Geriatrics addresses the health needs of older adults, focusing on frailty, dementia, falls, and chronic disease management.
Send us all your questions or requests, and our expert team will assist you.
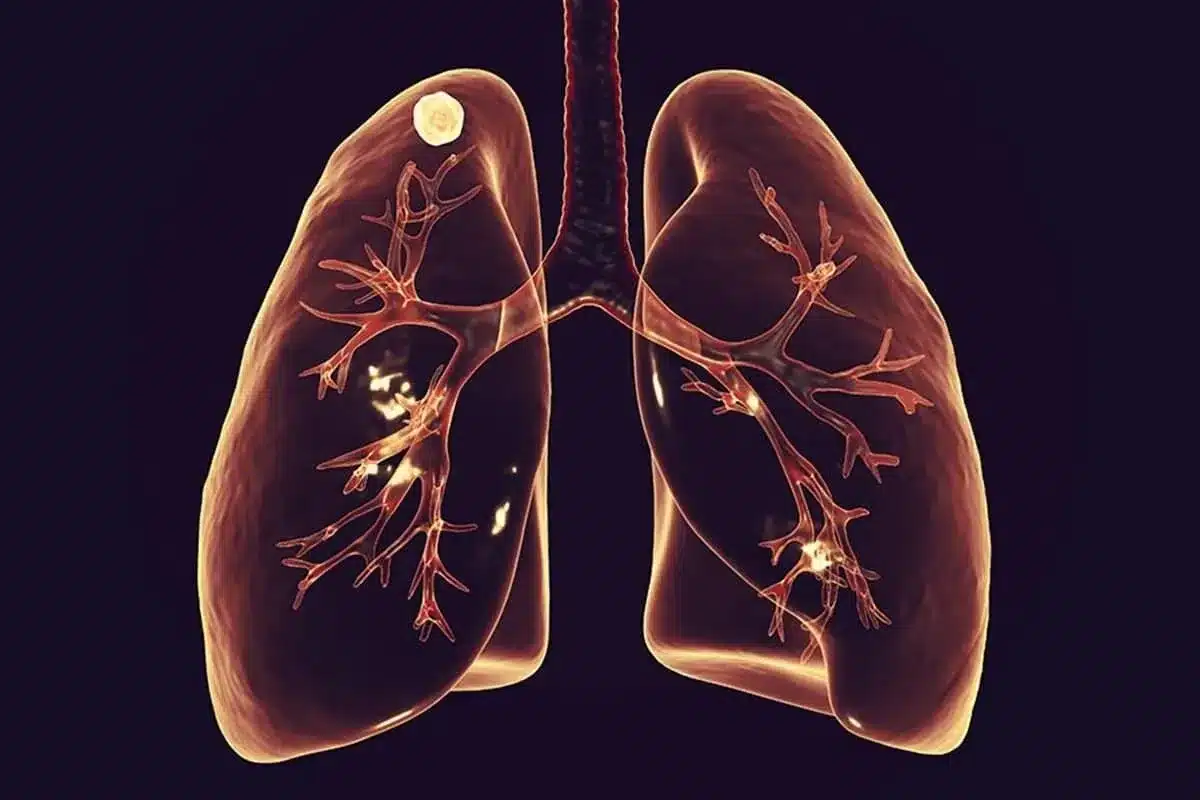
Pulmonary disease encompasses a vast array of pathological conditions affecting the lungs and the respiratory system.
This complex network of organs and tissues is responsible for the critical exchange of oxygen and carbon dioxide, a process essential for sustaining life. When this system is compromised, it impacts every cell in the human body by limiting oxygen delivery.
The term covers everything from acute infections like pneumonia to chronic, progressive conditions such as Chronic Obstructive Pulmonary Disease and pulmonary fibrosis. Modern medicine views the respiratory system not just as a pair of air sacs but as a dynamic interface between the body and the external environment.
Breathing is an autonomic process controlled by the brainstem, yet it relies on the mechanical integrity of the thoracic cage and the diaphragm. Air enters through the upper respiratory tract, where it is warmed, humidified, and filtered before reaching the delicate structures of the lower lungs.
