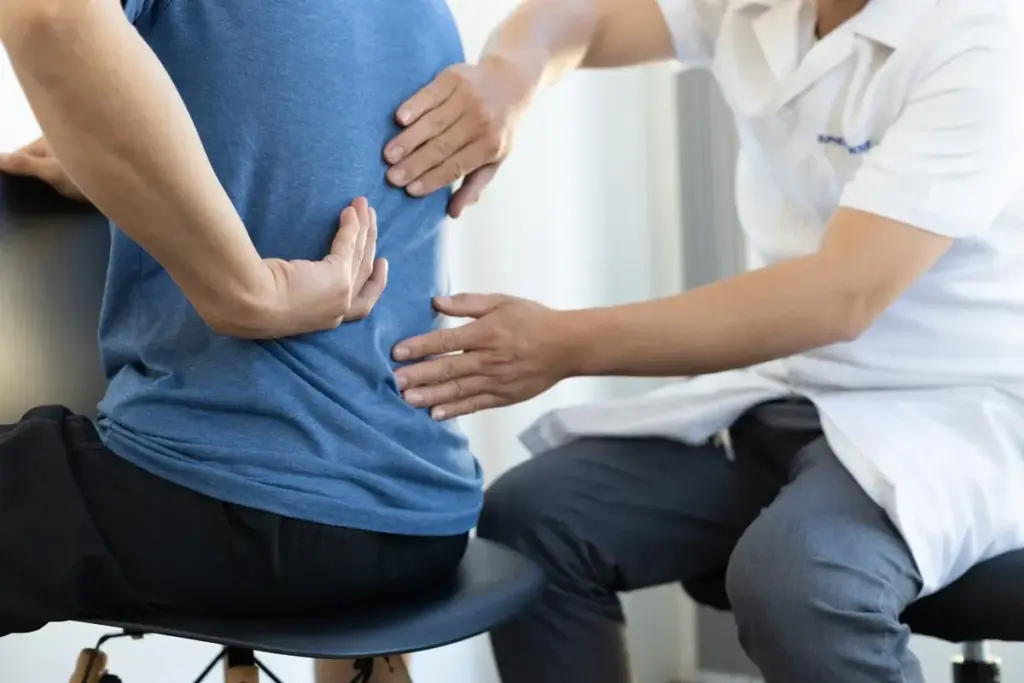
Degenerative spine disease is a big problem worldwide, causing a lot of back pain. Research shows that nearly 40% of adults have some spine changes by age 40. Knowing how this disease progresses is key to managing it well and improving life quality.
At our institution, we take degenerative spine disease seriously. We offer personalized care to meet each patient’s needs. Our focus is on spine health and back pain relief.
The speed at which degenerative spine disease progresses varies a lot. It depends on genetics, lifestyle, and age. We’ll look into this condition, its progression rates, and what affects it. This will help you manage it better.
Does degenerative disc disease worsen quickly? Understand the progression timeline and discover proven strategies to stop the pain fast.
Key Takeaways
- Degenerative spine disease is a common condition affecting the intervertebral discs.
- Its progression is influenced by genetics, lifestyle, and age.
- Understanding the condition is key to effective management.
- Personalized care can significantly improve spine health and provide back pain relief.
- Early intervention is critical for slowing disease progression.
