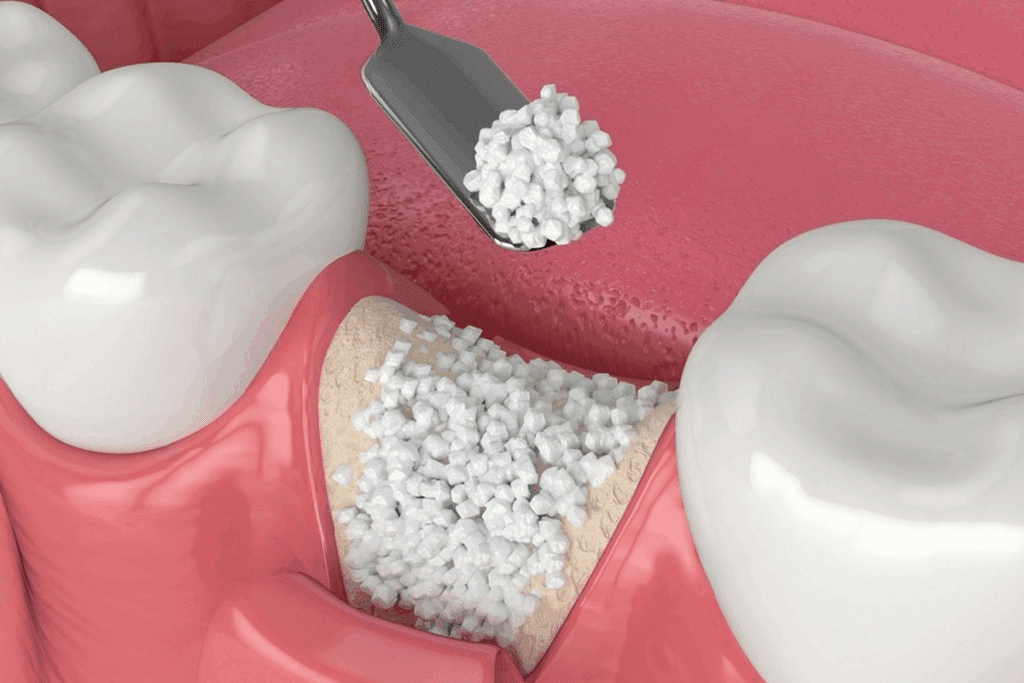
When bones are damaged by trauma, infections, tumors, or diseases, fixing them is key. Cadaver bone grafts are a top choice for fixing bones. They have changed how doctors do orthopedic and reconstructive surgery.
Johns Hopkins Medicine says bone grafting is a surgery that uses bone from another person to fix bones. Every year, 2.2 million surgeries use bone grafting. Knowing about cadaver bone grafts is very important.
We will look at how cadaver bone grafts help fix bones. We’ll talk about how they are made, the different types, and how they are used in medicine. This will give you a deep look into using cadaver bone grafts for bone repair.
Explaining the procedure and effectiveness of using a cadaver Bone transplant (allograft) for reconstruction.
Key Takeaways
- Cadaver bone grafts are a key procedure for fixing bone problems.
- Bone grafting is a surgery that uses bone to fix damaged bones.
- Cadaver bone grafts offer custom solutions for patients.
- They have greatly improved orthopedic and reconstructive surgery.
- It’s important to understand cadaver bone grafts for fixing bone issues.
