
Allogeneic bone marrow transplantation is a complex process. It involves replacing a patient’s bone marrow with healthy stem cells from a donor. Recent advancements in care and teamwork have greatly improved survival rates at top centers.
The success rates of hematopoietic cell transplantation are seeing a big change. Data show that adults have a one-year survival rate of about 68% to 86%. Centers like Cedars-Sinai and Dana-Farber Brigham Cancer Center are doing even better, with rates over 80%.
These improvements highlight the key role of specialized care and donor matching in transplant success. As we keep improving, we’re seeing better results for patients getting HSC transplants.
Key Takeaways
- The one-year survival rate for adults after allogeneic bone marrow transplants ranges from 68% to 86%.
- Top-tier centers are achieving higher success rates, with some reporting rates above 80%.
- Specialized care and donor compatibility are key to transplant success.
- Recent advancements in care protocols have led to better survival rates.
- Multidisciplinary teamwork is vital for achieving high success rates in hematopoietic cell transplantation.
The Science Behind Allogeneic Bone Marrow Transplantation
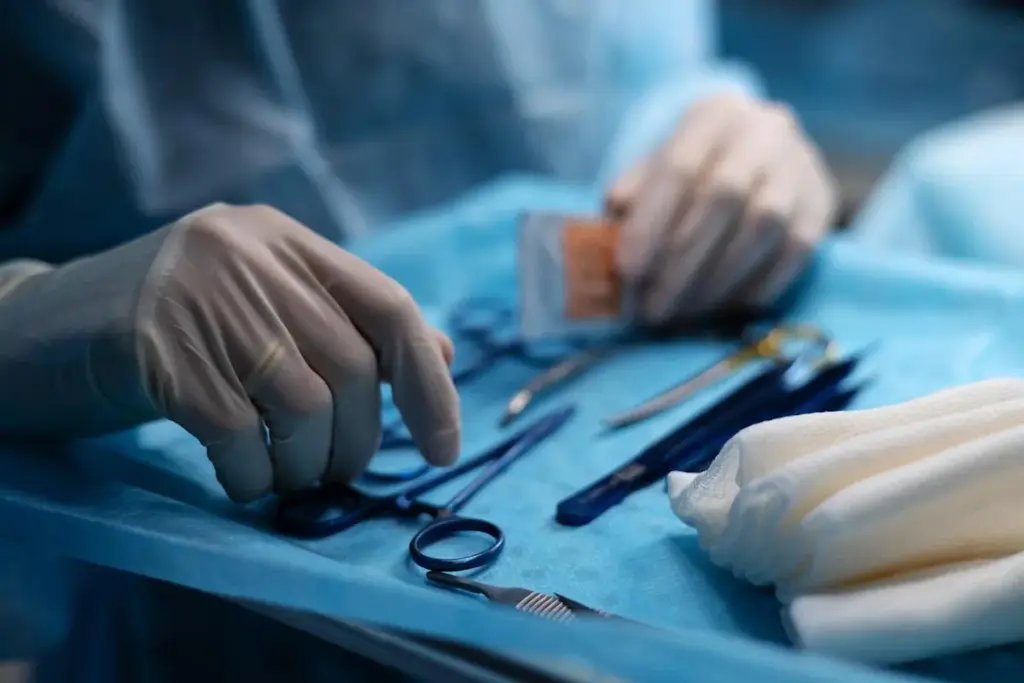
Understanding allogeneic bone marrow transplantation is key for those considering it. This treatment uses healthy stem cells from a donor to replace a patient’s bone marrow. It offers hope for many blood-related diseases and disorders.
Definition and Basic Procedure
Allogeneic bone marrow transplantation involves getting stem cells from a donor. These cells are then given to the patient after their bone marrow is cleared. This lets the donor stem cells grow and make healthy blood cells.
Differences Between Allogeneic and Autologous Transplants
The main difference is where the stem cells come from. Allogeneic transplants use donor cells, while autologous transplants use the patient’s own cells. Allogeneic transplants can fight cancer better, thanks to a graft-versus-leukemia effect as studies show.
Stem Cell Sources and Collection Methods
Stem cells for allogeneic transplants can come from bone marrow, blood, or umbilical cord blood. How they’re collected changes based on the source. Bone marrow is taken out surgically, while blood stem cells are collected through apheresis.
Choosing the right stem cell source and collection method is important. It depends on many factors, like who the donor is, the patient’s health, and the disease being treated.
Current Global Success Rates of Allogeneic Transplants
Allogeneic bone marrow transplants have seen big improvements thanks to new medical tech and treatment methods. Better donor matching, treatment plans, and care after transplant have boosted patient results. This shows how far we’ve come in helping patients.
