Endocrinology focuses on hormonal system and metabolic health. Learn about the diagnosis and treatment of diabetes, thyroid disorders, and adrenal conditions.
Send us all your questions or requests, and our expert team will assist you.
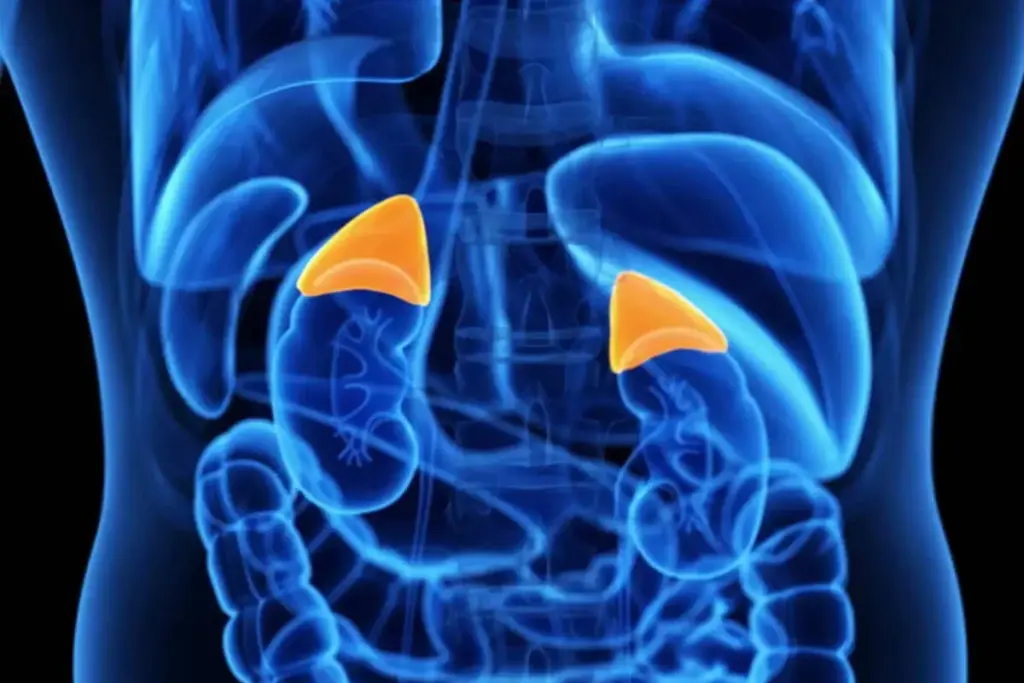
Diagnosing pheochromocytoma requires a systematic and meticulous approach, combining biochemical evidence of catecholamine excess with anatomical localization of the tumor. Because the symptoms can be nonspecific, the diagnostic pathway begins with biochemical testing to confirm the presence of a secretory tumor before proceeding to imaging. This sequence is critical to avoid unnecessary radiation and to interpret imaging findings in the correct context. Once a biochemical diagnosis is established, advanced imaging modalities are employed to locate the tumor and assess for metastatic spread. The evaluation also encompasses genetic testing to identify potential hereditary syndromes, which impacts management and family screening. This section details the rigorous process of confirming the diagnosis, localizing the lesion, and preparing for treatment.
The cornerstone of pheochromocytoma diagnosis is the demonstration of elevated catecholamine metabolites in the blood or urine. Catecholamines are metabolized into metanephrines within the tumor cells and other tissues. Because catecholamine secretion can be episodic, measuring the parent hormones (epinephrine, norepinephrine) can sometimes yield false-negative results if blood is drawn between attacks. However, metanephrines are produced continuously by the tumor and leak into the circulation, providing a more stable and reliable marker of tumor activity. Therefore, measuring free metanephrines in plasma or fractionated metanephrines in urine is the recommended initial screening step.
