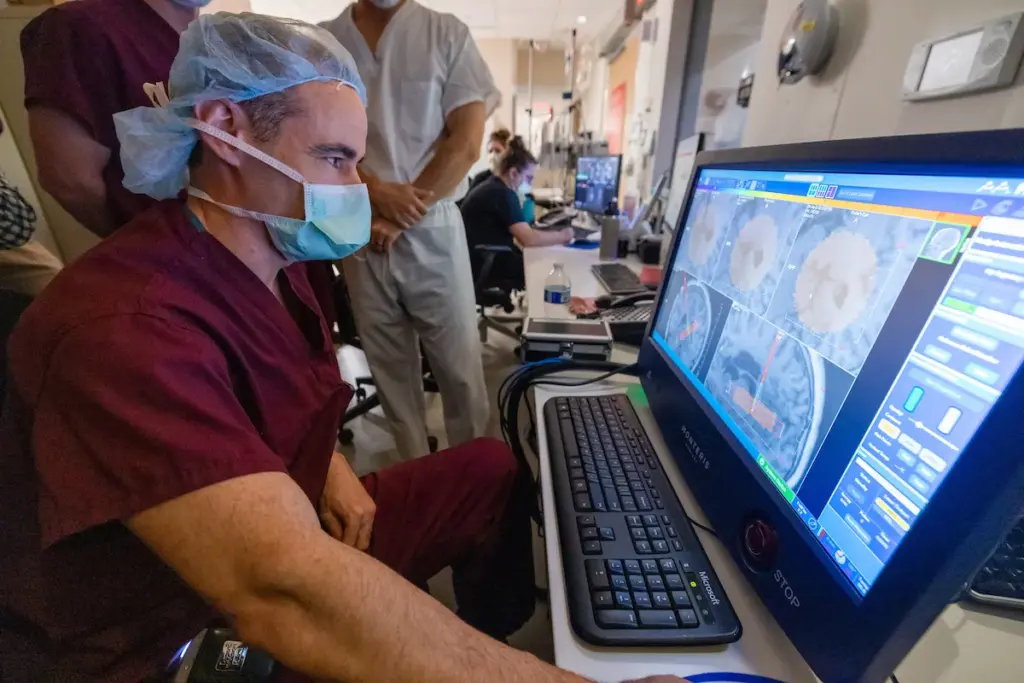
Neurosurgery is a complex field that has made significant advancements in recent years. Studies show that the success rate of neurosurgery changes with the type of procedure and the condition being treated. For example, removing brain tumors has gotten much better thanks to new surgical methods and technology.
The success rate of neurosurgery is a big worry for both patients and doctors. How well neurosurgery works, like cerebral tumor surgery, depends on many things. These include the skill of the neurosurgeon and the specific condition being treated.
Key Takeaways
- The success rate of neurosurgery depends on the type of procedure.
- Brain tumor removal has a high success rate due to advancements in surgical techniques.
- The expertise of the neurosurgeon plays a crucial role in the success of neurosurgery.
- Neurosurgical treatment outcomes vary based on the underlying condition.
- Recent studies have shown significant improvements in neurosurgery success rates.
