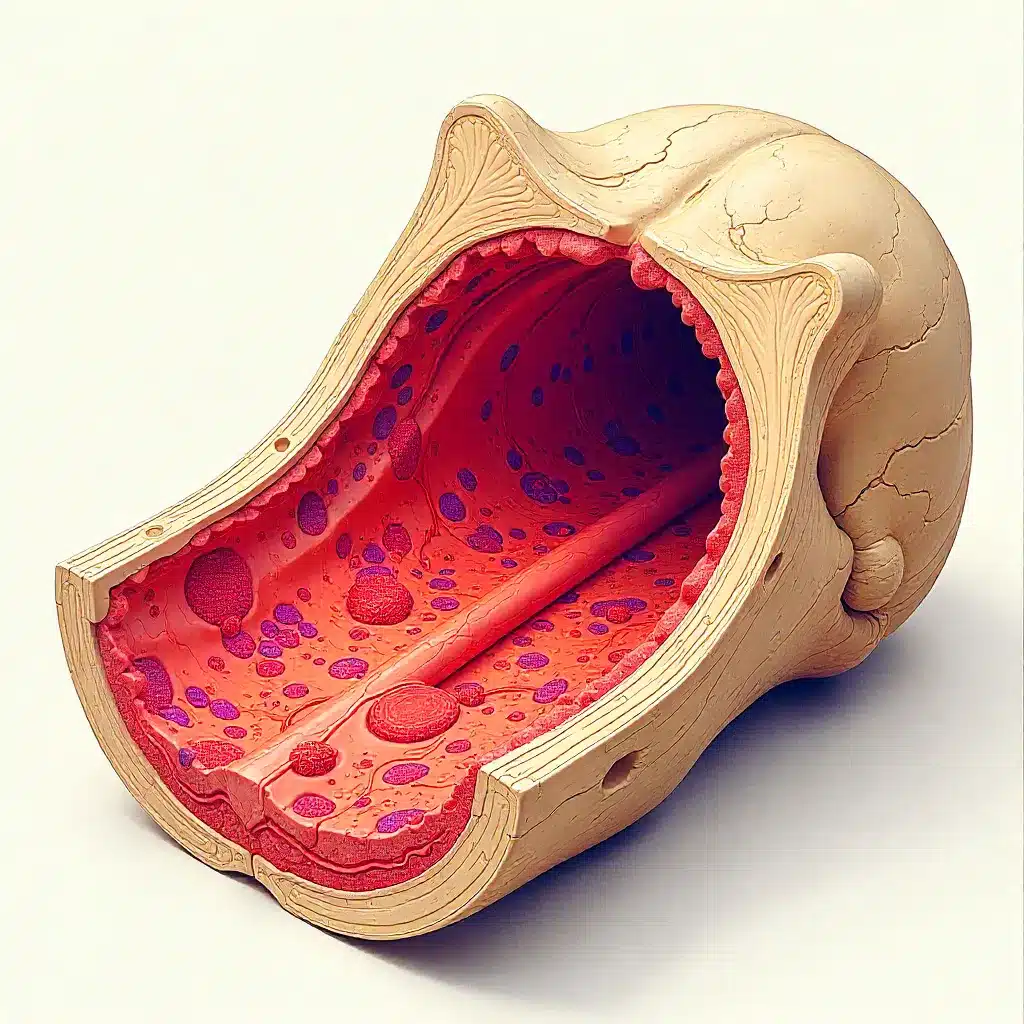
** Infiltrative marrow disorders affect thousands of people each year, occurring when abnormal cells invade the bone marrow.** This invasion disrupts the bone marrow’s ability to make blood. Diseases like multiple myeloma and myelodysplastic syndromes are examples.
These disorders are more common than you might think. For instance, multiple myeloma is found in about 1.8% of all cancers. It’s important to understand these conditions to find better treatments. At Liv Hospital, we aim to improve how we diagnose and manage these complex diseases.
Key Takeaways
- Infiltrative marrow disorders involve abnormal cells invading the bone marrow.
- Conditions like multiple myeloma and myelodysplastic syndromes are types of infiltrative marrow disorders.
- These disorders disrupt the normal blood-forming function of the bone marrow.
