Geriatrics addresses the health needs of older adults, focusing on frailty, dementia, falls, and chronic disease management.
Send us all your questions or requests, and our expert team will assist you.
Glaucoma symptoms and causes vary depending on the type of the condition and the speed at which optic nerve damage develops. One of the most challenging aspects of glaucoma is that many individuals experience little to no noticeable symptoms in the early stages, particularly in the most common forms. This silent progression means that vision loss may occur gradually over time without obvious warning signs, underscoring the importance of understanding both how glaucoma presents and why it develops.
The causes of glaucoma are complex and multifactorial. While elevated intraocular pressure is a well-recognized risk factor, it is not the sole cause of the disease. Structural characteristics of the eye, genetic predisposition, and age-related changes all interact to influence how glaucoma develops and progresses.
Symptoms of glaucoma depend largely on whether the condition progresses slowly or presents suddenly. Many people do not recognize symptoms until significant vision loss has occurred.
In early stages, especially in open angle glaucoma, symptoms are often absent. Vision may appear normal, and daily activities may not be affected.
When early symptoms do occur, they may include
• Subtle loss of peripheral vision
• Difficulty noticing objects to the side
• Reduced visual awareness in low-contrast environments
Because these changes develop gradually, they are frequently overlooked.
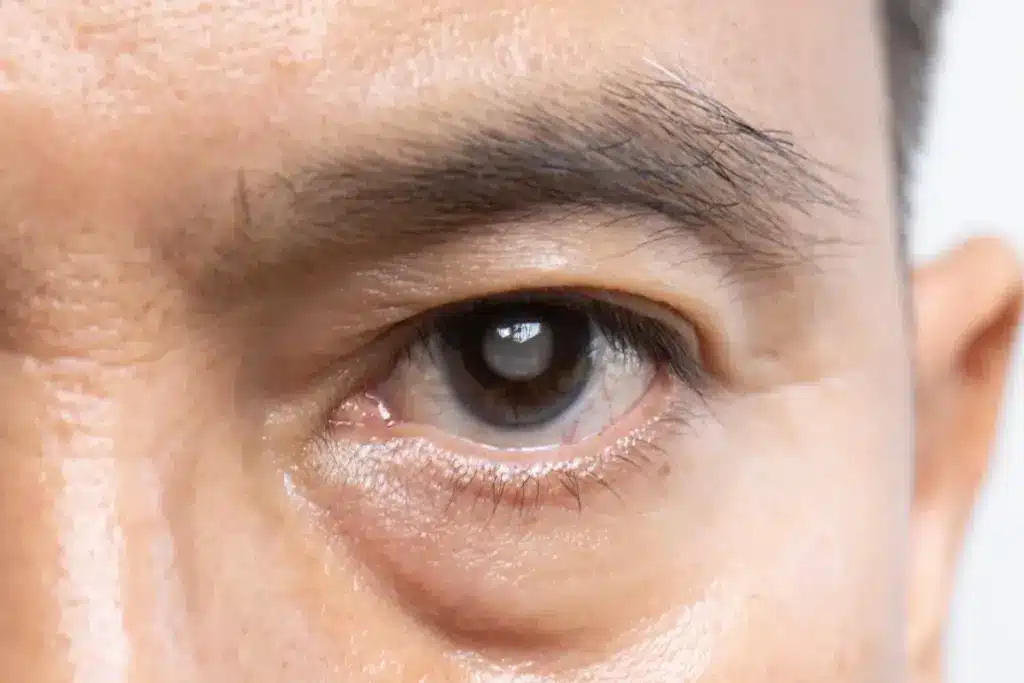
As glaucoma advances, visual field loss becomes more pronounced and begins to interfere with daily life.
The most characteristic sign of glaucoma is gradual narrowing of the visual field. Individuals may notice
• Bumping into objects
• Difficulty navigating unfamiliar spaces
• Reduced awareness of movement at the edges of vision
This pattern of vision loss reflects ongoing optic nerve damage.
In later stages, central vision may be affected. This can lead to difficulty with reading, facial recognition, and tasks requiring fine visual detail.