The Scope and Evolution of Modern Neurosurgery
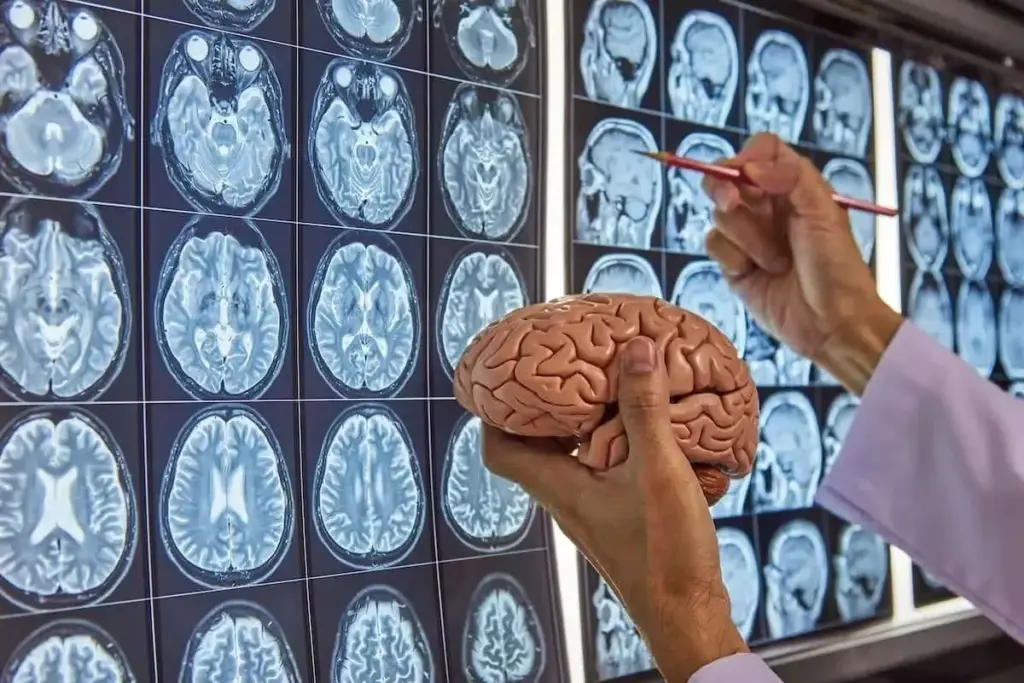
Modern neurosurgery has seen big changes thanks to new tech and methods. These changes have made surgeries better and more successful. Now, brain operation surgery has better results for patients.
Neurosurgery now covers many procedures, from removing brain tumors to small surgeries. This growth is thanks to neurosurgical oncology. It has made it possible to treat cases that were once too hard.
Types of Neurosurgical Procedures
Neurosurgery includes many types of procedures. These are:
- Tumor resections
- Arteriovenous malformation (AVM) treatments
- Spinal surgeries
- Trauma surgeries
- Functional neurosurgery for conditions like Parkinson’s disease
Each procedure needs careful planning and a team of experts.
Common Conditions Requiring Neurosurgical Intervention
Neurosurgery helps with many issues, like brain tumors and spinal problems. Thanks to new methods, brain tumor operation success rates have gone up.
Some common problems that need neurosurgery are:
- Brain tumors, both benign and malignant
- Cerebral aneurysms and arteriovenous malformations
- Spinal cord injuries and degenerative spinal conditions
- Hydrocephalus and other cerebrospinal fluid disorders
It’s important for patients and doctors to know about these conditions and how neurosurgery helps treat them.
Measuring Success in Neurosurgery
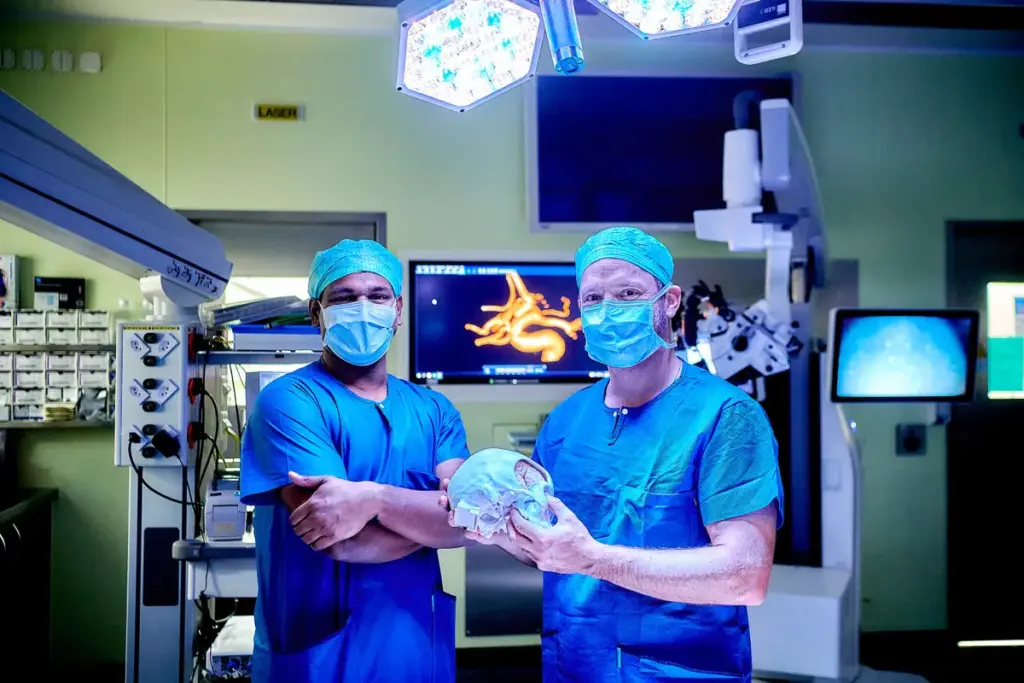
Success in neurosurgery is measured by looking at many things. We check how well patients do after surgery. This includes how they recover and their health over time.