- Multiple myeloma accounts for approximately 1.8% of all cancers.
- Effective treatment strategies rely on a thorough understanding of these conditions.
The Structure and Function of Bone Marrow
It’s important to know how bone marrow works to understand blood cell production and health. Bone marrow is a key part of our body’s system for making blood.
Normal Bone Marrow Composition
Bone marrow has many cells, including those that make all blood cells. It also has a supportive part that helps blood cell production. The marrow has blood vessels and nerves for nutrients and signals.
|
Component |
Function |
|---|---|
|
Hematopoietic Stem Cells |
Give rise to all blood cells (red blood cells, white blood cells, platelets) |
|
Supportive Stroma |
Provides the microenvironment necessary for hematopoiesis |
|
Blood Vessels |
Supply nutrients and oxygen to the marrow |
|
Nerves |
Regulate marrow function through signaling |
Hematopoiesis: The Blood-Forming Process
Bone marrow makes blood cells through hematopoiesis. It starts with stem cells that turn into different blood cells. This process is controlled by growth factors and cytokines.
Hematopoiesis involves several key stages:
- Proliferation of hematopoietic stem cells
- Differentiation into lineage-specific progenitor cells
- Maturation into functional blood cells
- Release of mature blood cells into the circulation
Distribution of Bone Marrow Throughout the Body
Bone marrow is found in many parts of the body, like the vertebrae and pelvis. In kids, it’s mostly red marrow, which makes lots of blood cells. Adults have more yellow marrow, which is fat and less active.
The vertebrae have a lot of red marrow in adults too. This is important for making blood. Knowing where bone marrow is helps doctors diagnose and treat diseases.
Bone Marrow in Vertebrae: Anatomy and Significance
Understanding the anatomy of vertebral bone marrow is key to knowing its importance. It’s a vital part of the hematopoietic system. It plays a big role in making blood cells.
Unique Features of Vertebral Bone Marrow
The bone marrow in our vertebrae has unique features that set it apart. It’s full of blood vessels, which help with nutrient and waste exchange. This is important for the high metabolic activity needed for blood cell production.
Some key aspects of vertebral bone marrow include:
- High cellularity, with a predominance of hematopoietic cells
- A rich vascular supply, supporting the metabolic demands of hematopoiesis
- A complex microenvironment that supports the development of various blood cell lineages
Red vs. Yellow Marrow Distribution in the Spine
The spine has both red and yellow marrow. Red marrow makes blood cells, while yellow marrow is mostly fat. It acts as a backup for red marrow.
In adults, red and yellow marrow are spread differently in the spine. Red marrow is found more in the:
- Vertebral bodies
- Pelvis
- Ribs
- Sternum
This pattern is important because it affects where marrow disorders might show up in the spine.
Clinical Importance of Vertebral Marrow Health
Keeping vertebral bone marrow healthy is vital for our well-being. The health of vertebral marrow is very important. It’s linked to our body’s ability to make blood cells. Problems with the marrow can cause anemia, infections, and bleeding issues.
Some key factors that highlight the clinical importance of vertebral marrow health include:
- The role of vertebral marrow in hematopoiesis
- The impact of marrow infiltration disorders on vertebral health
- The possible effects of vertebral marrow disorders on our quality of life
Defining Infiltrative Marrow Disorders
“Infiltrative marrow disorder” means diseases where bad cells get into the bone marrow. This messes up how it works. We’ll look at what these disorders are, the kinds of bad cells involved, and how they affect the bone marrow.
Abnormal Cell Invasion of Bone Marrow
Bad cells getting into the bone marrow is a big problem. It can happen because of cancers or other diseases. This can mess up the marrow’s job of making blood cells.
When bad cells get into the marrow, it can cause big issues. These include anemia, infections, and bleeding disorders. Knowing how this happens helps doctors find better ways to treat it.
Disruption of Normal Blood-Forming Function
The bone marrow makes blood cells like red and white blood cells, and platelets. But when bad cells get in, they can stop this from happening. This means fewer healthy blood cells are made.
This can lead to fatigue, more infections, and easy bruising. How bad these symptoms are depends on how much of the marrow is affected and what kind of bad cells are there.