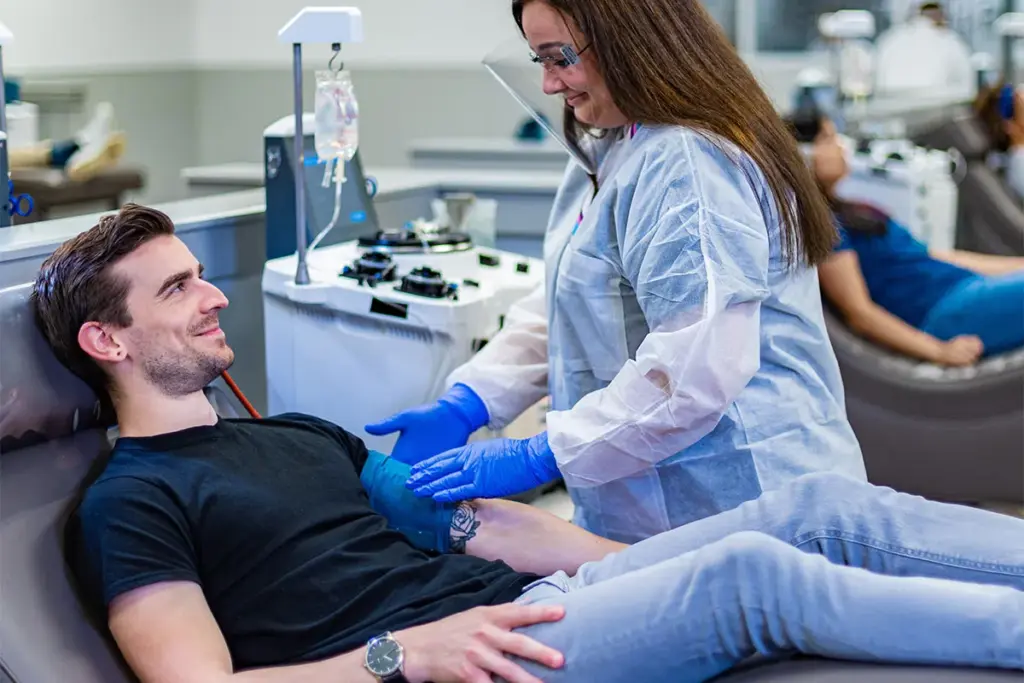
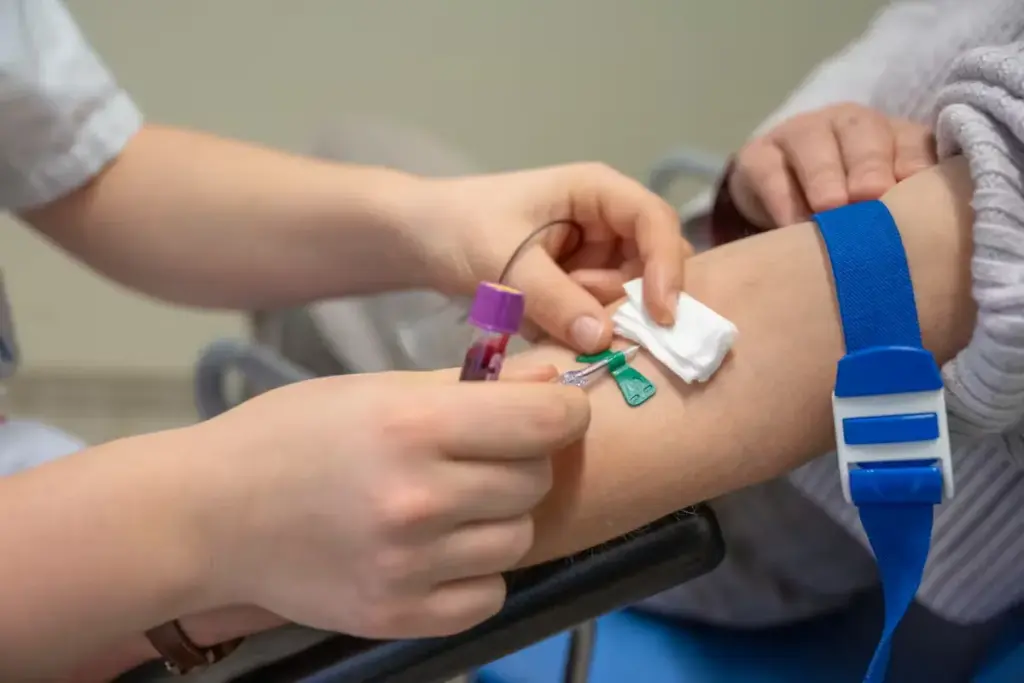
The measurement of plasma free metanephrines is considered the most sensitive test for detecting pheochromocytoma. This blood test measures the levels of normetanephrine and metanephrine. A result showing levels significantly above the upper limit of normal is highly suggestive of the disease. Blood needs to be drawn with the patient in a supine position, having rested for at least 20 to 30 minutes, to minimize stress-induced catecholamine release which could lead to false positives. The high sensitivity of this test means that a negative result reliably excludes the presence of a catecholamine-secreting tumor in most symptomatic patients.
Alternatively, or as a confirmatory test, a 24-hour urine collection for fractionated metanephrines and catecholamines can be performed. This test integrates hormone production over a full day, which can be helpful in patients with sporadic secretion patterns. It measures total metanephrine and normetanephrine output. Proper collection technique is vital; the urine must be kept cool and acidic to prevent degradation of the catecholamines. While slightly less sensitive than the plasma test, the urinary test has high specificity and is an excellent tool for confirming positive plasma results or for use in settings where plasma assays are not available.

