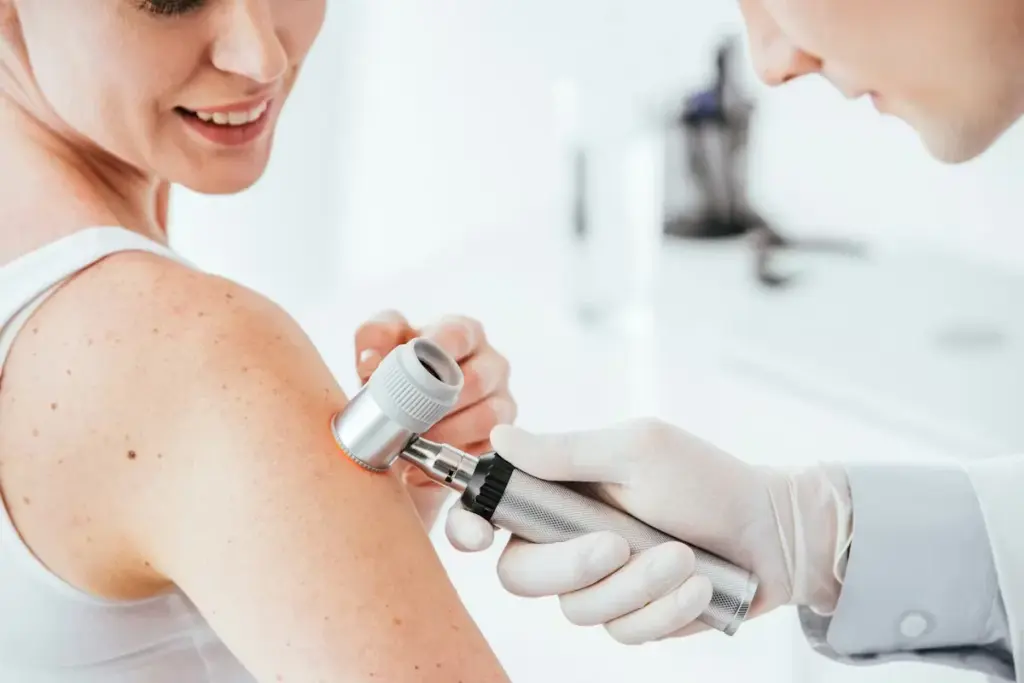
For those at risk of melanoma, the journey doesn’t stop after a dermoscopy. At Liv Hospital, we focus on follow-up care. This is based on solid research and advanced methods to catch problems early.
Follow-up care is key for those with melanoma history or high risk. We use proven follow-up methods to keep a close eye on patients. This way, we can act fast when needed.
Key Takeaways
- Regular digital follow-up is essential for high-risk patients after a dermoscopy.
- Follow-up care may include removal, monitoring, or reassurance based on the dermoscopic findings.
- Early detection is critical for optimal outcomes in melanoma patients.
- Liv Hospital employs advanced protocols for follow-up care, ensuring high-quality treatment.
- Patients with a personal history of melanoma benefit from digital follow-up monitoring.
The Role of the Dermatoscope in Skin Cancer Screening
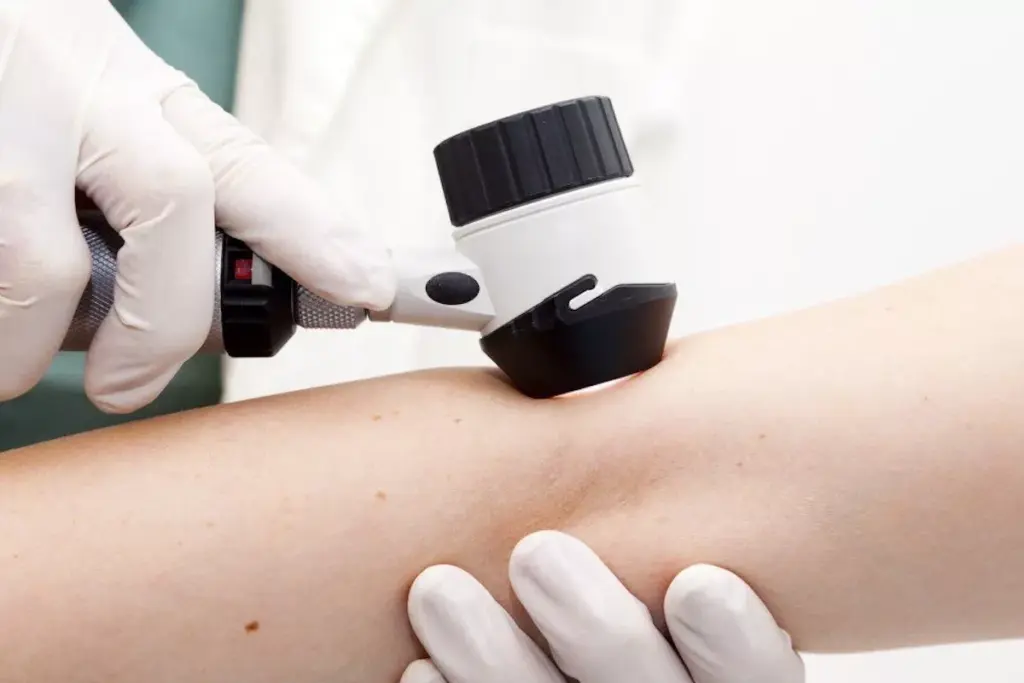
Dermatoscopy has changed how we look at skin lesions. It helps us see more details, leading to earlier skin cancer detection.