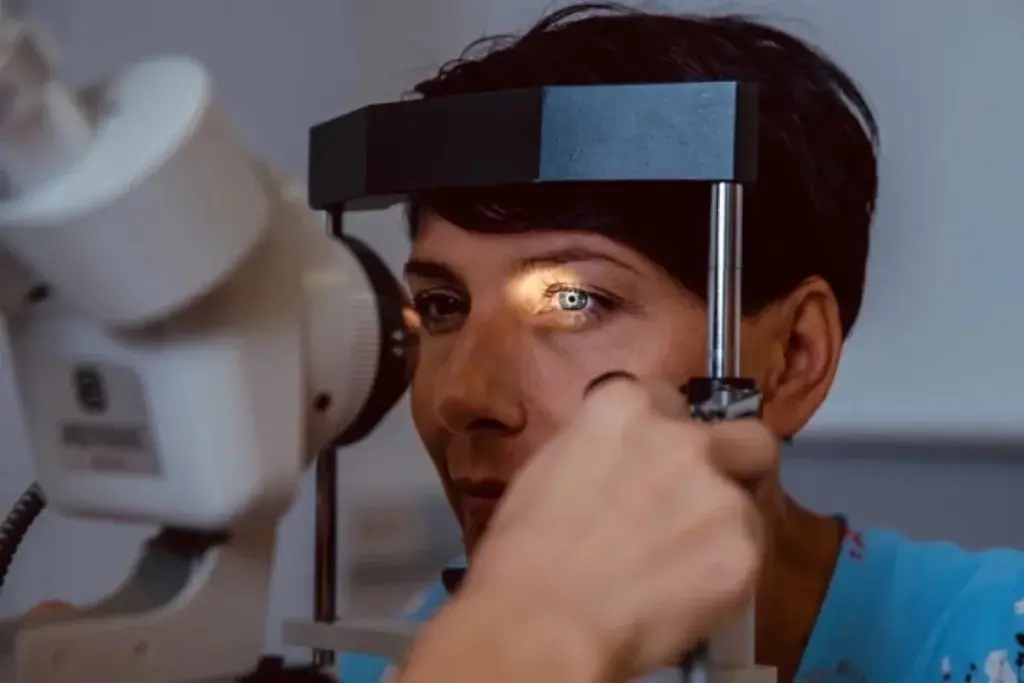
Angle closure glaucoma differs from open angle glaucoma in both presentation and urgency.
Acute angle closure glaucoma may present suddenly and requires immediate medical attention. Symptoms can include
• Sudden eye pain
• Blurred vision
• Halos around lights
• Headache and nausea
These symptoms result from a rapid rise in intraocular pressure and are distinct from the silent progression seen in other forms.
In chronic forms, symptoms may be mild or intermittent, resembling those of open angle glaucoma but related to gradual narrowing of the drainage angle.
Glaucoma develops when optic nerve fibers are damaged, most often due to impaired fluid dynamics within the eye.
The eye continuously produces fluid that must drain at the same rate to maintain stable pressure. When drainage is reduced, pressure can build up and place stress on the optic nerve.
This imbalance may be caused by
• Reduced efficiency of the drainage system
• Blockage or narrowing of the drainage angle
• Structural resistance within the outflow pathways
Certain anatomical features of the eye increase susceptibility to glaucoma.
Some optic nerves are more sensitive to pressure-related stress, even at lower pressure levels. This helps explain why glaucoma can occur without elevated pressure.
The shape of the eye and configuration of the drainage angle influence how fluid exits the eye. Narrow angles increase the risk of angle closure forms of glaucoma.
Genetics play an important role in glaucoma risk. Individuals with a family history of glaucoma are more likely to develop the condition.
Hereditary factors may influence
• Optic nerve structure
• Fluid drainage efficiency
• Age of onset
While glaucoma is not always inherited, genetic predisposition is a recognized risk factor.
The risk of glaucoma increases with age, reflecting cumulative structural and vascular changes within the eye.
Systemic factors that may contribute include
• Reduced blood flow to the optic nerve
• Age-related tissue changes
• Coexisting health conditions affecting circulation
These influences interact with ocular factors to shape disease progression.