Understanding Cadaver Bone Grafts
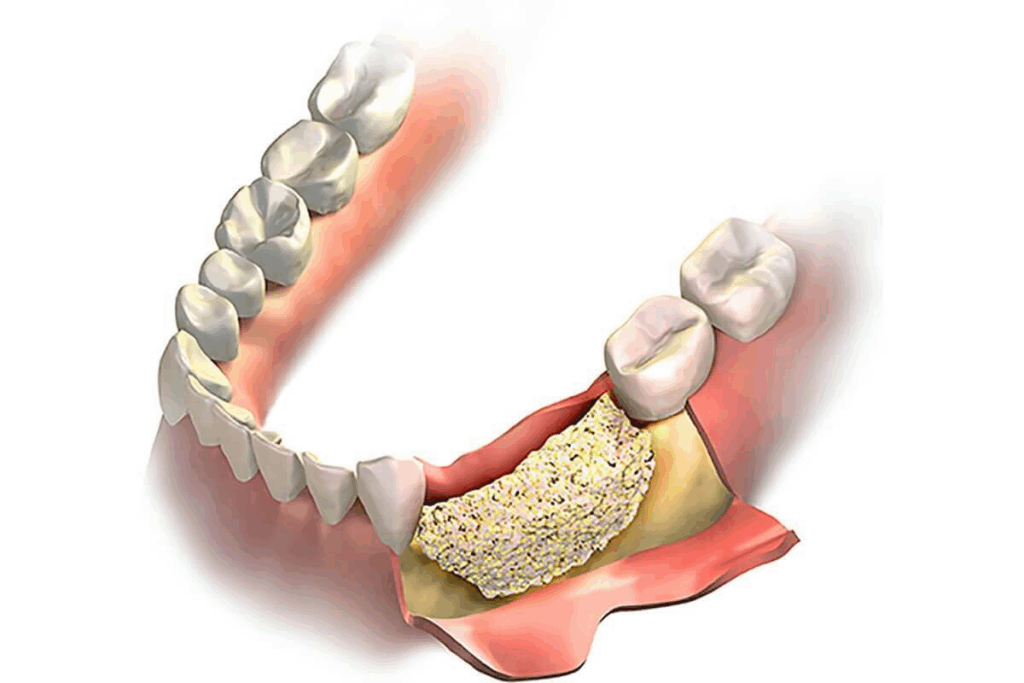
Cadaver bone grafts play a big role in today’s orthopedic and dental fields. They come from living donors or people who have passed away. These grafts are processed to lower the chance of immune reactions and disease spread.
Definition and Classification of Allografts
Cadaver bone grafts, or allografts, are bone taken from one person and given to another. They are sorted by how they are processed. The main types are fresh-frozen, freeze-dried, and demineralized bone matrix (DBM).
Knowing how allografts are classified helps figure out if they’re right for certain surgeries. For example, fresh-frozen grafts keep their strength and are used for big bone grafts. Freeze-dried grafts are more flexible and can be used in many ways.
| Type of Allograft | Processing Method | Common Applications |
|---|---|---|
| Fresh-Frozen | Stored at very low temperatures | Structural bone grafting, trauma reconstruction |
| Freeze-Dried | Freeze-drying to remove moisture | Various bone grafting procedures, including spinal fusion |
| Demineralized Bone Matrix (DBM) | Demineralization to expose growth factors | Bone regeneration, spinal fusion, and tumor resection defects |
Sources of Cadaver Bone Material
Cadaver bone comes from living donors and those who have passed away. The process of getting this bone is very careful. Donors are checked for health issues and diseases to make sure the bone is safe.
Using cadaver bone grafts is getting more common. This is because they are easy to get and don’t hurt the donor. With more dental implants, the need for bone grafts is growing. Cadaver bone grafts are key in these surgeries.
The Science Behind Bone Transplant Procedures
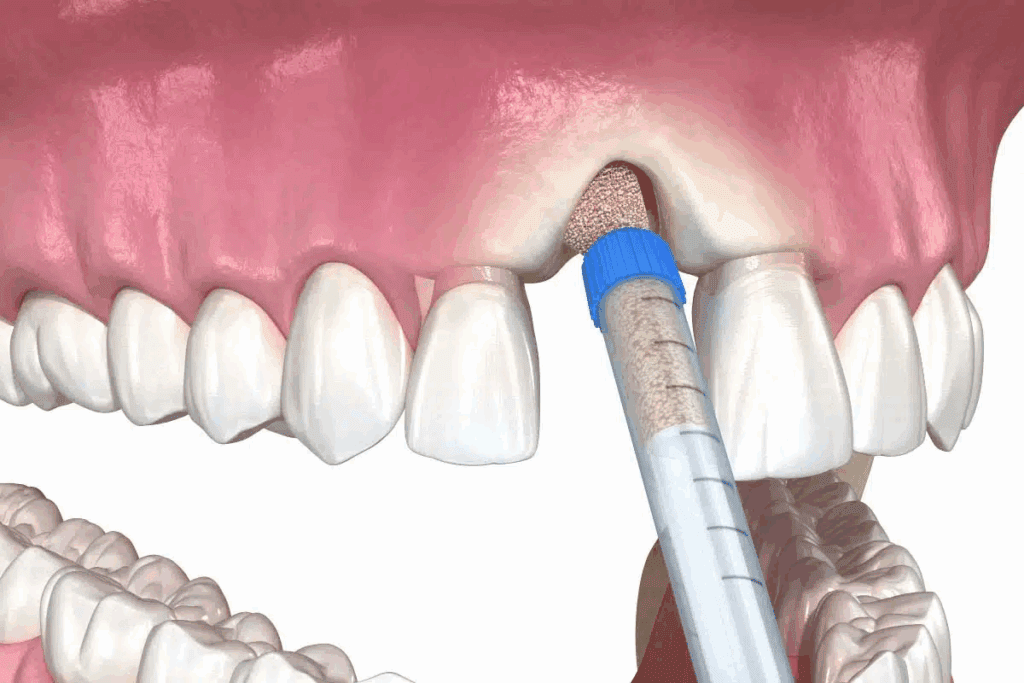
Bone grafting is key in orthopedic and dental surgery. It relies on understanding how bones heal and grow. We’ll look at the science behind bone transplantation, including how bones heal and grow back.
