Allergic rhinitis is an immune reaction causing sneezing and congestion. It occurs when you breathe in allergens like pollen, dust, or pet dander.
Send us all your questions or requests, and our expert team will assist you.
Allergic rhinitis definition refers to inflammation of the inside of the nose caused by an allergen. Most people know this condition as “hay fever.” It happens when your immune system overreacts to particles in the air that are usually harmless. Instead of ignoring them, your body treats them like dangerous invaders.
The term comes from Greek words. “Rhino” means nose, and “itis” means inflammation. So, it literally translates to “nose inflammation.” This reaction triggers the release of chemicals in your body, such as histamine. This leads to the annoying symptoms many people face every year.
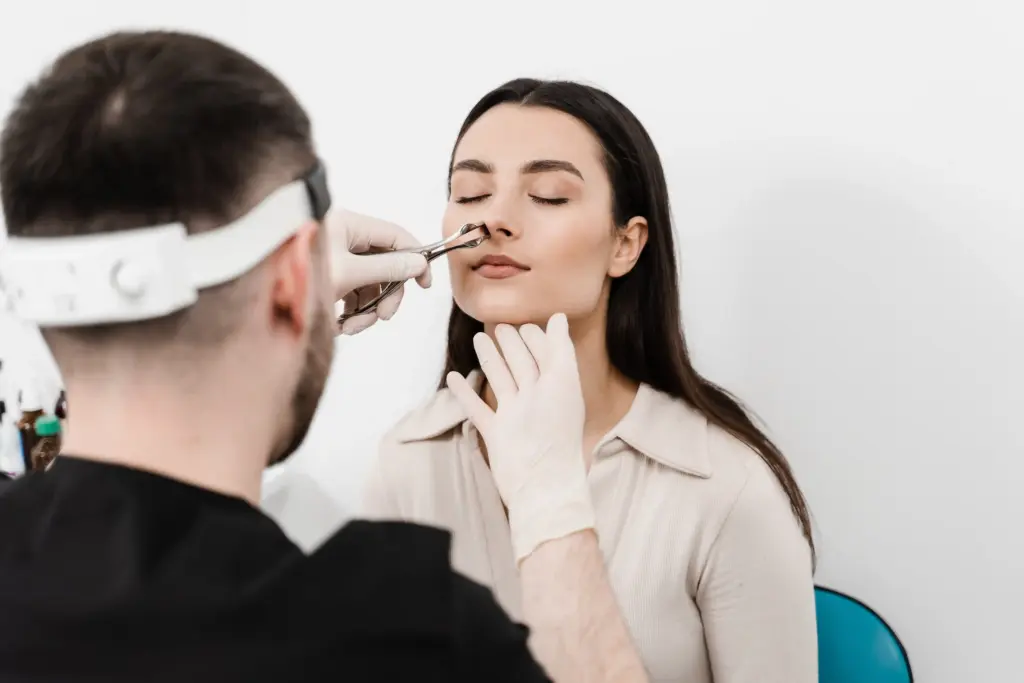
When someone with allergic rhinitis inhales an allergen, their immune system makes a specific antibody called Immunoglobulin E (IgE). These antibodies attach to mast cells in the tissues of the nose and eyes. When the allergen enters again, it binds to the IgE, causing the mast cells to burst and release histamine and other chemicals. This release leads to swelling, itching, and excess fluid.
