Geriatrics addresses the health needs of older adults, focusing on frailty, dementia, falls, and chronic disease management.
Send us all your questions or requests, and our expert team will assist you.
Diagnosis and Evaluation of heart failure in older adults requires a nuanced approach that balances clinical rigor with the unique physiological changes of aging. At Liv Hospital, our multidisciplinary team tailors each assessment to the individual’s medical history, functional status, and personal goals, ensuring that every step of the process aligns with international standards of care.
Heart failure affects approximately 10% of people over 65 worldwide, and its prevalence continues to rise as life expectancy improves. Early identification and precise evaluation are critical because timely intervention can reduce hospitalizations, improve quality of life, and extend survival. This page provides a comprehensive overview of the diagnostic pathway, from initial clinical assessment to advanced imaging and functional testing, specifically designed for international patients seeking world‑class care.
Whether you are a patient, a family member, or a referring physician, the information below will guide you through the essential components of a thorough heart‑failure work‑up, highlighting the expertise and resources available at Liv Hospital’s geriatrics department.
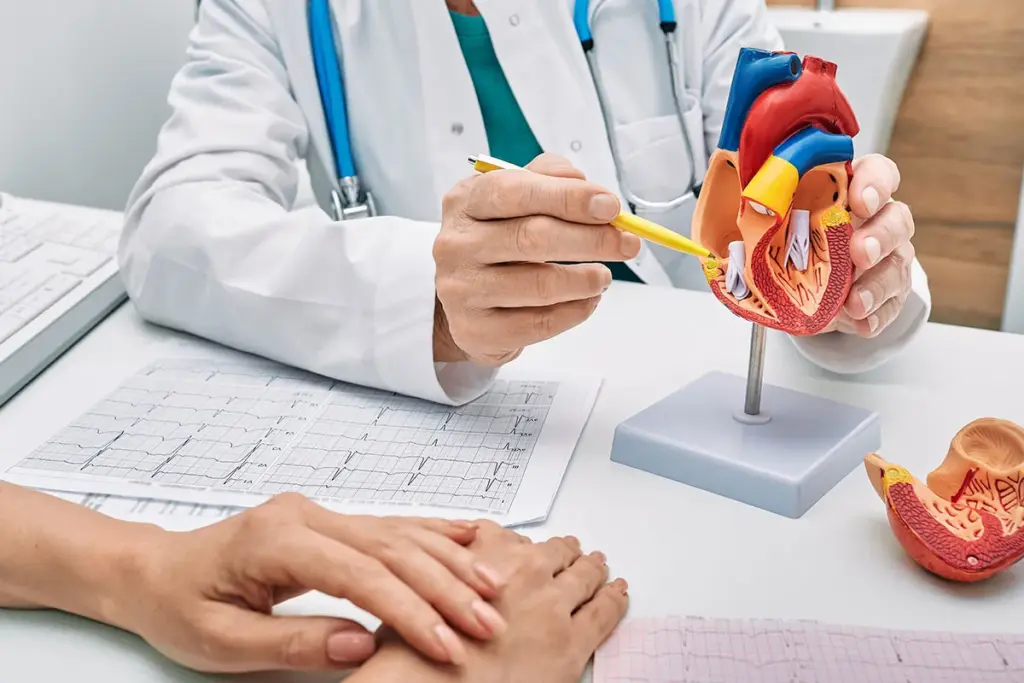
The first step in evaluating heart failure is a thorough clinical assessment. Technology gives doctors numbers, but the physical exam provides important clues about the patient’s blood flow and fluid status. This step looks for signs of fluid buildup and poor blood flow, which are key features of advanced heart failure.

