Cancer involves abnormal cells growing uncontrollably, invading nearby tissues, and spreading to other parts of the body through metastasis.
Send us all your questions or requests, and our expert team will assist you.
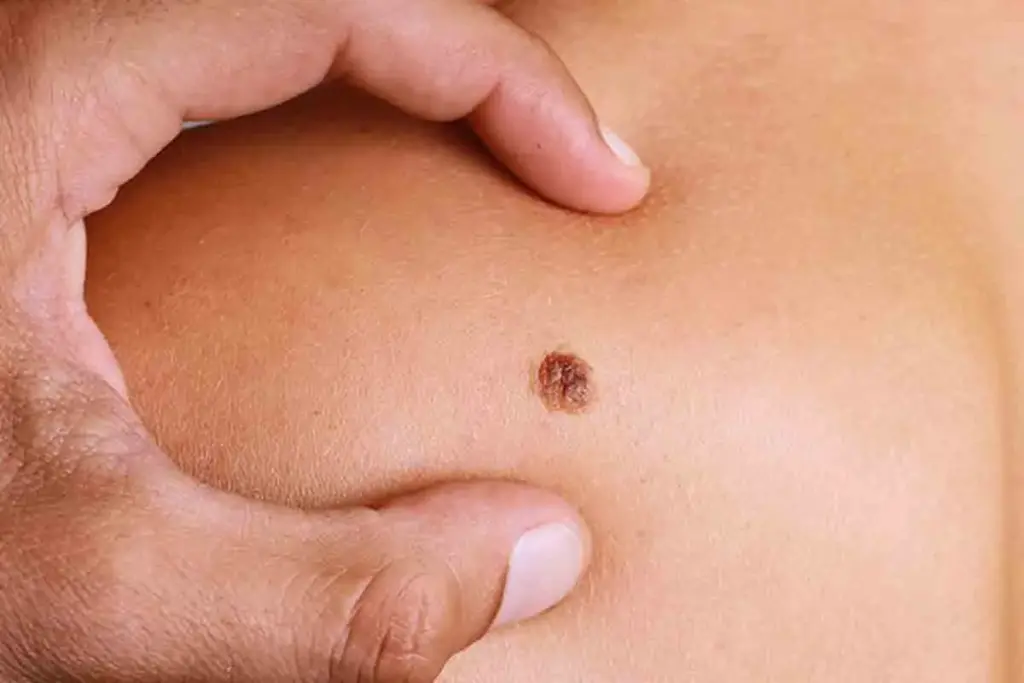
Surgery is the primary treatment for early-stage melanoma and is curative for the majority of patients. The standard procedure is a Wide Local Excision (WLE). After the diagnostic biopsy confirms melanoma, the surgeon must go back and remove a safety margin of normal-appearing skin around the original tumor site. This ensures that any microscopic cancer cells spreading horizontally in the skin are removed.
The Breslow depth of the tumor strictly dictates the width of this margin:
The excision extends down to the muscle fascia (the covering of the muscle) to ensure the full depth of the skin and subcutaneous fat is cleared. The wound is then closed with sutures. In some cases, particularly on the face or lower legs, where skin is tight, a skin graft or a flap (moving skin from a nearby area) may be required to close the wound.
