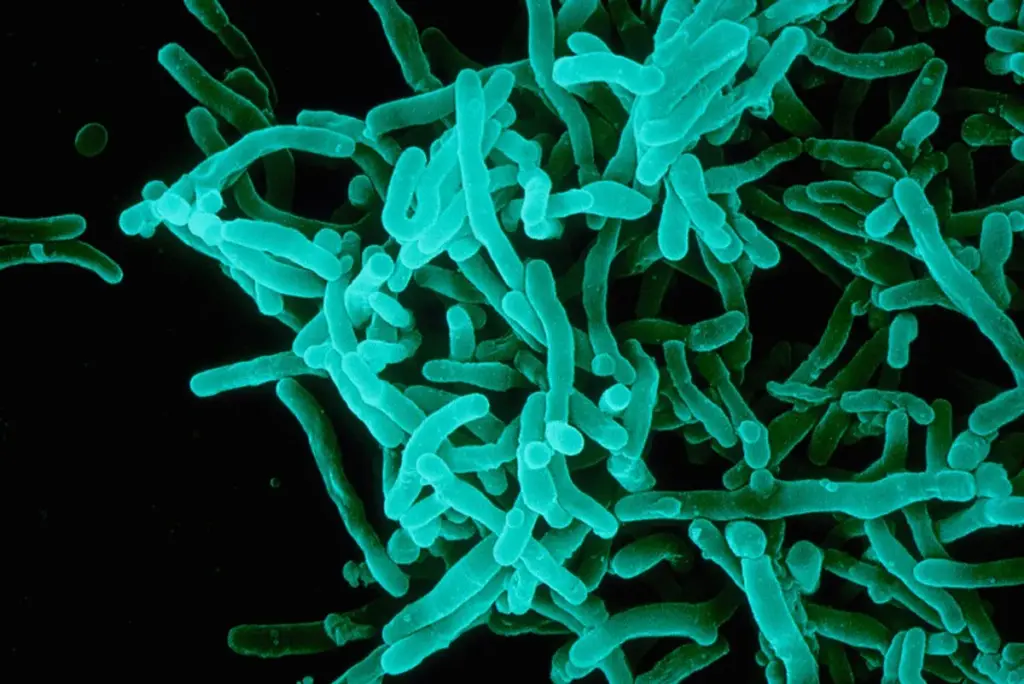
Corynebacterium infections are becoming a big problem in healthcare today. These bacteria are shaped like rods or circles and don’t move. They can cause infections in the throat, lungs, and urinary tract.
At Liv Hospital, we know how important it is to identify and test these bacteria correctly. There are over 80 types of Corynebacterium, and each can resist antibiotics differently. We aim to provide top-notch care for international patients. This includes making sure we have the right antibiotics to treat these infections effectively.
Key Takeaways
- Accurate identification of Corynebacterium species is critical for effective treatment.
- Antibiotic susceptibility testing is essential due to variable resistance patterns.
- According to the Johns Hopkins ABX Guide, certain species, such as C. tuberculostearicum, may be misidentified by lab and often exhibit multidrug resistance.
- C. urealyticum can cause genitourinary infections that may progress to bacteremia and endocarditis.
- C. striatum is an emerging nosocomial pathogen associated with various infections.
Understanding Corynebacterium Species and Their Clinical Significance
More than 80 Corynebacterium species have been found, with over 50 causing human infections sometimes. This shows how hard it is to diagnose and treat these infections.
The Corynebacterium genus includes Corynebacterium diphtheriae, which causes diphtheria. Other species like C. pseudodiphtheriticum, C. propinquum, and C. accolens can also cause infections.
Diversity of Corynebacterium Species
The Corynebacterium genus is very diverse. Different species have different traits and can be more or less harmful. This diversity is key to understanding these bacteria’s impact on health.
Pathogenic Potentia in Human Infections
Corynebacterium species can lead to many infections in humans. These can range from small infections to serious diseases. The harm they cause depends on the host’s immune system.
Corynebacterium diphtheriae causes diphtheria, a serious disease. Other species, like C. pseudodiphtheriticum and C. propinquum, mainly harm people with weak immune systems.
Nondiphtherial Corynebacteria (Diphtheroids)
Nondiphtherial corynebacteria, or diphtheroids, are becoming more common in hospitals. They are often seen as contaminants but can cause serious infections in some people.
The table below shows how diphtheroids play a role in infections:
| Infection Type | Common Species Involved | Patient Population |
| Urinary Tract Infections | C. glucuronolyticum, C. urealyticum | Immunocompromised, Catheterized patients |
| Bacteremia | C. jeikeium, C. striatum | Immunocompromised, Patients with indwelling catheters |
| Endocarditis | C. jeikeium, C. striatum | Patients with prosthetic valves, Intravenous drug users |
Clinical Presentations and Diagnosis
Diagnosing Corynebacterium species infections needs a detailed approach. These bacteria can affect many body parts. It’s key for doctors to know the signs and challenges in diagnosing these infections.
