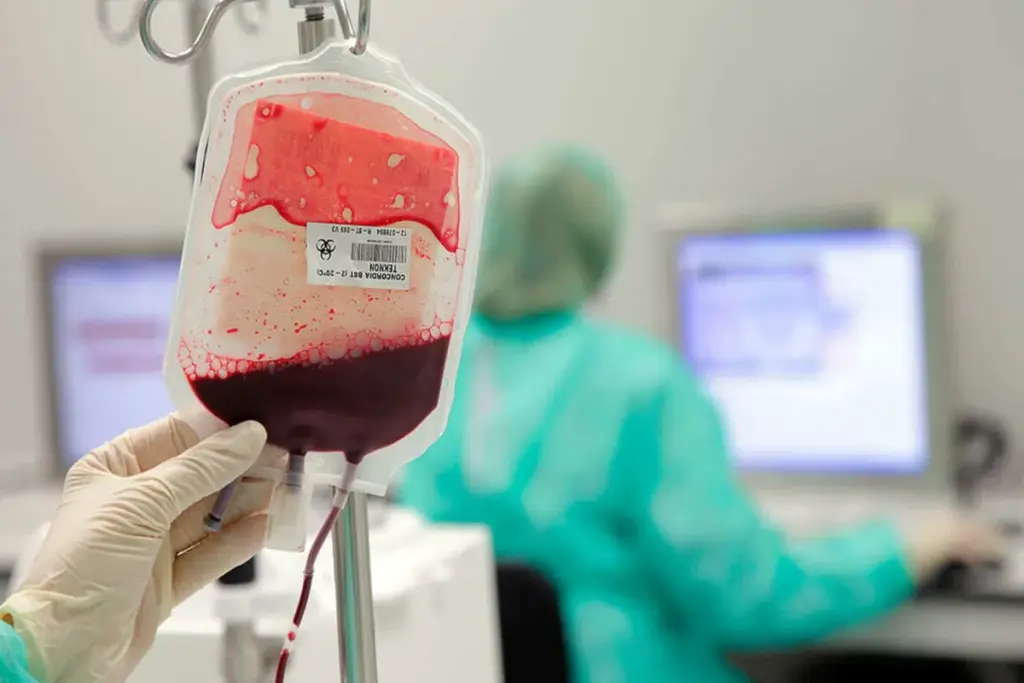
When patients get autologous transfusion, they get their own blood. This is safe but not always possible. So, other options are needed when this isn’t an option.
Allogeneic blood transfusion is a key alternative. It uses blood from others. This is important when a patient can’t use their own blood.
Top hospitals like Liv Hospital focus on safer blood transfusions. Knowing the options to autologous therapy is key for the best care.
Key Takeaways
- Autologous transfusion uses a patient’s own blood.
- Allogeneic blood transfusion is a primary alternative when autologous transfusion is not feasible.
- Allogeneic transfusion involves using blood donated by others.
- Patient-focused innovations are key for safer transfusions.
- Understanding alternatives to autologous therapy is vital for the best care.
Understanding Autologous Medical Term and Transfusion Basics
In transfusion medicine, autologous transfusion is a standout. It uses a patient’s own blood components. This method is getting more attention because it can lower risks from other blood transfusions.
Autologous transfusion collects, stores, and reinfuses a patient’s blood or blood components. It’s very helpful in surgeries where a lot of blood loss is expected.
Definition and Purpose of Autologous Transfusion
Autologous transfusion means a patient gets their own blood. This reduces the chance of bad reactions and infections. The main goal is to give a safe, compatible blood transfusion, just for that patient.
This method has many benefits. It lowers the risk of immune reactions, infections, and blood type problems. It’s great for people with rare blood types or those who have developed antibodies against certain blood components.
Limitations and Contraindications
Autologous transfusion has some downsides. It needs careful planning before surgery, can waste blood, and is more expensive. These factors include the cost of collecting and storing the blood.
Some health issues, like infections or cancers, might make autologous transfusion not suitable. It’s important to check the patient’s health history and current condition before deciding on this procedure.
|
Aspect |
Autologous Transfusion |
Allogeneic Transfusion |
|---|---|---|
|
Blood Source |
Patient’s own blood |
Donor blood |
|
Risk of Transfusion Reactions |
Lower |
Higher |
|
Infectious Disease Transmission |
Lower |
Higher |
|
Preoperative Planning Required |
Yes |
No |
Knowing about autologous transfusion helps healthcare providers make better choices for patients. This knowledge is key to understanding other transfusion methods and improving patient care.
