Cancer involves abnormal cells growing uncontrollably, invading nearby tissues, and spreading to other parts of the body through metastasis.
Send us all your questions or requests, and our expert team will assist you.
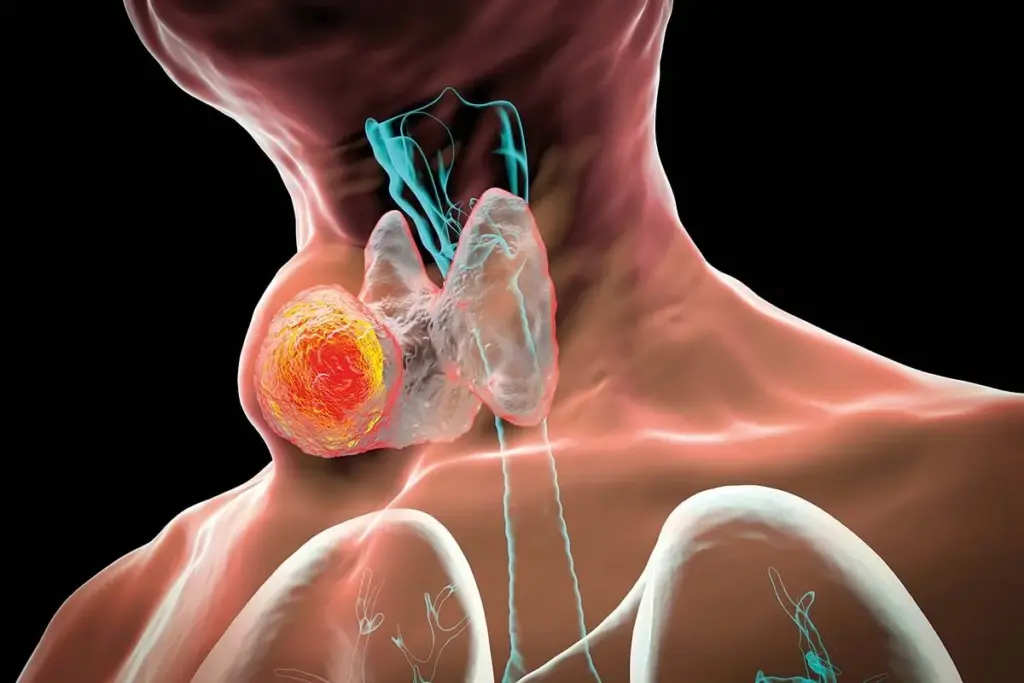
The most frequent clinical presentation of thyroid cancer is the discovery of a lump or nodule in the neck. Interestingly, the vast majority of thyroid nodules—estimates range up to ninety-five percent—are benign. However, distinguishing a malignant nodule from a benign colloid cyst or adenoma is the central diagnostic task. Malignant nodules are typically painless, firm to the touch, and may be fixed to the surrounding tissues rather than moving freely when the patient swallows.
Often, these nodules are discovered incidentally. A patient might undergo a CT scan of the neck for trauma, a carotid ultrasound for stroke risk, or a PET scan for another cancer, and a thyroid nodule is found by chance. This is referred to as an “incidentaloma.” While the lack of symptoms might suggest benignity, asymptomatic nodules carry the same risk of malignancy as palpable ones.
When a nodule is large enough to be felt or seen, it may appear as a swelling in the lower front of the neck. It is important to note that the size of the nodule does not perfectly correlate with cancer risk; small micronodules can be malignant, while large goiters can be entirely benign. However, rapid growth of a nodule over a period of weeks or months is a concerning sign that warrants immediate evaluation to rule out aggressive subtypes like anaplastic carcinoma or thyroid lymphoma.
While early-stage thyroid cancer is often asymptomatic, locally advanced disease manifests through the compression or invasion of adjacent anatomical structures. The thyroid gland wraps around the trachea (windpipe) and the esophagus (food pipe). A tumor growing posteriorly can compress the esophagus, leading to dysphagia—a sensation of food sticking in the throat or difficulty swallowing solid foods.
Compression of the trachea can cause shortness of breath (dyspnea), particularly when lying flat or during physical exertion. In some cases, patients may experience stridor, a high-pitched wheezing sound caused by turbulent airflow through a narrowed airway. This is a medical emergency indicating significant airway compromise.
A particular and concerning symptom is hoarseness or a change in voice quality. The recurrent laryngeal nerves, which control the vocal cords, run in the grooves between the trachea and the esophagus, directly behind the thyroid lobes. If a thyroid tumor invades this nerve, it causes vocal cord paralysis. A patient presenting with a thyroid nodule and new-onset hoarseness has a high probability of invasive malignancy. This symptom implies that the cancer has extended beyond the thyroid capsule.