Common Infection Sites
Corynebacterium species can infect the respiratory tract, urinary tract, skin, and soft tissues. Urinary tract infections (UTIs) caused by these bacteria, known as diphtheroids in urine, are significant in some groups. Finding these bacteria in urine can be tricky, but they can cause serious infections, mainly in those with weakened immune systems.
Risk Factors in Immunocompromised Patients
People with weakened immune systems face a higher risk of severe Corynebacterium infections. This includes those with HIV/AIDS, undergoing chemotherapy, or who have had organ transplants. These patients often need more intense and focused treatments.
Laboratory Identification and Susceptibility Testing
Getting the right lab tests and knowing how bacteria react to antibiotics is key. The antibiotic resistance of Corynebacterium species can differ a lot. So, testing each species is vital for choosing the best treatment.
| Corynebacterium Species | Common Infection Sites | Notable Antibiotic Resistance |
| C. diphtheriae | Respiratory tract | Penicillin, Erythromycin |
| C. jeikeium | Bloodstream, Catheters | Vancomycin (rare), Multiple antibiotics |
| C. urealyticum | Urinary tract | Multiple antibiotics, including Vancomycin |
Knowing the specific Corynebacterium species and its antibiotic resistance is key. This helps doctors pick the best treatment. It’s important for managing the infection well and lowering the chance of complications.
Effective Corynebacterium Species Treatment Strategies
Corynebacterium species infections are a challenge in healthcare. They need specific treatments based on the type and antibiotic resistance. We will discuss effective treatments, focusing on the best antibiotics and special considerations for each species.
First-Line Antibiotic Options
Vancomycin and linezolid are top choices for treating Corynebacterium infections. They are effective against most species. These drugs are key for serious infections where the exact species is unknown or resistance is a concern.
- Vancomycin works well against many Corynebacterium species.
- Linezolid is a good option for patients needing long-term treatment.
Species-Specific Treatment Approaches
Different Corynebacterium species react differently to antibiotics. So, treatments must be tailored. For example, Corynebacterium striatum may need special treatment because it’s resistant to many drugs. It’s important to refer to a study on antibiotic resistance to choose the right treatment.
Treatment of Urinary Tract Diphtheroids
Diphtheroids in the urinary tract need special treatment. The choice of antibiotic should be based on lab tests to ensure it works. Common treatments include:
- Trimethoprim-sulfamethoxazole for strains that are susceptible.
- Nitrofurantoin as an alternative for simple urinary tract infections.
Duration and Monitoring of Therapy
The length of antibiotic treatment for Corynebacterium infections depends on the infection’s location and severity. It’s vital to monitor therapy closely. This ensures the treatment is working and prevents antibiotic resistance. Regular check-ups and lab tests are key for the best results.
In summary, treating Corynebacterium infections well requires knowing the species, choosing the right antibiotics, and watching the treatment closely. By following these steps, healthcare providers can give the best care to patients with these complex infections.
Conclusion
Getting the right diagnosis and treatment for Corynebacterium species infections is key. We’ve shown how these bacteria are diverse and important in healthcare. We’ve also talked about how to treat them effectively.
It’s important to know how non-diphtherial Corynebacteria, or diphtheroids, can cause infections. This is true, even more so for people with weakened immune systems. It’s also critical in cases where diphtheroids are found in urine.
At our institution, we’re dedicated to top-notch healthcare for everyone. We focus on accurate diagnoses and effective treatments for Corynebacterium species infections. This includes those caused by diphtheroids. Our goal is to help patients get better and provide care with compassion.
FAQ:
What are Corynebacterium species and why are they significant in healthcare?
Corynebacterium species are a wide range of bacteria. Over 80 species have been described. Some can cause infections, mainly in people with weakened immune systems. Knowing about them helps doctors diagnose and treat infections better.
How are Corynebacterium species infections typically diagnosed?
Doctors use lab tests to find and test the bacteria. They check which antibiotics work best. Knowing if a person’s immune system is weak is also key.
What are the common clinical presentations of Corynebacterium species infections?
These infections can show up in different ways. For example, as urinary tract infections or blood infections. It depends on the type of bacteria and the person’s health.
How are Corynebacterium species infections treated?
Treatment focuses on antibiotics that match the bacteria. Doctors choose the best antibiotic based on lab tests. This approach helps treat the infection effectively.
What is the significance of diphtheroids in urine, and how are they treated?
Finding diphtheroids in urine means a urinary tract infection. Doctors need to test the bacteria to choose the right antibiotic. Knowing how harmful these bacteria can be is important for treatment.
Are Corynebacterium species infections contagious?
Yes, these infections can spread. The risk is higher in hospitals, mainly for people with weak immune systems. Good infection control is vital to stop the spread.
What is the importance of monitoring therapy for Corynebacterium species infections?
Keeping an eye on treatment is key. It ensures the treatment works and makes changes if needed. This is based on how the patient responds and lab tests.
Can Corynebacterium species develop antibiotic resistance?
Yes, they can become resistant to antibiotics. Testing their sensitivity is important for choosing the right treatment.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC172934/

































