Endocrinology focuses on hormonal system and metabolic health. Learn about the diagnosis and treatment of diabetes, thyroid disorders, and adrenal conditions.
Send us all your questions or requests, and our expert team will assist you.
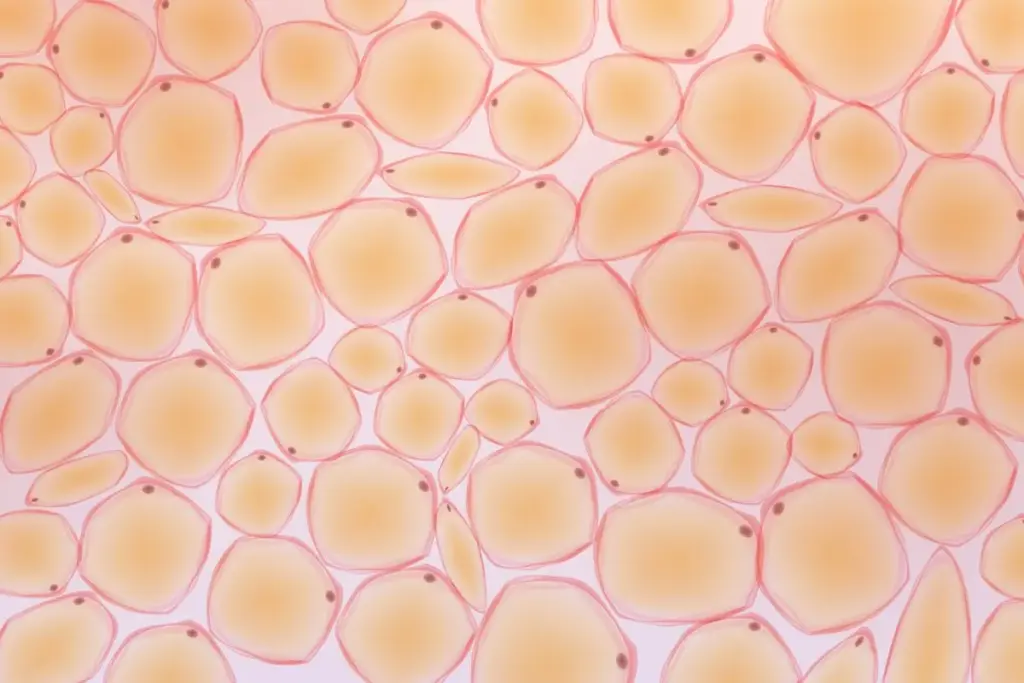
Obesity is recognized in modern medicine not merely as a consequence of lifestyle choices but as a complex, chronic, and relapsing disease process characterized by excessive accumulation of body fat that impairs health. This condition represents a significant departure from normal physiological homeostasis, involving intricate interactions between genetic susceptibility, environmental factors, and metabolic regulation. The historical perception of weight as a simple balance of caloric intake versus expenditure has evolved into a sophisticated understanding of neurohormonal pathways that actively defend body weight. As a global health challenge, it requires a definition that transcends aesthetic concerns and focuses on the pathological impact of adipose tissue on organ systems. Medical professionals now utilize precise classification systems to categorize severity and guide therapeutic interventions, moving away from stigma and toward evidence-based management. Understanding the fundamental definition and scope of this condition is the first critical step in addressing its multifactorial nature and implementing effective long-term care strategies.
The fundamental biology of weight regulation involves a highly integrated system designed to preserve energy stores for survival. In the context of this chronic disease, the regulatory mechanisms that typically maintain energy balance become dysregulated, leading to a persistent positive energy balance and subsequent fat storage. Adipose tissue, once thought to be an inert storage depot for triglycerides, is now understood to be a dynamic endocrine organ that secretes bioactive peptides and hormones. These secretions influence appetite, energy expenditure, and insulin sensitivity across the entire body.
When the expansion of adipose tissue exceeds its vascular supply or structural capacity, it leads to cellular stress, inflammation, and dysfunction. This pathogenic adiposity drives the metabolic complications associated with the disease. The biological basis also encompasses the gut-brain axis, where signals from the gastrointestinal tract communicate with the hypothalamus to regulate hunger and satiety. Disruptions in this communication network can lead to a biological drive to consume food that overrides conscious intent. Consequently, the disease state is maintained by powerful physiological forces that resist weight loss, explaining why voluntary calorie restriction often fails to produce sustained results without addressing the underlying biological drivers.