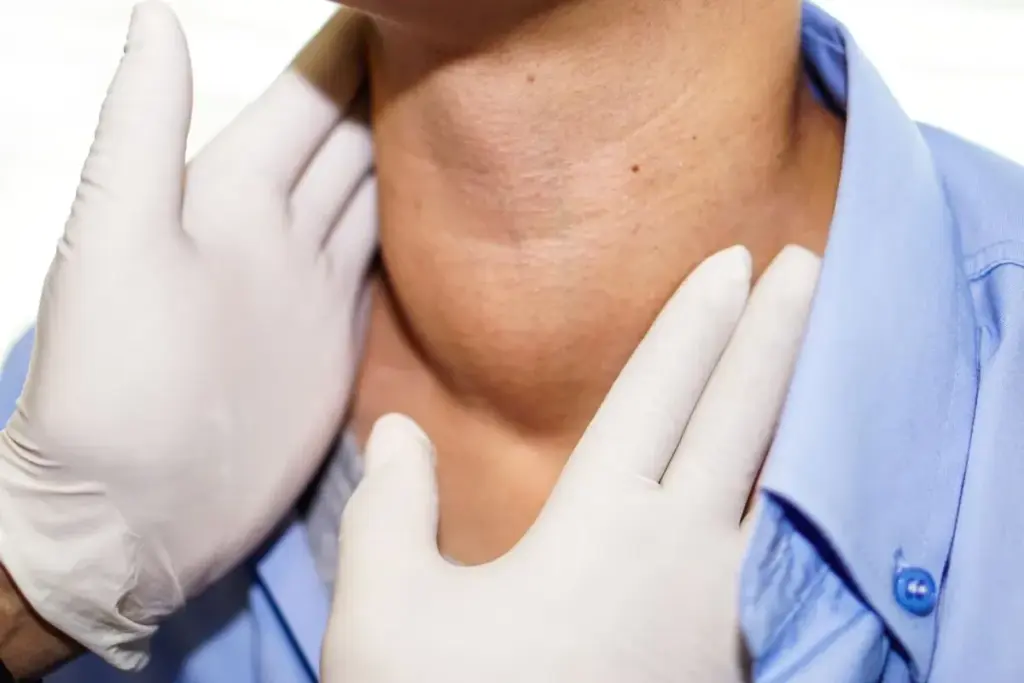
Ionizing radiation is the most well-established environmental risk factor for the development of differentiated thyroid cancer, particularly papillary thyroid carcinoma. The thyroid gland in children is susceptible to the mutagenic effects of radiation. Historically, this link was solidified by the observation of dramatic spikes in thyroid cancer incidence among survivors of the atomic bombings in Japan and children living in the fallout path of the Chernobyl nuclear disaster.
In a medical context, therapeutic radiation used in the past to treat benign conditions like acne, tonsillitis, or thymus enlargement has led to delayed thyroid cancers in adults. Currently, the risk is most relevant for survivors of childhood cancers (such as Hodgkin’s lymphoma) who received radiation therapy to the neck or chest. The latency period—the time between exposure and cancer development—can range from five years to decades.
The mechanism involves radiation-induced double-strand DNA breaks. If the cell repairs these breaks incorrectly, it can lead to chromosomal rearrangements, such as the RET/PTC rearrangement, which is frequently found in radiation-associated papillary thyroid cancers. It is crucial to note that routine diagnostic X-rays, including dental X-rays, involve extremely low doses and are not considered significant risk factors compared to therapeutic high-dose radiation.
Iodine is a double-edged sword in thyroid pathology. The thyroid requires iodine to synthesize hormones, and iodine intake in a population influences the type of thyroid pathology observed. In regions with severe iodine deficiency, the thyroid gland enlarges to capture more iodine, leading to goiters. Historically, these regions had higher rates of Follicular Thyroid Carcinoma and Anaplastic Carcinoma.
Conversely, in regions with sufficient or high iodine intake (such as the United States and many coastal nations), the overall incidence of goiter is lower, but the distribution of cancer types shifts. High iodine intake is associated with a higher prevalence of Papillary Thyroid Carcinoma and thyroiditis (inflammation).
While adequate iodine is essential for health, sudden excessive intake can trigger autoimmune thyroid issues. However, diet generally plays a minor role in thyroid cancer compared to other malignancies. There is no convincing evidence that specific foods (like cruciferous vegetables) cause thyroid cancer in humans with normal iodine status. The primary dietary focus remains on ensuring adequate, but not excessive, iodine intake through iodized salt or seafood.