Osteoinduction, Osteoconduction, and Osteogenesis
Three main processes are vital for bone graft success: osteoinduction, osteoconduction, and osteogenesis. Osteoinduction means the graft can start bone cell growth. Osteoconduction is when the graft helps new bone grow by providing a structure. Osteogenesis happens when the graft has living cells that create new bone.
Cadaver bone grafts work through these processes too. They don’t have living cells but can help new bone grow. The way they’re processed makes them fit perfectly for different needs, helping them support bone growth.
Integration Process of Cadaver Grafts
Integrating cadaver grafts into the host bone is complex. It involves inflammation, bone breakdown, and new bone growth. The graft acts as a base for new tissue to grow into.
How well the graft integrates depends on several things. These include how it’s processed, its size and shape, and the blood flow in the area. Proper care and handling of the graft are key for successful integration.
Current Statistics and Future Projections
Bone grafting is a common surgery, with 2.2 million done worldwide each year. This number is expected to grow by 13% every year. This is because more people are getting older and needing orthopedic care.
As bone grafting advances, we can expect better results and more uses for it. New technologies and materials will likely be big parts of this progress.
Types of Cadaver Bone Grafts Available
Cadaver bone grafts come in many forms to meet different needs. This variety helps surgeons pick the best graft for each patient. It boosts the chances of a successful surgery.
Structural Allografts
Structural allografts are needed for big bone repairs. They’re great for fixing bones damaged by accidents, tumors, or other issues. They give bones the support they need right away, helping patients move and heal faster.
Demineralized Bone Matrix (DBM)
Demineralized Bone Matrix (DBM) comes from cadaver bones and works well for spinal fusions. It has growth factors that help bones grow. DBM is perfect for helping bones heal in many orthopedic and dental cases.
Morselized and Cancellous Chips
Morselized and cancellous chips fill in bone gaps. They’re made from small pieces of cancellous bone. They help new bone grow and are good for many surgeries.
Customized Grafts for Specific Applications
New tech lets surgeons make custom bone grafts for each patient. These grafts fit exactly where they’re needed. This personal touch can lead to better results by fitting better and healing faster.
In summary, the wide range of cadaver bone grafts means surgeons can tailor treatments for each patient. Knowing about these grafts helps surgeons make the best choices for their patients.
Processing and Preparation Methods
The steps to prepare cadaver bone grafts are key to their safety and success. These steps aim to reduce disease risks and immune reactions. They also keep the graft’s structure and biological functions intact.
Deep Freezing Techniques
Deep freezing is a common way to keep cadaver bone grafts safe. It cools the graft to very low temperatures. This stops biological activity, lowering disease and rejection risks.
Deep freezing also keeps the graft’s structure strong. This makes it good for many orthopedic and dental uses.
Freeze-Drying Protocols
Freeze-drying, or lyophilization, is another important step. It freezes the graft and then removes water vapor. Freeze-drying lets grafts be stored for a long time without needing constant cold.
This makes it easier to share and use grafts in surgeries.
Sterilization and Disease Prevention Measures
Sterilization is critical to stop diseases from spreading. Different methods like gamma irradiation and ethylene oxide are used. These methods kill germs without harming the graft’s properties.