Allogeneic Blood Transfusion: The Primary Alternative
When we can’t use autologous transfusion, allogeneic blood transfusion is the next best option. It uses blood from donors. This blood is tested and processed to make sure it’s safe and matches the recipient’s blood type.
How Allogeneic Transfusions Work
The process starts with blood donation. Donated blood is checked for diseases and then split into parts like red blood cells and plasma. Each part is kept in the right conditions until it’s given to a patient.
Compatibility testing is key. It matches the donor’s blood with the recipient’s to avoid bad reactions. We use the latest methods to reduce the risk of these reactions.
Current Statistics and Usage in the United States
In the US, allogeneic blood transfusions are common. In 2023, over 12 million units were used. This shows how often this method is needed.
The 12 Million Units Perspective
Allogeneic transfusions are vital, as seen by the numbers. Here are some stats:
|
Year |
Units Transfused (in millions) |
Percentage Change |
|---|---|---|
|
2020 |
11.4 |
– |
|
2021 |
11.8 |
+3.5% |
|
2022 |
11.9 |
+0.8% |
|
2023 |
12.1 |
+1.7% |
The table shows more units are being used each year. This means more people are relying on allogeneic blood transfusions.
“The demand for blood components continues to rise, driven by an aging population and advances in medical treatments that require blood transfusions.”
— American Red Cross
We keep working to make allogeneic blood transfusions safer and more effective. This way, patients get the best care possible.
Risks and Complications of Allogeneic Blood Transfusions
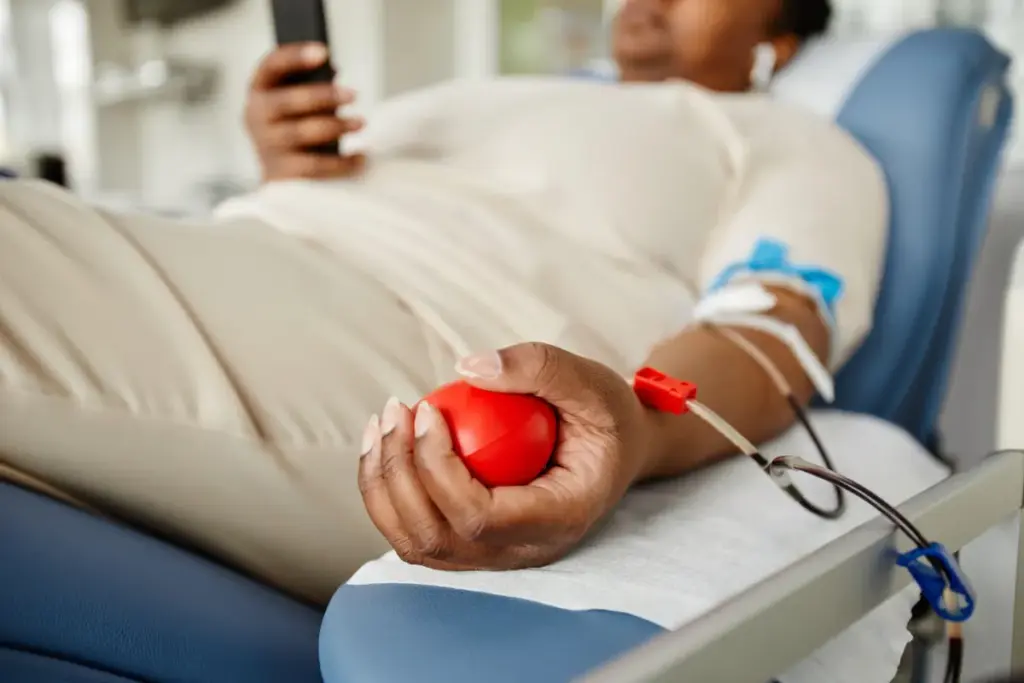
Allogeneic blood transfusions save lives but carry risks. Healthcare providers must manage these risks carefully. Understanding the challenges of allogeneic transfusions is key.
Transfusion Reactions
Transfusion reactions are a big risk with allogeneic blood transfusions. These reactions can be mild or severe and come in different types.