One-Year Survival Statistics
Adults’ one-year survival rates after allogeneic bone marrow transplants vary from 68% to 86%. This range is influenced by the patient’s health at transplant and the treatment used. Top hospitals have even better survival rates, showing the power of expert care.
Three-Year Overall Survival Rates
The three-year survival rate is about 53%. This number shows the tough journey patients face after transplant. Yet, it also shows we’re making progress in improving long-term results.
Disease-Specific Outcome Variations
Success in allogeneic bone marrow transplants depends a lot on the disease type. For example, leukemia patients might have different survival rates than others. Knowing these differences helps tailor treatments better.
As we keep improving in allogeneic bone marrow transplants, we must focus on what affects success. This includes the disease, patient age, and how well the donor matches. By understanding these, we can give patients even better care and outcomes.
Leading Transplant Centers and Their Exceptional Outcomes

Allogeneic bone marrow transplantation has seen big improvements. This is thanks to top transplant centers. They’ve not only raised survival rates but also raised the bar in patient care and treatment.
Cedars-Sinai’s 85.8% One-Year Survival Achievement
Cedars-Sinai has hit a high mark with an 85.8% one-year survival rate in bone marrow transplants. This shows their dedication to the latest treatments and caring for patients fully.
Dana-Farber Brigham Cancer Center’s 80.6% Success Rate
The Dana-Farber Brigham Cancer Center boasts an 80.6% success rate in bone marrow transplants. Their success comes from a team effort that includes new therapies and strong support care. For more on their achievements, check out their latest news release.
What Sets Top-Tier Centers Apart
So, what makes these centers stand out? The main reasons are:
- Customized treatment plans for each patient
- Full care before and after the transplant
- Leading-edge research and clinical trials
- A team of experts working together
These factors together make a strong system. It boosts patient results and survival chances.
European Registry Data: Tracking 20,000+ Allogeneic Transplants
Recent data from European registries shows over 20,000 allogeneic transplants. This gives us valuable insights into transplant success rates. It helps us understand the current state of allogeneic bone marrow transplantation in Europe.
Comprehensive European Transplant Statistics for 2023
The European registry data gives us a detailed look at allogeneic transplant outcomes in 2023. Key statistics include:
|
Category |
Number of Transplants |
Success Rate |
|---|---|---|
|
Related Donor Transplants |
8,000 |
75% |
|
Unrelated Donor Transplants |
12,000 |
68% |
These statistics show a big improvement in allogeneic transplantation. Success rates have gone up a lot compared to before.
Comparative Analysis with North American Outcomes
When we compare European transplant outcomes with North America, some trends stand out. North American centers have seen slightly higher success rates in some areas. But European data shows a steady trend across different donor types.
“The European registry data provides a robust foundation for understanding allogeneic transplant outcomes, enabling us to identify best practices and areas for improvement.”
Transplant Specialist
Regional Variations in Transplant Protocols
There are clear regional differences in transplant protocols across Europe. For example, some Northern European centers use more intense conditioning regimens. In contrast, Southern European centers focus on reduced-intensity protocols.
It’s important to understand these regional differences. This helps us improve transplant outcomes and develop standard best practices across regions.
Critical Factors Influencing Allogeneic Bone Marrow Transplant Success
Several key factors affect the success of allogeneic bone marrow transplants. These factors are important for better transplant results and higher survival rates.
Disease Type and Stage at Transplantation
The disease type and stage at transplant time greatly influence success. Patients with early-stage disease usually do better than those with advanced disease.
Patient Age and Pre-existing Health Conditions
Patient age and health conditions are also very important. Older patients or those with serious health issues may face higher risks. This is because they have less physical strength and are more likely to get complications.
Donor Selection and HLA Compatibility
Donor selection and HLA compatibility are key to transplant success. A well-matched donor lowers the risk of graft-versus-host disease (GVHD). This improves survival chances. The level of HLA matching greatly affects transplant results.
In summary, allogeneic bone marrow transplant success depends on many factors. These include disease type, patient age, donor selection, and HLA compatibility. By carefully managing these factors, healthcare providers can improve patient outcomes. This leads to better success rates in allogeneic bone marrow transplantation.
Donor Types and Their Impact on Transplant Outcomes
The choice of donor is key to a successful bone marrow transplant. The donor type greatly affects the outcome. Many factors play a role in this.
Related vs. Unrelated Donor Comparisons
Choosing between a related or unrelated donor is a big decision. Related donors, like siblings or parents, are a better match because they share genes. Research shows that transplants from related donors have lower risks of GVHD and better survival rates than those from unrelated donors.
