Cancer involves abnormal cells growing uncontrollably, invading nearby tissues, and spreading to other parts of the body through metastasis.
Send us all your questions or requests, and our expert team will assist you.

The diagnostic pathway for testicular cancer is a streamlined, evidence-based algorithm designed to rapidly confirm malignancy, define the histological subtype, and determine the anatomical extent of the disease. Given the rapid doubling time of germ cell tumors, diagnostic expediency is critical. The process integrates physical examination, high-resolution ultrasonography, serological tumor marker analysis, and cross-sectional imaging. Staging in testicular cancer differs from that in other solid tumors; it incorporates serum tumor markers (S levels) into the traditional TNM (Tumor, Node, Metastasis) system, recognizing that persistent marker elevation indicates active disease even in the absence of radiographic findings. This bio-anatomical staging system allows for exquisite precision in risk stratification and therapeutic planning.
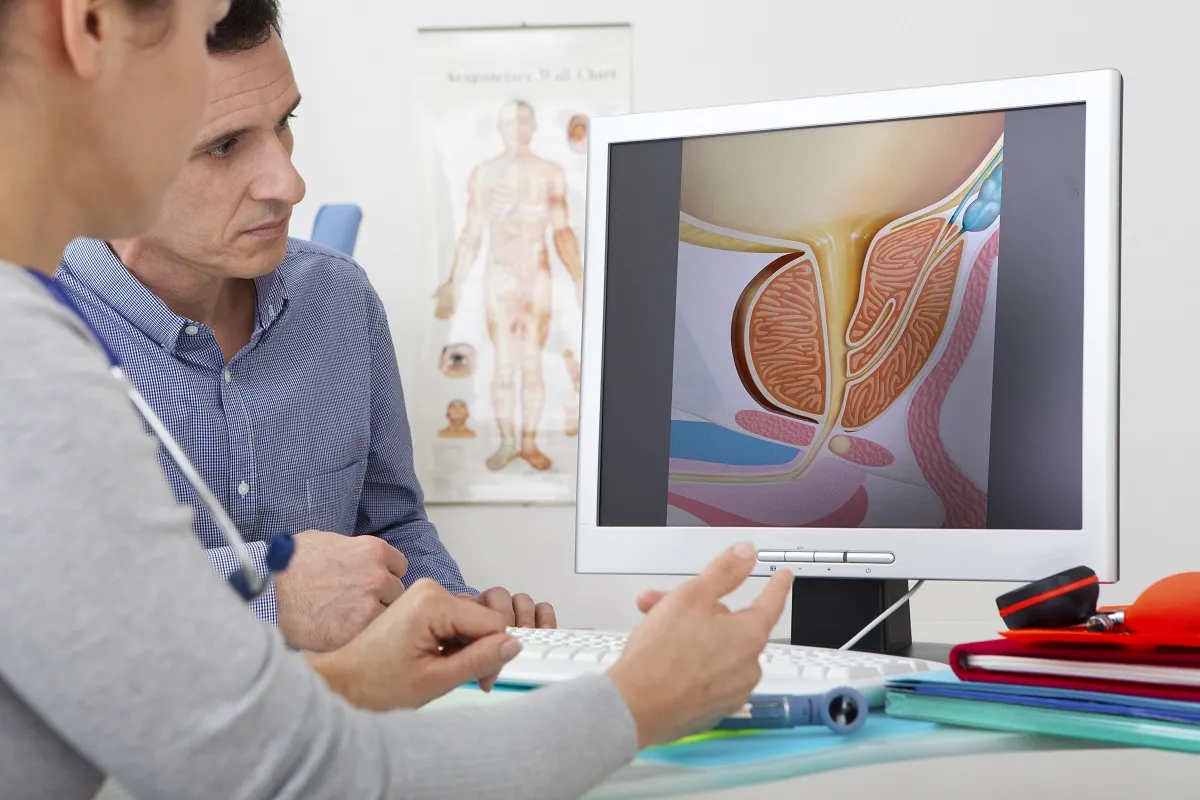
The initial evaluation begins with scrotal ultrasonography, the gold standard for characterizing testicular masses. This modality uses high-frequency sound waves to distinguish between intratesticular lesions (highly suspicious for malignancy) and extratesticular lesions (such as epididymal cysts or varicoceles, which are typically benign). On ultrasound, seminomas usually appear as homogeneous, hypoechoic (dark) lesions, often well-demarcated. Non-seminomas appear more heterogeneous, often with cystic spaces and calcifications (echogenic foci), reflecting their mixed tissue composition and areas of hemorrhage or necrosis. Ultrasound’s sensitivity for detecting testicular tumors approaches 100 percent, making it an indispensable tool for initial triage.
Testicular cancer is one of the few malignancies where serum tumor markers are diagnostic, prognostic, and essential for monitoring. Three key markers are evaluated: Alpha-Fetoprotein (AFP), Human Chorionic Gonadotropin (hCG), and Lactate Dehydrogenase (LDH). Yolk sac elements and embryonal carcinoma produce AFP; it is never elevated in pure seminoma. Therefore, a significant elevation of AFP in a patient with a biopsy-proven seminoma implies the presence of occult non-seminomatous elements, fundamentally altering the treatment plan.
Beta-hCG can be elevated in both seminomas and non-seminomas. In seminomas, it is produced by syncytiotrophoblastic giant cells, and levels are usually lower than in non-seminomas, where choriocarcinoma elements can drive levels into the millions. LDH is a nonspecific marker of tissue turnover and tumor burden; its elevation correlates with metastatic disease volume and is an independent prognostic factor in advanced stages. The rate of decline of these markers after orchiectomy (surgical removal of the testicle) follows predictable half-lives; a failure to normalize indicates residual metastatic disease.
Diagnostic Technologies and Procedures
Unlike other cancers, where a pre-operative biopsy is standard, a transscrotal biopsy is contraindicated in suspected testicular cancer. Cutting through the scrotum can disrupt the lymphatic drainage pathways, potentially seeding cancer cells into the inguinal lymph nodes or the scrotal skin, areas that are generally not at risk. Instead, the standard diagnostic procedure is a Radical Inguinal Orchiectomy. The surgeon makes an incision in the groin (inguinal canal), clamps the spermatic cord (vascular and lymphatic supply) high up to prevent tumor cell dissemination, and removes the entire testicle and cord en bloc. This provides the pathologist with the intact organ for accurate histological subtyping and assessment of local invasion (e.g., into the rete testis or tunica vaginalis), which are critical for pathological staging (pT stage).
Once the diagnosis is confirmed histologically, systemic staging determines the extent of disease. CT scans of the abdomen and pelvis are mandatory to assess the retroperitoneal lymph nodes. A node larger than one centimeter in the short axis is considered suspicious. Chest imaging (X-ray or CT) is used to screen for pulmonary metastases. Based on these findings and post-operative marker levels, patients are categorized into Stage I (localized), Stage II (nodal spread), or Stage III (distant metastasis).
Furthermore, the International Germ Cell Cancer Collaborative Group (IGCCCG) classification stratifies metastatic patients into Good, Intermediate, or Poor Risk groups. This risk stratification is based on the primary site (testis vs. mediastinum), the site of metastases (lung vs. non-pulmonary visceral), and the magnitude of marker elevation. This sophisticated biological staging dictates the intensity of chemotherapy, ensuring that patients are neither under-treated nor over-treated.
Molecular Profiling and Future Diagnostics