Clinical Outcome Metrics
Clinical metrics are key to seeing if surgery works. We look at:
- Survival Rates: How many patients live after surgery, like for brain tumors.
- Complication Rates: How often problems happen after surgery, affecting patients.
- Reoperation Rates: How often patients need more surgery after the first one.
These numbers tell us a lot about how well surgery works. They help us know what to improve.
Quality of Life Assessments
Quality of life is important to see how surgery affects daily life. We check:
- Functional Status: How well patients can do everyday things and stay independent.
- Cognitive Function: How well patients think, remember, and make decisions.
- Pain Management: How well we manage pain to make patients more comfortable.
By looking at these, we understand how surgery affects patients’ lives. This helps us make better treatment plans.
Long-term Survival Statistics
Long-term survival stats are crucial, especially for brain tumors. We look at:
- Overall Survival: How long patients live after being diagnosed and treated.
- Progression-Free Survival: How long the disease doesn’t get worse.
- Disease-Specific Survival: Survival rates for specific neurosurgical conditions.
These numbers show how well surgery works over time. They help patients understand their chances.
By using clinical metrics, quality of life checks, and long-term survival stats, we get a full picture. This helps us improve care for patients.
Factors Influencing Neurosurgical Outcomes
It’s important to know what affects neurosurgical results. Neurosurgery is complex and needs skill and the right tools.
Patient-Related Factors
Things about the patient can change how well surgery goes. This includes their health, age, and any other health issues. For example, people with diabetes or high blood pressure might face more risks during surgery.
Surgeon Experience and Hospital Volume
The skill of the neurosurgeon and how often the hospital does surgeries matter a lot. Research shows that more experienced surgeons and hospitals that do a lot of surgeries have better results. This means fewer deaths from brain surgery.
Technological Resources Available
New technology has made neurosurgery safer and more precise. Tools like advanced imaging and surgical systems help a lot. They can lower the death rate from brain surgery.
|
Factor |
Influence on Outcome |
|---|---|
|
Patient Health |
Higher comorbidity burden can increase complication risk |
|
Surgeon Experience |
More experienced surgeons have lower complication rates |
|
Technological Resources |
Advanced technology improves precision and safety |
To get better results from neurosurgery, we need to look at many things. This includes the patient’s health, the surgeon’s skill, and the technology used. By focusing on these areas, we can make neurosurgery more successful.
Cerebral Tumor Surgery: Comprehensive Success Rate Analysis
Looking into the success rate of cerebral tumor surgery means checking several important factors. This surgery, also known as brain tumor removal, is very complex. It needs careful planning and execution. The success depends on the tumor type, patient health, and technology used.
Classification of Brain Tumors
Brain tumors are sorted by type, grade, and where they are. Knowing this helps figure out the best treatment. The main types are:
- Benign Tumors: These are non-cancerous and grow slowly.
- Malignant Tumors: These are cancerous and grow fast, spreading to other brain areas.
Overall Success Metrics for Brain Tumor Removal
Success in brain tumor removal surgery is measured in different ways. These include:
- Extent of Tumor Removal: How much of the tumor is removed during surgery.
- Patient Survival Rate: The percentage of patients who live for a certain time after surgery.