Haploidentical Transplantation Advancements
Haploidentical transplantation uses a half-match donor, often a family member. This method has grown, making more donors available, even for those without a full match. New techniques have lowered GVHD risks and improved results.
Umbilical Cord Blood as an Alternative Source
Umbilical cord blood (UCB) is a new option for stem cell transplants. It’s quick to get and has a lower GVHD risk. But, UCB units often have fewer cells, which can be a problem for adults.
|
Donor Type |
GVHD Risk |
Overall Survival |
|---|---|---|
|
Related Donor |
Lower |
Higher |
|
Unrelated Donor |
Higher |
Lower |
|
Haploidentical Donor |
Moderate |
Improving |
|
Umbilical Cord Blood |
Lower |
Varies |
Pre-Transplant Conditioning: Balancing Efficacy and Toxicity
Getting the pre-transplant conditioning right is key for allogeneic bone marrow transplants. It affects both how well the transplant works and its side effects. The choice of conditioning regimen can greatly impact the transplant’s success.
Myeloablative vs. Reduced-Intensity Conditioning Regimens
Myeloablative conditioning regimens aim to wipe out the patient’s bone marrow. They use strong doses of chemotherapy and/or radiation. This method is effective but can be very harsh.
Reduced-intensity conditioning (RIC) regimens, by contrast, use lower doses. They aim to weaken the immune system enough for donor cells to take hold. RIC is better for older patients or those with health issues who can’t handle stronger treatments.
Personalized Conditioning Based on Patient Factors
Personalized conditioning regimens are becoming more common. They tailor the treatment to the patient’s specific needs, age, and health. This approach tries to boost transplant success while cutting down on side effects.
Novel Conditioning Approaches
New methods are being looked into to better transplant outcomes. These include targeted therapies that aim to kill cancer cells more precisely. They also aim to make conditioning less intense but just as effective.
Several factors influence the choice of conditioning regimen:
- Disease type and stage
- Patient age and comorbidities
- Donor type and HLA compatibility
By carefully weighing these factors, doctors can create the best pre-transplant conditioning plans. This helps improve patient results.
Post-Transplant Care Pathways That Enhance Survival Rates
Good care after a transplant is key to helping patients live longer. The time after a transplant is very important. It’s when we manage problems and make sure patients do well.
Graft-versus-Host Disease Prevention and Management
Graft-versus-host disease (GVHD) is a big problem after a bone marrow transplant. GVHD prevention strategies include using medicines to keep the immune system in check and choosing the right donor. We have a detailed plan to prevent and treat GVHD. This helps keep patients safe and healthy.
Infection Control Strategies
Patients after a transplant are at high risk for infections because their immune system is weak. Infection control measures include using antibiotics, antifungals, and antivirals, and keeping everything clean. We make a plan for each patient to keep infections away.
Long-term Follow-up and Survivorship Programs
Keeping up with patients long after their transplant is very important. Our survivorship programs help manage long-term effects and chronic GVHD. We offer ongoing care that meets each patient’s needs, improving their life quality.
|
Care Pathway |
Description |
Benefits |
|---|---|---|
|
GVHD Prevention |
Immunosuppressive medications and careful donor selection |
Reduced risk of GVHD |
|
Infection Control |
Prophylactic medications and hygiene practices |
Minimized infection risk |
|
Long-term Follow-up |
Monitoring for late effects and managing chronic GVHD |
Enhanced quality of life |
By using these care paths, we help more patients survive and live better lives after a bone marrow transplant.
Liv Hospital’s Excellence in Allogeneic Transplantation
Liv Hospital leads in allogeneic transplantation, using the latest methods for top patient results. We aim to give the best healthcare, showing it in our detailed allogeneic bone marrow transplant approach.
International Competition Through Cutting-Edge Protocols
We compete globally by using the newest in allogeneic transplantation. Our methods are made to get the best results, with innovative treatments and state-of-the-art technology. a top expert says, “Success in allogeneic transplantation comes from being able to adapt and innovate.”
“The future of allogeneic transplantation is bright, with new technologies and treatments on the horizon.”
Continuous Quality Improvement Vision
At Liv Hospital, we always aim to improve quality. We want to keep our care at the highest level by constantly checking and improving our methods. This ensures our patients get the best results.
Ethical, Innovative “5-Star Tourism Healthcare” Programs
Our “5-star tourism healthcare” programs make care easy and comfortable for international patients. We focus on patient-centered care, making sure every part of our service, from treatment to stay, meets top quality and ethics.
Liv Hospital combines the latest medical methods with a focus on quality and patient happiness. Our commitment to excellence never wavers, and we keep working to give our patients the best care.
Recent Advances Revolutionizing Allogeneic Transplant Success
New breakthroughs in immunotherapy and precision medicine are changing allogeneic transplants. These advancements have greatly boosted patient survival and improved their quality of life after the transplant.