Clinical practice relies on standardized classification systems to stratify risk and determine appropriate treatment pathways. The most widely utilized metric is the Body Mass Index, a calculation based on an individual’s height and weight. While it has limitations regarding body composition differentiation, it serves as a functional screening tool for population health. The classification is divided into distinct categories, beginning with overweight status and progressing through three classes of increasing severity.
Beyond simple numerical values, modern staging systems also incorporate the presence and severity of weight-related complications. These functional staging systems provide a more nuanced picture of a patient’s health status than weight alone. For instance, an individual with a lower BMI but significant metabolic disease may require more aggressive intervention than a person with a higher BMI but no immediate metabolic abnormalities. This shift towards a complications-centric diagnosis ensures that treatment is prioritized based on health impact rather than just body size.
While the Body Mass Index is the standard for initial assessment, it does not distinguish between muscle mass and fat mass, nor does it account for fat distribution. Athletes or individuals with high muscularity may be misclassified as having excess adiposity when their metabolic health is optimal. Conversely, individuals with normal weight may have excessive visceral fat, placing them at risk for metabolic syndrome. Therefore, clinical evaluation often supplements this metric with waist circumference and body composition analysis to obtain a true representation of health risk.
The location of fat storage is as critical as the total amount of fat. Visceral adipose tissue, which accumulates deep within the abdominal cavity and surrounds vital organs, is metabolically active and particularly harmful. Unlike subcutaneous fat, visceral fat releases free fatty acids and inflammatory cytokines directly into the portal circulation, affecting the liver and systemic metabolism. Identifying central adiposity is essential for accurate risk stratification, as it is a strong predictor of cardiovascular disease and type 2 diabetes independent of total body weight.
The progression from healthy weight to a disease state involves a cascade of pathophysiological changes that alter how the body processes and stores energy. At the cellular level, adipocytes undergo hypertrophy and hyperplasia, leading to a state of chronic low-grade inflammation. This systemic inflammation is a hallmark of the condition and contributes to the development of insulin resistance, where cells become less responsive to the hormone insulin. As a result, the pancreas must produce higher levels of insulin to maintain blood glucose control, eventually straining pancreatic function.
Furthermore, the dysregulation extends to lipid metabolism, often resulting in elevated triglycerides and low levels of high-density lipoprotein cholesterol. These metabolic disturbances create a pro-atherogenic environment that damages blood vessels and increases the risk of cardiovascular events. The pathophysiology also involves oxidative stress, where an imbalance between free radicals and antioxidants leads to cellular damage. This stress impacts the mitochondria, the energy powerhouses of cells, reducing their efficiency and further impairing metabolic flexibility. Understanding these deep physiological changes is crucial for recognizing that the disease impacts nearly every organ system, from the liver and heart to the brain and kidneys.

The prevalence of this metabolic disease has reached epidemic proportions in many developed nations, presenting a profound challenge to public health systems. Data indicates a steady rise in rates across all age groups, genders, and socioeconomic demographics, although disparities persist. This upward trend is driven by a complex convergence of factors, including the widespread availability of energy-dense, nutrient-poor foods and a built environment that encourages sedentary behavior. The impact is not just on individual health but also places a tremendous strain on healthcare infrastructure due to the management of associated chronic conditions.
Monitoring these epidemiological trends allows health authorities to allocate resources effectively and design targeted intervention programs. It highlights the urgent need for systemic changes in food policy, urban planning, and healthcare delivery to reverse the trajectory. The focus has shifted from solely treating individual cases to implementing population-level strategies that create environments conducive to metabolic health.

The development of this disease is rarely due to a single cause; rather, it is the result of a dynamic interplay between an individual’s genetic makeup and their environment. Genetic predisposition plays a substantial role in determining susceptibility, influencing factors such as metabolic rate, fat storage efficiency, and food seeking behavior. Genome-wide association studies have identified numerous genetic variants linked to body mass regulation, suggesting that for many, the biological deck is stacked against maintaining a lean physique in the modern environment.
However, genetics alone do not explain the rapid rise in prevalence observed in recent decades. The obesogenic environment acts as a trigger for these genetic predispositions. Factors such as the ubiquity of ultra-processed foods, aggressive marketing, and the reduction of physical activity in daily life interact with genetic vulnerabilities to drive weight gain. Epigenetics, the study of how behaviors and environment can cause changes that affect the way genes work, also plays a role. Maternal health and nutrition during pregnancy can imprint metabolic traits on the offspring, potentially programming them for weight issues later in life. This intersection of nature and nurture underscores the complexity of the disease and the necessity for multifaceted prevention and treatment approaches.

Viewing this condition as a multi-factorial chronic disease transforms the clinical approach from acute weight loss attempts to long-term management. Like hypertension or diabetes, it requires continuous care, monitoring, and adjustment of therapeutic strategies. The “chronic” designation acknowledges that the physiological changes associated with the disease are persistent and that the body has powerful counter-regulatory mechanisms that resist weight loss and promote weight regain. This biological reality explains why short-term interventions typically yield temporary results.
Recognizing the multifactorial nature means addressing the diverse contributors, including psychological factors like stress and trauma, social determinants like income and education, and biological drivers like hormonal imbalances. Effective management often requires a team-based approach involving physicians, dietitians, behavioral health specialists, and exercise physiologists. This comprehensive model ensures that all aspects of the patient’s health are considered, moving beyond simplistic advice to eat less and move more. It validates the patient’s experience and reduces the stigma often associated with the struggle to manage weight, framing it correctly as a medical issue requiring medical solutions.

Send us all your questions or requests, and our expert team will assist you.
It is classified as a disease because it involves specific physiological dysfunction and dysregulation of body weight pathways that impair health. The body actively defends a higher weight through hormonal and neural signals, making it a complex medical condition distinct from simple willpower.
Severity is primarily categorized using Body Mass Index classes, ranging from Class I to Class III, which correlates with increasing health risk. Physicians also evaluate the presence of weight-related complications like diabetes or hypertension to determine the clinical stage.
Visceral fat is metabolically active and releases inflammatory substances directly into the portal blood system, affecting the liver and systemic metabolism. Its accumulation around internal organs is strongly linked to insulin resistance, heart disease, and other metabolic disorders.
Genetics can significantly increase susceptibility by influencing appetite and metabolism, but they do not guarantee the disease. Environmental factors and lifestyle behaviors interact with genetic predisposition to determine whether the condition develops and progresses.
The primary goal is to improve health outcomes and quality of life by treating weight-related complications, rather than focusing solely on cosmetic weight loss. Successful management involves sustainable lifestyle changes, often supported by medical or surgical therapies to maintain metabolic health.




Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)