Categories of Infiltrating Cells
Infiltrative marrow disorders are grouped by the type of cells that get into the marrow. The main groups are:
- Cancerous cells, like those in leukemia, lymphoma, and multiple myeloma.
- Non-cancerous cells, found in storage disorders or inflammatory conditions.
Knowing which kind of cells are in the marrow is key. It helps doctors figure out the best treatment and what to expect for the patient.
Epidemiology and Statistics of Infiltrative Marrow Disorders
It’s key to know about the spread of infiltrative marrow disorders. This knowledge helps in making better health plans and improving care for patients. These diseases, like multiple myeloma and myelodysplastic syndromes, affect health systems worldwide.
Prevalence of Multiple Myeloma
Multiple myeloma is a rare but serious cancer, making up about 1.8% of all cancers. It’s more common in developed countries. As people live longer and diagnosis gets better, we expect more cases.
Myelodysplastic Syndromes Statistics
Myelodysplastic syndromes (MDS) hit 4-5 individuals per 100,000 each year. It’s more common in older folks, and its numbers go up with age. For more on MDS, check out on it.
Age and Demographic Distribution
The age and who gets these diseases show important patterns. Most cases of multiple myeloma and MDS happen in people over 65. The numbers also vary by race and ethnicity.
Key trends include:
- More cases with age
- Different rates in different groups
- More common in rich countries
Knowing these facts is vital for health planning, setting up resources, and creating specific treatments.
Pathophysiology of Marrow Infiltration
Marrow infiltration is a complex process. It involves many cellular mechanisms and changes in the marrow environment. Disorders like this happen when abnormal cells invade the bone marrow. This invasion disrupts normal blood cell production.
Cellular Mechanisms of Infiltration
Abnormal cells entering the bone marrow is a complex process. These cells can push out normal blood cells, causing low counts. These cells can come from blood cancers or other cancers that spread.
Research shows that changes in cell adhesion and the marrow environment play a big role. For example, in multiple myeloma, cancer cells stick to marrow cells, helping them grow.
Microenvironmental Changes
The bone marrow environment is key in marrow infiltration. When abnormal cells invade, the environment changes. This can include more blood vessels, fibrosis, and changes in cytokines. These changes help the abnormal cells grow and survive.
In myelodysplastic syndromes, the marrow environment gets messed up. This leads to poor blood cell production. Knowing about these changes helps us find better treatments.
Impact on Normal Marrow Function
Marrow infiltration affects normal marrow function a lot. It can cause anemia, low platelets, and low white blood cells. It can also cause bone pain and fractures.
|
Condition |
Effect on Marrow Function |
Clinical Manifestations |
|---|---|---|
|
Multiple Myeloma |
Displacement of normal hematopoietic cells |
Anemia, bone pain, hypercalcemia |
|
Myelodysplastic Syndromes |
Ineffective hematopoiesis |
Cytopenias, risk of progression to AML |
|
Metastatic Cancer |
Replacement of marrow with malignant cells |
Bone pain, pathological fractures |
Understanding marrow infiltration is key to treating related disorders. By studying how it works, we can find better treatments. This helps improve patient outcomes.
Multiple Myeloma: A Primary Infiltrative Disorder
Multiple myeloma greatly affects the bone marrow’s structure and function. We’ll look at how it changes the marrow on MRI, the non-secretory variant, and the problems it causes in the spine.
Patterns of Marrow Infiltration on MRI
Multiple myeloma shows different ways of marrow infiltration on MRI. These can be diffuse, focal, or a mix of both. Knowing these patterns helps doctors diagnose and stage the disease.
Using MRI to check marrow infiltration is key in managing multiple myeloma. It spots early changes and tracks how well treatments work.
Non-Secretory Variant Characteristics
The non-secretory variant of multiple myeloma doesn’t produce detectable proteins in the blood or urine. Yet, it can cause a lot of bone marrow problems and complications.
Diagnosing this variant is tricky. It mainly relies on imaging and bone marrow biopsies. Knowing its traits is vital for the right treatment.
Vertebral Involvement and Complications
Multiple myeloma often affects the spine, leading to fractures and spinal cord compression. This can really hurt your quality of life, causing pain and making it hard to move.