Febrile Reactions (5-10% Risk)
Febrile reactions are common, happening in 5-10% of cases. They cause a rise in body temperature and may include chills. Quick action is needed to prevent things from getting worse.
Allergic Reactions and TRALI
Allergic reactions can happen, from mild to severe. Transfusion-Related Acute Lung Injury (TRALI) is a serious issue. It causes lung problems and can be deadly. TRALI is a major cause of death from transfusions.
“The risk of TRALI highlights the importance of choosing the right donor and watching the recipient closely.”
Immunosuppression and Long-term Complications
Allogeneic blood transfusions can weaken the immune system. This can harm patients, mainly those who have had surgery or have cancer. Long-term issues might include getting infections more easily and tumors coming back.
Infectious Disease Transmission Concerns
There’s a chance of getting infectious diseases from allogeneic blood transfusions. This includes viruses like HIV and hepatitis B and C, and new ones. Thanks to better screening, these risks are lower, but they’re not gone.
Patient Blood Management (PBM) as a Modern Alternative
Patient Blood Management (PBM) is a new way to cut down on blood transfusions. It focuses on making a patient’s blood better before, during, and after surgery. This helps lower the risks of blood transfusions.
Core Principles
PBM uses a team effort to care for patients. Optimizing patient blood before surgery is key. This means treating anemia and improving blood health.
During surgery, minimizing blood loss is the goal. This is done with careful surgical methods and the right tools. After surgery, managing anemia well helps avoid transfusions.
Three Pillars of Implementation
PBM has three main parts:
- Preoperative Optimization: This means finding and treating anemia, stopping certain medicines, and making sure the patient’s blood volume is good.
- Intraoperative Blood Conservation: Using careful surgery, electrocautery, and cell salvage helps reduce blood loss.
- Postoperative Care: Handling anemia with iron therapy and avoiding too many blood tests are important steps.
Success Rates
PBM has been shown to greatly lower transfusion rates. Hospitals using PBM have seen a 20-40% reduction in transfusions. This not only lowers transfusion risks but also improves patient results.
|
PBM Component |
Description |
Benefit |
|---|---|---|
|
Preoperative Optimization |
Treating anemia, stopping anticoagulants |
Reduces transfusion need |
|
Intraoperative Blood Conservation |
Meticulous surgery, cell salvage |
Minimizes blood loss |
|
Postoperative Care |
Managing anemia, minimizing diagnostic blood draws |
Improves recovery |
By using PBM, healthcare can greatly improve patient care and lessen blood transfusion needs. This modern method follows the latest research and guidelines. It ensures patients get the best treatment.
Cell Salvage Techniques in Modern Medicine
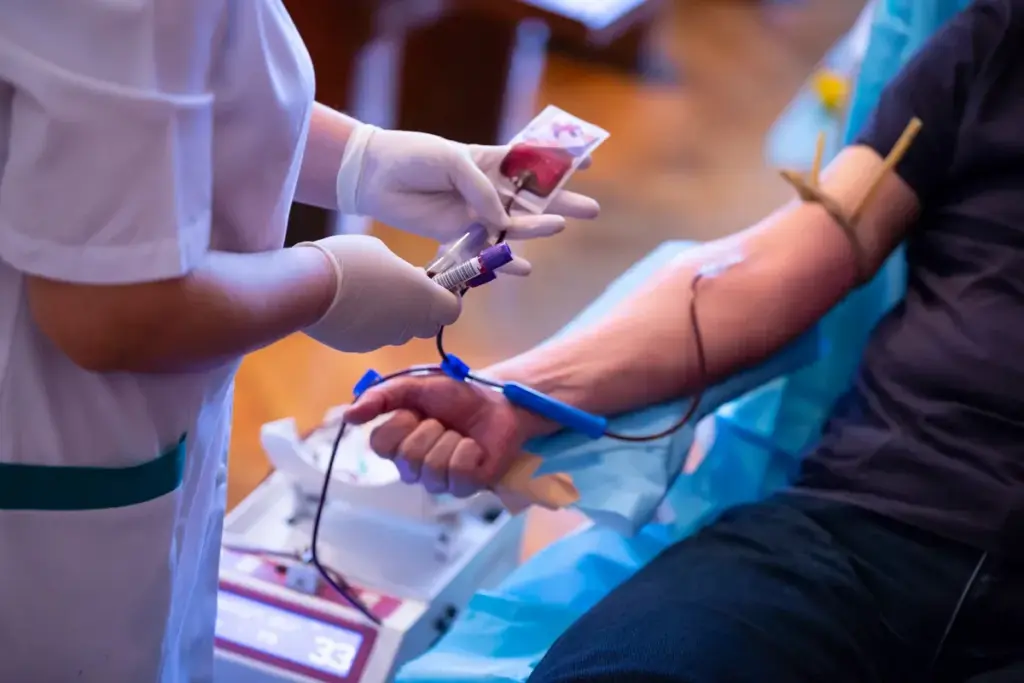
In today’s medicine, cell salvage is key for cutting down blood loss. It helps reduce the need for blood from others. This method collects and returns a patient’s own blood lost during or after surgery.
