
Arteriovenous malformation (AVM) surgery is a complex procedure that has garnered significant attention due to its ability to drastically improve or save lives. Studies have shown that the success rate of AVM surgery varies significantly based on the location and type of AVM, making it a critical concern for both patients and healthcare providers.
For patients considering AVM surgery, understanding the before and after avm surgery outcomes is key. The journey through AVM treatment is not just about the surgical procedure itself. It’s also about the care received before and after surgery, which greatly impacts the treatment’s success.
We will explore the intricacies of AVM surgery, including success stories and treatment results. This will provide a detailed overview for those seeking this complex medical intervention.
Key Takeaways
- AVM surgery success rates vary based on the AVM’s location and type.
- Understanding the before and after aspects of AVM surgery is critical for patient care.
- Comprehensive care before and after surgery impacts treatment success.
- AVM treatment results have shown significant improvement in patient outcomes.
- Success stories from AVM surgery highlight the procedure’s great promise.
Understanding Arteriovenous Malformations (AVMs)
It’s important for both patients and doctors to know about arteriovenous malformations (AVMs). These malformations can really affect brain health. AVMs consist of abnormal connections between arteries and veins, typically located in the brain or spine.
What is an AVM?
An arteriovenous malformation (AVM) is a mix-up of blood vessels in the brain. It messes up normal blood flow. Unlike normal blood vessels, AVMs don’t have a capillary bed. This means there’s a direct link between arteries and veins.
This can lead to many neurological symptoms and serious problems.
Key characteristics of AVMs include:
- Abnormal connections between arteries and veins
- High blood flow through the malformation
- Risk of rupture and bleeding
- Potential for neurological damage
Common Locations of AVMs in the Brain
AVMs can happen in different parts of the brain. Some places are more common than others. The most frequent sites include:
- Cerebral hemispheres: Often affecting the frontal, parietal, or temporal lobes.
- Basal ganglia and thalamus: Deep-seated AVMs that can be challenging to treat.
- Brainstem: AVMs in this area are very risky because of the brainstem’s important functions.
Knowing where an AVM is helps doctors figure out the best treatment. This might include avm surgery brain procedures.
Symptoms and Diagnosis
The symptoms of AVMs can vary a lot. They depend on where and how big the AVM is. Common symptoms include:
- Seizures
- Headaches
- Neurological deficits (e.g., weakness, numbness)
- Hearing or vision disturbances
Doctors use advanced imaging like MRI, CT scans, or angiography to diagnose AVMs. These tests help doctors understand the AVM’s structure and location. This is key for planning brain avm surgery or other treatments.
Types of AVM Surgery
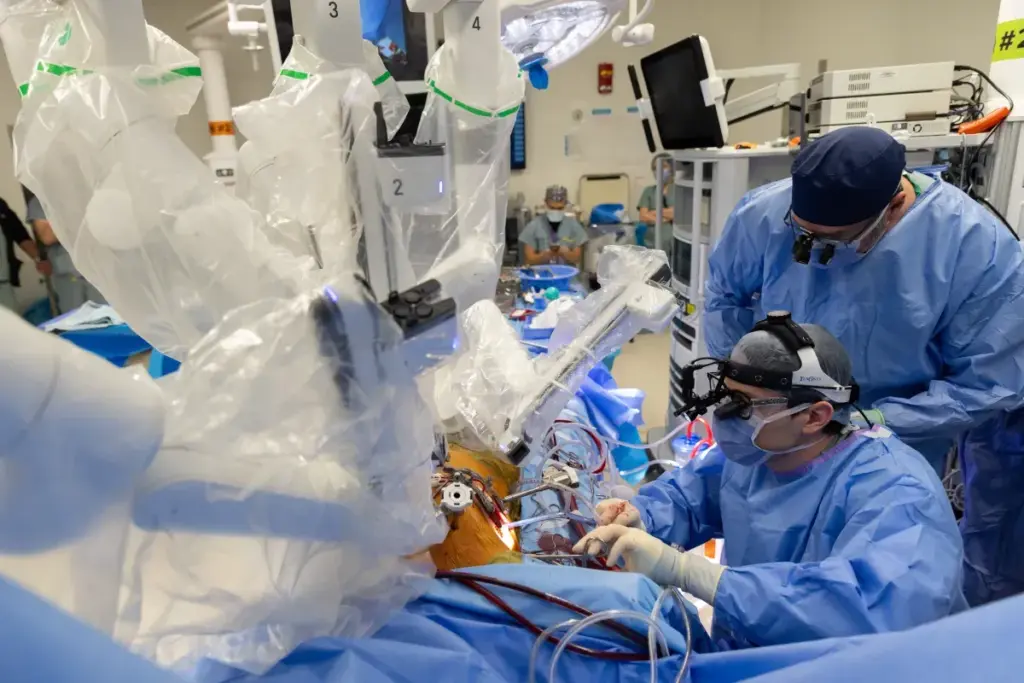
There are several ways to treat Arteriovenous Malformations (AVMs), each with its own benefits. The right surgery depends on the AVM’s size, location, and health of the patient.