Immunotherapy Integration in Transplant Protocols
Adding immunotherapy to transplant plans has shown great promise. It boosts the graft-versus-leukemia effect and cuts down on graft-versus-host disease (GVHD).
Precision Medicine Approaches to Transplantation
Precision medicine lets doctors create treatment plans that fit each patient’s needs. This personalized approach makes transplants more effective and safer.
Enhanced Supportive Care Measures
Better supportive care, like improved infection control and GVHD management, has helped patients. This care ensures patients get the best support from start to finish.
|
Advance |
Description |
Benefit |
|---|---|---|
|
Immunotherapy |
Enhances graft-versus-leukemia effect |
Reduces relapse rates |
|
Precision Medicine |
Personalized treatment plans |
Improves efficacy and reduces toxicity |
|
Supportive Care |
Comprehensive care pathways |
Enhances patient outcomes and quality of life |
Optimizing Patient Selection for Successful Allogeneic Transplants
To increase success rates, choosing the right patients for allogeneic bone marrow transplants is key. It’s vital to pick patients carefully for the best results in this complex procedure.
Disease-Specific Transplant Timing
The timing of an allogeneic transplant matters a lot. It depends on the disease being treated. For some leukemias, transplanting early is best. Others might need a more careful timing.
Comprehensive Comorbidity Assessment Tools
Tools for assessing comorbidities are very helpful. They help find out if a patient’s health issues could affect the transplant’s success. This way, doctors can make better choices for each patient.
Psychosocial Preparation and Support Systems
Preparing patients mentally and socially is also critical. It’s about making sure they have the support they need. This includes their mental health and their social network, which is important for recovery.
By focusing on these areas, we can make patient selection better. This leads to higher success rates in allogeneic bone marrow transplants. Choosing the right patients is the foundation of successful transplants. Careful consideration of these factors is essential for the best results.
Conclusion: The Evolving Landscape of Allogeneic Bone Marrow Transplantation
The field of allogeneic bone marrow transplantation is growing fast. This is thanks to new ideas in immunotherapy, precision medicine, and care support. In 2019, the United States saw 9,299 such transplants. Survival rates vary, with 100-day survival rates between 90% and 93%. Three-year survival rates range from 53% to 74% for different groups.
Looking ahead, allogeneic bone marrow transplantation will keep getting better. Research and new methods in donor selection, treatment plans, and care after transplant will help patients more. For more details, check out the National Center for Biotechnology Information.
The future looks bright for allogeneic bone marrow transplantation. Breakthroughs in immunotherapy and precision medicine could make treatments better and more available. As the field grows, we’ll see better survival rates and care for patients.
FAQ
What is an allogeneic bone marrow transplant?
An allogeneic bone marrow transplant is a medical procedure. It replaces a patient’s bone marrow with healthy stem cells from a donor.
What is the success rate of allogeneic bone marrow transplants?
Adults have a one-year survival rate of 68% to 86% after these transplants. Top centers can achieve even higher success rates.
What factors influence the success rate of allogeneic bone marrow transplants?
Several factors affect the success rate. These include the patient’s condition, the donor’s compatibility, and the treatment used.
What is the difference between allogeneic and autologous transplants?
Allogeneic transplants use donor stem cells. Autologous transplants use the patient’s own stem cells.
What are the different sources of stem cells for allogeneic bone marrow transplants?
Stem cells can come from related or unrelated donors. They can also come from umbilical cord blood.
What is haploidentical transplantation?
Haploidentical transplantation uses a donor who is a half-match to the patient.
What is pre-transplant conditioning, and why is it necessary?
Pre-transplant conditioning is a key step. It erases the diseased bone marrow and prepares the body for the transplant.
What are the different approaches to pre-transplant conditioning?
There are myeloablative and reduced-intensity regimens. Personalized conditioning is also used based on patient factors.
How is graft-versus-host disease prevented and managed?
Graft-versus-host disease is prevented and managed with immunosuppressive medications and supportive care.
What is the role of immunotherapy in allogeneic bone marrow transplantation?
Immunotherapy is used to enhance the graft-versus-tumor effect. It aims to improve patient outcomes.
How is patient selection optimized for successful allogeneic transplants?
Patient selection is optimized through disease-specific timing and comorbidity assessment. Psychosocial preparation and support systems are also key.
What is the significance of long-term follow-up and survivorship programs in allogeneic bone marrow transplantation?
Long-term follow-up and survivorship programs are vital. They monitor outcomes, manage late effects, and improve quality of life.
References



































