Endocrinology focuses on hormonal system and metabolic health. Learn about the diagnosis and treatment of diabetes, thyroid disorders, and adrenal conditions.
Send us all your questions or requests, and our expert team will assist you.
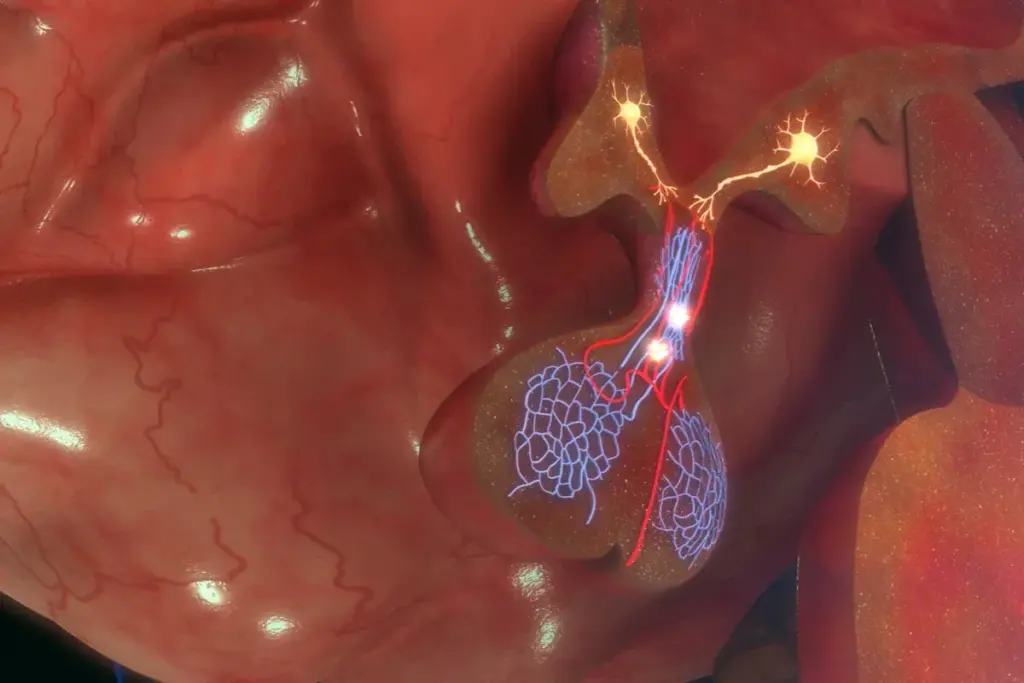
The pituitary gland, often referred to as the master gland of the human endocrine system, plays a pivotal role in regulating critical physiological processes, including growth, metabolism, and reproduction. A pituitary tumor, clinically known as a pituitary adenoma, represents an abnormal growth of cells within this small but significant gland located at the base of the brain. These tumors are generally benign, meaning they are non-cancerous and do not metastasize to other parts of the body, yet their impact on health can be profound due to their strategic location and hormonal influence. Understanding the nature of these tumors requires a comprehensive examination of their anatomical context, classification, and the biological mechanisms that drive their development. Patients diagnosed with a pituitary mass often face a complex clinical landscape involving endocrinological assessments and neurosurgical consultations. This section establishes the foundational knowledge necessary to navigate the complexities of pituitary tumors, defining their scope, prevalence, and the fundamental distinction between functional and non-functional growths, providing a clear starting point for patients and caregivers seeking to understand this medical condition.
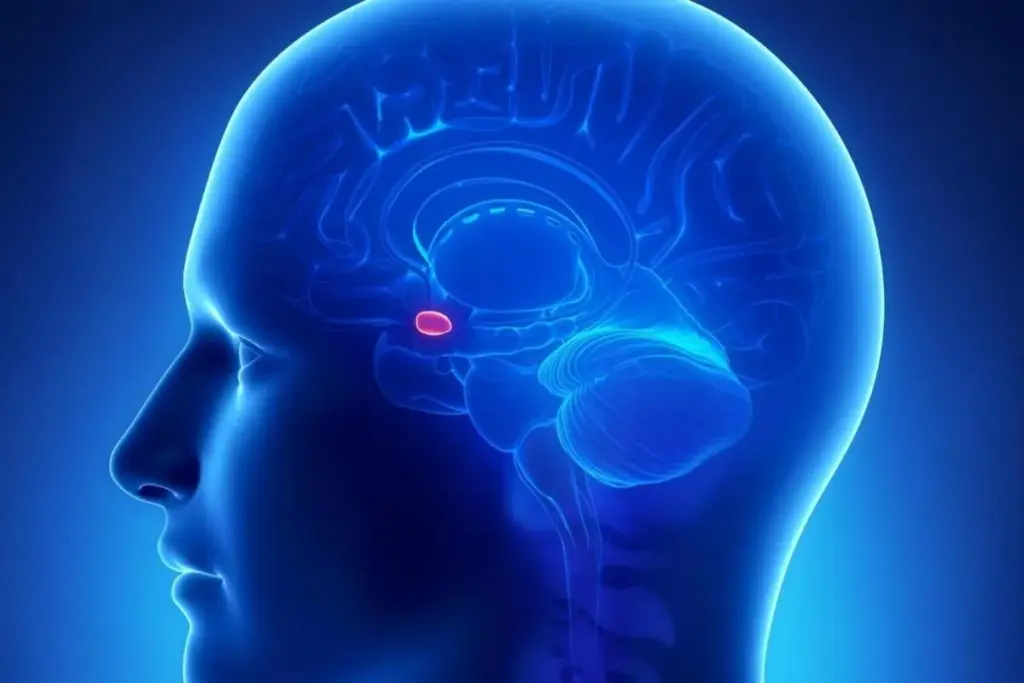
The pituitary gland is a pea-sized organ housed within the sella turcica, a bony depression in the sphenoid bone at the base of the skull. Despite its diminutive size, it exerts overarching control over the entire endocrine system by secreting hormones that signal other glands to produce their respective hormones. This gland is connected to the hypothalamus, a region of the brain that integrates neural and endocrine signals, ensuring that the body maintains homeostasis in response to internal and external stressors. The intricate relationship between the hypothalamus and the pituitary gland forms the hypothalamic-pituitary axis, which is the central command center for hormonal regulation. Any disruption in this area, such as the growth of a tumor, can mechanically compress surrounding structures or alter the delicate balance of hormone secretion, leading to widespread systemic effects.
