Hair transplant surgery restores hair density using advanced FUE and DHI techniques. Learn about the procedure, diagnosis of hair loss, and recovery process.
Send us all your questions or requests, and our expert team will assist you.
Providing an overview and definition of trichotillomania hair pulling is essential for anyone considering hair restoration or seeking relief from this compulsive behavior. Trichotillomania, classified as a body‑focused repetitive behavior disorder, involves recurrent urges to pull out one’s own hair, leading to noticeable hair loss and psychological distress. International patients who arrive at Liv Hospital often wonder how this condition may affect their candidacy for hair‑transplant procedures and what therapeutic pathways are available. Recent studies suggest that up to 2 % of the global population experiences trichotillomania at some point in their lives, highlighting the importance of clear, evidence‑based information.
This page delivers a detailed overview and definition of trichotillomania, covering its origins, clinical signs, diagnostic criteria, and current treatment modalities. Whether you are a patient, a caregiver, or a medical professional, the following sections will equip you with the knowledge needed to make informed decisions about hair health and potential surgical interventions.
Trichotillomania, often referred to as hair‑pulling disorder, is a chronic psychiatric condition characterized by an irresistible urge to remove hair from the scalp, eyebrows, eyelashes, or other body areas. The overview and definition of this disorder emphasizes its classification under the Diagnostic and Statistical Manual of Mental Disorders (DSM‑5) as an Obsessive‑Compulsive and Related Disorder.
Region | Estimated Prevalence |
|---|---|
North America | ≈1.5 % |
Europe | ≈1.2 % |
Asia | ≈0.8 % |
The condition can emerge at any age, but it most commonly begins during adolescence. Understanding these fundamentals provides a solid overview and definition that guides further exploration of causes and treatments.

While the exact etiology of trichotillomania remains unclear, research points to a combination of genetic, neurobiological, and environmental influences. The overview and definition of its causes helps clinicians tailor individualized care plans.
Family studies indicate a higher incidence among first‑degree relatives, suggesting a hereditary component. Twin studies show concordance rates up to 50 % in monozygotic pairs.
Stressful life events, trauma, or chronic anxiety can exacerbate hair‑pulling episodes. Additionally, certain cultural practices that involve frequent hair manipulation may increase susceptibility.
Recognizing these risk factors is crucial for a comprehensive overview and definition that informs both preventive strategies and therapeutic interventions.
The clinical picture of trichotillomania varies widely, ranging from mild, occasional pulling to severe, daily episodes causing extensive alopecia. An accurate overview and definition of symptoms assists healthcare providers in differentiating this disorder from other hair‑loss conditions.
Patients often report feelings of tension before pulling and a sense of relief afterward. Many experience shame, embarrassment, or social withdrawal, which can compound the disorder’s impact.
Comorbidity | Prevalence Among Trichotillomania Patients |
|---|---|
Obsessive‑Compulsive Disorder | ≈30 % |
Depressive Disorders | ≈25 % |
Anxiety Disorders | ≈20 % |
By integrating these observations into a clear overview and definition, clinicians can better assess severity and plan appropriate treatment pathways.

