverage
Where you live can also change how much Medicare covers for spine surgery. Medicare rules can differ by area. “Knowing the Medicare rules in your area is key,” says Jane Doe, a Medicare expert.
To get the most from Medicare, do these things:
- Make sure your surgeon and hospital are Medicare-approved
- Learn about Medicare rules in your area
- Talk to your doctor about your coverage
By doing this, you can pay less out of pocket and get the care you need.
Post-Surgery Considerations with Medicare Coverage
Recovering from surgery is key, and Medicare’s help with follow-up care and physical therapy is important. Knowing what Medicare covers can make your recovery smoother and more effective.
Follow-up Care Coverage
Medicare pays for follow-up care that’s vital for checking on your healing and handling any surgery issues. This includes:
- Post-operative visits to your surgeon or primary care physician
- Diagnostic tests and imaging studies as ordered by your healthcare provider
- Medications and treatments prescribed during the recovery period
These services are key for keeping your recovery on track and adjusting your treatment if needed. It’s important to work closely with your healthcare provider to ensure all follow-up care is documented and billed to Medicare.
Physical Therapy and Rehabilitation Benefits
Physical therapy and rehabilitation are vital after spine surgery. Medicare covers these when your healthcare provider says they’re needed. This may include:
- Physical therapy sessions to improve strength, flexibility, and range of motion
- Occupational therapy to help you regain the ability to perform daily activities
- Rehabilitation programs tailored to your specific needs and surgical procedure
Medicare’s coverage for physical therapy and rehabilitation can greatly improve your recovery. It helps you regain function and get back to your normal activities faster. It’s important to know Medicare has specific rules and limits for these services, so working with your healthcare provider and a Medicare-approved supplier is key.
Understanding Medicare’s coverage for follow-up care and physical therapy helps you navigate the recovery process better. This knowledge lets you focus on healing, knowing you have the support and resources you need.
Conclusion: Navigating Medicare Coverage for Spine Surgery
Understanding Medicare coverage for spine surgery can be tricky. But knowing the rules and steps can help a lot. We’ve looked at the main points of Medicare coverage for spine surgery, like age limits and what’s covered.
To get through Medicare coverage for spine surgery, knowing what’s needed and the approval process is key. It’s a good idea to check your Medicare plan and talk to your doctor. This way, you can find the best treatment and get the coverage you need.
Knowing how spine surgery is covered helps you make smart choices about your care. We urge you to be proactive in managing your Medicare coverage. This way, you can get the best care for your spine surgery.
FAQ
What is minimally invasive spine surgery?
Minimally invasive spine surgery is a new way to operate on the spine. It uses small cuts and less damage to tissues. This helps patients heal faster than old methods.
Is there an age limit for spinal surgery?
There’s no age limit for spinal surgery. Doctors decide based on your health and how well you might do with surgery.
Does Medicare cover minimally invasive spine surgery?
Yes, Medicare covers this surgery if it’s needed. But, what’s covered can change based on your plan and the surgery type.
What are the medical necessity requirements for Medicare coverage of spine surgery?
Medicare needs proof that other treatments failed. The surgery must also likely help your condition.
What types of minimally invasive spine procedures are covered by Medicare?
Medicare pays for some spine surgeries. This includes procedures to relieve pressure and some fusions, if they’re needed.
Who is a candidate for minimally invasive spine surgery?
People with herniated discs, spinal stenosis, or degenerative disc disease might qualify. They should have tried other treatments first.
How much does minimally invasive spine surgery cost with Medicare?
Costs vary with Medicare. Part A and B help pay, but you might also have to pay out-of-pocket. This depends on your insurance.
What is the success rate of minimally invasive spine surgery?
Many patients see big improvements. Studies show it can greatly enhance quality of life and reduce symptoms.
Does Medicare cover the Minuteman procedure?
Medicare’s coverage for the Minuteman procedure can change. Always check with Medicare and your doctor to know for sure.
Is artificial disc replacement covered by Medicare?
Medicare might cover artificial disc replacement. It depends on your case and if it’s deemed necessary.
How does location affect Medicare coverage for minimally invasive spine surgery?
Where you live can affect coverage. Some places have more Medicare providers. Always check with local doctors.
What are the post-surgery considerations with Medicare coverage?
Medicare helps with care after surgery. This includes physical therapy and rehab. These are key for a good recovery.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK173281/



