Dealing with spine problems needs a team effort. This includes surgery, radiation, and medicine to fix the spine and ease symptoms.
Myelodysplastic Syndromes and Bone Marrow Infiltration
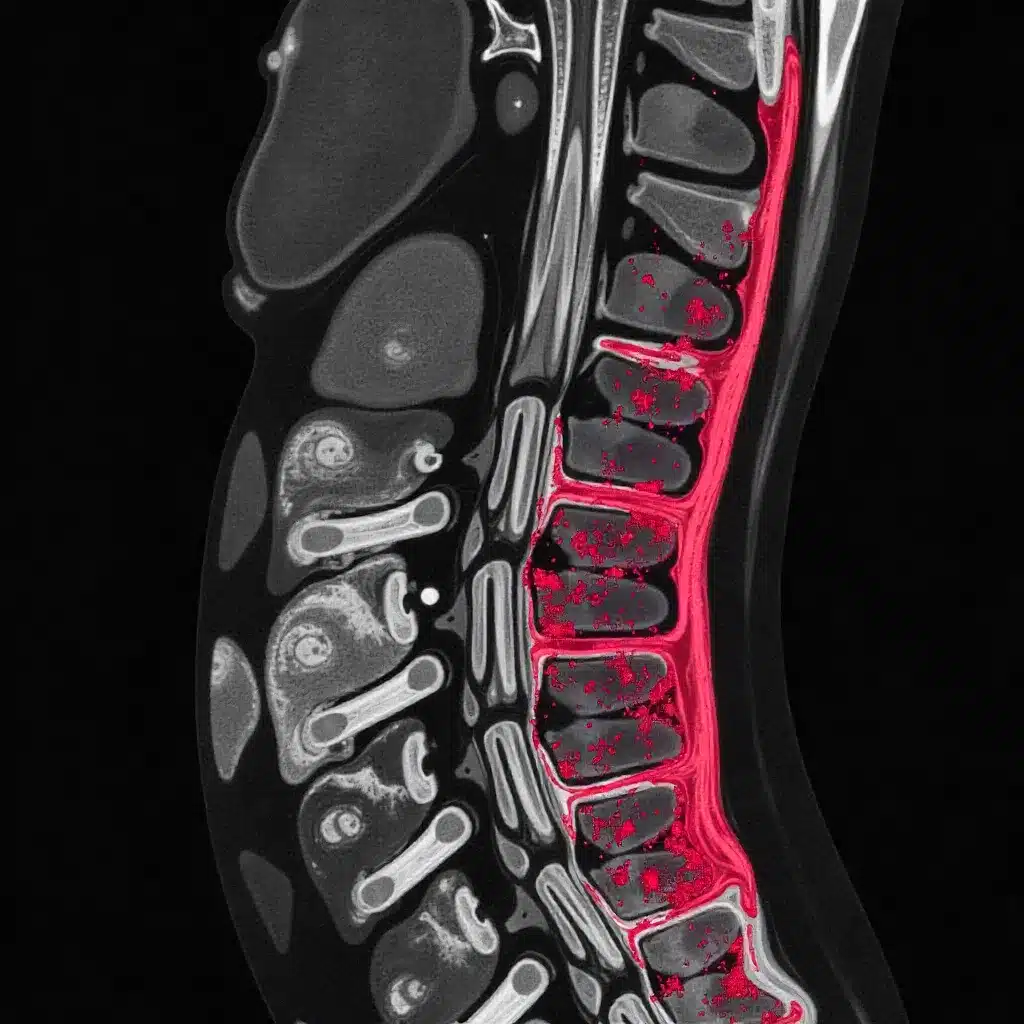
Myelodysplastic syndromes (MDS) are complex disorders. They happen when the bone marrow can’t make blood cells right because of abnormal cells. These syndromes are caused by clonal hematopoiesis, where the bone marrow makes bad cells that don’t grow right. This leads to low blood counts.
Abnormal Cell Infiltration Patterns
In MDS, the bone marrow gets filled with bad cells. This messes up the marrow’s normal work. It can cause many problems, like:
- Impaired erythropoiesis, leading to anemia
- Thrombocytopenia from bad megakaryopoiesis
- Neutropenia, making infections more likely
The way these bad cells spread can change with different MDS types. This affects how the disease shows up and how it might progress.