The primary site of gas exchange is the alveoli, microscopic sacs surrounded by capillaries. Here, oxygen diffuses into the bloodstream while carbon dioxide is expelled. Disruption at this microscopic level is the hallmark of many severe pulmonary diseases.
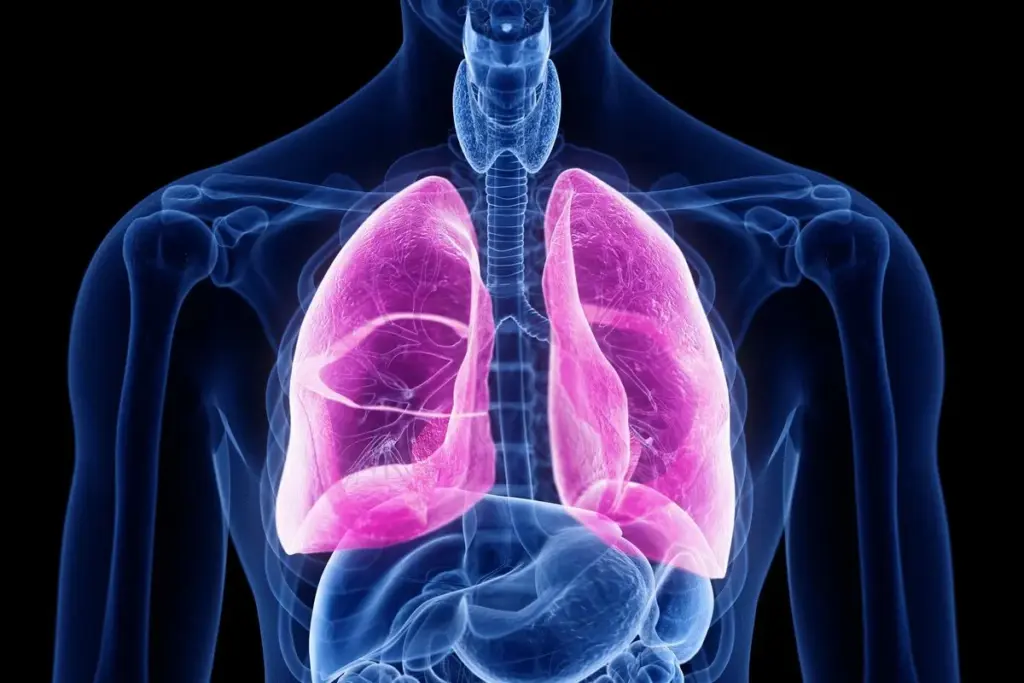
Obstructive lung diseases are characterized by a physical blockage or narrowing of the airways, making it difficult to exhale fully. The air remains trapped inside the lungs, leading to hyperinflation and reduced efficiency of fresh air intake.
Common conditions in this category include asthma, COPD, and bronchiectasis. The narrowing can be caused by inflammation, excess mucus production, or the destruction of the elastic tissue that holds airways open.
Unlike obstructive conditions, restrictive lung diseases prevent the lungs from fully expanding with air. This restriction reduces the total volume of air the lungs can hold. It is often described as trying to breathe while wearing a tight corset.
This limitation can arise from stiffness within the lung tissue itself, such as in pulmonary fibrosis, or from external factors affecting the chest wall, such as severe scoliosis or neuromuscular disorders.
COPD is a progressive disease that makes it hard to breathe. It encompasses two main conditions: emphysema and chronic bronchitis. In emphysema, the air sacs are damaged and lose their elasticity, while chronic bronchitis involves long term inflammation of the airways.
This condition is largely preventable and is most commonly associated with long term exposure to irritants, primarily cigarette smoke. However, modern research also highlights the role of biomass fuel smoke and occupational dust in its development.
Asthma is a chronic condition causing inflammation and narrowing of the bronchial tubes. It is defined by its reversibility and hyperresponsiveness to various triggers. These triggers can be allergens, cold air, exercise, or viral infections.
During an attack, the muscles around the airways tighten, and the lining swells while producing excess mucus. This triad of constriction, edema, and secretion drastically reduces the diameter of the airway, causing the characteristic wheeze.