The Nature of Degenerative Disc Disease
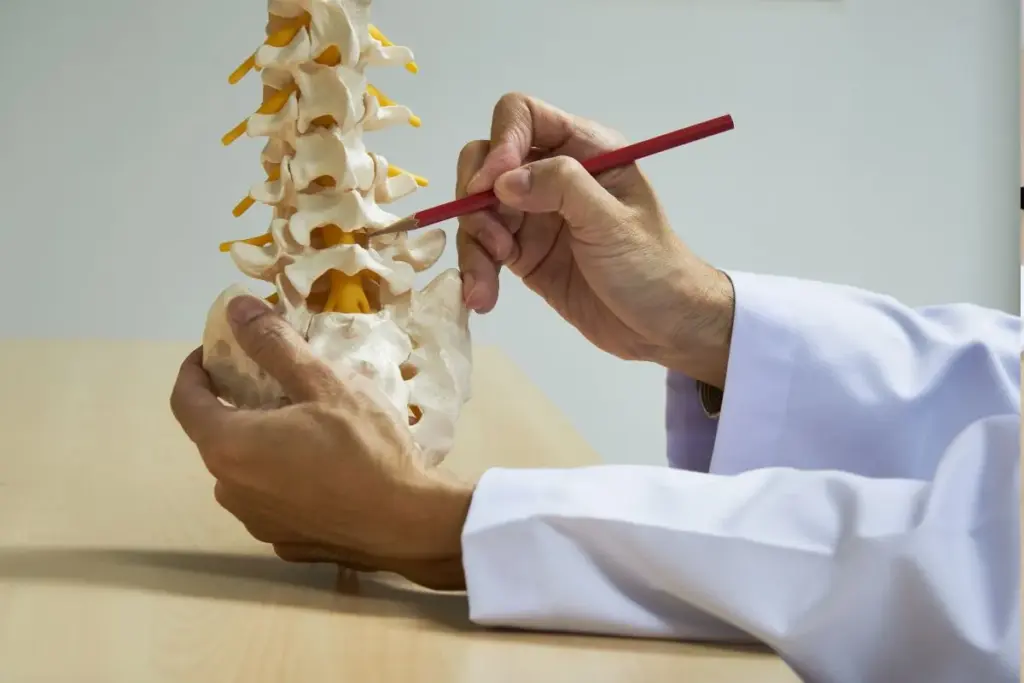
Understanding degenerative disc disease is key. It’s a common condition where the intervertebral discs in our spine wear out. These discs are like cushions between the vertebrae, helping our spine move smoothly and absorb shocks.
Definition and Pathophysiology
Degenerative disc disease happens when the discs in our spine start to break down. This can cause back pain and discomfort. It’s a complex process involving changes in the discs’ chemistry and structure.
The discs lose water and their outer layer starts to break down. This can cause the disc to bulge out, pressing on nerves and leading to pain.
Common Terminology and Medical Abbreviations
In medicine, degenerative disc disease has several names and abbreviations. The most well-known is DDD, short for Degenerative Disc Disease. Other terms include intervertebral disc degeneration and degenerative disorder. Knowing these terms helps doctors and patients talk clearly about the condition.
Some important terms related to degenerative disc disease are:
- Degenerative Disc Disease (DDD): The condition where the discs in our spine wear out.
- Intervertebral Disc Degeneration: The process of the discs in our spine getting worse.
- Disc Herniation: When the soft center of the disc bulges out through the outer layer.
By understanding degenerative disc disease, we can better handle its diagnosis and treatment. This knowledge helps both patients and doctors work together more effectively.