- Quality of Life: How surgery affects the patient’s life, like thinking, moving, and feeling well.
|
Tumor Type |
Success Rate (%) |
5-Year Survival Rate (%) |
|---|---|---|
|
Benign |
85-90 |
90-95 |
|
Malignant |
60-70 |
30-50 |
Factors Affecting Cerebral Tumor Surgery Outcomes
Many things can change how well cerebral tumor surgery goes. These include:
- Surgeon’s Experience: The skill and experience of the neurosurgeon.
- Technological Resources: The tools and imaging tech available.
- Patient’s Overall Health: The patient’s health and any other health issues.
By knowing these factors and how they affect surgery success, we can improve brain tumor treatment. This helps patients get better results.
Brain Tumor Surgery Survival Rate by Tumor Type
The type of brain tumor greatly affects a patient’s survival rate and prognosis. Brain tumors vary from benign to very malignant. This means we need to understand how each type impacts surgery results.
High-Grade Gliomas and Glioblastomas
High-grade gliomas, like glioblastomas, are very aggressive and hard to treat. Even with new surgical methods and treatments, the outlook is often bleak. Survival chances improve with more complete tumor removal. But, these tumors spread out, making full removal hard.
Low-Grade Gliomas
Low-grade gliomas have a better outlook, with higher survival rates. The aim of surgery is to remove as much tumor as possible while keeping brain function intact. These slow-growing tumors can still offer long survival times, even with less complete removal, thanks to treatments like radiation.
Meningiomas and Other Benign Tumors
Meningiomas and other benign tumors usually have great surgical results. These tumors are often completely removed by surgery, making it a cure. The main challenge is where the tumor is located and how it affects nearby brain areas.
Metastatic Brain Tumors
Metastatic brain tumors come from cancers elsewhere in the body. Their survival rate depends on the brain tumor and the cancer’s status. Surgery for these tumors can help patients live longer and better, especially with other treatments like radiation or radiosurgery.
In summary, the survival rate after brain tumor surgery depends a lot on the tumor type. Knowing these differences helps doctors tailor treatments for better results.
Brain Surgery Death Rate: Understanding Mortality Risk
Brain surgery is a lifesaving procedure but comes with risks. It’s important to know the mortality risk to make informed decisions.
Recent studies show the mortality rate for brain surgery has improved. This is thanks to better neurosurgical techniques and care before and after surgery. However, the brain surgery death rate can change a lot. This depends on the surgery type, patient health, and the neurosurgical team’s skill.
Procedure-Specific Mortality Statistics
The mortality rate for brain surgery varies by procedure. For example:
- Cerebral tumor surgery has a mortality rate of 1-5%.
- Arteriovenous malformation (AVM) surgery has a mortality risk of about 2-3%.
- Complex procedures, like those in deep brain structures, may have higher mortality rates.
Common Complications Leading to Mortality
Several complications can happen during or after brain surgery. These can lead to death. These include:
- Infection: Postoperative infections can be severe and life-threatening.
- Hemorrhage: Bleeding during or after surgery is a significant risk.
- Cerebral Edema: Swelling of the brain can lead to increased intracranial pressure and potentially fatal outcomes.
- Stroke or Cerebral Vasospasm: These vascular complications can result in significant morbidity and mortality.
Risk Stratification Models
Neurosurgeons use risk stratification models to understand and lower mortality risks. These models look at patient and procedure factors to predict outcomes. By identifying high-risk patients and tailoring management strategies, we can potentially reduce the mortality rate of brain surgery.
In conclusion, while brain surgery has risks, understanding these risks is key to improving outcomes. Advances in neurosurgical oncology and surgical techniques offer hope for better survival rates and quality of life for patients undergoing brain surgery.
Brain Cyst Surgery Survival Rate and Outcomes
Knowing the survival rate and outcomes of brain cyst surgery is key for patients. This surgery is complex and needs precision to get the best results.
Types of Intracranial Cysts
Intracranial cysts come in different types, each with its own traits and treatment plans. The main types are:
- Arachnoid cysts
- Colloid cysts
- Epidermoid cysts
- Dermoid cysts
It’s vital to know the exact type of cyst for the best surgery plan.