Good sterilization is key to graft safety for use in surgeries.
Using these advanced methods improves the safety and success of cadaver bone grafts. This leads to better results for patients in bone repair surgeries.
Patient Selection and Evaluation
Choosing the right patients for cadaver bone grafts is key to success in reconstructive surgery. We need to check each patient’s health to see if cadaver bone grafting is right for them.
Indications for Cadaver Bone Grafting
Cadaver bone grafting helps those with bone loss from trauma, infections, or tumors. It’s also used in orthopedic and dental surgeries where bone needs to be rebuilt. We decide on cadaver bone grafts based on the patient’s health, bone loss, and how well the graft might work.
Common indications include:
- Trauma-induced bone loss
- Tumor resections
- Infections leading to bone damage
- Congenital bone defects
Contraindications and Risk Factors
While cadaver bone grafting is helpful, there are some things to watch out for. Active infections, poor blood flow at the graft site, and health issues like diabetes or smoking are concerns.
Key risk factors involve:
- Active infection at the graft site
- Poor blood supply
- Systemic diseases (e.g., diabetes)
- Lifestyle factors (e.g., smoking)
Pre-Operative Assessment Protocols
Before surgery, a detailed check-up is vital to spot risks and boost graft success. This includes looking at the patient’s medical history, doing a physical exam, and using imaging to see the bone defect and tissue around it.
Pre-operative assessment involves:
- Detailed medical history
- Physical examination
- Imaging studies (X-rays, CT scans, MRI)
- Laboratory tests to assess overall health
By carefully picking patients for cadaver bone grafting, we can make these surgeries more successful. This leads to better results for our patients.
Pre-Surgical Planning for Successful Reconstruction
Effective pre-surgical planning is key for bone reconstruction success. It involves advanced imaging, choosing the right graft, and picking the best surgical method.
Imaging Requirements and Measurements
CT scans and MRI are vital for planning. They give detailed info on defect size, bone quality, and tissue anatomy. Accurate measurements help pick the right graft size and type, ensuring a smooth integration and fewer complications.
A leading orthopedic surgeon says, “Preoperative imaging is not just about seeing the defect. It’s about understanding the patient’s anatomy and planning with precision.” This shows how important imaging is for good results.
Graft Selection and Sizing
The right graft depends on several things. These include defect size, location, patient age, and health. We look at options like structural allografts, demineralized bone matrix, and morselized cancellous chips to find the best fit for each case.
- Structural allografts for large defects or when significant structural support is needed
- Demineralized bone matrix for promoting osteoinduction
- Morselized cancellous chips for filling small defects or augmenting other grafts
Surgical Approach Determination
Choosing the surgical approach is a big step in planning. We look at the defect’s location, graft type, and patient anatomy. A well-planned approach reduces tissue trauma and speeds up recovery.
“The key to a successful bone grafting procedure lies in meticulous pre-surgical planning, including the selection of the appropriate surgical approach.”
By planning the surgical approach carefully, we ensure the graft is placed right. This gives the patient the best possible outcome.
Step-by-Step Surgical Technique
Using cadaver grafts for bone reconstruction needs a precise surgical method. The steps include preparing the patient and fixing the graft in place.
Anesthesia and Patient Positioning
The first step is to give the right anesthesia for comfort and less pain. We then position the patient for the best access to the area.
Recipient Site Preparation
Preparing the site for the graft is key. We clean and remove any bad tissue to make it ready for the graft.
Graft Preparation and Customization
Next, we shape the graft to fit the patient’s needs. It’s done in a clean area to avoid infection.
Placement and Fixation Methods
After preparing, we place the graft carefully. We use plates, screws, or other devices to keep it stable and help it integrate.
| Surgical Step | Description | Key Considerations |
|---|---|---|
| Anesthesia and Patient Positioning | Administering anesthesia and positioning the patient for optimal access. | Patient comfort, safety, and access to the surgical site. |
| Recipient Site Preparation | Cleaning and preparing the area for graft placement. | Removing diseased tissue, creating a healthy environment. |
| Graft Preparation and Customization | Preparing and customizing the cadaver bone graft. | Sterility, sizing, and shaping to fit the defect. |
| Placement and Fixation | Placing and securing the graft at the recipient site. | Stability, fixation methods, and promoting integration. |
Clinical Applications of Cadaver Bone Grafts
Cadaver bone grafts have changed orthopedic surgery a lot. They are used in many procedures to fix bone problems. This makes them very useful for complex bone issues.