Average Progression Rates of Spinal Degeneration
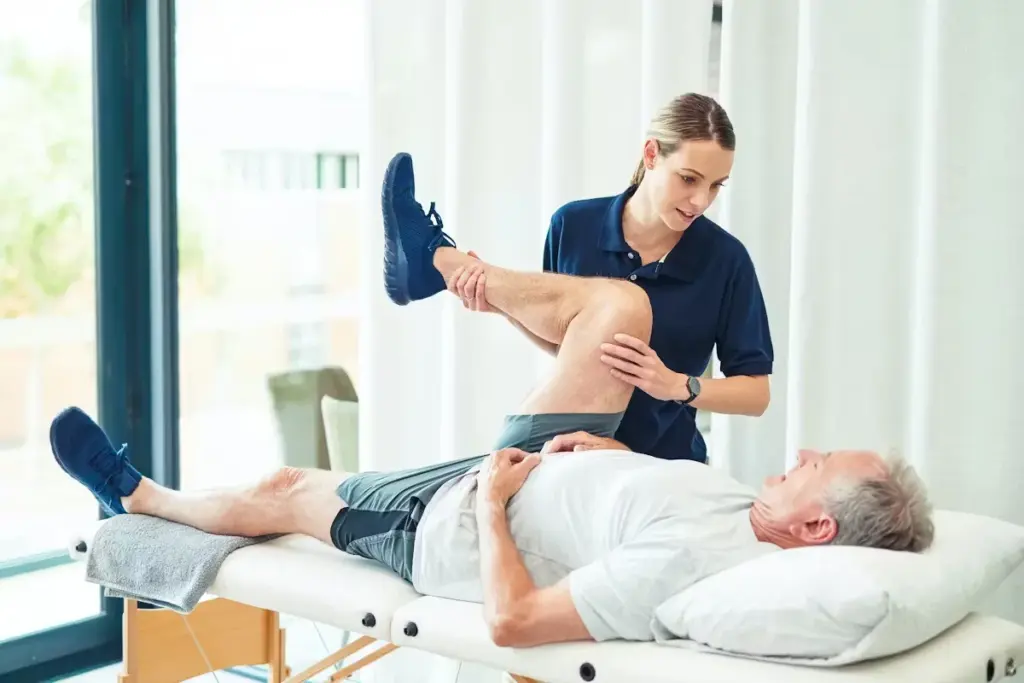
Knowing how fast spinal degeneration moves is key to fighting degenerative disc disease. The speed of this process affects how well treatments work and a patient’s life quality.
Normal Aging vs. Pathological Degeneration
It’s important to tell normal aging from pathological degeneration of the spine. Normal aging brings gradual changes that don’t hurt spinal function much. But, pathological degeneration speeds up and gets worse, causing big problems and pain.
Typical Progression Timeframes
How fast degenerative disc disease gets worse varies a lot. Age, genes, and lifestyle can change how fast it moves. It can go slow, taking years or decades, but sometimes it gets worse fast because of other reasons.
- Early stages: Minimal symptoms, gradual progression
- Moderate stages: Noticeable symptoms, moderate progression
- Advanced stages: Significant symptoms, potentially rapid progression
Individual Variation Factors
Many things can change how fast degenerative disc disease gets worse. Genetics are a big deal, with some people getting worse faster because of their genes. Lifestyle factors like smoking, how active you are, and your job can also affect it. Knowing these helps doctors make plans that fit each person’s needs.
By understanding what makes degenerative disc disease get worse, doctors can help more. They can slow it down and make patients’ lives better.
The 4 Stages of Degenerative Disc Disease
Degenerative disc disease goes through four stages, each with its own signs. Knowing these stages helps doctors diagnose and treat the condition better.
Stage 1: Initial Degeneration (0-5 years)
The first stage is when the discs start to break down, usually in the first 0-5 years. The discs lose water and become less flexible, causing them to shrink. People might not feel much pain yet, but doctors can see changes in the spine through scans.
Stage 2: Moderate Degeneration (5-10 years)
The second stage is when the discs get worse, between 5-10 years. The discs keep breaking down, and the outer layer might crack. This can cause mild back pain and stiffness.
Stage 3: Advanced Degeneration (10-15 years)
The third stage is when the discs are really worn out, between 10-15 years. The discs are almost gone, and the joints in the spine might get arthritis. People start to feel more pain, have trouble moving, and might even feel pain in their nerves.
Stage 4: Severe Degeneration (15+ years)
The last stage is when the discs are almost completely gone, after 15 years or more. The spine becomes unstable, and people feel a lot of pain. They might also lose a lot of mobility and have nerve problems.
|
Stage |
Timeframe |
Characteristics |
Symptoms |
|---|---|---|---|
|
1 |
0-5 years |
Initial degeneration, loss of disc hydration and height |
Mild or no symptoms |
|
2 |
5-10 years |
Moderate degeneration, annulus fibrosus cracks |
Mild back pain and stiffness |
|
3 |
10-15 years |
Advanced degeneration, facet joint osteoarthritis |
Chronic back pain, limited mobility |
|
4 |
15+ years |
Severe degeneration, significant disc height loss |
Severe pain, significant loss of mobility |
Progression Patterns by Spinal Region
Degenerative disc disease shows different patterns in different parts of the spine. Knowing these patterns helps doctors diagnose and treat better.
