Endocrinology focuses on hormonal system and metabolic health. Learn about the diagnosis and treatment of diabetes, thyroid disorders, and adrenal conditions.
Send us all your questions or requests, and our expert team will assist you.

The clinical presentation of gigantism is dominated by rapid and excessive linear growth, but the symptoms extend far beyond simple height. Because growth hormone and IGF-1 receptors are located on cells throughout the body, the disorder manifests as a systemic syndrome affecting soft tissues, internal organs, metabolism, and the nervous system. The onset is often insidious; the acceleration in growth velocity may initially be mistaken for a vigorous pubertal growth spurt. However, as the condition progresses, the growth becomes disproportionate and is accompanied by a constellation of other physical and physiological signs.
Recognizing these symptoms early is critical for preventing irreversible skeletal deformities and metabolic damage. Parents and clinicians must look beyond the growth chart to identify the subtle markers of hormonal excess, such as widening hands, facial changes, or unexplained sweating. This section details the multifaceted symptomatic landscape of gigantism, ranging from obvious musculoskeletal changes to less visible metabolic and neurological disruptions.
The most hallmark sign of gigantism is distinctively rapid vertical growth. Children with this condition will often cross percentile lines on pediatric growth charts, eventually exceeding the 97th percentile and continuing to grow at a velocity that far outstrips their peers. This growth is driven by the relentless stimulation of the epiphyseal plates in the long bones of the legs and arms. Unlike a normal growth spurt which has a natural deceleration phase, the growth in gigantism is sustained and aggressive unless hormonally checked.
Height velocity refers to the rate at which a child grows over a specific period, usually measured in centimeters per year. In gigantism, this velocity remains elevated significantly longer than normal. A child might grow several inches in a few months. This rapid extension places immense strain on the body. The muscles and tendons struggle to keep pace with the lengthening bones, often leading to flexibility issues and susceptibility to injury. The sheer speed of growth can be alarming to parents, as clothing and shoes are outgrown in weeks rather than months.
The rapid lengthening of the skeleton often comes at a cost to structural integrity. The joints, particularly the knees and hips, bear the brunt of the increased leverage and body weight. Slipped capital femoral epiphysis, a condition where the ball of the hip joint slips off the thigh bone, is a risk due to the weakened growth plate structure. Scoliosis and kyphosis, curvatures of the spine, are also common as the vertebral column grows rapidly and sometimes unevenly. The bones themselves may be less dense initially due to the speed of turnover, increasing the risk of fractures or pain akin to severe growing pains.

Growth hormone does not discriminate between bone and soft tissue. Consequently, patients with gigantism experience significant thickening of the skin and enlargement of soft tissues. This often manifests as a coarsening of facial features. The nose may become broader, the lips thicker, and the forehead more prominent (frontal bossing). The tongue may enlarge (macroglossia), which can lead to speech difficulties or sleep apnea due to airway obstruction.
Internally, the organs are also subjected to this growth signal. Visceromegaly, or the enlargement of internal organs, is a serious concern. The heart, liver, kidneys, and spleen may all grow to sizes larger than normal. While a larger liver or spleen might not immediately cause failure, a larger heart (cardiomegaly) is structurally less efficient and prone to long-term failure. The enlargement of the vocal cords and sinuses typically results in a deepening of the voice, which may sound surprisingly mature for a child’s chronological age.