Microsurgical Resection
Microsurgical resection is a traditional and effective method. It involves removing the malformation from the brain. This method is good for AVMs that are easy to reach and at high risk of bleeding. It requires a lot of precision and is done by skilled neurosurgeons.
A leading neurosurgeon says, “Microsurgical resection is a direct way to get rid of the AVM. It has a high success rate for certain patients.”
“The key to successful microsurgery is meticulous technique and a thorough understanding of the AVM’s anatomy.”
Endovascular Embolization
Endovascular embolization is a less invasive procedure. It uses materials like coils or liquids to shrink the AVM. This makes it easier to treat or even remove the need for surgery. It’s often used with other treatments.
|
Treatment Modality |
Description |
Advantages |
|---|---|---|
|
Microsurgical Resection |
Surgical removal of AVM |
High cure rate, direct removal |
|
Endovascular Embolization |
Minimally invasive embolization |
Reduces AVM size, less invasive |
|
Stereotactic Radiosurgery |
High-dose radiation to AVM |
Non-invasive, effective for small AVMs |
Stereotactic Radiosurgery
Stereotactic radiosurgery (SRS) is a non-invasive treatment. It uses high-dose radiation to close the AVM over time. SRS works well for small to medium-sized AVMs that are hard to reach surgically. Its success depends on the AVM’s size and location.
Hybrid Approaches
For complex AVMs, a mix of techniques, called hybrid approaches, might be used. For example, embolization followed by surgery or SRS. This approach tailors treatment to each patient’s AVM.
As neurosurgery advances, AVM treatment becomes more personalized and effective. Knowing about different surgeries helps patients and doctors make the best treatment plans.
Determining Candidacy for AVM Surgery
Choosing to have AVM surgery is a big decision. It depends on many important factors. Not every patient with arteriovenous malformations (AVMs) is a good candidate for surgery. A detailed check-up is needed to find the best treatment.
Factors That Influence Surgical Decisions
Several key factors influence the decision to proceed with AVM surgery. These include:
- AVM Size and Location: Larger AVMs or those located in critical areas of the brain may pose greater surgical risks.
- Patient’s Age and Health: Younger patients or those with fewer health issues are generally considered better candidates for surgery.
- Symptoms and Previous Hemorrhages: Patients who have experienced bleeding due to their AVM may be more likely to undergo surgery.
- AVM Characteristics: The presence of certain features, such as deep venous drainage or associated aneurysms, can affect surgical decisions.
The Spetzler-Martin Grading System
The Spetzler-Martin Grading System is a widely used method for assessing the risks associated with AVM surgery. This system grades AVMs based on:
- Size: Larger AVMs receive higher scores.
- Location: AVMs in critical or eloquent areas of the brain are scored higher.
- Deep Venous Drainage: Presence of deep venous drainage increases the score.
The total score helps predict surgical risks and outcomes, guiding treatment decisions.
When Surgery May Not Be Recommended
In some cases, the risks associated with AVM surgery may outweigh the benefits. Surgery may not be recommended for:
- Patients with high-grade AVMs that are difficult to access or are located in very sensitive areas.
- Those with significant health issues that increase surgical risks.
- AVMs that have not bled and are considered low-risk.
In such cases, alternative treatments or conservative management may be considered. This approach focuses on monitoring and managing symptoms.
Understanding the factors that influence AVM surgery candidacy is key. By evaluating individual patient characteristics and AVM features, healthcare providers can choose the best treatment. This approach optimizes AVM treatment results and post AVM surgery care.