Cervical Disc Degeneration Timeline
Cervical disc disease moves faster than others because the neck is more active. People often feel neck pain and arm pain. Things like posture and past injuries can speed up this process.
Research says cervical disc disease can start in the early twenties. It keeps getting worse over time. Smoking and bad posture can make it worse faster.
Lumbar Degenerative Disc Disease Advancement
Lumbar disc disease is common and can really hurt your life. The lower back carries a lot of weight, which can cause it to degenerate. Symptoms include back pain, stiffness, and sometimes nerve problems.
|
Stage |
Symptoms |
Typical Age Range |
|---|---|---|
|
Early |
Mild back pain |
20-40 |
|
Moderate |
Moderate back pain, stiffness |
40-60 |
|
Advanced |
Severe back pain, neurological symptoms |
60+ |
Thoracic Spine Degeneration Rates
Thoracic spine disease is less common because the rib cage helps stabilize it. But, when it happens, it can cause a lot of pain. Symptoms include mid-back pain and sometimes nerve problems.
The rate of thoracic spine disease can be affected by things like scoliosis or past surgeries. Knowing how it works is key to finding the right treatment.
Symptom Evolution Throughout Disease Progression
The symptoms of degenerative disc disease change over time. This shows how spinal discs deteriorate. Patients may face various symptoms that affect their life quality. Knowing these changes helps in managing and treating the disease.
Early Warning Signs and Timeframes
Early signs of degenerative disc disease include mild back pain or stiffness. These symptoms happen after rest or inactivity. Studies show these signs can appear years before the condition worsens.
Mid-Stage Symptom Development (5-10 years)
Between 5 to 10 years after symptoms start, back pain gets worse. Pain may spread to arms or legs, depending on the disc location. Activities can make the pain worse.
Advanced Stage Manifestations (10+ years)
After 10 years, symptoms become severe and limit mobility. Patients may feel numbness, tingling, or weakness in their limbs. At this stage, daily activities and life quality are greatly affected.
|
Stage |
Typical Symptoms |
Timeframe |
|---|---|---|
|
Early Stage |
Mild back pain, stiffness |
0-5 years |
|
Mid-Stage |
Pronounced back pain, radiating pain |
5-10 years |
|
Advanced Stage |
Severe pain, limited mobility, neurological symptoms |
10+ years |
Knowing how symptoms change in degenerative disc disease is key. It helps in creating better treatment plans. Healthcare providers can then target pain management and spinal health.
Factors That Accelerate Degenerative Disc Disease Progression
Degenerative disc disease isn’t just about getting older. Many things can make it worse faster. Knowing what these are is key for both patients and doctors to better manage the disease.
Genetic Influences on Progression Speed
Genetics play a big part in how fast degenerative disc disease gets worse. Studies show that people with a family history of the disease tend to see it progress faster. Genetic factors can weaken the discs, making them more prone to wear and tear. Knowing your genetic risk can help in planning how to prevent and treat the disease.
Lifestyle Accelerators
Our lifestyle choices can really affect how fast degenerative disc disease gets worse. Smoking and being overweight are two big lifestyle factors that speed up the disease. Smoking cuts off blood flow to the discs, starving them of nutrients. Being overweight adds more stress to the spine. Choosing a healthier lifestyle can help slow down the disease’s progression.
Occupational and Activity-Related Factors
Jobs and certain activities can also make degenerative disc disease worse. Jobs that involve heavy lifting, bending, or twisting can stress the spine more. Sports or activities that put repetitive strain on the spine can also speed up the disease. Being aware of these can help protect your spine.