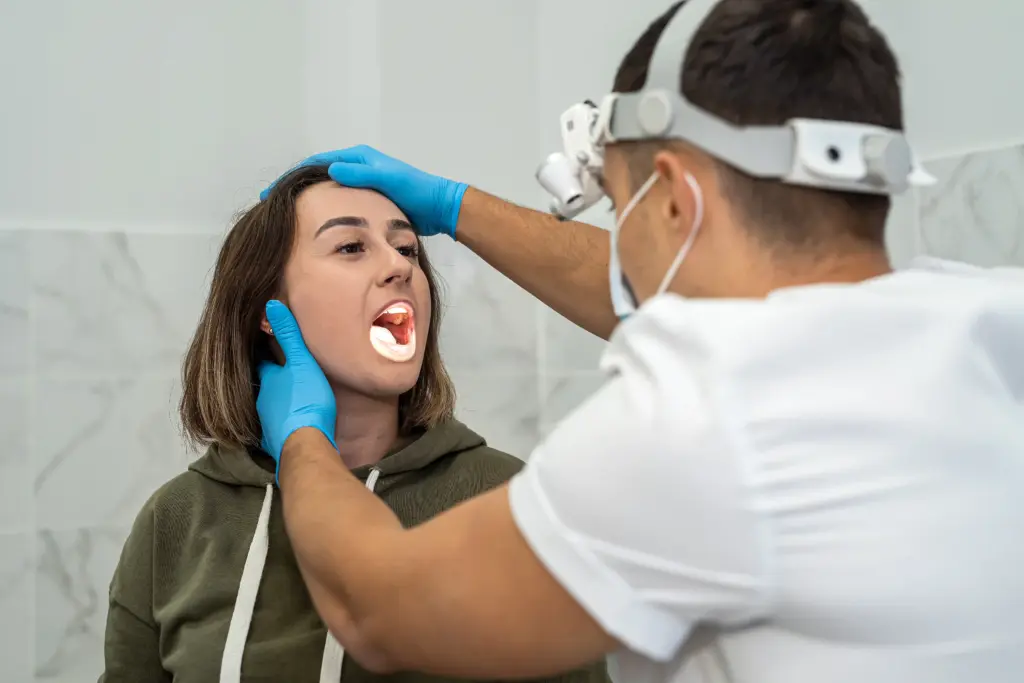
It is important to distinguish allergic rhinitis from other conditions. Although it shares symptoms with the common cold, a cold is caused by a virus, while allergic rhinitis results from an immune response to non-living particles.
It is also distinct from non-allergic rhinitis. Non-allergic rhinitis causes a runny nose without an immune reaction. It can be triggered by weather changes, spicy food, or strong smells, but it does not involve IgE antibodies.
Doctors group allergic rhinitis into two main types based on when they happen.
Some people may have both types. They might have symptoms all year that get worse during pollen season.
Beyond the seasonal types, doctors also classify the condition by how it affects daily life. This helps them decide on the best treatment.
Proper classification ensures that patients get the right level of care.
Eyes: Allergic conjunctivitis commonly develops, causing redness, itching, and tearing.
Ears: Nasal inflammation can obstruct the Eustachian tubes, leading to ear pressure, popping, or fluid buildup.
Throat: Post-nasal drip may trigger throat irritation or a persistent cough.
Lungs: The nasal–lung connection is well established; allergic rhinitis often coexists with asthma, and poorly controlled allergies can worsen asthma symptoms.
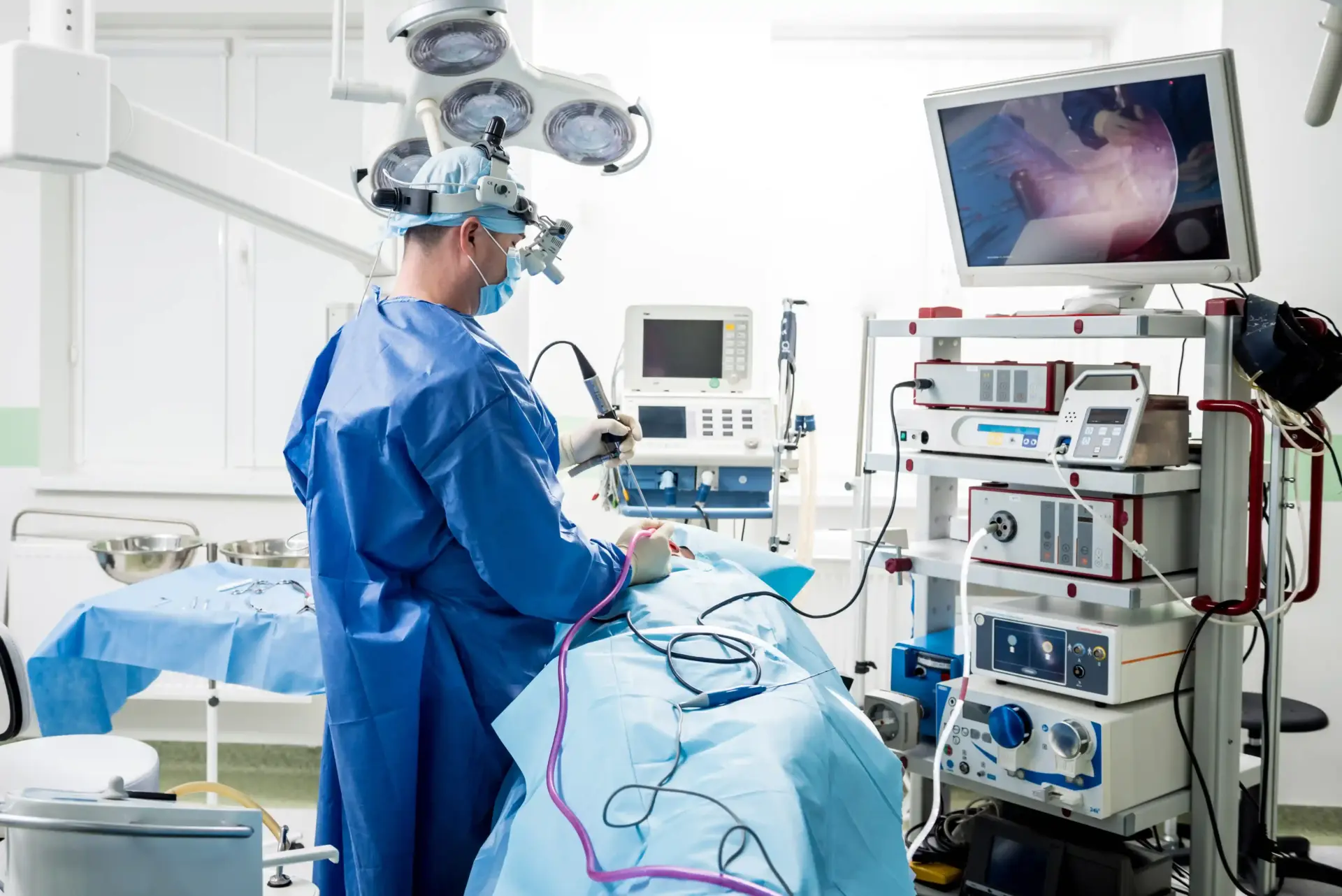
Allergic rhinitis, though often considered mild, carries significant medical and public-health consequences. It is one of the most common chronic conditions worldwide, contributing to considerable healthcare costs and reduced productivity. Its symptoms impair quality of life by disrupting sleep and causing fatigue, affecting concentration in children and work performance in adults. Effective management is therefore important for maintaining daily function and overall well-being.
In medicine, allergic rhinitis is often viewed as part of a bigger picture called the “Atopic March.” This concept describes how allergic diseases often progress in a child.
It frequently starts with eczema (skin rash) in infancy. Then, it may progress to food allergies. Later, the child develops asthma. Finally, they develop allergic rhinitis. Understanding this progression helps doctors predict and sometimes prevent future issues. Treating the nose can sometimes help protect the lungs.