The diagnostic process must rigorously exclude benign conditions. Epididymo-orchitis (infection) can present with a swollen, tender testicle; however, symptoms usually respond to antibiotics, and an ultrasound shows increased blood flow (hyperemia) rather than a discrete mass. Testicular torsion is a surgical emergency presenting with acute pain and loss of blood flow, distinct from the painless mass of cancer. Hematomas from trauma can mimic tumors but typically resolve over time. Careful correlation of clinical history, physical exam, and ultrasound findings is essential to avoid unnecessary orchiectomy for benign pathology while ensuring no malignancy is missed.
Systemic Evaluation and Pre-treatment Assessment

Send us all your questions or requests, and our expert team will assist you.
Performing a biopsy through the scrotal skin disrupts the natural lymphatic drainage of the testicle. This can cause cancer cells to spread to the groin lymph nodes (inguinal nodes), which is not the typical route of spread. This complicates treatment and may require more extensive surgery or radiation to the groin area. The testicle is removed via the groin incision to avoid this risk.
Stage I testicular cancer means the cancer is confined entirely to the testicle and has not spread to the lymph nodes or other organs. Even if the tumor markers were elevated before surgery, they must return to normal after the testicle is removed for the cancer to remain Stage I. This stage has an excellent prognosis and often requires only surveillance.
The “S” stage refers to Serum tumor markers (AFP, hCG, LDH). Unlike other cancers, testicular cancer staging includes the levels of these markers after the testicle is removed. S0 means markers are regular. S1, S2, and S3 indicate progressively higher levels of markers in the blood, suggesting that active cancer cells remain in the body and necessitate chemotherapy.
Tumor markers are handy but not perfect. Not all testicular cancers produce markers (e.g., pure choriocarcinoma produces high hCG but normal AFP; some seminomas produce no markers). Therefore, normal marker levels do not guarantee the absence of cancer. However, if markers are elevated, they are particular indicators of disease activity and response to treatment.
The testicles develop near the kidneys in the fetus and descend into the scrotum before birth. They drag their blood supply and lymphatic vessels with them. Therefore, the first place testicular cancer spreads is not the groin, but the retroperitoneal lymph nodes in the back of the abdomen. A CT scan is the best way to inspect these nodes for enlargement.



Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)