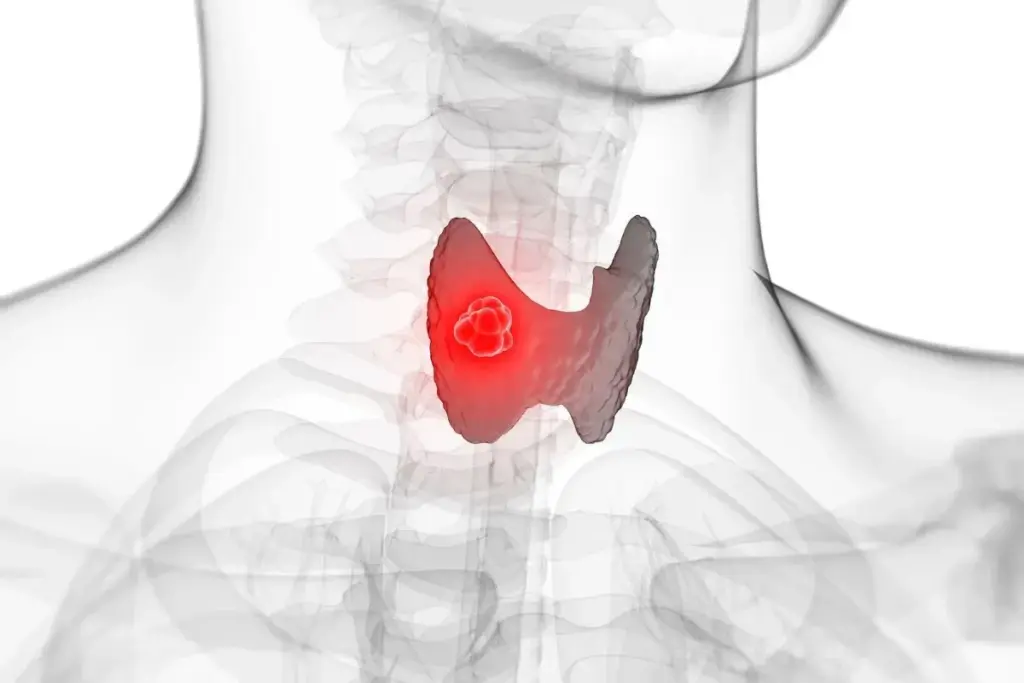
While sporadic mutations drive most cases, hereditary factors are critical in specific subtypes. The most significant is the link between Medullary Thyroid Carcinoma (MTC) and Multiple Endocrine Neoplasia type 2 (MEN2). MEN2 is an autosomal dominant syndrome caused by germline mutations in the RET gene. Patients with MEN2A or MEN2B have a near one hundred percent risk of developing MTC, often in childhood or early adulthood. Because of this, children identified as gene carriers usually undergo prophylactic thyroidectomy—removal of the thyroid before cancer develops.
Familial Non-Medullary Thyroid Cancer (FNMTC) is a term used when two or more first-degree relatives are affected by papillary or follicular cancer in the absence of a known syndrome. The specific genes driving FNMTC are less well defined than in MEN2, but they are likely to involve low-penetrance susceptibility genes. These familial cancers tend to be more aggressive, with a higher rate of multifocality (multiple tumors) and lymph node metastasis.
Other genetic syndromes that carry an increased risk of thyroid cancer include Cowden Syndrome (PTEN mutation), which is linked to breast, uterine, and follicular thyroid cancers, and Familial Adenomatous Polyposis (FAP), which is primarily a colon cancer syndrome but also predisposes to a specific variant of papillary thyroid cancer (cribriform-morular variant).

Send us all your questions or requests, and our expert team will assist you.
Hoarseness in the context of a thyroid nodule is caused by the tumor pressing on or invading the recurrent laryngeal nerve. This nerve controls the muscles that open and close the vocal cords. If the nerve is damaged, one vocal cord may become paralyzed, leading to a breathy, raspy voice. This is a sign that the nodule is likely malignant and invasive.
There is no scientific evidence that psychological stress directly causes thyroid cancer. Stress can affect the immune system and thyroid hormone levels, potentially exacerbating autoimmune thyroid conditions, but it does not induce the genetic mutations required for cancer cells to form.
The radiation dose from a modern dental X-ray or mammogram is incredibly low and is not considered a significant risk factor for thyroid cancer. The risk is associated with high-dose therapeutic radiation (like for treating lymphoma) or nuclear fallout. However, using a thyroid shield during dental X-rays is a reasonable precaution, especially for children.