The gland is anatomically divided into two distinct lobes: the anterior lobe, or adenohypophysis, and the posterior lobe, or neurohypophysis. The anterior lobe is responsible for synthesizing and releasing the majority of pituitary hormones, including growth hormone, prolactin, and adrenocorticotropic hormone. It is derived from ectodermal tissue and is highly vascularized to facilitate the rapid transport of hormones into the bloodstream. The posterior lobe, conversely, is an extension of neural tissue from the hypothalamus and stores hormones like oxytocin and vasopressin. The proximity of the pituitary gland to the optic chiasm, where the optic nerves cross, is of critical clinical importance, as upward growth of a tumor can impinge upon these nerves, causing characteristic visual impairments.
Functionally, the pituitary gland serves as the body’s thermostat for hormonal activity. It monitors the levels of circulating hormones and adjusts its output accordingly through negative feedback loops. For instance, if thyroid hormone levels drop, the pituitary releases thyroid-stimulating hormone to prompt the thyroid gland to increase production. This regulatory capability extends to the adrenal glands, the gonads, and the liver. The proper functioning of these feedback mechanisms is essential for maintaining metabolic rate, stress response, and reproductive viability. A tumor within the pituitary can disrupt these pathways either by hypersecreting a specific hormone, thereby ignoring feedback inhibition, or by compressing normal pituitary tissue, leading to a deficiency in one or more essential hormones.

Pituitary adenomas are the most common type of pituitary disorder, accounting for a significant percentage of all intracranial tumors. These growths originate from the epithelial cells of the anterior pituitary lobe. While the term tumor can evoke fear of malignancy, the vast majority of pituitary adenomas remain localized and grow slowly over years. They are distinct from other sellar masses such as craniopharyngiomas or Rathke’s cleft cysts, which have different developmental origins and treatment protocols. The definition of a pituitary adenoma encompasses a spectrum of behaviors, from small, incidental findings that require no intervention to large, aggressive masses that invade the cavernous sinuses or compress the brain tissue.

One of the primary distinctions in the classification of pituitary tumors is whether the tumor cells are biologically active. Functional tumors, also known as secreting tumors, produce excess amounts of one or more pituitary hormones. This hypersecretion leads to specific clinical syndromes that are often the presenting complaint of the patient. Conversely, non-functional tumors do not produce biologically active hormones. These masses often grow silently until they reach a size sufficient to cause neurological symptoms through mass effect. The management strategies for these two categories differ significantly, with functional tumors often amenable to medical therapy targeting the hormone pathways, while non-functional tumors are primarily managed surgically if they threaten vision or neurological function.
Secreting tumors are further categorized by the specific hormone they produce. A prolactinoma, which secretes prolactin, is the most common type and can cause reproductive dysfunction and galactorrhea. Somatotroph adenomas secrete growth hormone, leading to acromegaly in adults or gigantism in children. Corticotroph adenomas produce adrenocorticotropic hormone, resulting in Cushing’s disease. Each of these subtypes presents with a unique constellation of symptoms driven by the excess hormone. For example, the metabolic changes seen in Cushing’s disease are distinct from the skeletal overgrowth of acromegaly. Early identification of the specific hormone excess is vital for targeted treatment and prognosis.
Non-functional adenomas, also termed null-cell adenomas, do not result in a clinical syndrome of hormone excess. Instead, they are often detected when the patient undergoes imaging for an unrelated reason or when the tumor grows large enough to cause headaches or vision loss. Because they lack a hormonal marker, they can be more challenging to diagnose in the early stages. The primary concern with non-secreting masses is their physical expansion. As they enlarge, they can compress the normal pituitary gland, leading to hypopituitarism, or press against the optic chiasm. Treatment focuses on relieving this pressure and preserving the function of the remaining normal gland tissue.