Success Rates for Different Cyst Removal Techniques
The success of brain cyst surgery depends on several things. These include the cyst type, its location, and the surgery method. Each method has its own success and complication rates, as shown in the table below:
|
Surgical Technique |
Success Rate |
Complication Rate |
|---|---|---|
|
Craniotomy |
85-90% |
5-10% |
|
Endoscopic Surgery |
80-85% |
3-7% |
|
Stereotactic Aspiration |
70-80% |
5-15% |
Table: Success and complication rates for different brain cyst surgery techniques.
Craniotomy is very successful but has a higher risk of complications than endoscopic surgery. The right technique depends on the cyst and the patient’s health.
The survival rate for brain cyst surgery has gotten better thanks to new surgical methods and technology. Knowing these details helps patients make better treatment choices.
Tumor Resection Procedure: Techniques and Efficacy
Tumor resection is key in treating brain tumors. It can be very successful, depending on the method used. The success of these procedures greatly affects how well patients do.
Gross Total vs. Subtotal Resection
The amount of tumor removed is very important. Gross total resection aims to remove the whole tumor. But, this isn’t always possible because of where the tumor is.
In some cases, subtotal resection is done. This means removing as much of the tumor as possible without harming the brain.
Choosing between these two options is complex. Gross total resection might lead to better results, but it also risks brain damage if not done right.
Impact of Resection Extent on Patient Outcomes
The amount of tumor removed greatly affects how well a patient does. Patients who have the whole tumor removed usually do better than those who don’t. But, the patient’s overall health and the type of tumor also matter a lot.
For example, removing all of a malignant tumor is very hard. In these cases, treatments like chemotherapy and radiation might be used along with surgery to help the patient.
Advanced Intraoperative Mapping for Safer Resection
New techniques have made tumor removal surgeries safer and more effective. Tools like intraoperative MRI and functional brain mapping help find important brain areas and the tumor’s edges during surgery.
These tools help neurosurgeons remove tumors more accurately. This reduces the chance of brain damage and improves patient results. By using real-time data, surgeons can make better choices during surgery.
Minimally Invasive Brain Surgery: Outcomes and Advantages
Minimally invasive brain surgery has changed how we treat brain tumors. It offers many benefits to patients. This method uses smaller incisions, which means less damage to tissue and faster recovery times.
We are always looking into new ways to improve minimally invasive brain surgery. We want to know how different techniques work and what they offer. We will look at endoscopic approaches, laser interstitial thermal therapy (LITT), and stereotactic radiosurgery.
Endoscopic Approaches to Brain Tumors
Endoscopic surgery uses a thin, flexible tube with a camera and light. It lets doctors see and remove tumors with little harm to the brain. This method is great for tumors near the brain’s surface or hard to reach with open surgery.
Endoscopic surgery has many benefits. It uses smaller cuts, causes less brain damage, and lowers the risk of problems. But, it works best for certain tumors.
Laser Interstitial Thermal Therapy (LITT)
Laser Interstitial Thermal Therapy (LITT) uses laser heat to kill tumor cells. It’s good for deep tumors that are hard to get to with surgery.
LITT has many advantages. It causes less damage to nearby tissue, lowers infection risk, and shortens hospital stays. But, it’s important to choose the right patients for LITT, as it works differently for each tumor.
Stereotactic Radiosurgery as an Alternative
Stereotactic radiosurgery (SRS) is a precise radiation therapy. It focuses radiation on the tumor. Even though it’s not surgery, SRS is a minimally invasive option for brain tumors.
SRS has its own benefits. It’s non-invasive, has few side effects, and can treat tumors that are hard to reach. It’s best for small to medium tumors and can be a good choice for some brain tumors.
|
Treatment Option |
Benefits |
Limitations |
|---|---|---|
|
Endoscopic Surgery |
Minimally invasive, precise tumor removal |
Dependent on tumor location and size |
|
Laser Interstitial Thermal Therapy (LITT) |
Effective for deep-seated tumors, minimal tissue damage |
Variable effectiveness based on tumor type |
|
Stereotactic Radiosurgery (SRS) |
Non-invasive, precise radiation delivery |
Limited to small to medium-sized tumors |
As neurosurgery advances, methods like endoscopic surgery, LITT, and SRS will become more important. Each has its own benefits and is right for different patients.