The dermatoscope is key in our work. It lets us do detailed mole checks. We see things we can’t see with our eyes, making our diagnoses better.
How Dermoscopic Imaging Enhances Diagnostic Accuracy
Dermoscopic imaging makes diagnosing skin lesions easier. With a dermoscope, we spot patterns and structures that show if a mole is cancerous.
|
Diagnostic Feature |
Naked Eye Examination |
Dermoscopic Examination |
|---|---|---|
|
Lesion Patterns |
Limited visibility |
Detailed pattern analysis |
|
Structural Details |
Not visible |
Clear visualization |
Types of Lesions That Warrant Dermoscopic Examination
Not every skin lesion needs a dermoscope check. But, some types really benefit from it. These include atypical, changing, or suspicious lesions.
Using dermoscopy in our exams helps us give more accurate diagnoses. This leads to better treatment plans for our patients.
Immediate Post-Dermoscopy Procedures and Results
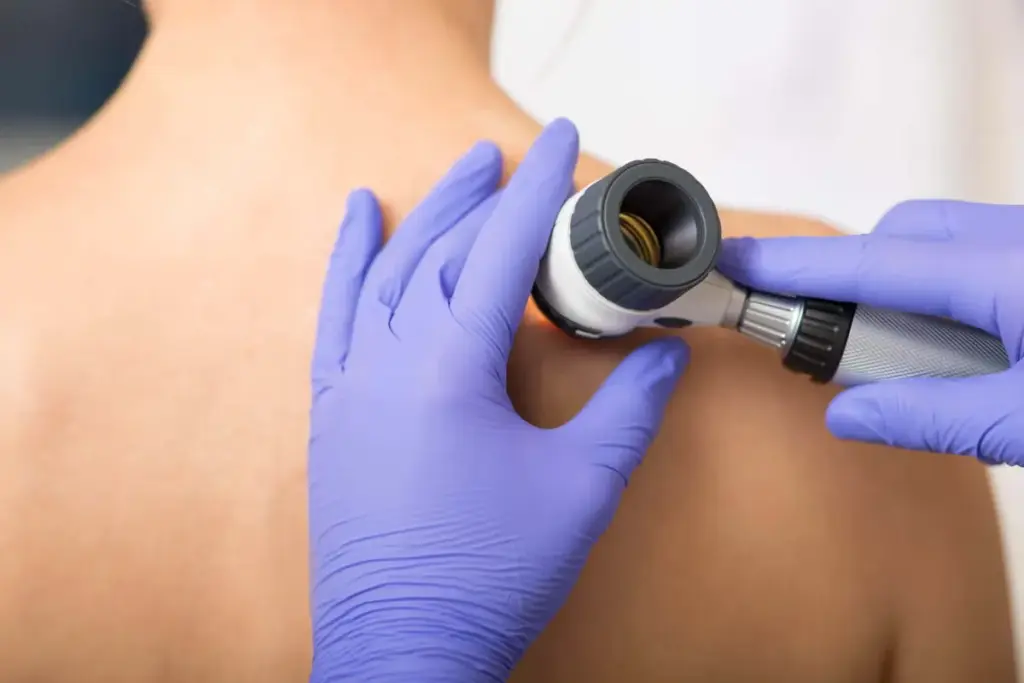
After the dermoscopy, our team shares the findings right away. This first look is key to figuring out what’s next for your care.
