
Urticaria, also known as hives, affects millions of people worldwide. It causes discomfort and distress. We aim to help you understand this condition. Defining hives (Urticaria), explaining the common triggers, symptoms, and when to seek emergency medical attention.
Hives are itchy, raised welts. They can be acute or chronic, often caused by allergic reactions. Managing it well is important for a good quality of life.
Understanding urticaria is essential. We will look into its causes, symptoms, and treatments. This will help you manage this complex condition better.
Key Takeaways
- Urticaria is a common skin condition that can significantly impact daily life.
- It is characterized by itchy, raised welts and can be acute or chronic.
- Allergic reactions are a common trigger for urticaria.
- Effective management involves understanding its causes and symptoms.
- Treatment options vary depending on the severity and type of urticaria.
What Are Hives?
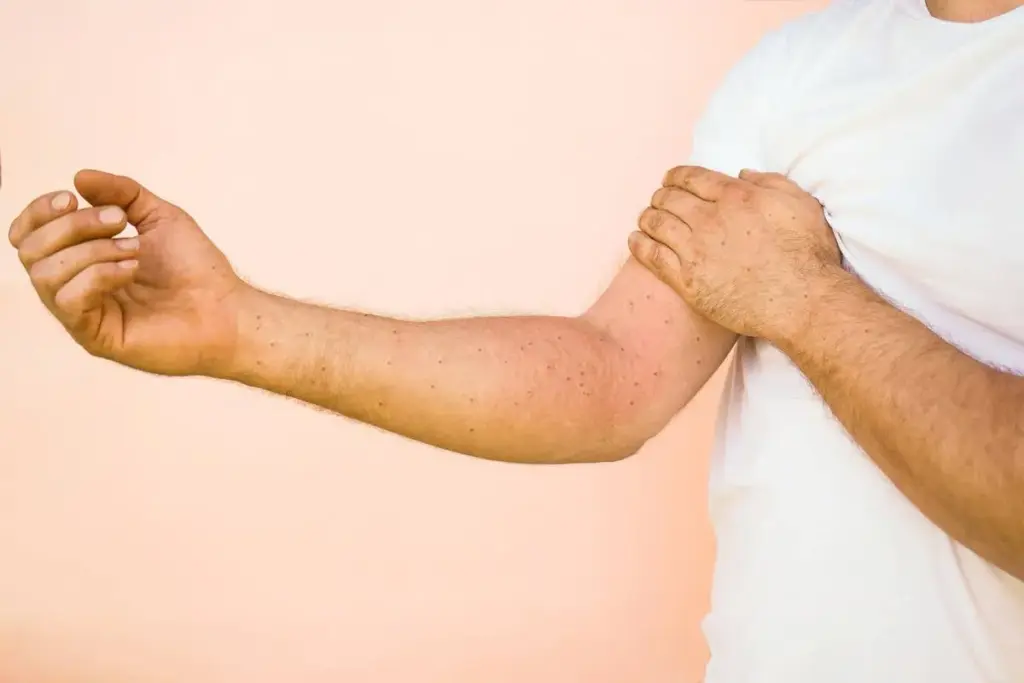
Hives, also known as urticaria, are a skin reaction that results in itchy, raised welts. These welts can vary in size and can appear anywhere on the body. We will explore the definition, symptoms, types, and risk factors associated with hives.
Definition and Symptoms
Hives are characterized by itchy, red, or white raised areas on the skin. They can be acute or chronic, with the former lasting less than six weeks and the latter persisting beyond six weeks. Symptoms can include:
- Itchy skin
- Red or white raised welts
- Swollen areas
Types of Hives
There are two main types of hives: acute and chronic. Acute hives are the most common form and typically result from an allergic reaction. Chronic hives, on the other hand, can be caused by a variety of factors, including autoimmune disorders.
Risk Factors
Several factors can increase the risk of developing hives, including:
- Allergies to foods, medications, or insect stings
- Infections such as the common cold or flu
- Autoimmune disorders
- Stress
Causes of Hives
Hives, or urticaria, can be caused by many things, like allergies and environmental factors. Knowing what causes them is key to managing and preventing hives.