Preparing for AVM Surgery
To get the best results from AVM surgery, you need to prepare well. This includes your health, medications, and how you feel. Getting ready for surgery can make you feel less anxious and help you recover better.
Medical Evaluations and Tests
Before surgery, you’ll go through many tests. These help doctors understand your health and the AVM. They might use imaging tests like MRI or angiography to see where the AVM is and how it works.
You might also have blood tests, electrocardiograms (ECGs), and other checks. These help doctors know if you’re healthy enough for surgery and if there are any risks.
Medication Adjustments
Changing your medications is a big part of getting ready for surgery. Some medicines might be stopped before surgery to lower the risk of bleeding. For example, anticoagulant medications that make your blood thinner might be stopped.
Tell your doctor about all the medicines you take. This includes prescription drugs, over-the-counter medicines, and supplements. They can tell you what changes you need to make.
Mental and Emotional Preparation
Getting ready mentally and emotionally is just as important as physical preparation. Talk to your healthcare team about your worries and hopes. They might offer counseling or psychological support to help with anxiety and getting ready for after surgery.
Try relaxation techniques like deep breathing, meditation, or yoga. These can help you feel less stressed and more positive before surgery.
The AVM Surgical Procedure
Surgery for AVMs uses the latest medical tech and skilled neurosurgeons. The success of the surgery depends on the team’s skill and the tech used.
Anesthesia and Surgical Setup
The first step is giving the patient general anesthesia. This keeps them comfortable and calm during the surgery. A team of experts, including neurosurgeons and nurses, work together. They use advanced tools to watch the surgery in real-time.
“The key to successful AVM surgery lies in meticulous planning and precise execution,” says a renowned neurosurgeon. “Our team works closely together to ensure that every aspect of the procedure is carefully managed.”
Surgical Techniques for Brain AVM Surgery
There are different ways to do brain AVM surgery. Microsurgical resection uses a microscope to remove the AVM. Endovascular embolization blocks blood flow to the AVM. Stereotactic radiosurgery uses radiation to slowly close the AVM.
Duration and Complexity Factors
The time it takes for AVM surgery varies. It depends on the AVM’s size, location, and the patient’s health. The surgery can last from a few hours to several hours. The team keeps a close eye on the patient’s health during the surgery.
Advanced Technologies Used in AVM Surgery
Modern tech is key to better AVM surgery results. Intraoperative imaging lets the team see the AVM and brain in real-time. Neuronavigation systems help find and remove the AVM accurately. These tools, along with the team’s skill, make the surgery safer and more effective.
As medical tech gets better, so does AVM treatment. This brings new hope to patients everywhere. We use the latest tech to give our patients the best care.
Before and After AVM Surgery: What to Expect
Knowing what to expect before and after AVM surgery can help ease anxiety. We aim to make the journey ahead clear and understandable.
Immediate Pre-Surgical Experience
The days before AVM surgery are key for getting ready. We recommend medical checks to make sure you’re ready. This includes blood tests, imaging, and a look at your medical history.
It’s crucial to adjust your medications as advised by your doctor, as stopping certain medicines can help minimize surgical risks. This might mean stopping some to avoid problems with surgery or anesthesia.
First 24-48 Hours Post-Surgery
The first 24-48 hours after surgery are watched closely. Patients are observed in the ICU for any immediate issues, like bleeding or changes in the brain.
After surgery, we focus on pain management, checking your brain health, and preventing problems. We use the latest methods to keep you comfortable.
Hospital Stay Duration
How long you stay in the hospital depends on your surgery and health. Typically, it’s a few days to a week.
Our team works together to handle any issues, manage pain, and help you recover smoothly.
Initial Recovery Milestones
The early recovery has important milestones. Start with gentle movements and slowly add more activities as you can.
Follow-up appointments are key to check on your healing and address any issues.
Understanding these milestones helps you navigate your recovery. It shows you what to expect at each stage.
AVM Surgery Success Rates
Understanding AVM surgery success rates is complex. It depends on the malformation’s characteristics and the treatment used. Knowing this is key for both patients and doctors.
Overall Success Statistics
Research shows AVM surgery can be very effective. Success rates range from 80% to over 90% in some cases. Success rates depend on the Spetzler-Martin grade of the AVM. Lower grades usually mean better results.