Once biochemical testing has confirmed the diagnosis, the next step is to locate the tumor using anatomical imaging. The adrenal glands are the primary focus, given that the vast majority of these tumors arise there. Computed Tomography (CT) and Magnetic Resonance Imaging (MRI) are the standard modalities used for localization. The choice between CT and MRI often depends on the patient’s characteristics, such as age, pregnancy status, and potential for radiation exposure, as well as the institution’s expertise. Both modalities provide detailed anatomical information necessary for surgical planning.
A CT scan of the abdomen and pelvis with and without contrast is typically the first-line imaging study. Pheochromocytomas usually appear as solid, heterogeneous masses in the adrenal bed. They may show areas of necrosis, hemorrhage, or calcification. On non-contrast scans, they tend to have higher attenuation (density) compared to benign adrenal adenomas. The administration of contrast helps to delineate the tumor’s vascularity and relationship to adjacent structures like the vena cava and renal vessels. CT offers excellent spatial resolution, which is crucial for the surgeon to understand the anatomy prior to resection.
MRI is an extremely valuable alternative, particularly for children, pregnant women, or patients with contrast allergies. Pheochromocytomas have a characteristic appearance on T2-weighted MRI images, often described as a “light bulb” sign due to their high signal intensity. This feature can help distinguish them from other adrenal masses. MRI is also superior in delineating the tissue planes and identifying extra-adrenal paragangliomas, especially those located near the spine or major blood vessels. Its lack of ionizing radiation makes it the preferred modality for patients requiring repeated imaging over a lifetime.
When anatomical imaging is equivocal, or when there is a suspicion of multifocal or metastatic disease, functional imaging is employed. These nuclear medicine scans use radiolabeled molecules that specifically target chromaffin cells. MIBG (metaiodobenzylguanidine) scintigraphy is a classic functional test where a radioisotope similar to norepinephrine is injected and taken up by the tumor cells. More recently, PET-CT scans using gallium-68 DOTATATE have emerged as a highly sensitive tool, particularly for detecting metastatic lesions and hereditary paragangliomas. These functional scans essentially “light up” the metabolic activity of the tumor, confirming that an anatomical mass is indeed the source of the excess hormones.
Given the strong hereditary component of pheochromocytoma, genetic testing is now recommended for all patients diagnosed with the condition, regardless of family history or age. Identifying a germline mutation changes the clinical management significantly. For instance, patients with MEN 2 or VHL mutations often have bilateral adrenal tumors or are at risk for tumors in other organs. Knowing the genetic status allows for screening of family members who may also be carriers. A genetic counselor plays a vital role in explaining the implications of positive results, guiding the testing of relatives, and helping the patient understand the long-term risks.
The differential diagnosis for pheochromocytoma is broad due to its nonspecific symptoms. Clinicians must rule out other causes of secondary hypertension such as renal artery stenosis or hyperaldosteronism. Endocrine disorders like hyperthyroidism, carcinoid syndrome, and hypoglycemia can mimic the adrenergic symptoms. Anxiety disorders, panic attacks, and drug withdrawal states are also common confounders. The rigorous use of biochemical testing helps to objectively separate pheochromocytoma from these other conditions. It is important to avoid premature diagnosis based solely on symptoms without biochemical confirmation.
One of the challenges in diagnosing pheochromocytoma is the potential for medications to interfere with biochemical assays, leading to false-positive results. Many common drugs, including tricyclic antidepressants, certain antipsychotics, decongestants, and even acetaminophen, can alter catecholamine metabolism or interfere with the laboratory assay. A thorough medication review is essential before testing. Ideally, interfering medications should be tapered or discontinued for a period before blood or urine collection, under the supervision of a physician, to ensure the accuracy of the results.

Send us all your questions or requests, and our expert team will assist you.
The measurement of plasma free metanephrines is widely considered the most sensitive initial screening test for detecting the presence of the tumor.
Lying down and resting ensures that stress or physical activity does not artificially raise your hormone levels, which could lead to a false positive result.
No, a CT scan can show a mass, but biochemical tests are needed to prove that the mass is producing excess hormones and is actually a pheochromocytoma.
Since up to 40 percent of cases are genetic, testing helps identify hereditary syndromes that require monitoring of other organs and screening of family members.
Yes, many medications like antidepressants and decongestants can interfere with the test, so your doctor may adjust your meds before the test.




Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)