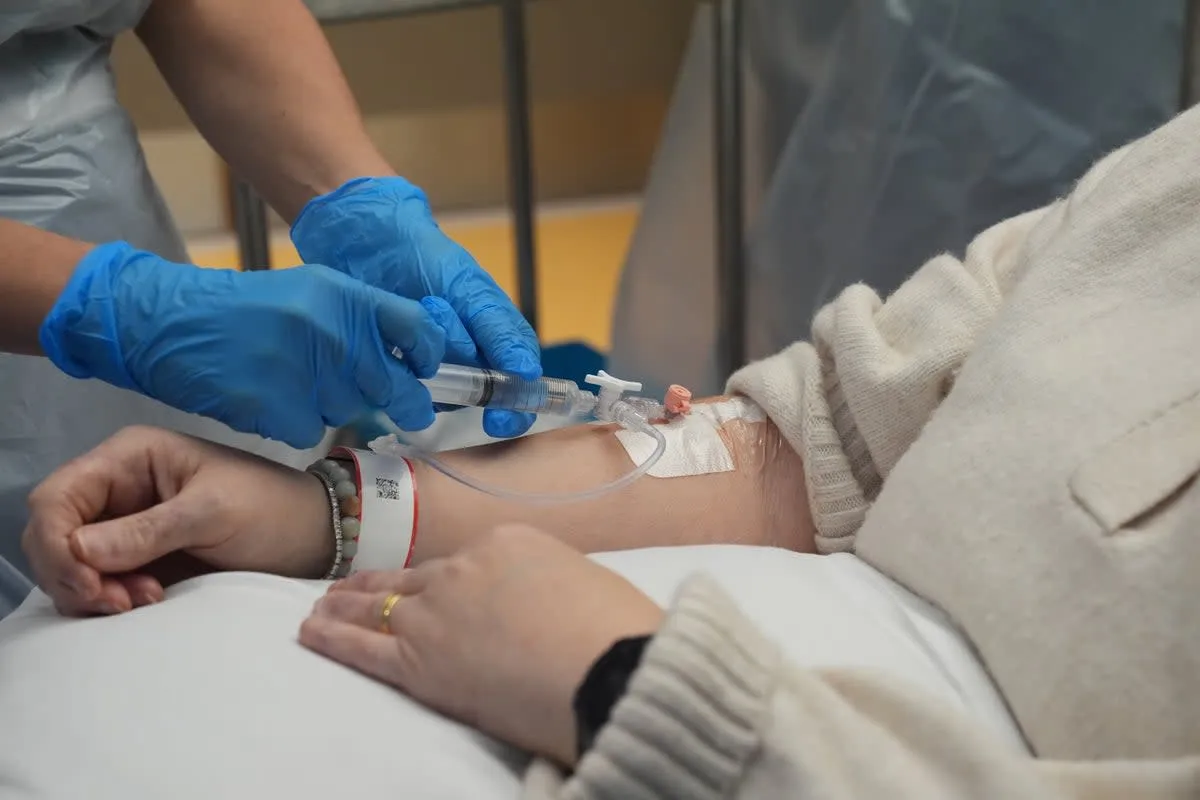
If the Sentinel Lymph Node Biopsy is positive, it indicates that the cancer has spread to the regional basin. Historically, patients with a positive sentinel node underwent a Completion Lymph Node Dissection (CLND), in which all remaining lymph nodes in the area (axilla, groin, or neck) were surgically removed.
However, recent major clinical trials (like MSLT-II) have shifted this paradigm. Data showed that for many patients with a small amount of cancer in the sentinel node, removing all the remaining nodes did not improve overall survival compared to monitoring them closely with ultrasound. Therefore, CLND is now performed less frequently. It is generally reserved for patients with bulky nodal disease (nodes that can be felt) or enormous burdens of metastatic disease in the sentinel node.
Instead of immediate extensive surgery, patients with positive sentinel nodes are typically offered Adjuvant Systemic Therapy (immunotherapy or targeted therapy). This treats the whole body, targeting residual cells in remaining nodes and distant organs, providing a survival benefit without the morbidity of complete nodal dissection (such as lymphedema).

The treatment of advanced melanoma has been revolutionized by immunotherapy, particularly checkpoint inhibitors. These drugs do not kill cancer cells directly; instead, they unleash the patient’s own immune system to fight the tumor.
PD-1 Inhibitors (Pembrolizumab, Nivolumab) target the PD-1 receptor on T-cells. Typically, cancer cells bind to PD-1 to tell the T-cell, “don’t attack me.” By blocking this interaction, these drugs remove the “brakes” on the immune system, allowing T cells to recognize and destroy the melanoma.
CTLA-4 Inhibitors (Ipilimumab) work at an earlier stage of immune activation. CTLA-4 is a protein that downregulates the immune system. Blocking it enhances the priming and expansion of T-cells in the lymph nodes.