Same-Day Findings and Initial Assessment
We talk about the results with you after the dermoscopy. We explain what we found about the lesions. If they look okay, we might just tell you to keep an eye on them.
If something looks off, we’ll talk about more tests. Mole mapping and checking skin help us watch for changes. This is important for catching problems early.
Documentation Methods for Future Comparison
Keeping good records is important for watching your skin. We take detailed mole photographs using advanced imaging. These pictures are kept in your file for later checks.
|
Documentation Method |
Purpose |
Benefits |
|---|---|---|
|
Detailed Imaging |
Captures lesion characteristics |
Enhances diagnostic accuracy |
|
Digital Storage |
Stores images for future comparison |
Facilitates monitoring over time |
When Additional Testing May Be Recommended
If the dermoscopy shows something that worries us, we might suggest a biopsy. This choice depends on what we found and your skin’s health.
Our team is here to help you through every step. We want to make sure you know what’s happening and feel okay with it.
Risk Stratification Following Dermoscopic Examination
After a dermoscopic exam, we need to figure out who’s at high risk for skin cancer. This step is key to deciding how to follow up with patients.
Identifying High-Risk Patients
We look at several things to find out who’s at high risk. This includes their history of melanoma and if they have many unusual moles.
Personal and family melanoma history is very important. If someone has a family member with melanoma, they need to be watched more closely.
Impact of Personal and Family Melanoma History
Having had melanoma before makes you more likely to get it again. A family history of melanoma, too, raises your risk. We consider these when figuring out your risk level.
For example, if you have a family history of melanoma, you might need to see us more often. We make sure each patient gets the right care based on their risk.
How Multiple Atypical Nevi Affect Follow-Up Plans
Having many unusual moles is another sign of higher risk. People with lots of these moles need to be checked more often.
Our team at Liv Hospital uses special tools to plan your follow-ups. We understand the risks from dermoscopy to give you the best care.
By focusing on risk after dermoscopy, we make sure high-risk patients get the care they need. This helps improve skin cancer treatment outcomes.
Customized Follow-Up Schedules Based on Risk Assessment
At Liv Hospital, we make follow-up plans based on each patient’s risk. We know everyone’s situation is different. So, we tailor our care to fit their needs.
3-Month Follow-Up Protocol for Very High-Risk Patients
For those at very high risk, we suggest a 3-month check-up. This helps us spot any changes in skin lesions early. We can then act quickly if needed.
During these visits, we also look at any new skin issues. We adjust our plans based on what we find.
6-Month Follow-Up Protocol for Moderate-Risk Patients
Those at moderate risk should see us every 6 months. This keeps us in touch without being too much trouble. We teach them how to check their skin and protect it from the sun.
Annual Follow-Up Recommendations for Lower-Risk Patients
For those at lower risk, we suggest an annual check-up. This balance keeps us alert but also respects their lower risk. We keep an eye on their skin and change plans if needed.
Adjusting Schedules Based on New Findings
Follow-up plans can change. We adjust them based on what we find during skin checks. If a patient’s risk changes, we update their schedule to make sure they get the right care.
Digital Dermoscopy Monitoring Systems and Their Benefits
Advanced digital dermoscopy systems are changing how doctors diagnose and watch skin issues. At Liv Hospital, we use these top technologies. This helps us give our patients the best diagnoses and care plans.
Total Body Photography Integration
Digital dermoscopy systems can take total body photos. This lets doctors see all moles and lesions on a patient’s body. It helps them spot new or changing spots during check-ups.
Comparative Analysis of Lesions Over Time
These systems help doctors compare lesions over time. They track changes in size, shape, color, and texture. This is key for catching melanoma early, when it’s easiest to treat.
AI-Assisted Change Detection in Modern Systems
Today’s systems use AI to spot changes in lesions. AI algorithms look at images and find small changes that humans might miss. This makes our diagnoses more accurate and helps patients get better care.
Using digital dermoscopy systems is a big step forward in dermatology. They combine total body photos, comparisons, and AI to offer top-notch care. This care is proactive and tailored to each patient’s needs.
Statistical Realities: Melanoma Risk After Initial Dermoscopy
Dermoscopy results can give us clues about melanoma risk. But what do the numbers really mean? Knowing the stats on melanoma risk after dermoscopy is key for staying alert.