Factors That Influence Success
Many things affect AVM surgery success. These include the malformation’s size and location, the patient’s age and health, and the surgery techniques. The experience of the neurosurgical team is also very important.
Complete vs. Partial AVM Obliteration
The main goal of surgery is to completely remove the AVM. But, sometimes only part of it can be removed, mainly if it’s complex or in a sensitive brain area. The difference between complete and partial removal affects long-term results.
Success Rates by AVM Type and Location
AVM type and location greatly affect surgery success. AVMs in deep or sensitive brain areas are harder to treat and may have lower success rates. It’s important to understand these differences to set realistic hopes.
We know each patient is different, and success rates can vary a lot. Our team works closely with patients to offer personalized care. We aim to increase the chances of successful outcomes for each patient.
AVM Surgery Recovery Timeline
Knowing the recovery timeline after AVM surgery helps patients prepare. Recovery is a gradual process with different stages. Each stage has its own challenges and milestones.
First Week After Surgery
The first week is key for a good recovery. Patients are watched closely in the ICU for the first 24-48 hours. They might feel headaches, nausea, and fatigue, which are treated with medicine.
a top neurosurgeon, says, “The first week is very important. Managing symptoms well can greatly affect the outcome.”
“The first week is about recovery and adjustment, both physically and emotionally.”
First Month of Recovery
In the first month, patients keep getting better and adjusting. It’s important to see the doctor regularly to check on healing. They should avoid hard work to prevent problems.
- Start to do more physical activities as the doctor says.
- Watch for signs of infection or other issues.
- Go to all scheduled doctor visits.
Three to Six Months Post-Surgery
By three to six months, many see big improvements. The brain heals more, and symptoms from the AVM start to go away. But, some might have lasting effects like seizures or brain problems that need ongoing care.
|
Recovery Stage |
Typical Symptoms |
Recommended Actions |
|---|---|---|
|
First Week |
Headaches, nausea, fatigue |
Rest, medication management |
|
First Month |
Continued fatigue, possible neurological deficits |
Gradual increase in activity, follow-up appointments |
|
Three to Six Months |
Improving symptoms, possible residual effects |
Ongoing rehabilitation, symptom management |
Long-Term Recovery (Beyond Six Months)
Recovery beyond six months varies a lot. Some fully recover, while others face lasting effects from surgery or the AVM. It’s vital to keep seeing doctors to manage long-term issues and watch for AVM return.
Key factors influencing long-term recovery include:
- The size and location of the AVM.
- The presence of any pre-surgical neurological deficits.
- The effectiveness of the surgical intervention.
Helping patients understand the recovery timeline is key. It helps manage expectations and aim for the best results.
Potential Complications of AVM Surgery
It’s important for patients and doctors to know about AVM surgery risks. This surgery is very effective for treating arteriovenous malformations. But, it’s key to understand the possible dangers.
Immediate Surgical Complications
Right away, surgery can lead to bleeding, stroke, or harm to brain tissue. The skill of the surgical team and modern technology help lower these risks.
Short-Term Complications
Soon after, patients might face seizures, infection, or brain swelling. Doctors manage these with medicine and watchful care in the hospital.
Long-Term Complications
Later, problems could be neurological deficits like weakness, numbness, or thinking changes. The chance of these issues depends on the AVM’s size, location, and how it’s treated.
Risk Factors for Complications
Several things can make surgery risks higher. These include the size and location of the AVM, the patient’s overall health, and the surgical approach. Knowing these helps in making better treatment choices.
Every patient is different, and AVM surgery risks can vary a lot. So, it’s vital for patients to talk about their specific risks and worries with their doctor.
Advanced Devices and Technology in AVM Treatment
Medical technology has changed how we treat brain AVMs, bringing hope to patients everywhere. New devices and technologies have made AVM surgery safer and more effective.
Embolization Materials and Devices
Embolization is key in treating AVMs. It uses materials like Onyx and N-butyl cyanoacrylate (NBCA) to block the malformation. Flow-diverting stents are also being used for complex AVMs.
Imaging and Navigation Systems
Advanced imaging and navigation systems are essential for diagnosing and treating AVMs. 3D angiography and intraoperative MRI help neurosurgeons see the AVM clearly. They plan the surgery and check if it’s done right during the operation.