Predominance in Older Adults
MDS mostly hits older people, with more cases after 60. People usually get diagnosed around 70. Why it’s more common in older folks includes:
- Genetic changes that build up over time
- Effects of environmental and treatment mutagens
- Changes in the bone marrow with age
Knowing these reasons helps find MDS early in older adults.
Progression and Risk Stratification
MDS can turn into acute myeloid leukemia (AML) at different rates. It’s key to figure out the risk to plan treatment. The Revised International Prognostic Scoring System (IPSS-R) helps by looking at:
- Cytogenetic abnormalities
- Blast percentage in the bone marrow
- How bad the blood counts are
This system sorts patients by risk. Doctors can then choose the best treatment for each person. This makes care better and life quality higher.
Other Malignant Infiltrative Disorders of Bone Marrow
The bone marrow can be affected by many cancers, not just multiple myeloma. Leukemias and lymphomas are examples. These cancers harm the marrow’s function, causing health problems.
Leukemias: Acute and Chronic Forms
Leukemias are cancers of blood cells in the bone marrow. Acute leukemias start quickly and need fast treatment. Chronic leukemias grow slower but can also cause problems.
These cancers can make the marrow fail. This failure leads to anemia, infections, and bleeding issues.
We will look at acute myeloid leukemia (AML) and chronic lymphocytic leukemia (CLL). We’ll see how each type affects people differently.
Lymphomas with Marrow Involvement
Lymphomas are cancers of the lymphatic system that can spread to the bone marrow. Hodgkin lymphoma and non-Hodgkin lymphoma (NHL) are the main types, with NHL being more common. When lymphoma affects the marrow, it can cause low blood counts and other symptoms.
Lymphoma in the marrow makes it harder to plan treatment. We’ll talk about how this affects treatment plans for lymphoma patients.
Metastatic Cancer to Vertebral Bone Marrow
Metastatic cancer in the spine is common in cancers like breast, prostate, and lung. It can cause spine fractures, spinal cord issues, and a lot of pain.
We’ll cover how cancer spreads to the spine and its effects. We’ll also discuss how to diagnose and treat it.
Non-Malignant Causes of Marrow Infiltration
Non-malignant causes of marrow infiltration are many and can affect bone marrow function a lot. These conditions can cause different symptoms, making it hard to diagnose and treat them.
Storage Disorders Affecting Marrow
Storage disorders are conditions where certain substances build up in cells, causing marrow infiltration. Gaucher disease and Niemann-Pick disease are examples.
Gaucher disease happens when the body can’t break down glucocerebroside. This leads to anemia, low platelets, and bone pain.
|
Disease |
Deficient Enzyme |
Accumulated Substance |
Clinical Features |
|---|---|---|---|
|
Gaucher Disease |
Glucocerebrosidase |
Glucocerebroside |
Anemia, thrombocytopenia, bone pain |
|
Niemann-Pick Disease |
Sphingomyelinase |
Sphingomyelin |
Hepatosplenomegaly, neurological deterioration |
Inflammatory and Granulomatous Conditions
Inflammatory and granulomatous conditions, like sarcoidosis, can also cause marrow infiltration. Sarcoidosis forms non-caseating granulomas in organs, including the bone marrow.
Granulomas in the bone marrow can cause low blood counts and other blood problems. A bone marrow biopsy is often needed for diagnosis.
Histiocytic Disorders
Histiocytic disorders, including Langerhans cell histiocytosis, are another type of non-malignant marrow infiltration. These conditions involve the growth of histiocytes in tissues, including the bone marrow.
Langerhans cell histiocytosis can show up in different ways, from single bone lesions to affecting many organs. Doctors diagnose it by looking at tissue samples.
We’ve talked about different non-malignant causes of marrow infiltration. Each has its own signs and effects. Knowing about these conditions helps doctors make the right diagnosis and treatment plan.
Clinical Manifestations of Infiltrative Marrow Disorders
It’s key to know the signs of infiltrative marrow disorders early. This helps in quick diagnosis and treatment. These disorders cause symptoms because abnormal cells fill the bone marrow.