How to Remove Tumor from Brain: Modern Surgical Approaches
Neurosurgery has made big strides in removing brain tumors. This complex task needs careful planning and precise execution. It also requires a deep understanding of neurosurgical techniques.
Preoperative Planning and Imaging
Good preoperative planning is key for successful brain tumor removal. We use MRI and CT scans to find the tumor and see how it affects the brain. These scans help us make detailed 3D models of the brain.
Functional MRI (fMRI) and diffusion tensor imaging (DTI) help us spot important brain areas. This reduces the chance of neurological problems after surgery. By combining these imaging methods, we make brain tumor removal safer and more effective.
Surgical Navigation Systems
Surgical navigation systems are crucial in modern neurosurgery. They help us remove tumors with greater precision. These systems use GPS-like technology to track instruments in real-time, based on the patient’s anatomy.
- Improved accuracy in tumor localization
- Enhanced ability to preserve critical brain structures
- Reduced risk of complications during surgery
Using these systems, we can tailor the surgery for better results.
Intraoperative Decision-Making
Decisions made during surgery are vital for brain tumor removal. We watch the patient’s brain function closely and adjust our plan as needed. Intraoperative imaging and neuromonitoring help us make quick, informed decisions.
By combining advanced planning, navigation systems, and quick decision-making, we can remove brain tumors effectively. This approach minimizes risks and helps patients recover better.
Advanced Brain Tumor Surgery Technologies
New techniques are making brain tumor surgeries more precise and effective. The field of neurosurgical oncology is changing fast. This is thanks to new technologies that are helping patients get better.
Intraoperative MRI and Ultrasound
Intraoperative MRI (iMRI) and ultrasound are changing how surgeons remove brain tumors. iMRI lets surgeons see the tumor in real-time during surgery. This helps them remove more of the tumor while keeping the brain safe.
Ultrasound gives real-time feedback on the tumor’s location. It’s very useful when the brain shifts during surgery. This helps surgeons adjust their plan.
|
Technology |
Benefits |
Limitations |
|---|---|---|
|
Intraoperative MRI |
Real-time imaging, more complete resections |
High cost, limited availability |
|
Intraoperative Ultrasound |
Real-time feedback, portable |
Operator-dependent, limited depth penetration |
Fluorescence-Guided Surgery
Fluorescence-guided surgery is a new way to make brain tumor removal more precise. It uses a dye that lights up tumor cells during surgery. This makes it easier to see and remove the tumor.
This method has been shown to help remove more of the tumor. 5-aminolevulinic acid (5-ALA) is a dye that works well for this. It helps doctors see and remove malignant gliomas better.
Robotic and Computer-Assisted Neurosurgery
Robotic and computer-assisted neurosurgery are leading the way in brain tumor surgery. These systems offer enhanced precision and dexterity. This means surgeons can do more complex surgeries with better results.
Robotic systems help with minimally invasive procedures. This means less recovery time and possibly better outcomes. Computer-assisted neurosurgery uses advanced software and hardware. It helps plan and execute surgeries with great precision.
- Robotic systems offer enhanced precision and dexterity.
- Computer-assisted neurosurgery improves planning and execution.
- Minimally invasive procedures reduce recovery time.
Brain Tumor Treatment Success Rate: Multimodal Approaches
Using different treatments together is key to fighting brain tumors. This means combining surgery, radiation, chemotherapy, and new treatments like immunotherapy. This mix is helping patients live longer and better.
Combining Surgery with Radiation Therapy
Surgery and radiation work together well to fight brain tumors. Radiation therapy hits any cancer cells left after surgery. This helps stop the tumor from coming back.
|
Treatment Modality |
1-Year Survival Rate |
3-Year Survival Rate |
|---|---|---|
|
Surgery Alone |
60% |
20% |
|
Surgery + Radiation Therapy |
80% |
40% |
Role of Chemotherapy in Improving Outcomes
Chemotherapy is very important for treating brain tumors, especially for glioblastoma and anaplastic astrocytoma. Temozolomide is a drug that helps when used with radiation. It makes patients live longer.