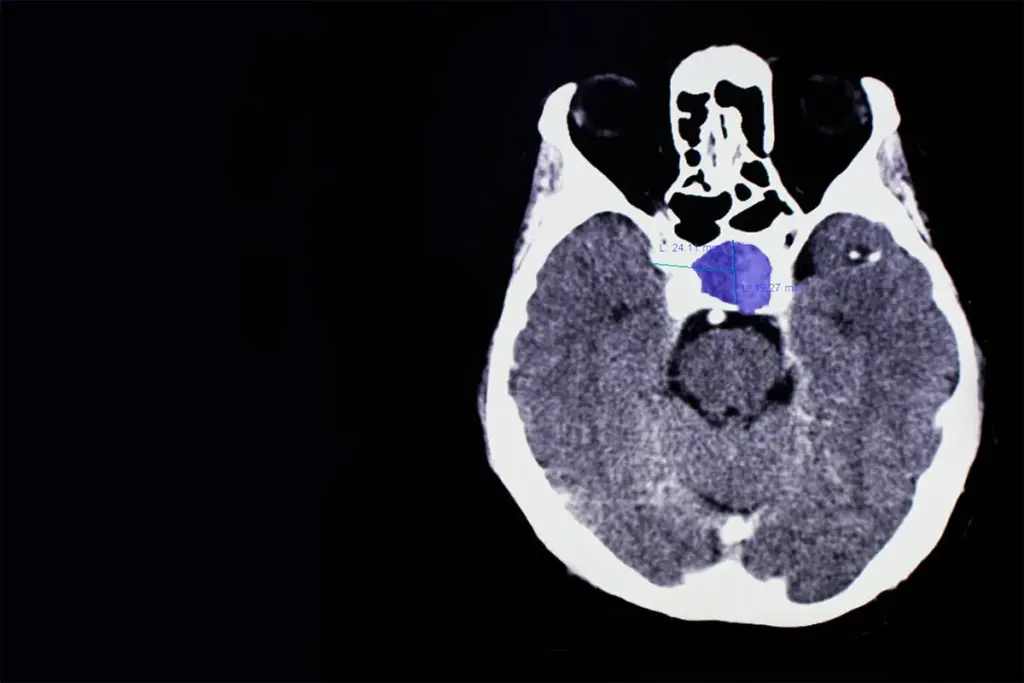
The size of a pituitary tumor is a key determinant in its classification and management. Tumors measuring less than ten millimeters in diameter are classified as microadenomas. These are often confined within the sella turcica and are less likely to cause mass effect symptoms, although they can still be hormonally active and symptomatic. Tumors measuring ten millimeters or larger are termed macroadenomas. Macroadenomas have a higher propensity to extend beyond the sella, potentially invading the cavernous sinuses or compressing the optic apparatus. Giant adenomas, those exceeding four centimeters, present significant surgical challenges and require a multidisciplinary approach. Invasiveness refers to the tumor’s extension into surrounding structures, such as the sphenoid sinus or brain tissue, which can complicate surgical removal and increase the risk of recurrence.

Pituitary tumors are relatively common, with autopsy studies suggesting they may be present in a significant portion of the population as incidental findings. Clinically significant pituitary tumors, however, are less frequent. They affect individuals of all ages but are most commonly diagnosed in adults between the third and sixth decades of life. There is no strong gender predilection for pituitary tumors overall, although specific subtypes like prolactinomas are more frequently diagnosed in women, while null-cell adenomas are slightly more common in men. Understanding the epidemiology helps clinicians maintain a high index of suspicion when patients present with vague symptoms like unexplained headaches or menstrual irregularities.
The biological mechanisms driving the development of pituitary tumors involve a complex interplay of genetic mutations and cellular dysregulation. Unlike many other cancers, common oncogenes are rarely mutated in pituitary adenomas. Instead, the pathogenesis is often linked to alterations in cell cycle regulation, growth factor signaling, and tumor suppressor genes. Monoclonality is a hallmark of these tumors, indicating they arise from a single mutated cell that undergoes uncontrolled expansion. Research into the molecular pathways, such as the aryl hydrocarbon receptor interacting protein gene, has provided insights into familial cases. Understanding these pathways is not only academic but paves the way for developing targeted pharmacological therapies that can inhibit tumor growth or hormone secretion at the cellular level.

Send us all your questions or requests, and our expert team will assist you.
A functional tumor produces excess hormones that cause specific symptoms related to that hormone. A non-functional tumor does not produce hormones and usually causes symptoms by pressing on nearby structures.
No, pituitary tumors are almost always benign adenomas and are not classified as brain cancer. They do not spread to other parts of the body like malignant cancers do.
It is very rare for a pituitary tumor to disappear without treatment, although some may stop growing. Spontaneous shrinkage can occur due to apoplexy, but medical evaluation is always required.
They are quite common, with some studies suggesting they exist in up to 20 percent of people. However, the majority are tiny, cause no symptoms, and never require treatmen
Yes, with appropriate management and monitoring, most patients lead normal, active lives. Treatment is effective at controlling hormone levels and preserving vision and brain function.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)