Anemia and Other Cytopenias
Anemia is a main symptom of these disorders. It happens when abnormal cells replace normal blood-making cells. This leads to fewer red blood cells, causing anemia. Other blood cell shortages, like neutropenia and thrombocytopenia, can also happen.
|
Cytopenia |
Causes |
Clinical Impact |
|---|---|---|
|
Anemia |
Reduced red blood cell production |
Fatigue, weakness |
|
Neutropenia |
Decreased neutrophil count |
Increased infection risk |
|
Thrombocytopenia |
Low platelet count |
Bleeding, bruising |
Bone Pain and Vertebral Complications
Bone pain is a common symptom. It comes from cancer cells in the bone marrow causing bone damage. This can lead to vertebral problems.
Vertebral fractures can weaken the spine. This might cause spinal cord issues and nerve problems.
The symptoms can vary based on where and how much the spine is affected. Back pain can be severe and really hurt.
Other Clinical Features
Patients with these disorders may also lose weight, feel very tired, and get infections easily. These symptoms can really affect their life quality. They need a full treatment plan.
It’s vital to spot these signs early. This way, we can give the best care to those with infiltrative marrow disorders.
Diagnostic Approaches to Infiltrative Disorders in Vertebral Bone Marrow
Getting a correct diagnosis for infiltrative disorders in vertebral bone marrow is key. We use different methods to check these conditions fully.
Laboratory Evaluation and Blood Tests
Laboratory tests are very important for diagnosing these disorders. We do a complete blood count (CBC) to look for signs like anemia or low blood cells. Tests like serum protein electrophoresis (SPEP) and urine protein electrophoresis (UPEP) help find proteins linked to diseases like multiple myeloma.
We also check for inflammation by looking at markers like erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP). These markers can show if there’s inflammation or infection.
Bone Marrow Aspiration and Biopsy Techniques
Bone marrow aspiration and biopsy are key for diagnosing these disorders. These methods let us see the bone marrow’s cells and structure up close. We do these under local anesthesia and use imaging if needed for accurate samples.
The aspirate gives us info on the marrow’s cell count and shape. The biopsy sample gives a detailed look at the marrow’s structure and any diseases.
Vertebral Biopsy: Indications and Procedures
Vertebral biopsy is needed when we need to take a sample from the vertebral bone marrow. This is often when imaging shows a specific lesion or when other tests don’t give clear results. We use CT or fluoroscopy for precise targeting of the area.
Choosing to do a vertebral biopsy depends on many things. These include the patient’s health, the suspected disease, and the risks and benefits of the procedure.
Advanced Imaging of Bone Marrow in Vertebrae
Advanced imaging has changed how we look at bone marrow in vertebrae. It gives us new insights into diseases. This helps doctors diagnose and track conditions better, leading to better care for patients.
MRI Patterns in Infiltrative Disorders
Magnetic Resonance Imaging (MRI) is key in checking bone marrow. It shows the marrow’s details and spots disease patterns. For example, it can see changes in marrow that might mean disease.
MRI patterns show different signs of disease. You might see changes in marrow signal. These can mean things like multiple myeloma or cancer spread. New MRI methods like DWI and DCE-MRI give even more info. They show how cells and blood vessels are in the marrow.
PET-CT Evaluation of Marrow Involvement
Positron Emission Tomography-Computed Tomography (PET-CT) is also vital for checking bone marrow. It mixes PET’s function info with CT’s body details. This gives a full view of the disease.
PET-CT is great for seeing how active marrow lesions are. This helps figure out how serious the disease is and if treatment is working. For example, in multiple myeloma, it spots active disease and tracks how treatment changes it.
Emerging Imaging Modalities
New imaging methods are being looked at for better bone marrow checks. Emerging imaging modalities like PET-MRI are promising. They mix PET and MRI strengths for detailed info.
New tech like advanced diffusion-weighted imaging and special PET tracers might be even better. They could spot and understand marrow diseases better. As these techs get better, they’ll help more in diagnosing and treating marrow diseases.
Treatment Strategies for Infiltrative Marrow Disorders
Managing infiltrative marrow disorders needs a detailed plan. It’s based on the condition, how much marrow is affected, and the patient’s health. Understanding these factors is key to effective treatment.