Trauma Reconstruction
Trauma reconstruction is a big use of cadaver bone grafts. When injuries are severe, they can cause a lot of bone loss. This makes healing hard. But, cadaver bone grafts help fix this by making bones strong again.
Tumor Resection Defects
Removing tumors often leaves big holes in bones. This is a big problem for doctors. Cadaver bone grafts fill these gaps, making bones strong again.
Key benefits of using cadaver bone grafts in tumor resection defects include:
- Restoration of bone structure
- Promotion of bone healing
- Reduced risk of complications
Spinal Fusion Procedures
Spinal fusion is another area where cadaver bone grafts are used a lot. They help bones in the spine stick together. This is key for treating many spinal problems.
“The use of allografts in spinal fusion has become a standard practice, giving a reliable option instead of using bone from the patient.”
Joint Reconstruction Applications
Cadaver bone grafts are also used in joint surgeries. They help when there’s a lot of bone loss or damage. This makes joints work better and hurts less.
Cadaver bone grafts are used in many ways, from fixing injuries and tumors to helping with spinal and joint problems. Their ability to help in so many ways makes them very important in surgery.
Enhancing Graft Success Rates
To boost graft success, we use several methods. These include biological enhancements, growth factors, and synthetic materials. Let’s dive into how these help in bone grafting.
Biological Augmentation Options
Biological augmentation means using natural materials to help grafts heal better. This includes platelet-rich plasma (PRP), bone marrow aspirate, and other substances. They help in bone growth and healing.
Platelet-rich plasma (PRP) is made from your own blood. It’s rich in growth factors that help bones grow back.
“The use of PRP in bone grafting has shown promising results, with studies indicating improved graft integration and healing rates.”
Growth Factors and BMPs
Growth factors are key in healing. They help cells grow and change. Bone Morphogenetic Proteins (BMPs) are special growth factors that help bones form.
| Growth Factor | Function |
|---|---|
| BMP-2 | Osteoinduction, promotes bone formation |
| BMP-7 | Enhances bone repair and regeneration |
Combination with Synthetic Materials
Using synthetic materials with cadaver bone grafts adds strength. Materials like calcium phosphate cements or bioactive glasses help fill gaps. They also support new bone growth.
Using synthetic materials with bone grafts is a promising method. It combines the best of both worlds. This approach leads to better and more lasting results in bone surgeries.
Post-Operative Management and Rehabilitation
The time after surgery is key for those with cadaver bone grafts. A detailed rehab plan is needed. Good care is vital to avoid problems and help the graft heal well.
Immediate Post-Surgical Care
Right after surgery, we watch for signs of trouble like infection or graft rejection. Keeping the area clean and taking care of the wound is very important.
Patients are told to rest, use ice to reduce swelling, and keep the affected limb up. This helps blood flow better.
Progressive Weight-Bearing Protocols
These plans slowly add weight to the grafted bone. This helps it get stronger and heal right. The plan varies based on where the graft is, what it’s for, and the patient’s health.
For example, after fixing a lower limb, patients start with no weight on it. Then, they move to some weight and eventually full weight. A physical therapist guides them.
Physical Therapy Regimens
Physical therapy is key in getting back to normal. It helps with function, movement, and muscle strength. The plan is made just for the patient and their surgery.
Monitoring Graft Integration
We check on the graft’s healing with X-rays or CT scans. This lets us see how it’s doing and adjust the rehab plan if needed.
| Week | Weight-Bearing Status | Physical Therapy Focus |
|---|---|---|
| 1-2 | Non-weight-bearing | Range of motion exercises |
| 3-4 | Partial weight-bearing (25%) | Strengthening exercises |
| 5-6 | Partial weight-bearing (50%) | Balance and coordination training |
| 7-8 | Full weight-bearing | Functional activities training |
By managing the post-op period well and making rehab plans for each patient, we boost the success of bone grafting.
Managing Complications and Risks
It’s important to know and reduce risks with cadaver bone grafts for patient safety. Cadaver bone grafting is very effective but comes with risks. These include infection, graft failure, and disease transmission.