In summary, degenerative disc disease’s progression is influenced by genetics, lifestyle, and work-related factors. Understanding and tackling these can help manage the disease more effectively.
Diagnostic Methods for Tracking Disease Progression
Diagnosing and tracking degenerative disc disease involves imaging studies and clinical assessments. These methods are key to understanding the disease’s extent and creating a treatment plan.
Imaging Studies and Their Timing
Imaging studies like MRI and CT scans are vital for diagnosing and monitoring degenerative disc disease. They provide detailed information about the discs’ condition. This helps healthcare providers understand the disease’s stage.
The timing of these studies depends on symptoms and condition severity. For example, an MRI might be suggested for sudden symptom worsening or before surgery.
Clinical Assessment Timeline
Clinical assessments are also critical in managing degenerative disc disease. They include a detailed medical history and physical exams. These help evaluate the patient’s condition and track changes over time.
The frequency of these assessments varies based on disease stage and symptoms. Regular check-ups allow for treatment plan adjustments as needed.
Recommended Monitoring Frequency
The monitoring frequency for degenerative disc disease depends on several factors. These include disease stage, patient age, and overall health. Patients with early-stage disease may need less monitoring, while those with advanced disease require more.
Healthcare providers work with patients to create a personalized monitoring schedule. This balances disease management with the risks of frequent testing.
By using imaging studies, clinical assessments, and a tailored monitoring schedule, healthcare providers can track disease progression. They can then adjust treatment plans as needed.
Multilevel Degenerative Disc Disease: Complex Progression Patterns
It’s key to grasp how multilevel degenerative disc disease progresses. This condition affects multiple discs in the spine, causing significant changes. These changes can greatly affect how well a patient does.
Adjacent Segment Degeneration Timeline
Adjacent segment degeneration happens when the spinal segments next to a fused or degenerated one start to break down. This is a big deal in multilevel degenerative disc disease. It can make the disease get worse faster.
The time it takes for adjacent segment degeneration to show up can differ a lot. Research has found that:
- Within 5 years, many patients start to see signs of degeneration in the segments next to the fused or degenerated one.
- By 10 years, most patients with multilevel degenerative disc disease will have serious degeneration in the adjacent segments.
Whole Spine Involvement Progression
Whole spine involvement in degenerative disc disease is a more serious and complex stage. It’s marked by widespread degeneration across the spine. This can cause a lot of symptoms and make it hard to function.
Many things can affect how fast whole spine involvement progresses. These include:
- Genetics
- Lifestyle choices, like smoking and exercise
- History of spinal surgeries or injuries
Predicting Progression in Complex Cases
Figuring out how multilevel degenerative disc disease will progress in complex cases is tough. It needs a deep understanding of the patient’s health, lifestyle, and specific disease details.
We use top-notch imaging and clinical checks to track how the disease is moving. This helps us spot risks for faster degeneration. With this info, we can tailor treatments to slow down the disease and help patients do better.
Evidence-Based Methods to Slow Progression
To slow down degenerative disc disease, we need a mix of different methods. These methods help patients feel better and live better lives.
Physical Therapy Interventions
Physical therapy is key for keeping the spine mobile and strong. Targeted exercises help stabilize the spine and lessen pain. Research shows that physical therapy can really help slow down the disease.
A typical physical therapy program might include:
- Stretching exercises to improve flexibility
- Strengthening exercises to support the spine
- Low-impact aerobic exercises to enhance overall health
Pharmacological Approaches
Medications are also important for managing degenerative disc disease. Nonsteroidal anti-inflammatory drugs (NSAIDs) are often used to cut down pain and swelling.
|
Medication Type |
Purpose |
Benefits |
|---|---|---|
|
NSAIDs |
Reduce pain and inflammation |
Effective for short-term pain relief |
|
Corticosteroids |
Reduce inflammation |
Used for acute flare-ups |
|
Muscle relaxants |
Relax muscles |
Helpful for muscle spasms |
Regenerative Medicine
Regenerative medicine, like stem cell therapy, is showing promise. Stem cell therapy involves injecting stem cells to help heal and grow new tissue.