There is a correlation between Hashimoto’s thyroiditis (chronic inflammation) and Papillary Thyroid Carcinoma. Patients with Hashimoto’s are slightly more likely to be diagnosed with thyroid cancer, and often the cancer is found within the inflamed gland. Interestingly, patients with Hashimoto’s who develop cancer usually have a better prognosis, perhaps because the immune system is already active in the gland.
When a doctor performs a nuclear thyroid scan, they look at how the nodule takes up a radioactive tracer. If a nodule takes up less tracer than the surrounding healthy tissue, it is called “cold.” Cold nodules are non-functioning and have a higher risk of being cancerous than “hot” nodules, which are overactive and almost always benign.

We often see patients with hypothyroidism, a condition where the thyroid gland doesn’t make enough thyroid hormones. The ICD-10 code E03.9 is for “hypothyroidism, unspecified.”
Radioactive iodine (RAI) is a common treatment for Graves’ disease and thyroid cancer. Studies show it doesn’t shorten life for most patients. It might even
Getting the thyroid gland checked right is key to good health. MRI and ultrasound help a lot in checking how well the thyroid is working.
The thyroid gland is a key part of our body, found in the neck. It helps control how our body grows and works. At Liv
At Liv Hospital, we know how important an accurate diagnosis is for your health. A CT scan of the thyroid gland is key. It helps

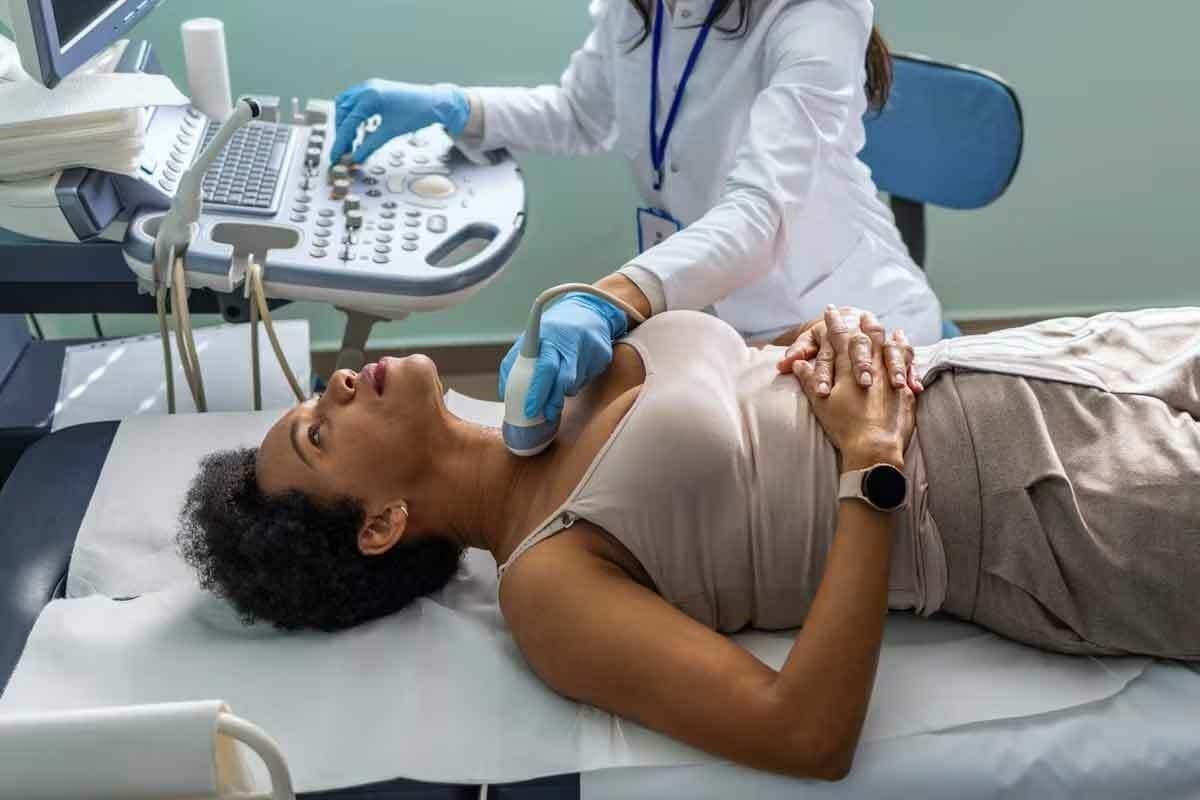
Understanding Thyroid Gland X-Ray and Ultrasound Knowing the normal size of the thyroid gland is key to detecting issues early. At Liv Hospital, we use

Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)