The excess of growth hormone acts as a counter-regulatory hormone to insulin. While insulin lowers blood sugar by helping cells absorb glucose, growth hormone raises blood sugar by promoting glucose release from the liver and inhibiting insulin sensitivity. This creates a state of insulin resistance, placing the child at a significantly higher risk for developing type 2 diabetes or impaired glucose tolerance. This metabolic strain is often present long before the diagnosis is made, manifesting as fatigue or excessive thirst.
Persistent exposure to high levels of growth hormone forces the pancreas to work overtime producing insulin to keep blood sugar stable. Over time, the beta cells of the pancreas may become exhausted. This can lead to overt diabetes mellitus, requiring dietary management or insulin therapy. Darkening of the skin in body folds, known as acanthosis nigricans, is a visible skin marker of this underlying insulin resistance and should prompt immediate metabolic evaluation in any child growing rapidly.
The presence of a pituitary tumor can disrupt the secretion of other pituitary hormones, specifically the gonadotropins (LH and FSH) that control puberty. Depending on the size of the tumor and the specific hormonal dynamics, a child may experience delayed puberty or, conversely, precocious (early) puberty. The compression of the pituitary stalk can prevent the signals for sexual maturation from being sent. This creates a clinical picture of a very tall but sexually underdeveloped adolescent. In other cases, co-secretion of prolactin by the tumor can cause distinct symptoms such as galactorrhea (breast milk production) and menstrual irregularities in females.
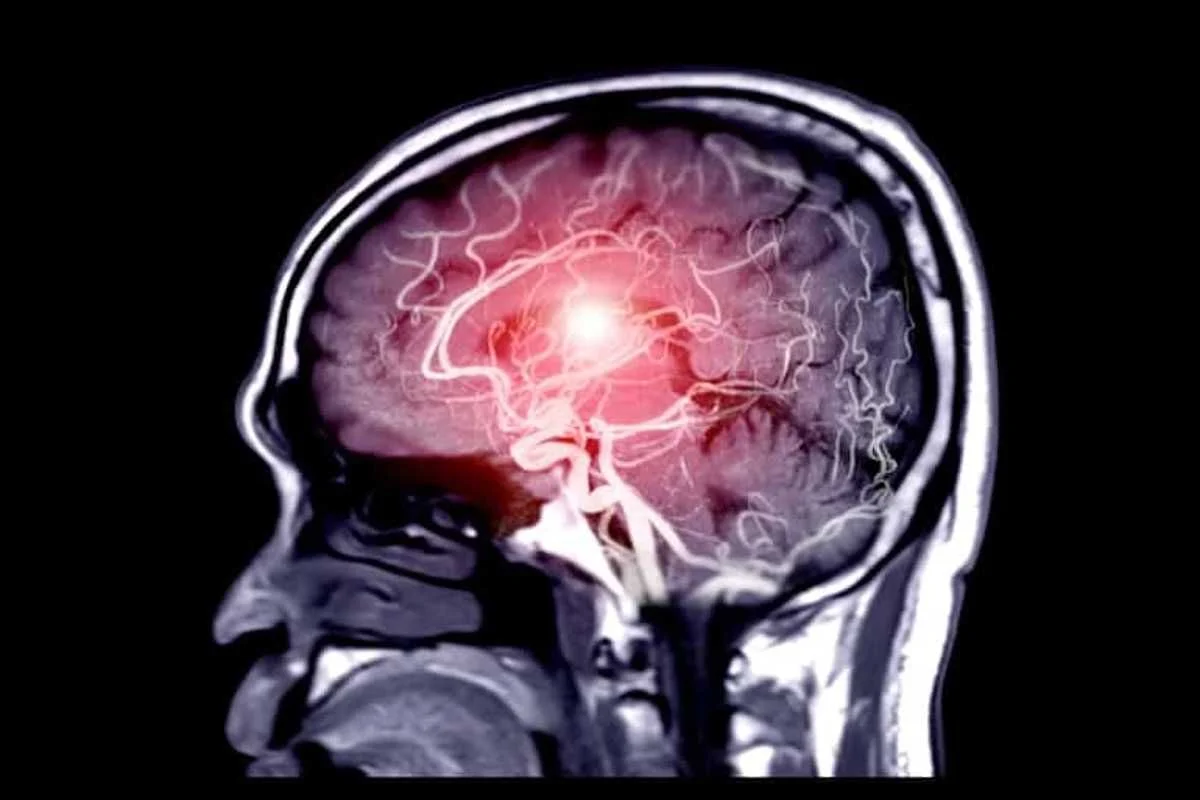
As the pituitary adenoma expands within the sella turcica, it functions as a space-occupying lesion in the brain. The primary neurological symptom is a persistent headache. These headaches are often described as deep, aching, and resistant to standard pain relief medications. They result from the stretching of the dural membrane that covers the pituitary gland. The severity of the headache often correlates with the rate of tumor growth rather than the absolute size.
Visual disturbances are the second major neurological complication. The optic chiasm, where the optic nerves cross, is located directly above the pituitary gland. Upward growth of the tumor compresses these nerves. The classic pattern of vision loss is bitemporal hemianopsia, which is the loss of peripheral vision in both eyes. Patients may report bumping into door frames or having a “tunnel vision” effect. If the compression is severe and prolonged, optic nerve atrophy can occur, potentially leading to permanent visual impairment.

The cardiovascular system is heavily burdened in gigantism. The heart must pump blood through a significantly larger body surface area and vascular network. This increased demand leads to left ventricular hypertrophy, where the main pumping chamber of the heart thickens. While initially an adaptive mechanism, this thickening eventually reduces the heart’s flexibility and efficiency.
Hypertension, or high blood pressure, is frequently observed in these young patients. The combination of increased fluid volume—driven by the sodium-retaining effects of growth hormone—and vascular stiffness creates a hypertensive state. If left unmanaged, this contributes to early-onset heart disease. Valve abnormalities are also more common, likely due to the overgrowth of connective tissue within the heart structures.

The psychological toll of gigantism is profound and often underappreciated. Children and adolescents are acutely sensitive to physical appearance and peer acceptance. Being dramatically taller than peers can lead to feelings of isolation, self-consciousness, and body dysmorphia. The rapid physical changes can be frightening, and the attention drawn by their height is often unwanted.

Send us all your questions or requests, and our expert team will assist you.
The most common early signs are rapid height growth that exceeds normal rates, significantly increasing shoe and glove sizes, and a noticeable coarsening of facial features.
Yes, many children experience joint pain, back pain, and growing pains due to rapid skeletal expansion, as well as frequent headaches caused by tumor pressure.
The pituitary tumor can press on the optic nerves located nearby, leading to a loss of peripheral vision or general visual clarity if not treated.
Yes, patients often experience excessive sweating (hyperhidrosis) and may have thickened, oily skin due to the effects of excess growth hormone on skin glands.
Despite the rapid growth, children often feel profound fatigue and weakness because the body is expending immense energy on growth and metabolism is disrupted.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)