Allergic Reactions
Allergic reactions often lead to hives. When the body finds an allergen, it releases histamine. This chemical makes blood vessels leak, causing hives’ swelling and redness. Foods, drugs, and insect bites are common allergens.
For example, eating foods like peanuts or shellfish can cause hives in some. Medications, like antibiotics or NSAIDs, can also trigger allergic reactions that show up as hives.
Infections and Illnesses
Infections and illnesses can also cause hives. Viral infections, like the common cold, can lead to hives in some people. Bacterial infections, like urinary tract infections, and parasitic infections can also cause hives.
Certain autoimmune disorders, like thyroiditis or lupus, can also cause hives. These conditions make the body attack its own tissues, sometimes leading to hives.
Environmental Triggers
Environmental factors can also trigger hives. Extreme temperatures, whether hot or cold, can cause hives in some. Sun exposure can also lead to hives, known as solar urticaria.
Stress is another factor that can trigger hives. The exact reason is not fully understood, but stress can make hives worse or start them in some people. Tight clothing or skin friction, where clothes rub against the skin, can also cause hives.
The Immune System’s Role in Hives
The body’s immune response plays a big part in hives. It involves many cells and chemicals working together. When the immune system sees a threat, it can start a chain of reactions that may lead to hives.
Histamine is a key chemical in allergic reactions. Histamine release is a key step in getting hives. When an allergen gets into the body, the immune system notices it. It then releases histamine and other chemicals.
Histamine Release
Histamine is stored in mast cells all over the body. When an allergen hits a mast cell, it makes histamine spill into the blood. This makes blood vessels open up, leading to increased permeability. This causes the symptoms of hives, like itching, redness, and swelling.
Knowing about histamine meaning in hives is important. Histamine is more than just a chemical; it’s a messenger that warns the body of threats. In hives, this warning is often too strong for the danger.
How the Body Reacts
The body’s reaction to histamine is what shows as hives. Histamine makes blood vessels open, letting fluid into the tissue. This creates the itchy welts seen in urticaria. Antihistamines help by blocking histamine, reducing antihistamine hives rash symptoms.
In severe cases, the immune system’s reaction can cause anaphylaxis. This is a serious condition that needs quick medical help. Knowing how the body reacts to threats helps manage hives and prevent worse reactions.
Understanding the immune system’s role in hives and histamine’s part in it helps us see why treatment is so important. This includes using antihistamines and other treatments to control the immune system’s response.
Common Allergens Linked to Hives
Knowing what causes hives is key to managing them. Hives often come from allergic reactions. These can be from foods, insect stings, or medicines. We’ll look at these common causes and how they lead to hives.
Foods That Trigger Hives
Some foods can cause allergic reactions and hives. Nuts, shellfish, dairy, and eggs are common culprits. If you have hives from food allergies, avoiding these foods is vital. Keeping a food diary can help track which foods cause reactions.
Nuts and Seeds: Tree nuts and peanuts are common allergens. Even small amounts can cause a reaction. People with nut allergies need to be careful with food labels.
Shellfish and Fish: These can also cause hives. The proteins in them can lead to severe allergic reactions.
Insect Stings and Bites
Insect stings and bites can also cause hives. For some, the venom can trigger a severe reaction. If you get hives from an insect sting, see a doctor to figure out what to do.
- Bees and Wasps: Their stings can cause allergic reactions, including hives.
- Mosquito Bites: While usually less severe, they can cause hives in some people.
Medications That Can Cause Hives
Some medicines can cause hives as an allergic reaction. Antibiotics, NSAIDs, and blood pressure medicines are common culprits. If you think a medicine is causing hives, talk to your doctor about other options.
Antibiotics: Penicillin and other antibiotics can cause hives. If you get hives after starting a new antibiotic, call your doctor right away.