Intraoperative Cell Salvage Methods
Intraoperative cell salvage collects, cleans, and returns a patient’s blood lost during surgery. It’s widely accepted for its role in lowering the need for blood from others. The process includes suctioning blood, cleaning it, and then putting it back into the patient.
Postoperative Blood Recovery Systems
Postoperative blood recovery systems gather and return blood lost after surgery. They’re great for surgeries with a lot of bleeding after. These systems help keep the patient’s blood in and cut down on the need for more transfusions.
Cell salvage, including intraoperative and postoperative methods, is vital in surgery today. It saves the patient’s blood and lowers risks from blood from others, like reactions and infections.
Using cell salvage, doctors can greatly improve patient care and outcomes.
Synthetic Oxygen Carriers and Blood Substitutes
Medical technology is getting better, leading to new synthetic oxygen carriers and blood substitutes. These new options aim to make blood transfusions safer and more reliable. They could help patients in need without the risks of traditional blood transfusions.
Current Development Status of Artificial Blood
Creating artificial blood has been a goal for a long time. Advances in engineering and materials science are helping us get closer. Synthetic oxygen carriers are showing promise in carrying oxygen like red blood cells do.
“The development of artificial blood substitutes is a critical step towards reducing our reliance on donated blood,” says a leading researcher in the field.
Hemoglobin-based oxygen carriers (HBOCs) are making progress. They aim to work like hemoglobin in red blood cells. HBOCs could be used in trauma care, surgery, and treating certain medical conditions.
Hemoglobin-Based Oxygen Carriers (HBOCs)
HBOCs are a key area in artificial blood development. They are made to carry oxygen to tissues and organs like natural hemoglobin. Using HBOCs could reduce the need for donated blood, lowering risks of reactions and infections.
HBOCs can be stored longer than donated blood and might be compatible with everyone. But, making them safe and effective is a big challenge. It requires a lot of testing and clinical trials.
As we keep working on synthetic oxygen carriers and blood substitutes, we’re getting closer to safer blood transfusions. This could greatly improve patient care and outcomes. Ongoing research will likely lead to more innovation in this field.
Comparing Autologous Medical Term Applications with Alternatives
When we talk about blood transfusions, it’s important to compare autologous and allogeneic methods. Healthcare providers must look at the good and bad sides of each to make the right choice.
Clinical Outcomes: Autologous vs. Allogeneic Approaches
Research shows different results for safety and success in autologous and allogeneic transfusions. Using a patient’s own blood can lower the chance of bad reactions and diseases. But, blood from donors is easier to get but might have more risks.
Studies suggest autologous transfusions work better for some surgeries. Yet, they can be pricey and hard to set up. We need to think about these points when picking a transfusion method.
Cost-Benefit Analysis of Different Transfusion Methods
It’s key to look at the cost and benefits of autologous and allogeneic transfusions. Autologous transfusions might be better for patients but cost more. Allogeneic transfusions are cheaper but might lead to more problems, which could cost more in the long run.
We should think about all costs, not just the transfusion itself. This includes the cost of dealing with complications and making patients better. By looking at all these, we can choose the most affordable transfusion options.
In the end, picking between autologous and allogeneic transfusions depends on many things. We need to think about how well they work, the cost, and what’s best for the patient. By knowing the pros and cons, we can give our patients the best care.