“The addition of temozolomide to radiation therapy has become a standard treatment for glioblastoma, significantly improving patient outcomes.” –
A leading neuro-oncologist
Emerging Immunotherapies and Targeted Treatments
New treatments like immunotherapy and targeted therapy are showing great promise. They aim to attack cancer cells without harming healthy brain tissue. This could lead to fewer side effects and better results.
- Checkpoint inhibitors
- CAR T-cell therapy
- Targeted therapies against specific genetic mutations
As research keeps getting better, we can expect even more success in treating brain tumors. Adding these new therapies to treatment plans will likely help patients even more.
Brain Tumor Surgery Cost in the United States
Knowing the cost of brain tumor surgery is important for patients in the U.S. The cost can be high, and understanding it helps manage expenses.
Average Costs for Different Procedures
The cost of brain tumor surgery varies. It depends on the procedure type, case complexity, and treatment center location. On average, costs range from $50,000 to over $100,000.
A simple biopsy might cost less, while a complex tumor resection with advanced technologies could be more expensive.
Insurance Coverage and Reimbursement
Insurance coverage is key in reducing the cost of brain tumor surgery. Most plans cover neurosurgical procedures, but coverage varies.
Patients should check their insurance to know what’s covered, deductibles, and out-of-pocket costs.
Financial Assistance Programs
Financial assistance programs can help a lot. Many organizations offer support for medical expenses, including brain tumor surgery costs.
These programs may provide grants, help with medication, or travel expenses. Patients should look into these options to reduce financial stress.
Understanding surgery costs and exploring financial help are crucial for managing treatment expenses.
Selecting an Expert Brain Tumor Surgeon
When you get a brain tumor diagnosis, picking the right surgeon is key. Brain tumor surgery is complex and needs a lot of skill and experience. We need to consider several important factors when looking for a neurosurgeon.
Credentials and Specialization
A top brain tumor surgeon should have special training in neurosurgical oncology. They should have fellowship training in neuro-oncology or a related field. This shows they have advanced knowledge and skills in treating brain tumors. Board certification is also important, as it proves they meet certain standards in their field.
We want surgeons who are not only skilled but also keep up with new advancements in neurosurgical oncology. Being involved in research and clinical trials shows their commitment to the latest care.
Hospital Resources and Technology Access
The care a surgeon provides is also affected by the hospital’s resources. Hospitals with the latest imaging technologies, like intraoperative MRI, can improve surgery results. Having a team of neuro-oncologists, radiation oncologists, and rehabilitation specialists ensures patients get all-around care.
We look for hospitals with a strong neurosurgery department and a good reputation. It’s also important to have ICUs with experienced neurointensivists for postoperative care.
Patient Volume and Outcome Statistics
A surgeon’s experience, based on the number of procedures they do, is a big factor in success. Surgeons who do more procedures tend to have better results. We check outcome statistics, like complication and survival rates, to see how well a surgeon performs.
|
Criteria |
High-Volume Surgeon |
Low-Volume Surgeon |
|---|---|---|
|
Complication Rate |
Lower |
Higher |
|
Survival Rate |
Higher |
Lower |
|
Patient Satisfaction |
Higher |
Lower |
By looking at these factors, patients can make smart choices when picking a brain tumor surgeon. It’s about finding a surgeon who has the right mix of expertise, technology, and care for their needs.
Innovative Brain Tumor Treatment: Future Directions
New trends in precision medicine, artificial intelligence, and delivery systems are changing brain tumor treatment. These advancements are opening up new hopes for patients and doctors. They are pushing the limits of what’s possible in neurosurgery.
Precision Medicine in Neurosurgery
Precision medicine is changing neurosurgery by making treatments more specific. Doctors can now use a tumor’s genetic makeup to create targeted therapies. This makes treatments more effective and reduces side effects.
Key Benefits of Precision Medicine:
- Personalized treatment plans based on tumor genetics
- Improved efficacy of therapies
- Reduced risk of adverse effects
A recent study found that precision medicine could greatly improve brain tumor treatment outcomes.
“Precision medicine represents a paradigm shift in the management of brain tumors, enabling clinicians to tailor treatment to the unique characteristics of each patient’s tumor.”