Stress can make hives worse or even trigger them. Managing stress with meditation, yoga, or deep breathing can help. For itchy skin from hives, use gentle skin care and avoid scratching.
For those with hives, finding the best allergy medicine is important. Antihistamines are often the first choice for treating hives. We’ll discuss treatment options further.
Diagnosis of Hives
Diagnosing hives, or urticaria, involves a few steps. Healthcare professionals look at medical history, do a physical exam, and sometimes run extra tests. Accurate diagnosis is key for good treatment and management.
Medical History and Physical Examination
Getting a detailed medical history is important. We ask about when symptoms started, what might have caused them, and past allergic reactions. A physical exam helps us see the hives’ size, shape, and where they are on the body.
We might check for bumps on the back of the tongue or other signs of an allergic reaction. This helps us understand the situation better.
Skin Testing for Allergies
Sometimes, we do skin tests to find out what’s causing the hives. We put small amounts of possible allergens on the skin and watch for reactions. This helps us know what to avoid.
Blood Tests for Underlying Conditions
Blood tests help us check for other health issues that might be causing the hives. We might do a complete blood count (CBC) or tests for specific antibodies. These tests help us figure out the best treatment.
Diagnosing hives can be tricky because there are many possible causes. But, by looking at medical history, doing physical exams, and using tests when needed, we can find the cause and manage it well.
The steps to diagnose hives include:
- Detailed medical history to identify triggers and past episodes.
- Physical examination to assess the hives’ characteristics.
- Skin testing to find specific allergens.
- Blood tests to check for underlying conditions.
By taking a thorough approach, we can give a clear diagnosis and create a treatment plan that fits the person’s needs.
Treatment Options for Hives
Treating hives requires a mix of methods to ease symptoms and find the cause. We know that a good plan might include medicine, changes in lifestyle, and other treatments.
Antihistamines and Their Function
Antihistamines are often the first choice for hives. They help with itching and redness by blocking histamine. Common antihistamines for hives are diphenhydramine and loratadine.
But, antihistamines can make you feel sleepy. Luckily, newer ones like loratadine are less likely to do this. This makes them a better choice for some.
|
Antihistamine Type |
Common Brands |
Side Effects |
|---|---|---|
|
First Generation |
Benadryl (diphenhydramine) |
Drowsiness, dry mouth |
|
Second Generation |
Claritin (loratadine) |
Less likely to cause drowsiness |
Corticosteroids for Severe Cases
For serious hives, doctors might suggest corticosteroids to lessen swelling. These are used for a short time because of possible long-term side effects. Corticosteroids can be taken by mouth or injected.
“Corticosteroids are effective in reducing inflammation and alleviating symptoms of hives, but their use should be limited to severe cases due to possible side effects.”
Alternative Therapies
Some people find relief from hives with methods like acupuncture, herbal supplements, and stress management. These options might not work for everyone. But, they can be part of a full treatment plan.
It’s important to talk to your doctor before trying any alternative therapy. This ensures it won’t harm your other treatments.
Lifestyle Modifications to Manage Hives
Managing hives well needs a mix of lifestyle changes. Making smart choices about what you eat and how you handle stress can really help. This can make your symptoms less bothersome.
Dietary Considerations
What you eat is key in managing hives. Some foods can make symptoms worse, while others can help. Keeping a food diary can help you see how different foods affect you.
- Avoid known allergens: Steer clear of foods you’re allergic to to cut down on hives.
- Opt for anti-inflammatory foods: Eating foods high in omega-3s, like salmon and flaxseeds, can lessen inflammation.
- Stay hydrated: Drinking lots of water is vital for healthy skin and overall health.
It’s smart to limit or avoid foods that often cause hives, like shellfish, nuts, and dairy, if you’re allergic or intolerant to them.
Stress Management Techniques
Stress can trigger hives, so managing it is key to controlling symptoms. Try different stress management methods to find what works for you.
- Meditation and mindfulness: Mindfulness and meditation can lower stress and promote calm.
- Yoga: Yoga can help manage stress and boost your overall health.