Radiosurgery Equipment
Radiosurgery is a non-surgical way to treat AVMs. It uses precise radiation to get rid of the malformation. Modern tools like Gamma Knife and CyberKnife are very accurate, protecting the brain.
Emerging Technologies
New technologies are coming into AVM treatment. Artificial intelligence (AI) and machine learning (ML) are being used to improve diagnosis and predict results. Nanotechnology might bring new embolization materials and methods.
As we keep improving AVM treatment, working together is key. Medical experts, researchers, and tech developers must collaborate. This way, we can get better AVM treatment results and help patients live better lives after brain AVM surgery.
Special Considerations for Brainstem AVM Surgery
Brainstem arteriovenous malformations (AVMs) are tough for neurosurgeons to handle. This is because they are in a very sensitive area. The brainstem connects the brain to the spinal cord. It controls important functions like breathing and heart rate.
Unique Challenges of Brainstem AVMs
Brainstem AVMs are hard to deal with because they are close to important parts of the brain. Surgeons need to know a lot about the brainstem’s structure. They also have to navigate through complex blood vessels.
One big challenge is avoiding damage to nearby brain tissue. This could lead to serious problems. So, surgeons use special techniques and the latest technology to help.
Surgical Approaches for Brainstem AVMs
There are different ways to treat brainstem AVMs, depending on the situation. Doctors might use surgery, endovascular embolization, or radiosurgery. Each method has its own benefits.
Choosing the right approach depends on many things. This includes the patient’s health and the AVM’s details. A team of experts works together to decide the best plan.
|
Surgical Approach |
Description |
Advantages |
|---|---|---|
|
Microsurgical Resection |
Direct surgical removal of the AVM |
Immediate removal of the AVM, possible complete removal |
|
Endovascular Embolization |
Minimally invasive procedure to block blood flow to the AVM |
Less risk of immediate surgery problems, can be used with other treatments |
|
Stereotactic Radiosurgery |
High-precision radiation therapy to obliterate the AVM |
Non-invasive, works well for small to medium AVMs, quick recovery |
Success Rates and Risk Assessment
Success in treating brainstem AVMs is measured in how well the malformation is removed and the patient’s recovery. Success rates depend on many factors. These include the AVM’s size, the surgery method, and the patient’s health before surgery.
“The treatment of brainstem AVMs requires a highly individualized approach, taking into account the unique characteristics of each patient’s condition and the latest advancements in neurosurgical techniques.”
Before surgery, doctors carefully assess the risks. They look at the chances of brain damage, surgery complications, and the AVM coming back. Advanced imaging, like MRI and angiography, helps with this.
Recovery Expectations
Recovering from brainstem AVM surgery can be complex and varies a lot. Many things can affect how well a patient recovers. These include the AVM’s size and location, the surgery type, and the patient’s health.
Patients usually need close care and monitoring after surgery. They might also need rehabilitation to deal with any brain problems that come up during recovery.
We know brainstem AVM surgery is scary. Our team is here to give you the best care and support. We want to make sure you get the best results possible.
Patient Success Stories: Life After AVM Surgery
Patients who have had AVM surgery share their stories. These stories give hope and practical advice for others facing AVM treatment. They show how recovery and life can change for the better.
Recovery Journeys
Every patient’s recovery is different. It depends on the AVM’s location, size, and the surgery type.a 32-year-old teacher, had surgery for a ruptured AVM in her brain. She talked about the key role of post AVM surgery care in her recovery.
“The first few weeks were tough. But with the right care and support, I got stronger and went back to my life.”
Quality of Life Improvements
Many patients see big improvements in their life after surgery.a 45-year-old businessman, had stereotactic radiosurgery for an AVM in his brainstem. He said it changed his life for the better.
“I went back to work and enjoyed time with my family without fear of bleeding. It was a game-changer.”
These AVM surgery success stories show the promise of treatment. They highlight the need for care tailored to each person.
Challenges Overcome
Recovery comes with big challenges.a 28-year-old artist, had surgery for a large AVM. She faced a long recovery but stayed determined.
“It was hard, but with my team and family’s support, I overcame it. I learned to adapt to my new life.”