Interstitial Lung Disease is a broad category including more than 200 disorders that cause inflammation and scarring of the interstitium. The interstitium is the tissue and space around the air sacs of the lungs.
When this tissue becomes scarred, the lungs become stiff and cannot expand easily. This scarring, or fibrosis, is often irreversible and progressive. Causes range from autoimmune diseases to exposure to hazardous materials like asbestos.

This subset of diseases affects the blood circulation within the lungs. The most prominent condition is Pulmonary Hypertension, where high blood pressure occurs specifically in the arteries of the lungs.
This high pressure forces the right side of the heart to work harder to pump blood through the lungs, eventually leading to heart failure. Pulmonary embolism, a blockage in a lung artery, is another critical vascular condition.
Respiratory infections remain a leading cause of morbidity globally. These can affect the upper or lower respiratory tract and are caused by viruses, bacteria, or fungi. Pneumonia is a severe infection that inflames the air sacs, which may fill with fluid or pus.
Modern challenges in this area include antibiotic resistant bacteria and novel viral pathogens. The lung’s local immune system is the first line of defense, but when overwhelmed, severe inflammation and tissue damage can occur.
While environmental factors are dominant, genetics play a significant role in pulmonary susceptibility. Alpha 1 antitrypsin deficiency is a genetic condition that predisposes individuals to early onset COPD, even without a history of smoking.
Cystic fibrosis is another genetic disorder that affects the lungs, in which a defective gene causes thick, sticky mucus to build up. This mucus clogs the tubes that carry air in and out of the lungs and traps bacteria.
The air we breathe at work or home significantly influences lung health. Occupational lung diseases are caused by inhaling dusts, fumes, or gases. Examples include coal worker’s pneumoconiosis and silicosis.
Long term exposure to these particles causes inflammation and scarring. Even in non industrial settings, indoor air quality issues like mold or radon can contribute to chronic pulmonary problems.
Sleep Disordered Breathing, particularly Obstructive Sleep Apnea (OSA), is a prevalent pulmonary concern. It involves recurrent episodes of partial or complete upper airway obstruction during sleep.
These interruptions in breathing lead to drops in oxygen levels and fragmented sleep. The cardiovascular stress caused by untreated apnea is significant, linking lung health directly to heart health.
The pleura is the thin membrane that lines the chest cavity and covers the lungs. Diseases of the pleura include pleurisy, pleural effusion, and pneumothorax. These conditions affect the space outside the lung but within the chest wall.
Fluid or air accumulating in this space compresses the lung, preventing it from expanding. This mechanical compression causes sharp pain and significant shortness of breath.

Send us all your questions or requests, and our expert team will assist you.
COPD is a progressive disease usually caused by smoking or irritants, where airflow is permanently limited. Asthma is an inflammatory condition often triggered by allergies, characterized by reversible airway obstruction. While symptoms overlap, their underlying causes and long term progression differ significantly.
Generally, lung tissue that has been destroyed or scarred, as in emphysema or fibrosis, cannot regenerate or grow back. Treatment focuses on preserving the remaining lung function and reducing symptoms. However, inflammation in conditions like asthma or acute infections is reversible.
Some pulmonary diseases have a direct genetic link, such as Cystic Fibrosis and Alpha 1 Antitrypsin Deficiency. For other conditions like asthma or COPD, genetics may play a role in susceptibility, meaning you are more likely to develop it if family members have it, but lifestyle is also a significant factor.
These are informal terms often used to describe symptoms. “Wet” conditions typically involve excess mucus or fluid, such as chronic bronchitis, pneumonia, or pulmonary edema. “Dry” conditions often involve scarring and a dry cough, such as those seen in interstitial lung disease or fibrosis.
The heart and lungs work as a unified system. The right side of the heart pumps blood to the lungs to get oxygen. If the lungs are diseased (high pressure), it strains the heart. Conversely, if the left heart fails, fluid backs up into the lungs, causing pulmonary edema.

 Geriatrics
Geriatrics Geriatrics
Geriatrics
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)