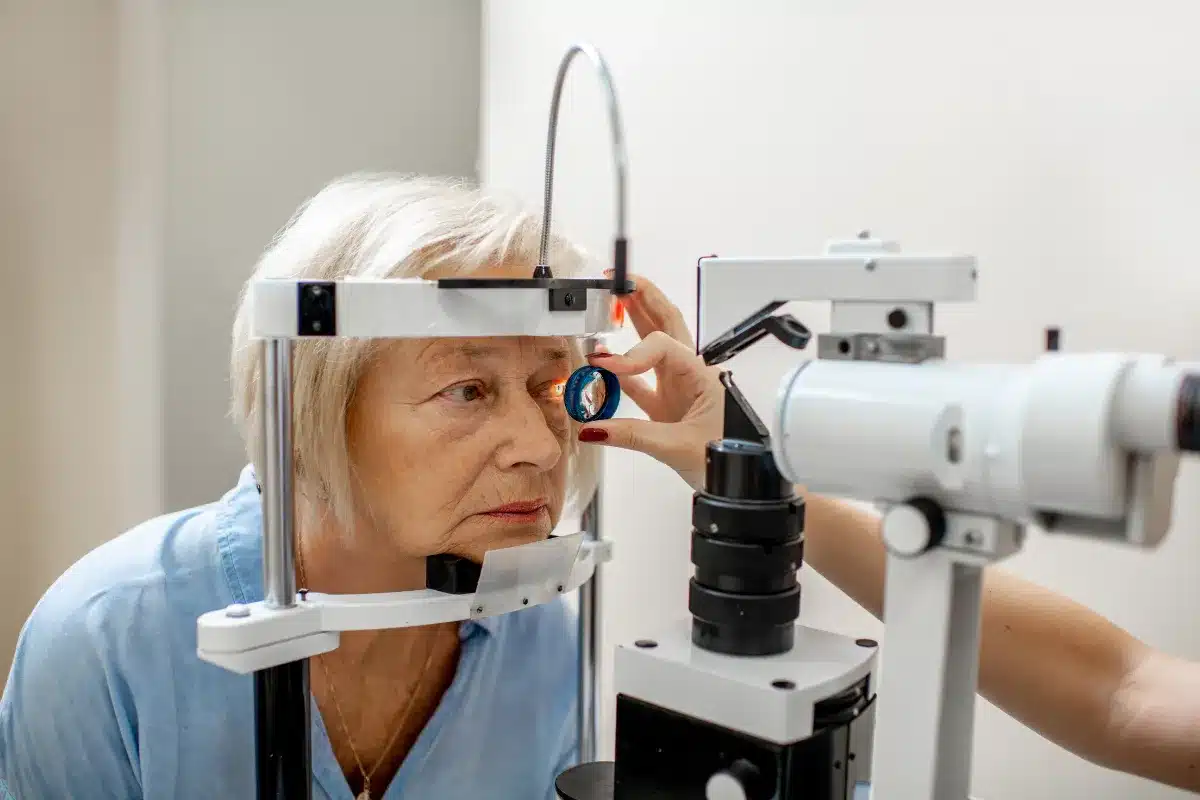
Many people do not notice glaucoma symptoms because vision loss begins peripherally and progresses slowly. The brain compensates for missing visual information, masking early deficits.
This makes routine eye examinations essential, particularly for individuals at higher risk.
Understanding glaucoma symptoms and causes supports earlier detection and more effective management. While vision loss cannot be reversed, identifying the condition before advanced damage occurs allows for strategies that help preserve remaining vision.
Recognizing risk factors and symptom patterns empowers individuals to seek timely evaluation and ongoing care.

Send us all your questions or requests, and our expert team will assist you.
Several systemic and ocular factors raise glaucoma risk in seniors. Non‑modifiable factors include age greater than 60, a family history of glaucoma, and ancestry such as African, Hispanic, or Asian. Modifiable risks involve high myopia, diabetes mellitus, hypertension, cardiovascular disease, and prolonged use of corticosteroid eye drops or systemic steroids. Recognizing these factors helps clinicians tailor preventive monitoring and lifestyle recommendations.
Glaucoma diagnosis combines several non‑invasive tests. Tonometry measures intraocular pressure, while ophthalmoscopy visualizes the optic nerve head. Gonioscopy assesses the drainage angle of the eye, crucial for distinguishing open‑angle from angle‑closure types. Perimetry (visual field testing) maps peripheral vision loss, and Optical Coherence Tomography (OCT) provides high‑resolution images of the retinal nerve fiber layer. Together, these tests confirm the presence of glaucoma, identify its type, and guide treatment planning.
No, glaucoma can develop even with normal eye pressure.
Glaucoma management aims to lower intraocular pressure and protect the optic nerve. First‑line therapy often involves topical eye drops such as prostaglandin analogues, beta‑blockers, or alpha agonists. Laser treatments like Selective Laser Trabeculoplasty (SLT) or Laser Iridotomy are used for specific types. Surgical options range from traditional trabeculectomy to minimally invasive glaucoma surgery (MIGS) and drainage devices. In some cases, oral carbonic anhydrase inhibitors are added. The choice depends on glaucoma type, severity, patient health, and tolerance of side effects.
Acute escalation of glaucoma requires prompt evaluation. Warning signs include sudden, severe eye pain often accompanied by blurred vision, rapid onset of halos around lights, a quick decrease in peripheral vision, or redness with nausea/vomitingtypical of an angle‑closure attack. Any abrupt change in vision after starting a new eye medication also warrants immediate assessment. Delaying care can lead to permanent optic nerve damage, so seniors should contact emergency services or an ophthalmology clinic without delay.

 Turp
Turp Turp
Turp Turp
Turp Turp
Turp Turp
Turp Turp
Turp
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)