Long-Term Outcomes
Long-term results for AVM surgery patients vary. But many fully recover and live normal lives. Studies show most patients see a big drop in bleeding risk.
Follow-up care is key to tracking these results and catching any issues early. Knowing the AVM surgery recovery timeline helps everyone prepare. It sets realistic goals and supports the recovery process.
Alternative and Complementary Treatments to AVM Surgery
Not all Arteriovenous Malformations (AVMs) need surgery. Other treatments are available for some patients. The choice depends on the AVM’s size, location, symptoms, and the patient’s health.
Observation and Monitoring
For some, watching and checking the AVM is enough. This is for small, symptom-free AVMs. Regular tests and visits help track any changes.
Key aspects of observation and monitoring include:
- Regular MRI or CT scans to monitor the AVM’s size and characteristics
- Clinical evaluations to assess for any new or worsening symptoms
- Patient education on recognizing symptoms that require immediate medical attention
Medication Management
Medicine can’t cure AVMs but can help with symptoms like seizures or headaches. It’s often used with other treatments or alone for those not suited for surgery.
|
Medication Type |
Purpose |
Examples |
|---|---|---|
|
Anticonvulsants |
To prevent seizures |
Carbamazepine, Levetiracetam |
|
Analgesics |
To manage pain |
Acetaminophen, Ibuprofen |
Emerging Treatments and Clinical Trials
Research is always looking for new AVM treatments. Some patients can join clinical trials for these new options.
As we learn more about AVMs, patients have more choices. Whether it’s new or established treatments, the aim is to give personalized care.
Conclusion: The Future of AVM Treatment
Looking at arteriovenous malformations (AVMs) and their treatments, AVM surgery stands out. It works well for many patients. Many have seen great improvements thanks to this surgery.
New medical tech and surgical methods are making AVM surgery even better. This means more people can live better lives after surgery. The road to recovery is tough, but knowing what to expect helps a lot.
The future of AVM treatment looks bright thanks to ongoing research and tech advancements. Healthcare teams will keep getting better at treating AVMs. This means patients will get even better care, leading to better results and happier patients.
FAQ
What is the success rate of AVM surgery?
The success rate of AVM surgery depends on several factors. These include the AVM’s size, location, and complexity. It also depends on the patient’s overall health. Generally, microsurgical resection has a high success rate. This is because most AVMs are completely removed in a significant number of cases.
How long is the recovery period after AVM surgery?
Recovery time after AVM surgery varies. It can range from several weeks to several months. The type of surgery, the AVM’s size and location, and the patient’s health all play a role.
What are the possible complications of AVM surgery?
Complications of AVM surgery include bleeding, infection, stroke, and neurological deficits. The risk of these complications depends on the AVM’s complexity, the surgical approach, and the patient’s health.
Can AVMs recur after surgery?
There is a small risk of AVM recurrence after surgery. This risk is higher if the AVM is not completely removed or if there are residual fragments. Long-term follow-up is necessary to monitor for recurrence.
What is the role of embolization in AVM treatment?
Embolization is a minimally invasive procedure. It reduces blood flow to the AVM by injecting materials that block or reduce flow. It is often used with other treatments, like surgery or radiosurgery, to enhance their effectiveness.
How does brainstem AVM surgery differ from other AVM surgeries?
Brainstem AVM surgery is more challenging. This is because the brainstem controls vital functions. The surgery requires careful planning and is often performed by specialized neurosurgeons.
What are the benefits of using advanced devices and technology in AVM treatment?
Advanced devices and technologies have improved AVM treatment. They include embolization materials, imaging and navigation systems, and radiosurgery equipment. These advancements make treatments safer and more effective, reducing complications and improving outcomes.
What can patients expect during the first 24-48 hours after AVM surgery?
In the first 24-48 hours after surgery, patients are closely monitored in the ICU. They are watched for signs of complications like bleeding or neurological changes. Pain management and supportive care are provided to ensure comfort and stability.
How do I prepare for AVM surgery?
Preparing for AVM surgery involves a thorough evaluation. This includes medical tests, medication adjustments, and mental and emotional preparation. Patients should follow their healthcare provider’s instructions carefully to prepare well for surgery and recovery.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC4422639/[3




