These drugs can be used alone (monotherapy) or in combination. The combination of Ipilimumab and Nivolumab is highly potent and has significantly extended survival for Stage IV patients, though it carries a higher risk of immune-related side effects. Immunotherapy is used both for unresectable metastatic disease and as adjuvant therapy after surgery for Stage III/IV patients to prevent recurrence.
Approximately 50% of cutaneous melanomas harbor a BRAF mutation (specifically V600E or V600K). This mutation turns the BRAF protein into a constantly active switch that drives cell division via the MAPK pathway. Targeted Therapy exploits this specific genetic vulnerability.
Patients with advanced melanoma are routinely tested for BRAF mutations. If positive, they can be treated with a combination of a BRAF Inhibitor (e.g., Dabrafenib, Vemurafenib, Encorafenib) and a MEK Inhibitor (e.g., Trametinib, Cobimetinib, Binimetinib). MEK is a protein downstream of BRAF; blocking both points in the pathway shuts down the growth signal more effectively and delays the development of drug resistance.
Unlike immunotherapy, which can take time to work, targeted therapy often produces rapid tumor shrinkage, making it excellent for patients with a high symptom burden. However, tumors can eventually develop resistance to these drugs. Therefore, they are often sequenced with immunotherapy. It is important to note that targeted therapy is ineffective in BRAF-wildtype (negative) patients.
While melanoma was historically considered radio-resistant, Radiation Therapy plays a specific role. It is rarely used as a primary cure. Still, it is valuable as Adjuvant Radiation after lymph node dissection if there is a high risk of local recurrence (e.g., many positive nodes or extracapsular extension). It is also widely used for Palliation, shrinking tumors that are causing pain, bleeding, or pressing on vital structures like the spinal cord or brain. Stereotactic Radiosurgery (Gamma Knife) is highly effective for treating melanoma brain metastases.
For melanoma confined to a limb (e.g., multiple nodules on a leg) that cannot be surgically removed, Isolated Limb Perfusion (ILP) or Infusion (ILI) may be used. These procedures involve surgically isolating the blood flow of the affected limb and circulating high-dose chemotherapy (Melphalan) and heat only through that leg. This delivers a potent dose to the tumor without exposing the rest of the body to toxic side effects.
Talimogene laherparepvec (T-VEC) is an oncolytic virus therapy injected directly into melanoma nodules. It is a modified herpes virus that infects cancer cells, causing them to burst, and simultaneously stimulates the immune system to attack nearby tumor cells.

Send us all your questions or requests, and our expert team will assist you.
Adjuvant therapy is given after the primary surgery to clean up any microscopic cells left behind and lower the risk of the cancer coming back. Neoadjuvant treatment is given before surgery to shrink the tumor, making it easier to remove, and to test how well the cancer responds to the drug while it is still visible.
For Stage III or IV patients where the cancer has been surgically removed (adjuvant setting), the standard treatment duration is usually one year. For patients with metastatic disease that cannot be removed, treatment usually continues for as long as it is working and side effects are manageable, often up to two years or more.
Targeted therapy drugs work like a key that fits a specific lock. The “lock” is the mutated BRAF protein. If your cancer does not have the BRAF mutation (BRAF wild-type), it doesn’t have that specific lock. Taking the drug would be ineffective because there is nothing for it to target, and it could actually cause harm by activating normal cells.
No, the actual delivery of radiation is painless, like getting an X-ray. You cannot feel the beam. However, side effects can develop over time, such as skin redness (like a sunburn) in the treated area, fatigue, or hair loss at the specific site.
A complete response means that all detectable signs of cancer have disappeared on scans and exams. While this is the goal, even patients with a “partial response” (tumor shrinks but doesn’t vanish) or “stable disease” (tumor stops growing) can live for many years with a good quality of life on these treatments.

 Cancer
Cancer Cancer
Cancer Cancer
Cancer Cancer
Cancer Cancer
Cancer
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)