Infection Prevention and Treatment
Infection is a big risk with any surgery, including cadaver bone grafting. We use strict infection prevention steps. These include:
- Pre-operative antibiotics
- Sterile surgical techniques
- Post-operative monitoring for signs of infection
If an infection happens, we treat it quickly. This might mean antibiotics, draining the infected area, or removing the graft.
Graft Failure Identification
Graft failure is another possible issue. Spotting it early is key to managing it. Signs of graft failure include:
- Pain at the graft site
- Instability or loosening of the graft
- Radiographic evidence of graft resorption or failure to integrate
When we find graft failure, we can start revision plans. This helps ensure the best outcome for the patient.
Disease Transmission Risk Assessment
The risk of disease from cadaveric grafts is low, thanks to strict screening and processing. We carefully look at:
- The screening process for donors
- The processing and sterilization methods used for the grafts
- The overall health of the recipient
Understanding these factors helps us lower the risk of disease transmission even more.
Revision Strategies
When complications happen, we need revision plans. These might include:
- Re-grafting with a new cadaveric graft
- Use of synthetic graft materials
- Additional surgical procedures to stabilize or repair the affected area
Having a detailed plan for complications ensures the best results for our patients with cadaver bone grafting.
Conclusion
Cadaver bone grafts are key in fixing bone problems. They help patients with skeletal issues. This method is a big step forward in surgery.
We’ve looked at cadaver bone grafts in detail. We talked about what they are, how they’re made, and where they’re used. They help fix bone damage from injuries, remove tumors, and even in spinal and joint surgeries.
Getting good results with these grafts needs careful planning and skill. It also requires good care after surgery. Knowing the ups and downs helps doctors give the best care to their patients.
In short, cadaver bone grafts are a trusted choice for fixing bones. As they get better, they’ll help more people in surgery. This will lead to better health outcomes for patients.
FAQ
What is a cadaver bone graft?
A cadaver bone graft, also known as an allograft, comes from a donor. It’s processed to lower the risk of immune reactions and disease. It’s used to fix bone defects.
What are the types of cadaver bone grafts available?
There are several types of cadaver bone grafts. These include structural allografts, demineralized bone matrix (DBM), and morselized chips. There are also customized grafts for specific needs.
How are cadaver bone grafts processed and prepared?
Cadaver bone grafts are processed in several ways. They are deep frozen, freeze-dried, and sterilized. This is to prevent disease and ensure they work well with the host bone.
What is the role of osteoinduction, osteoconduction, and osteogenesis in bone grafting?
Osteoinduction, osteoconduction, and osteogenesis help bone grafts work. They help the graft blend with the host bone and grow new bone.
What are the clinical applications of cadaver bone grafts?
Cadaver bone grafts are used in many ways. They help fix bone damage from trauma, remove tumors, and support spinal and joint surgeries.
How can the success rates of cadaver bone grafts be enhanced?
To improve success rates, biological enhancements and growth factors are used. Synthetic materials can also be added to grafts.
What is the importance of pre-surgical planning in bone reconstruction?
Good planning is key for successful bone reconstruction. It includes imaging, choosing the right graft, and picking the best surgery approach.
What are the principles of post-operative management and rehabilitation following cadaver bone grafting?
After surgery, care and rehabilitation are important. This includes immediate care, weight-bearing exercises, physical therapy, and checking graft integration.
How are complications and risks associated with cadaver bone grafting managed?
Risks are managed by preventing infections and treating graft failures. Disease risks are assessed, and revision surgeries are done when needed.
What is bone grafting?
Bone grafting is a surgery to fix bone defects. It involves transplanting bone tissue, which can come from the patient or a donor.
What is the difference between a cadaver bone graft and other types of bone grafts?
Cadaver bone grafts come from donors. Other grafts can be from the patient (autografts) or made (synthetic grafts).
Are cadaver bone grafts safe?
Yes, cadaver bone grafts are safe. They are processed to lower disease and immune reaction risks, making them a good choice for bone repair.
What is demineralized bone matrix (DBM)?
Demineralized bone matrix (DBM) is a type of graft. It’s processed to remove minerals, leaving a matrix that helps bone grow.
References
National Center for Biotechnology Information. Cadaver Bone Grafts in Orthopedic and Reconstructive Surgery. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC12009056/[3

