Implementation of Modern Transfusion Alternatives in Leading Hospitals
Leading hospitals are changing patient care with new transfusion methods. Liv Hospital is at the forefront, using advanced blood management strategies.
Liv Hospital’s Approach to Blood Management
Liv Hospital aims to be the best globally, focusing on innovation and safety. It uses Patient Blood Management (PBM) and cell salvage techniques to improve patient care. These methods cut down the need for blood from others.
The hospital’s Patient Blood Management program focuses on three main areas. It aims to keep blood levels right, reduce blood loss, and boost the body’s blood production. This approach has lowered transfusion rates by 20-40%, meeting global standards.
Aligning with Global Standards for Safety and Ethical Excellence
Liv Hospital follows international blood transfusion standards. It uses modern methods to ensure top-quality care and lower risks from traditional blood transfusions.
The hospital relies on autologous procedures, using a patient’s own blood. This reduces the chance of bad reactions and fits with the hospital’s goal of world-class healthcare.
Liv Hospital leads the way in using new transfusion methods. Its focus on innovation, safety, and ethics shows its dedication to outstanding patient care.
Conclusion
Looking at alternatives to autologous transfusion, we see a future where both old and new methods are used. Advances in Patient Blood Management (PBM), cell salvage, and synthetic oxygen carriers mark this evolution. These changes are key to improving transfusion medicine.
Healthcare providers can use a mix of allogeneic blood transfusion, PBM, cell salvage, and synthetic oxygen carriers. This approach helps manage blood resources better. It also reduces the risks of blood transfusions.
In autologous medical practice, having many options is vital for personalized care. As technology gets better, we’ll see more improvements in transfusion medicine. This will make treatments safer and more effective for patients.
FAQ
What is autologous transfusion?
Autologous transfusion uses a patient’s own blood. It’s collected, stored, and then given back to the patient during or after surgery. This reduces the need for blood from others.
What are the limitations of autologous transfusion?
It needs planning ahead. There’s a chance of blood waste. It’s not always available in emergencies. So, other options are sometimes needed.
How does allogeneic blood transfusion work?
Allogeneic blood transfusion uses blood from someone else. It’s checked for safety and match before being given to the patient. This helps avoid bad reactions.
What are the risks associated with allogeneic blood transfusions?
These transfusions can cause reactions and weaken the immune system. They might also lead to long-term problems or diseases. This makes careful thought and other options important.
What is Patient Blood Management (PBM)?
Patient Blood Management aims to cut down on blood transfusions. It does this by improving a patient’s blood before, during, and after surgery. It follows a three-pillar strategy.
How does cell salvage work?
Cell salvage collects and cleans a patient’s lost blood during surgery. Then, it’s given back to the patient. This reduces the need for blood from others and helps control blood loss.
What are synthetic oxygen carriers and blood substitutes?
Synthetic oxygen carriers and blood substitutes are new options. They include things like hemoglobin-based oxygen carriers (HBOCs). They aim to change how we do blood transfusions.
How do autologous and allogeneic transfusion approaches compare?
Autologous transfusion is safer but limited by availability. Allogeneic transfusion is more common but riskier. Each has its own benefits and drawbacks.
What is the role of leading hospitals like Liv Hospital in implementing modern transfusion alternatives?
Hospitals like Liv Hospital lead in using new transfusion methods. They use Patient Blood Management and cell salvage to improve patient care. They follow global safety and ethical standards.
What is autologous cell therapy?
Autologous cell therapy uses a patient’s own cells. These cells are collected, processed, and given back to the patient. It helps in healing and regeneration, showing promise in medicine.
What is autologous regenerative medicine?
Autologous regenerative medicine uses a patient’s own cells and tissues. It helps in healing and regeneration. It’s a new way to treat many medical conditions.
References
- PMC: https://pmc.ncbi.nlm.nih.gov/articles/PMC10293705/
- Canadian Blood Services: https://www.blood.ca/en/blood/blood-transfusion/types-blood-transfusion
- PMC: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6943137/
- AHA Journals: https://www.ahajournals.org/doi/full/10.1161/CIR.0000000000000689
- EMA: https://www.ema.europa.eu/en/human-regulatory/overview/blood-transfusion-products-overview
- BMJ: https://www.bmj.com/content/368/bmj.m400

