- Deep breathing exercises: Simple deep breathing can reduce stress and anxiety.
By adding these lifestyle changes to your daily life, you can manage hives better. This can also reduce how often and how severe hives happen.
When to Seek Medical Attention
It’s important to know when to get medical help if you have hives. Most hives are mild and can be treated with over-the-counter medicines. But, some cases can be serious and even life-threatening.
Signs of Severe Reactions
Severe hives can show up in different ways. Angioedema is one, where the skin and mucous membranes swell quickly. This swelling can be dangerous if it blocks the airways, making it hard to breathe.
Other signs of severe reactions include:
- Swelling of the face, lips, tongue, or throat
- Difficulty breathing or swallowing
- Abdominal cramps
- Rapid heartbeat
- A sudden drop in blood pressure
The release of histamine plays a big role in these reactions. It makes blood vessels widen, causing the symptoms of severe hives.
Emergency Care for Anaphylaxis
In serious cases, hives can be a sign of anaphylaxis, a deadly allergic reaction. If you or someone else has symptoms like trouble breathing, a fast heartbeat, or low blood pressure, call emergency services right away.
If you have an EpiPen or something like it, use it to help while waiting for help to arrive. Remember, anaphylaxis is a medical emergency that needs quick treatment.
Preventive Measures for Hives
To prevent hives, we need to understand and manage what causes them. By knowing and avoiding certain allergens and irritants, we can lower the chance of getting hives.
Identifying and Avoiding Triggers
Finding out what triggers hives is the first step. Common culprits include some foods, insect bites, and certain medicines. Keeping a diary to track when hives happen and what might have caused them is very helpful.
- Watch what you eat and note any foods that might cause hives.
- Stay away from known allergens, like certain insect bites or medicines.
- Wear long sleeves and pants when you’re outside to protect yourself.
A study in the Journal of Allergy and Clinical Immunology says avoiding known triggers is key to managing chronic hives.
Journal of Allergy and Clinical Immunology
Allergist Consultation
Talking to an allergist can give you advice and a treatment plan that fits you. They can help figure out what triggers your hives and suggest ways to avoid them.
|
Benefits of Consulting an Allergist |
Description |
|---|---|
|
Personalized Treatment Plans |
Allergists make plans that fit your specific needs and triggers. |
|
Trigger Identification |
Allergists use tests to find out what allergens are causing your hives. |
|
Preventive Strategies |
Allergists suggest ways to avoid triggers and manage hives. |
By working with an allergist and being proactive about managing triggers, you can reduce hives and live better.
Hives in Children
Hives in children are a common issue that worries both kids and their parents. They appear as itchy, raised welts on the skin. This can be scary, as they often show up suddenly.
It’s important to know what causes hives in kids and how to treat them. This helps keep them comfortable and healthy.
Common Causes in Pediatric Cases
In kids, hives can be caused by many things, just like in adults. But, the reasons might be different. Some common causes include:
- Allergic reactions to foods, insect bites, or medicines.
- Infections, like viral or bacterial ones, that can cause hives.
- Environmental factors, like cold, heat, or sunlight.
Also, kids with allergies like eczema or asthma might get hives more often.
Treatment Differences from Adults
While some treatments for hives are the same for everyone, kids need special care. This includes:
- Antihistamines are used, but the dose must fit the child’s age and weight.
- Corticosteroids might be used for serious cases, but with caution because of side effects in kids.
We also suggest non-medical ways to help, like keeping the child cool and avoiding triggers. This can ease their symptoms.
In summary, hives in children can be upsetting. But, knowing what causes them and how to treat them can make a big difference. It helps kids feel better and stay healthy.
Hives vs. Other Skin Conditions
It’s important to know the difference between hives and other skin conditions. Hives, or urticaria, can look like other skin problems. But, they have unique signs that make them stand out.
Distinguishing Hives from Eczema
Eczema, also known as atopic dermatitis, is a long-term condition. It makes the skin itchy and inflamed. Hives and eczema both cause itching and skin irritation, but they are different in many ways.