Diagnosing trichotillomania requires a thorough clinical interview, physical examination, and often standardized assessment scales. The overview and definition of diagnostic criteria ensures consistency across international patient evaluations.
Dermatologists assess hair‑pull patterns, scalp condition, and rule out alopecia areata or tinea capitis. Photographic documentation aids longitudinal monitoring.
These structured approaches form an essential overview and definition framework for accurate diagnosis, especially for patients traveling internationally for specialized care.
Effective management of trichotillomania blends behavioral therapy, pharmacotherapy, and, when appropriate, supportive technologies. A comprehensive overview and definition of treatment modalities equips patients with realistic expectations.
Medications are considered when behavioral approaches alone are insufficient.
Medication Class | Typical Use | Evidence Level |
|---|---|---|
Selective Serotonin Reuptake Inhibitors (SSRIs) | Reduce anxiety and compulsive urges | Moderate |
Clomipramine (TCA) | Target obsessive‑compulsive symptoms | Strong |
N‑acetylcysteine (NAC) | Modulate glutamate pathways | Emerging |
Support groups, mindfulness meditation, and wearable devices that alert the user to hand movements can complement primary therapies.
Integrating these strategies into a patient‑centered plan reflects a holistic overview and definition of trichotillomania treatment, aligning with Liv Hospital’s multidisciplinary approach.
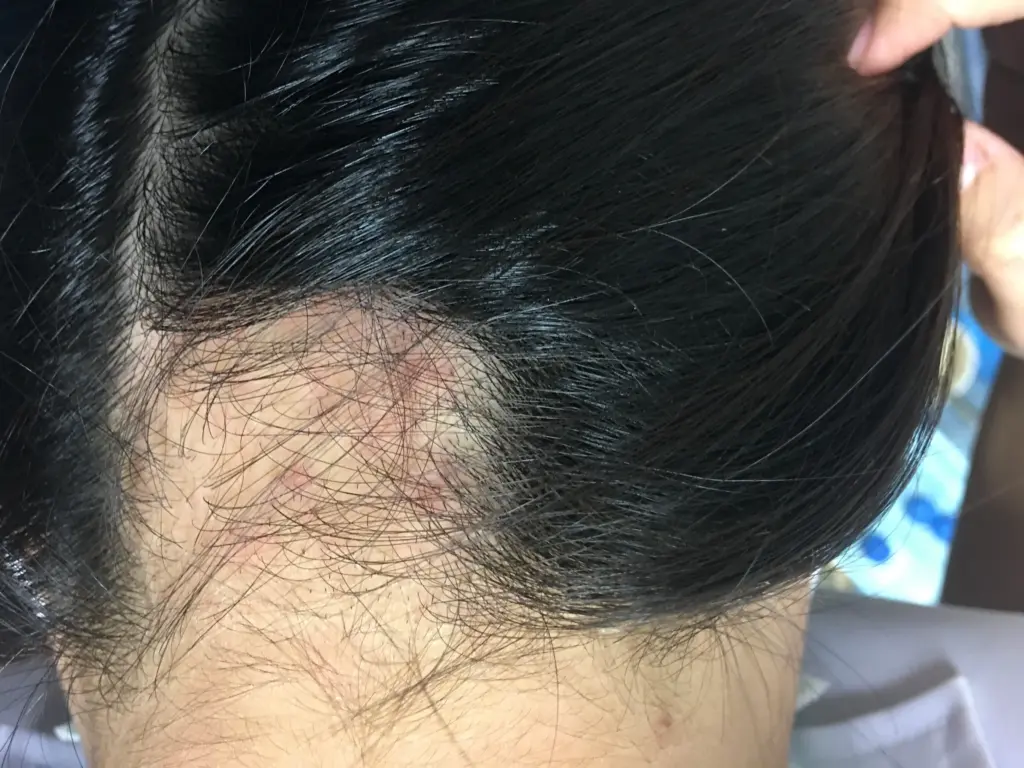
For individuals seeking hair‑transplant surgery, understanding how trichotillomania may affect outcomes is critical. This section provides an overview and definition of considerations specific to surgical candidacy.
Surgeons may employ protective dressings and post‑operative counseling to minimize the risk of post‑operative pulling. In some cases, a temporary pause in pulling behavior is required before graft placement.
Component | Recommended Action |
|---|---|
Medication | Continue SSRIs or NAC as prescribed. |
Therapy | Maintain weekly HRT sessions for at least three months. |
Follow‑up | Regular clinic visits every 2‑4 weeks during the first 3 months. |
By integrating this tailored overview and definition, patients and clinicians can collaboratively decide whether hair transplantation is feasible and safe.
Liv Hospital offers JCI‑accredited, internationally recognized care for patients with trichotillomania who are considering hair‑restoration solutions. Our multidisciplinary team combines psychiatric expertise, dermatology, and advanced hair‑transplant technology to deliver personalized treatment plans. International patients benefit from seamless coordination of appointments, interpreter services, and comfortable accommodation, ensuring a stress‑free experience from consultation to recovery.
Take the first step toward a healthier scalp and lasting confidence. Contact Liv Hospital today to schedule a comprehensive evaluation and explore tailored treatment options for trichotillomania and hair restoration.


Send us all your questions or requests, and our expert team will assist you.
Trichotillomania, also known as hair‑pulling disorder, involves recurrent hair‑pulling that leads to noticeable hair loss and psychological distress. The condition is listed in the DSM‑5 as an Obsessive‑Compulsive and Related Disorder, reflecting its compulsive nature. Patients experience tension before pulling and relief afterward, and attempts to stop the behavior are often unsuccessful. The disorder can affect any hair‑bearing area, including scalp, eyebrows, and eyelashes, and may begin in adolescence but persist into adulthood.
Research suggests a multifactorial etiology. Family and twin studies indicate a hereditary component, with higher prevalence among first‑degree relatives and up to 50 % concordance in monozygotic twins. Neurobiologically, altered serotonin and dopamine pathways and hyperactivity in cortico‑striatal circuits have been observed via functional MRI. Environmental triggers such as chronic stress, trauma, or cultural practices involving frequent hair manipulation can exacerbate the urge to pull. Understanding these factors helps clinicians tailor individualized treatment plans.
A clinician first conducts a thorough interview to assess the frequency, intensity, and impact of hair‑pulling. The DSM‑5 criteria require recurrent pulling resulting in hair loss, repeated attempts to stop, significant distress or impairment, and exclusion of other medical conditions. Dermatological examination rules out alopecia areata or tinea capitis. Standardized tools such as the Massachusetts General Hospital Hairpulling Scale (MGH‑HPS), Trichotillomania Diagnostic Inventory (TDI), and Clinical Global Impression (CGI) provide quantitative severity ratings, facilitating consistent assessment across international patients.
Behavioral interventions are first‑line and include Habit Reversal Training (awareness, competing response, social support), Cognitive‑Behavioral Therapy, and Acceptance and Commitment Therapy. When behavior‑based approaches are insufficient, medications such as SSRIs (reduce anxiety and compulsive urges), clomipramine (targets obsessive‑compulsive symptoms), and N‑acetylcysteine (modulates glutamate pathways) are prescribed, with varying evidence levels. Adjunctive support like mindfulness, support groups, and wearable devices that alert users to hand movements can further enhance outcomes. A multidisciplinary approach ensures comprehensive care.
Before a hair‑transplant, surgeons assess impulse control through a psychological evaluation and verify that hair‑pulling has been stable or absent for at least six months. Donor‑site quality and scalp health are documented. During surgery, protective dressings and post‑operative counseling minimize the risk of pulling. Post‑operative care includes continued pharmacotherapy (e.g., SSRIs or NAC), ongoing Habit Reversal Training, and frequent follow‑up visits (every 2‑4 weeks for the first three months) to monitor graft survival and prevent relapse.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)