Geriatrics addresses the health needs of older adults, focusing on frailty, dementia, falls, and chronic disease management.
Send us all your questions or requests, and our expert team will assist you.
What is Alzheimer’s disease, and how does it differ from the natural aging process? Alzheimer’s is a progressive neurodegenerative disorder that serves as the leading cause of dementia worldwide, accounting for 60-80% of all cases. It is characterized by the gradual accumulation of toxic proteins in the brain, which disrupts communication between neurons and eventually leads to widespread cellular death. In the landscape of modern geriatrics, Alzheimer’s is viewed not just as memory loss, but as a systemic failure of the brain’s biological resilience. As brain tissue undergoes atrophy (shrinking), individuals experience a steady decline in cognitive, behavioral, and physical functions.
While age is the primary risk factor, Alzheimer’s is a pathological condition rather than a normal consequence of growing older. In regenerative medicine, we focus on the “Neuro-metabolic” health of the brain, identifying how chronic inflammation and vascular decline accelerate the progression of the disease. Understanding this condition is the first step toward moving beyond uncertainty and fear. By recognizing Alzheimer’s as a physical illness of the brain, families can better navigate the journey of care, focusing on preserving the patient’s dignity and maximizing their functional independence.
The symptoms of Alzheimer’s disease extend far beyond simple forgetfulness; they represent a fundamental change in the brain’s “Executive Suite.” In the early stages, symptoms often manifest as Mild Cognitive Impairment (MCI), where a senior may struggle to find the right words or lose track of familiar items. As the disease transitions into the moderate phase, we observe significant behavioral shifts, spatial disorientation, and difficulty performing complex, multi-step tasks. These clinical markers reflect the spreading of cellular damage from the hippocampus to the cerebral cortex.
It is vital to identify when memory lapses become a pathological condition. Unlike normal age-related changes such as occasionally forgetting a name Alzheimer’s involves a failure of the brain’s “Retrieval and Storage” systems. Conditions like Aphasia (language loss), Apraxia (motor skill loss), and Agnosia (failure to recognize objects) are clear indicators of neurodegeneration. Identifying these conditions early allows for more effective intervention and the implementation of safety protocols within the home environment.
Environmental factors and cardiovascular health also play a major role. Conditions that damage the heart or blood vessels, such as high blood pressure, heart disease, stroke, and diabetes, can increase the risk of developing Alzheimer’s. Additionally, lifestyle choices regarding diet, physical activity, and social engagement are increasingly recognized as critical components in either accelerating or delaying the onset of symptoms.

The diagnostic process for Alzheimer’s has evolved from observation to precision-based Biomarker Identification. We perform a comprehensive evaluation that begins with neuropsychological testing to map cognitive strengths and weaknesses. It is essential to rule out “Reversible Dementias” caused by metabolic imbalances, vitamin deficiencies, or thyroid dysfunction. Our evaluation aims to differentiate Alzheimer’s from other conditions like Vascular Dementia or Lewy Body disease to ensure the most accurate treatment path.
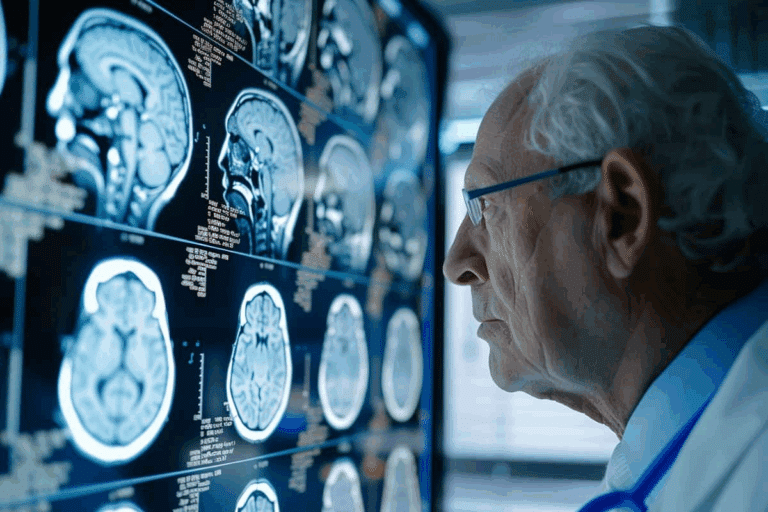
Modern evaluation utilizes Structural MRI and PET Scans to visualize the physical reality of the brain. MRI allows us to measure hippocampal volume, while specialized PET scans can detect the metabolic rate of brain cells or even the presence of amyloid plaques. By combining these images with genetic screening (such as the APOE-ε4 gene), we create a high-definition diagnostic profile. This precision allows families to plan for the future with a clear understanding of the disease’s progression.
Treatment for Alzheimer’s disease focuses on Symptom Stabilization and enhancing the brain’s remaining neural communication. We utilize pharmacological interventions like Cholinesterase Inhibitors and NMDA Receptor Antagonists to manage memory loss and confusion. In the landscape of regenerative medicine, we also explore newer monoclonal antibody therapies that aim to remove amyloid plaques from the brain, potentially slowing the rate of cognitive decline in early-stage patients.
Beyond medication, the “Circle of Care” involves creating a safe, low-stress environment for the patient. Non-Pharmacological Management, such as music therapy, cognitive stimulation, and routine-based care, helps reduce behavioral symptoms like agitation. We focus on preserving the patient’s dignity and supporting caregivers through education and respite care. The goal is to maximize the patient’s “Active Years” by integrating medical, nutritional, and emotional support into a single, unified care plan.
Wellness in Alzheimer’s care is founded on the concept of Neuro-protection. While we cannot fully prevent the disease, lifestyle interventions can build “Cognitive Reserve,” allowing the brain to better withstand pathological changes. We emphasize the MIND Diet, which focuses on berries, leafy greens, and healthy fats to lower the neuro-inflammation that fuels the disease. By protecting the brain’s vascular health, we ensure that neurons receive the oxygen and nutrients they need to stay resilient.
Physical activity is a primary trigger for Neurogenesis (the birth of new neural connections) in the hippocampus. Research shows a strong link between heart health and brain health; managing blood pressure and diabetes is essential for Alzheimer’s prevention. Furthermore, treating sensory losses like hearing impairment reduces the cognitive load on the brain and prevents the social isolation that often accelerates cognitive decline. Wellness is an active, lifelong commitment to brain health.

Send us all your questions or requests, and our expert team will assist you.
While having a parent or sibling with the disease raises your risk, most cases are not directly inherited. Genetics (like the APOE-ε4 gene) can influence your likelihood, but lifestyle and environmental factors play an equally significant role in most patients.
Dementia is an umbrella term for a decline in mental ability (the symptoms). Alzheimer’s is a specific disease (the cause) and is the most common reason why seniors develop dementia symptoms.
Yes. Although rare, younger-onset Alzheimer’s can affect people under 65. This form is often linked to specific, rare genetic mutations and tends to progress differently than the late-onset form
The MIND diet combines elements of Mediterranean and DASH diets. It focuses on foods like berries and leafy greens that have been clinically shown to reduce brain inflammation and the buildup of toxic proteins.
On average, people live 4 to 8 years after diagnosis, but many live as long as 20 years. The length of survival depends on the patient’s overall health and the quality of supportive care they receive.

 Bone Health
Bone Health Aesthetic Genital Surgery
Aesthetic Genital Surgery Geriatrics
Geriatrics Cardiology
Cardiology To Be Categorized
To Be Categorized Anxiety Disorders
Anxiety Disorders
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)