Key differences between hives and eczema:
- Hives are raised, itchy welts that can appear anywhere on the body. Eczema usually causes dry, scaly patches.
- Hives often come and go, sometimes disappearing in 24 hours. Eczema is a lasting condition.
- Hives can be caused by many things, like allergic reactions. Eczema is often linked to genetics and the environment.
|
Characteristics |
Hives |
Eczema |
|---|---|---|
|
Appearance |
Raised, itchy welts |
Dry, scaly patches |
|
Duration |
Can resolve within 24 hours |
Chronic condition |
|
Triggers |
Allergic reactions, infections |
Genetic predispositions, environmental factors |
Understanding Hives versus Rashes
Not all rashes are hives. Knowing the difference is key for the right treatment. Rashes can be caused by many things, like infections, allergic reactions, and irritants.
Identifying hives: Hives are known for being raised and itchy. They can be different sizes and often appear in groups. They can be triggered by allergic reactions or other factors.
If you have symptoms like bumps on the back of your tongue or need the best allergy medicine, see a healthcare professional. They can give you a proper diagnosis and treatment plan.
Living with Chronic Urticaria
Chronic urticaria can be tough to handle, but it’s possible to live an active life. We know that dealing with hives involves more than just physical symptoms. It also affects your emotions.
Coping Mechanisms
Finding ways to cope is key when you have chronic urticaria. This means staying away from things that trigger hives, eating well, and getting help from doctors and support groups. Knowing how urticaria affects your life helps you manage it better.
Support Networks
Talking to others who have hives can be really helpful. Support groups and online communities are great places to share stories and get advice. They show you that you’re not alone in this fight. We suggest checking out these resources to help you understand and manage your condition better.
FAQ
What is urticaria, and how is it different from other skin rashes?
Urticaria, or hives, is a skin condition with itchy, raised welts. It stands out from other rashes because of its unique look and how the body reacts. This often involves the release of histamine.
What are the main causes of hives, and how can they be identified?
Hives can come from allergic reactions, infections, environmental factors, or stress. Finding the cause involves a detailed medical history and physical check-up. Sometimes, tests like skin tests or blood tests are needed.
How do antihistamines work in treating hives, and what are their possible side effects?
Antihistamines block histamine receptors to lessen hives symptoms. Common side effects include feeling sleepy, dry mouth, and dizziness. But, newer antihistamines have fewer side effects.
Can dietary changes help manage hives, and what foods are commonly associated with triggering hives?
Yes, changing your diet can help with hives. Foods like shellfish, nuts, milk, eggs, and wheat often trigger them. Keeping a food diary can help find specific triggers.
How does stress trigger or worsen hives, and what stress management techniques are effective?
Stress can make hives worse by activating the immune system and releasing histamine. Good stress management includes meditation, yoga, deep breathing, and regular exercise.
What are the signs of a severe allergic reaction, and when should emergency care be sought?
A severe allergic reaction, or anaphylaxis, shows as trouble breathing, fast heartbeat, dizziness, and low blood pressure. Seek emergency care right away if you see these signs.
How can hives be prevented, and what role does an allergist play in managing the condition?
Preventing hives means avoiding triggers, staying healthy, and managing stress. An allergist helps find the cause, creates a treatment plan, and offers advice on managing hives.
Are there differences in the causes and treatment of hives in children compared to adults?
Yes, hives in children can have different causes and treatments than in adults. In kids, common causes include viral infections and allergies. Treatment for children must consider their age, weight, and health.
How can one differentiate hives from other skin conditions like eczema?
Hives are known for their itchy, raised welts that can appear anywhere. Eczema, on the other hand, has dry, scaly patches in specific areas.
What coping strategies and support resources are available for living with chronic urticaria?
To cope with chronic urticaria, keep a symptom diary, follow treatment plans, and manage stress. Support comes from online communities, support groups, and counseling. They offer emotional support and practical advice.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/29567674/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News



