– Recent Study
Artificial Intelligence Applications
Artificial intelligence (AI) is being used in neurosurgery to improve diagnosis and treatment. AI can analyze large amounts of data, like imaging and genomic information. This helps doctors make better decisions.
|
AI Application |
Description |
Potential Benefit |
|---|---|---|
|
Image Analysis |
AI-assisted analysis of MRI and CT scans |
Improved diagnostic accuracy |
|
Treatment Planning |
AI-driven planning for surgical interventions |
Enhanced precision and safety |
|
Outcome Prediction |
AI-based prediction of patient outcomes |
Informed decision-making |
Novel Delivery Systems for Therapeutics
New delivery systems are being created to make treatments for brain tumors more effective. These include methods like convection-enhanced delivery. They aim to get drugs directly to the tumor, avoiding traditional barriers.
As we look to the future, these new approaches will continue to shape brain tumor treatment. They offer hope for better patient outcomes and quality of life.
Conclusion: Navigating Neurosurgical Treatment Decisions
Choosing neurosurgical treatment needs careful thought, as Stephanie L. Woods, PhD, RN, points out. We’ve looked into neurosurgery’s complexities. This includes the success rates of different treatments and what affects outcomes.
It’s key to know the surgical options for brain tumors. The success of brain tumor treatment depends on many things. These include the tumor’s type and grade, the patient’s health, and the neurosurgical team’s skill.
When thinking about neurosurgical treatment, weigh the good against the bad. This helps patients make choices that fit their needs and situations.
Getting care from skilled neurosurgeons who use the newest methods is vital. This way, patients have the best chance for good treatment results.
FAQ
What is the overall success rate of brain tumor surgery?
The success rate of brain tumor surgery depends on the tumor type and the patient’s health. Benign tumors usually have a higher success rate than malignant ones.
How does the type of brain tumor affect the success rate of surgery?
The type of tumor greatly affects surgery success. Benign tumors like meningiomas have a better success rate than malignant ones like glioblastomas.
What are the survival rates for different types of brain tumors after surgery?
Survival rates vary by tumor type. For example, low-grade gliomas have better survival rates than high-grade gliomas or glioblastomas.
What is the mortality risk associated with brain surgery?
Brain surgery’s mortality risk depends on the procedure, patient health, and surgeon experience. Most neurosurgical procedures have low mortality rates.
How effective are minimally invasive brain surgery techniques?
Techniques like endoscopic approaches and laser interstitial thermal therapy (LITT) show promising results. They can reduce recovery time and improve outcomes for some conditions.
What is the role of advanced technologies in brain tumor surgery?
Technologies like intraoperative MRI and robotic-assisted neurosurgery improve surgery precision and safety. This leads to better patient outcomes.
How much does brain tumor surgery cost in the United States?
Brain tumor surgery costs in the United States vary widely. Costs can range from tens of thousands to hundreds of thousands of dollars, depending on the procedure and hospital.
What factors should be considered when selecting a brain tumor surgeon?
When choosing a brain tumor surgeon, look at their credentials, specialization, and patient outcomes. Ensure they have access to the necessary hospital resources for the best care.
What are the emerging trends in brain tumor treatment?
New trends include precision medicine and artificial intelligence in treatment. These advancements are expected to improve outcomes for brain tumor patients.
How can patients navigate neurosurgical treatment decisions?
Patients should discuss their condition and treatment options with their neurosurgeon. Understanding the risks and benefits of each approach helps make informed decisions.
What is the impact of combining surgery with other treatments like radiation therapy and chemotherapy?
Combining surgery with other treatments can improve outcomes. It can reduce tumor recurrence and increase survival rates for certain brain tumors.
What are the benefits of gross total resection versus subtotal resection in brain tumor surgery?
Gross total resection offers better outcomes than subtotal resection. However, outcomes depend on the tumor type and location.
How do surgeon experience and hospital volume affect neurosurgical outcomes?
Surgeon experience and hospital volume are key factors. More experienced surgeons and higher-volume hospitals usually achieve better results.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/41349031/



