Though it’s new, regenerative medicine might offer a way to slow down the disease.
Lifestyle Modifications
Changing our lifestyle is also important. Keeping a healthy weight and doing regular exercise can help slow the disease.
Other lifestyle changes include:
- Improving posture to reduce spinal stress
- Avoiding heavy lifting and bending
- Quitting smoking to enhance overall health
Treatment Timing Based on Progression Stage
Managing degenerative disc disease well means timing treatments right. Studies show that the right time for treatment changes with the disease’s stage. This highlights the need for a treatment plan that fits each person’s situation.
Early Intervention Window (0-5 years)
Acting early, in the first 0-5 years, can slow down the disease. At this time, conservative treatments like physical therapy and lifestyle changes are key. These help keep the spine moving and ease pain.
- Physical therapy to improve flexibility and strength
- Lifestyle modifications, including diet and exercise
- Pharmacological approaches for pain management
Mid-Stage Treatment Options (5-10 years)
When the disease moves to the mid-stage (5-10 years), treatments change to better manage symptoms. Keeping the spine mobile and controlling pain are main goals.
Treatment strategies at this stage include:
- Advanced physical therapy techniques
- Minimally invasive procedures for pain relief
- Continued lifestyle modifications with a focus on spinal health
Advanced Stage Management (10+ years)
In the advanced stages (10+ years), treatments get more serious. Options like spinal fusion or disc replacement are for severe cases where other treatments failed.
At this point, emerging therapies like regenerative medicine are being looked into. These new methods aim to fix or grow back damaged disc tissue, possibly stopping the disease’s progress.
Emerging Therapies and Their Place in Progression
Emerging therapies are a focus of ongoing research in treating degenerative disc disease. As we learn more about the disease, new treatments are being developed. Regenerative medicine is a promising area for future treatments.
We’re moving towards more personalized treatment plans. These plans consider the disease’s stage and the patient’s unique situation. This approach is becoming more critical in managing degenerative disc disease.
Real Patient Experiences: Managing Progression Over Time
Real patient stories give us a unique look at managing degenerative disc disease. They share their experiences and tips on slowing the disease’s progress.
How I Slowed My Degenerative Disc Disease
Many patients have slowed their disease through lifestyle changes, physical therapy, and medical help. For example, a patient might talk about how exercise and a healthy weight helped them.
“I was diagnosed with degenerative disc disease in my lower back at the age of 40. By committing to a regular yoga practice and making dietary changes, I was able to reduce my symptoms and slow the progression of the disease.” –
Patient Testimonial
Progression Timelines from Patient Perspectives
Seeing how degenerative disc disease progresses from a patient’s view helps others. Patients’ experiences show how factors like genetics and lifestyle affect their disease. The success of their treatment also plays a big role.
|
Stage |
Typical Symptoms |
Adaptation Strategies |
|---|---|---|
|
Early Stage |
Mild back pain, stiffness |
Regular exercise, physical therapy |
|
Moderate Stage |
Increasing pain, limited mobility |
Pain management medications, lifestyle adjustments |
|
Advanced Stage |
Severe pain, significant mobility issues |
Surgical options, complete pain management |
Adaptation Strategies at Different Stages
Patients adapt to degenerative disc disease in different ways, based on their disease stage. Early on, they often try physical therapy and exercise. As the disease gets worse, they might use pain meds and make lifestyle changes.
Looking at patient experiences and strategies helps us understand how to manage degenerative disc disease. It’s important for patients to work with their healthcare providers to create a treatment plan that fits them.
Long-Term Prognosis and Life Expectancy
Degenerative disc disease’s long-term outlook depends on several factors. These include the disease’s stage and the person’s overall health. Knowing these details is key for managing the condition well and planning for the future.