Disease-Specific Therapeutic Approaches
Different diseases need different treatments. For example, multiple myeloma might use targeted drugs. On the other hand, myelodysplastic syndromes could be treated with specific medications based on the type and risk.
We make treatment plans for each patient. We consider their age, health, and the details of their disease. This approach helps improve their quality of life.
Managing Cytopenias and Supportive Care
Dealing with cytopenias is vital in caring for these patients. Anemia, neutropenia, and thrombocytopenia can greatly affect their well-being. We use transfusions, growth factors, and other methods to manage these issues.
- Red blood cell transfusions to alleviate anemia
- Granulocyte-colony stimulating factor (G-CSF) to address neutropenia
- Platelet transfusions to manage thrombocytopenia
Supportive care also includes pain management, preventing infections, and nutritional support. These efforts aim to improve the patient’s quality of life.
Novel Therapies and Clinical Trials
New treatments and clinical trials are changing the game for these disorders. Novel therapies like immunotherapies and targeted treatments are showing promise. They target specific weaknesses in cancer cells.
We work hard to give our patients access to the newest treatments and trials. This way, they can benefit from the latest research and advancements.
Liv Hospital’s Approach to Infiltrative Marrow Disorders
Liv Hospital’s hematology department leads in managing infiltrative marrow disorders. We use new diagnostic and treatment methods. Our team works hard to give full care to patients with these conditions.
Latest Diagnostic Protocols
We use the newest ways to find and understand infiltrative marrow disorders at Liv Hospital. Our top-notch facilities and skilled hematopathologists help us make accurate diagnoses. We use advanced bone marrow tests and imaging like MRI and PET-CT scans.
Advanced Diagnostic Techniques:
- High-resolution MRI for detailed marrow assessment
- PET-CT scans for evaluating metabolic activity
- Molecular diagnostics for identifying specific genetic markers
Advanced Therapeutic Options
We tailor treatments to each patient’s needs at Liv Hospital. Our therapies include new methods like CAR-T cell therapy and clinical trials. We also offer traditional treatments like chemotherapy and targeted therapy.
Personalized Treatment Plans: We focus on personalized care. We make sure each patient’s treatment fits their unique situation and health.
Commitment to International Treatment Standards
Liv Hospital follows international standards for treating infiltrative marrow disorders. We do this by working with global experts and joining clinical trials. We also keep our treatment plans up to date with the latest research.
By combining the newest treatments and care with a focus on the patient, Liv Hospital offers top care for those with infiltrative marrow disorders. We aim for the best results for our patients.
Prognosis and Long-term Outcomes
The outlook for infiltrative marrow disorders depends on several key factors. These include the type of disorder, how much marrow is involved, and the patient’s health.
Prognostic Factors and Risk Stratification
Prognostic factors are vital in predicting long-term outcomes for patients with these disorders. They include the disease type, genetic mutations, and how well the patient responds to treatment. We use risk stratification systems to match treatments to each patient’s needs.
Key prognostic factors are the disease’s severity, the patient’s age, and their health. For example, some genetic mutations can worsen the prognosis. But, a strong response to treatment can greatly improve outcomes.
Monitoring Disease Progression
It’s important to regularly check how the disease is progressing. We use blood tests, bone marrow biopsies, and imaging to track changes. This helps us see if the disease is getting worse or if treatment is working.
By watching the disease closely, we can catch any signs of relapse or treatment failure early. This allows us to make changes to the treatment plan quickly. This approach helps improve patient outcomes and quality of life.
Quality of Life Considerations
Keeping the patient’s quality of life in mind is key when managing these disorders. We focus on treating the disease and helping with physical and emotional challenges.
Supportive care like pain management, nutrition support, and counseling is a big part of our care. By taking care of the whole patient, we aim to improve their well-being and strength during treatment.
In summary, understanding the prognosis and long-term outcomes of infiltrative marrow disorders requires a detailed approach. We consider many factors, monitor the disease, and focus on quality of life. This strategy helps us provide personalized care that improves patient outcomes and enhances their quality of life.
Conclusion: Advances in Understanding and Managing Infiltrative Marrow Disorders
We’ve looked into the complex world of infiltrative marrow disorders. We’ve seen how new ways to manage these conditions have changed patient care. In recent years, there’s been a big leap forward in diagnosing and treating these diseases.