Diagnosing and treating this condition involves several medical subspecialties. It is rarely a one-doctor job for severe cases.
The prevalence of allergic rhinitis is rising worldwide. Researchers believe this is due to climate change and urbanization. Warmer temperatures mean longer pollen seasons. Higher carbon dioxide levels make plants produce more potent pollen.
Urban pollution also plays a role. Diesel exhaust particles can attach to pollen grains. This makes the pollen more aggressive when it enters the nose. This combination of factors makes allergic rhinitis a growing priority for healthcare systems everywhere.

Send us all your questions or requests, and our expert team will assist you.
No, they are different conditions. Allergic rhinitis is inflammation caused by allergens like pollen or dust. A sinus infection (sinusitis) is usually caused by bacteria or viruses trapped in the sinuses. However, untreated allergies can lead to sinus infections by trapping mucus.
There is no absolute cure that works for everyone instantly. However, immunotherapy (allergy shots or drops) can alter the immune system. This can lead to long-term remission where symptoms disappear for years. Most treatments focus on managing symptoms effectively.
Yes, you can develop it at any time. It most commonly starts in childhood or the teen years. However, adults can develop new allergies later in life. This can happen if you move to a new location with different plants or get a new pet.
Yes, it can reduce your sense of smell. Chronic inflammation and swelling in the nasal passages can block air from reaching the smell receptors. This is usually temporary. Your sense of smell typically returns once the inflammation is treated and swelling goes down.
Yes, there are two main ways to test. A skin prick test involves placing a tiny amount of allergen on the skin to see if a bump forms. A blood test measures the level of IgE antibodies in your system. An ENT specialist can determine which test is best for you.






Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)