9% Annual Risk Within First Two Years Post-Melanoma
Research shows a 9% annual risk of new melanoma in the first two years after a previous one. This fact stresses the need for careful watching during this time. We suggest regular check-ups to spot any skin changes.
10-15% Development Rate During Multi-Year Surveillance
Over time, the risk of new melanomas can be 10% to 15%. This shows why we must stay vigilant and keep getting skin checks. Our team at Liv Hospital teaches patients about their risk and why they need to keep watching their skin.
How These Statistics Should Inform Patient Vigilance
These numbers tell us how critical it is for patients to check their skin regularly and keep up with doctor visits. Doing self-exams every month can catch new or changing spots early. Keeping a record of these changes is also key for tracking.
|
Time Frame |
Melanoma Development Risk |
Recommended Action |
|---|---|---|
|
First 2 years |
9% annual risk |
Regular follow-up appointments |
|
Multi-year surveillance |
10-15% development rate |
Ongoing vigilance and regular skin checks |
By grasping these statistical facts, patients can manage their risk better. They can take early steps to detect and prevent melanoma. We also stress the need for sun protection to lower the risk of new melanomas.
The Biopsy and Excision Process Following Suspicious Findings
When a dermoscopy shows something suspicious, we might need to do a biopsy or excision. At Liv Hospital, we know this can worry patients. We’re here to help them through every step.
Melanoma-to-Benign Lesion Ratio (1:7) in Monitored Patients
In patients who get regular checks, we find about 1 melanoma for every 7 benign lesions. This shows how careful we are when looking at suspicious spots.
What to Expect During and After a Skin Biopsy
A skin biopsy is a simple test where we take a sample of the suspicious area. We make sure it’s as comfortable as possible for you. Then, we send the sample to a lab for tests.
Our team will talk to you about the results. We’ll tell you what to do next based on what the tests show.
Recovery and Follow-Up After Lesion Removal
After removing a lesion, we give you clear instructions on how to care for the area. This helps it heal right. We also schedule follow-up visits to check on the healing and talk about the test results.
Pathology Results and Their Implications
The test results will tell us if the removed lesion is cancerous or not. If it is cancer, we’ll talk about the best treatment. This might include more surgery, regular check-ups, or other treatments.
We’re dedicated to supporting our patients. We make sure they get the care they need, tailored just for them.
Special Considerations for High-Risk Syndromes and Body Areas
High-risk syndromes and certain body areas need special care in dermoscopy. At our place, we focus on tailored dermoscopy for those with high-risk conditions. We also pay extra attention to sensitive or hard-to-see areas.
FAMMM Syndrome and 50% Increased Detection Sensitivity
FAMMM syndrome raises the risk of melanoma a lot. Dermoscopy is key in managing it, boosting detection by up to 50%. This helps spot atypical moles early, which could turn into melanoma.
Our team is skilled in dermoscopy for FAMMM syndrome. We watch for even the smallest changes in moles.
Monitoring Techniques for Difficult-to-See Areas
Some body parts, like the back, scalp, and legs, are tough to check well. We use special dermoscopy methods and tools for a closer look.
Total body photography is great for tracking changes in patients with many atypical nevi or melanoma history. It helps us see changes over time better.
Dermoscopy Applications for Genital and Other Sensitive Regions
Dermoscopy is not just for exposed skin. It’s also good for checking sensitive or genital areas. Our experts are careful and professional in these exams.
Using dermoscopy in genital areas can catch melanomas and other skin issues early. This improves patient results.
|
Body Area |
Dermoscopic Challenges |
Specialized Techniques |
|---|---|---|
|
Difficult-to-see areas (back, scalp) |
Limited visibility, hard to monitor |
Total body photography, specialized dermoscopic equipment |
|
Genital areas |
Sensitivity, difficulty in examination |
Gentle, careful dermoscopic examination, trained practitioners |
|
FAMMM syndrome patients |
Multiple atypical nevi, high melanoma risk |
Regular dermoscopic monitoring, enhanced detection sensitivity |
Patient Responsibilities Between Dermoscopy Appointments
Patients play a big role in their own skin care. At Liv Hospital, we stress the need for active participation in skin health. This includes catching any early signs of problems.
Monthly Self-Examinations: What to Look For
Regular self-checks are key to spotting new or changing spots. Remember the ABCDE rule:
- Asymmetry: Uneven shapes could be a sign.