New imaging tools like MRI and PET-CT help doctors see how far the disease has spread. This is key for creating the best treatment plans. Also, new treatments have given patients more options for managing their conditions.
At Liv Hospital, we’re all about top-notch healthcare for international patients. Our team works with each patient to offer care that fits their needs. We use the latest in diagnosis and treatment. As research finds more about these disorders, we’re ready to keep improving care and life quality for our patients.
FAQ
What is an infiltrative marrow disorder?
An infiltrative marrow disorder happens when abnormal cells invade the bone marrow. This invasion disrupts the marrow’s ability to make blood.
What is the role of bone marrow in the body?
Bone marrow is key for making blood cells. It produces red blood cells, white blood cells, and platelets through a process called hematopoiesis.
How is bone marrow distributed throughout the body?
Bone marrow is found throughout the body, including in vertebrae. It’s essential for healthy blood cell production.
What is the significance of vertebral bone marrow?
Vertebral bone marrow is a big part of the hematopoietic system. Its health is vital for overall well-being.
What are the types of infiltrating cells in infiltrative marrow disorders?
Infiltrating cells can be malignant, like in multiple myeloma, leukemia, and lymphoma. They can also be non-malignant, linked to storage disorders and inflammation.
How is multiple myeloma diagnosed?
Doctors use lab tests, bone marrow biopsies, and imaging like MRI and PET-CT to diagnose multiple myeloma.
What are the treatment options for infiltrative marrow disorders?
Treatment depends on the disorder. It may include specific therapies, managing blood issues, and supportive care. New treatments and trials are also options.
How does Liv Hospital approach the treatment of infiltrative marrow disorders?
Liv Hospital uses the latest diagnostic methods and offers advanced treatments. They follow international standards for patient care.
What is the prognosis for patients with infiltrative marrow disorders?
Prognosis varies by disorder and patient factors. It’s influenced by treatment success and overall health.
How can the quality of life be maintained for patients with infiltrative marrow disorders?
Quality of life is maintained by managing symptoms, tracking disease, and providing supportive care. Care is tailored to the patient’s needs.
What is the importance of advanced imaging in diagnosing infiltrative marrow disorders?
MRI and PET-CT are key for diagnosing and monitoring. They show how much marrow is involved.
What is the role of bone marrow biopsy in diagnosing infiltrative marrow disorders?
Bone marrow biopsy is vital for diagnosis. It examines bone marrow cells and environment to assess disorder presence and extent.
References
- Costachescu, D., & Ioniță, H. (2022). The importance of bone marrow infiltration patterns in multiple myeloma seen on magnetic resonance imaging: Case report and imaging perspective. Clinical Case Reports, 10(10), e6452. https://doi.org/10.1002/ccr3.6452 PubMed+1
- Bejar, D., Colombo, P. C., Latif, F., & Yuzefpolskaya, M. (2015). Infiltrative cardiomyopathies. Clinical Medicine Insights: Cardiology, 9(Suppl 2), 29–38. https://doi.org/10.4137/CMC.S19706 PubMed Central+1
- University of California, San Francisco. (n.d.). Myelodysplastic syndromes (MDS) – Conditions. Retrieved from https://www.ucsfhealth.org/conditions/myelodysplastic-syndromes UCSF Health
- National Toxicology Program, NIH. (n.d.). Atlas of cellular infiltration: Hematopoietic system – bone marrow infiltration (cellular/histiocyte). Retrieved from https://ntp.niehs.nih.gov/atlas/nnl/hematopoietic-system/bone-marrow/InfiltrationCellularHistiocyte PubMed Central
- National Cancer Institute. (n.d.). Multiple myeloma – cancer types. Retrieved from https://www.cancer.gov/types/myeloma PubMed Central
- Ma, X., Does, M., Raza, A., & Mayne, S. T. (2012). Epidemiology of myelodysplastic syndromes. The American Journal of Medicine, 125(7 Suppl), S2–S5. https://doi.org/10.1016/j.amjmed.2012.04.014



