Statistical Progression Data
Research shows that degenerative disc disease’s progression can differ a lot among people. Statistical data helps doctors give more accurate predictions about how the disease will progress.
Progression Rates: Studies reveal that how fast the disease progresses can be affected by age, genetics, and lifestyle. For example, a study in the Journal of Orthopaedic Research found that those with a family history of the disease tend to progress faster.
|
Disease Stage |
Average Progression Time |
Common Symptoms |
|---|---|---|
|
Initial Degeneration |
0-5 years |
Mild back pain, stiffness |
|
Moderate Degeneration |
5-10 years |
Increasing pain, limited mobility |
|
Advanced Degeneration |
10-15 years |
Significant pain, neurological symptoms |
Functional Independence Timeline
Keeping functional independence is a big concern for those with degenerative disc disease. Research shows that with the right care, many can stay independent for a long time.
Factors influencing functional independence include: how fast the disease progresses, the success of treatments, and overall health.
Life Expectancy with Degenerative Disc Disease
Even though degenerative disc disease is a chronic condition, it’s not usually life-threatening. People with this condition generally live as long as others, as long as they get the right care and management.
Realistic Expectations for Different Age Groups
Prognosis and life expectancy can change based on age and overall health. Younger patients can benefit from early treatment, while older patients may face more challenges due to other health issues.
Understanding these factors helps both patients and doctors set realistic goals and create personalized treatment plans.
Conclusion
Understanding degenerative disc disease is key to keeping your spine healthy and improving your life. We’ve looked at how this condition progresses, how it’s diagnosed, and how to manage it. We’ve seen how it affects different parts of the spine and how lifestyle and genetics play a role.
Understanding the symptoms and conducting appropriate tests can effectively manage degenerative disc disease. There are proven ways to slow it down, like physical therapy and changing your lifestyle. Finding the right time to start treatment is also important, and new treatments are showing promise.
In conclusion, treating degenerative disc disease needs a full approach. By using medical knowledge and focusing on the patient, we can make a big difference. Our talk shows how important spine health is and why we need more research and support for those with this condition.
FAQ
What is degenerative disc disease?
Degenerative disc disease is when the discs in your spine wear out. These discs act as cushions between your vertebrae.
How fast does degenerative disc disease progress?
How fast it progresses varies. It depends on your genetics, lifestyle, and age.
What are the four stages of degenerative disc disease?
There are four stages. Stage 1 is the start, lasting 0-5 years. Stage 2 is moderate, lasting 5-10 years. Stage 3 is advanced, lasting 10-15 years. Stage 4 is severe, lasting over 15 years.
How does degenerative disc disease progress in different spinal regions?
It progresses differently in the cervical, lumbar, and thoracic spine. Each area has its own timeline and symptoms.
What factors accelerate the progression of degenerative disc disease?
Several factors can speed up its progression. These include genetics, smoking, obesity, and certain jobs or activities.
How is degenerative disc disease diagnosed and tracked?
Doctors use imaging studies like MRI and CT scans. They also do clinical assessments to track the disease.
What are the evidence-based methods to slow the progression of degenerative disc disease?
There are several methods. These include physical therapy, medicine, regenerative medicine, and making lifestyle changes.
What is the long-term prognosis and life expectancy for individuals with degenerative disc disease?
Life expectancy varies. It depends on the disease stage, overall health, and lifestyle.
How can I manage degenerative disc disease?
Managing it requires a holistic approach. This includes lifestyle changes, treatment options, and adapting to different stages.
What is multilevel degenerative disc disease?
It’s when multiple discs in the spine degenerate. This leads to complex progression patterns.
How does degenerative disc disease affect life expectancy?
It can impact life expectancy. The effect varies based on the individual case and disease stage.
What are the symptoms of degenerative disc disease?
Symptoms change over time. Early signs, mid-stage symptoms, and advanced symptoms all exist.
Reference:
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/14613273/


