- Border: Irregular edges might mean melanoma.
- Color: Moles with many colors or uneven tones are suspicious.
- Diameter: Larger moles could be melanomas.
- Evolving: Changes in size, shape, or color over time are red flags.
By using the ABCDE rule, patients can keep an eye on their skin. They should report any odd changes to their doctor.
Proper Documentation of New or Changing Lesions
Keeping a record of changes is important. Patients should:
|
Documentation Method |
Description |
|---|---|
|
Photography |
Take clear, well-lit photos of new or changing lesions from multiple angles. |
|
Journaling |
Keep a record of observations, including dates and descriptions of changes. |
Good documentation helps doctors decide if further action is needed.
Sun Protection Strategies to Reduce New Melanoma Risk
Protecting your skin from the sun is key to avoiding melanoma. Patients should:
“Protecting your skin from the sun is one of the most effective ways to reduce your risk of developing melanoma,” says a dermatologist at Liv Hospital.
- Use broad-spectrum sunscreen with at least SPF 30 daily.
- Wear protective clothing, including hats and sunglasses.
- Seek shade, specially during peak sun hours.
When to Seek Immediate Attention Between Scheduled Visits
Seek immediate help if you notice:
- Rapid changes in a mole’s size, shape, or color.
- New symptoms such as bleeding or itching.
- Unusual or new lesions.
If unsure, always check with a healthcare provider. At Liv Hospital, we support our patients every step of the way.
Conclusion: The Value of Comprehensive Post-Dermoscopy Care
Comprehensive post-dermoscopy care is key to catching new melanomas early. At Liv Hospital, we stress the need for regular check-ups and patient education. We also use advanced tools like dermoscopy and dermatoscopy to spot skin changes quickly.
We tailor follow-up plans to each patient’s risk level. We use digital dermoscopy and teach patients how to check their skin and protect it from the sun. These steps help us find melanomas early and give our patients the best care.
We’re dedicated to top-notch healthcare and support for international patients. Our goal is to make the dermoscopy and dermatoscopy process smooth and effective. By using the latest technology and caring for our patients, we aim to improve their health and happiness.
FAQ
What is dermoscopy and how does it help in skin cancer screening?
Dermoscopy is a way to look at skin lesions without cutting. It uses a special tool called a dermatoscope. This helps doctors see what’s under the skin’s surface. It makes it easier to find skin cancers, like melanoma.
What happens after a dermoscopy examination?
After looking at your skin, you’ll get the results the same day. Our team will take pictures of your skin for future checks. They might also suggest more tests if needed.
How do you determine the risk level of patients after dermoscopic examination?
We look at your family history and how many moles you have. This helps us figure out how likely you are to get melanoma. Then, we plan how often you should come back for checks.
What are the follow-up protocols for patients with different risk levels?
We make a plan for each patient based on their risk. High-risk patients see us every 3 months. Those at moderate risk come every 6 months. And lower-risk patients see us once a year.
How do digital dermoscopy monitoring systems enhance patient care?
These systems take pictures of your whole body. They help us see how moles change over time. This makes it easier to spot any problems early.
What are the statistical realities of melanoma risk after initial dermoscopy?
Studies show that melanoma risk is high in the first two years after a diagnosis. We teach patients about their own risk. This helps them understand their situation better.
What happens if suspicious findings are detected during dermoscopy?
If we find something suspicious, we might need to take a biopsy. We’ll tell you what to expect and what the results mean.
Are there special considerations for certain high-risk syndromes or body areas during dermoscopy?
Yes, some syndromes and areas, like the genitals, need extra care. Our team knows how to handle these cases carefully.
What are the patient responsibilities between dermoscopy appointments?
You should check your skin every month and tell us about any changes. Also, protect your skin from the sun to lower your risk of new melanomas. We’ll tell you when to come in right away.
Do dermatologists use a dermatoscope for skin in the genital area?
Yes, dermatologists use a dermatoscope to check skin in sensitive areas. It helps find skin cancers early.
How often should I get a mole checked?
How often depends on your risk. Our specialists will tell you how often to come in based on your risk level.
What is mole mapping, and how does it help?
Mole mapping is taking pictures of moles to watch for changes. It helps find skin cancer early.
References
National Center for Biotechnology Information (NCBI): https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7282651/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