Today, doctors use blood tests called biomarkers to measure heart stress and the body’s response. These tests give clear data that help tell heart failure apart from other conditions with similar symptoms.
Heart failure in the elderly differs from that in younger populations due to age‑related cardiac remodeling, comorbidities, and altered pharmacodynamics. Recognizing these differences is the foundation of effective diagnosis and evaluation. The condition is typically classified by ejection fraction (EF) into reduced (HFrEF), preserved (HFpEF), or mildly reduced (HFmrEF) categories, each with distinct therapeutic implications.
Key factors influencing the presentation in geriatric patients include:
Accurate classification begins with a careful review of medical records, medication lists, and prior imaging. At Liv Hospital, we employ a structured assessment protocol that integrates geriatric expertise with cardiology, ensuring that age‑specific nuances are captured early in the diagnostic journey.
A thorough clinical assessment remains the cornerstone of heart‑failure diagnosis and evaluation. The process begins with a detailed history that captures symptom onset, functional limitations, and associated comorbidities. In geriatric patients, clinicians pay special attention to subtle signs such as nocturnal dyspnea, orthostatic dizziness, or unexplained weight loss.
Essential elements of the history include:
Physical examination focuses on signs of volume overload (e.g., peripheral edema, jugular venous distention) and perfusion deficits (e.g., cool extremities). In older adults, the presence of a third heart sound (S3) may be less pronounced, making reliance on imaging and biomarkers even more critical.
Liv Hospital’s geriatrics team utilizes standardized checklists and validated tools such as the New York Heart Association (NYHA) classification and the Kansas City Cardiomyopathy Questionnaire (KCCQ) to quantify symptom burden and guide subsequent testing.
Laboratory investigations provide objective data that complement clinical findings in the diagnosis and evaluation of heart failure. The most widely used biomarker is B‑type natriuretic peptide (BNP) or its N‑terminal pro‑form (NT‑proBNP), which rise in response to ventricular wall stress. In elderly patients, baseline levels may be elevated due to renal insufficiency or atrial fibrillation, necessitating age‑adjusted reference ranges.
Key laboratory panels include:
Advanced biomarker profiling, such as galectin‑3 and soluble ST2, is increasingly used in specialized centers to refine risk stratification. Liv Hospital’s laboratory is equipped with state‑of‑the‑art analyzers that deliver rapid, high‑precision results, enabling clinicians to make informed decisions during the evaluation phase.
Imaging provides the visual confirmation necessary for definitive diagnosis and evaluation of heart failure and its underlying structural causes. The cornerstone study is transthoracic echocardiography (TTE), which assesses chamber sizes, wall motion, valvular function, and ejection fraction. In geriatric patients, TTE is preferred for its non‑invasiveness and bedside availability.
Additional imaging options include:
Liv Hospital utilizes a fully integrated imaging suite, allowing seamless transition from TTE to CMR or CT under the same care pathway. All studies are interpreted by board‑certified cardiologists with specific expertise in geriatric cardiology, ensuring that age‑related anatomic variations are accurately reported.




Send us all your questions or requests, and our expert team will assist you.
An echocardiogram uses sound waves to create images of the heart and is excellent for assessing valve function and blood flow velocities. A cardiac MRI uses magnetic fields to create high-definition images that provide superior detail of the heart’s tissue composition, distinguishing healthy muscle, scar tissue, and inflammation.
The Ejection Fraction represents the percentage of blood the left ventricle pumps out with each contraction. It is the primary metric used to categorize heart failure into specific types, dictates which medications are prescribed, and serves as a key benchmark for measuring the success of treatments, including regenerative therapies.
Hibernating myocardium refers to heart muscle that is alive but has stopped contracting normally due to chronically reduced blood flow. Identifying this tissue is crucial because, unlike dead scar tissue, hibernating muscle can recover function if blood flow is restored through stenting, bypass surgery, or angiogenic cell therapies.
BNP is a hormone produced by the heart when it is under stress or stretched by fluid overload. Measuring BNP levels helps doctors confirm the diagnosis of heart failure, as levels are typically elevated in patients with the condition, and helps track the effectiveness of treatment.
While not always required for the initial diagnosis, a stress test is a valuable tool for evaluating the cause and severity of heart failure. It helps determine if the condition is caused by coronary artery disease and provides an objective measure of the patient’s functional capacity.

 General Surgery
General Surgery Dentistry
Dentistry Ear Nose Throat
Ear Nose Throat Acid Disorders
Acid Disorders Geriatrics
Geriatrics
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)