
For patients with complex bowel conditions, surgical advancements bring new hope. We know surgery can be scary, but our main goal is to improve your life and independence.Guide to the different types and reasons for ileostomy diversion surgery.
An ileostomy is a surgery that lets stool leave the body without going through the colon or anus. During this, part of the small intestine, called the ileum, is brought through a belly opening, called a
At trusted healthcare places, we offer full care for those needing bowel reconstruction. Bowel diversion methods, like different ileostomies, are designed to fit each person’s needs.
Key Takeaways
- Understanding ileostomy diversion is key for patients facing bowel reconstruction.
- Different types of ileostomy diversion offer tailored solutions for individual needs.
- Bowel diversion techniques can restore quality of life and independence.
- Comprehensive care is available at trusted healthcare institutions.
- Surgical advancements in bowel reconstruction provide new hope for patients.
The Fundamentals of Ileostomy Diversion
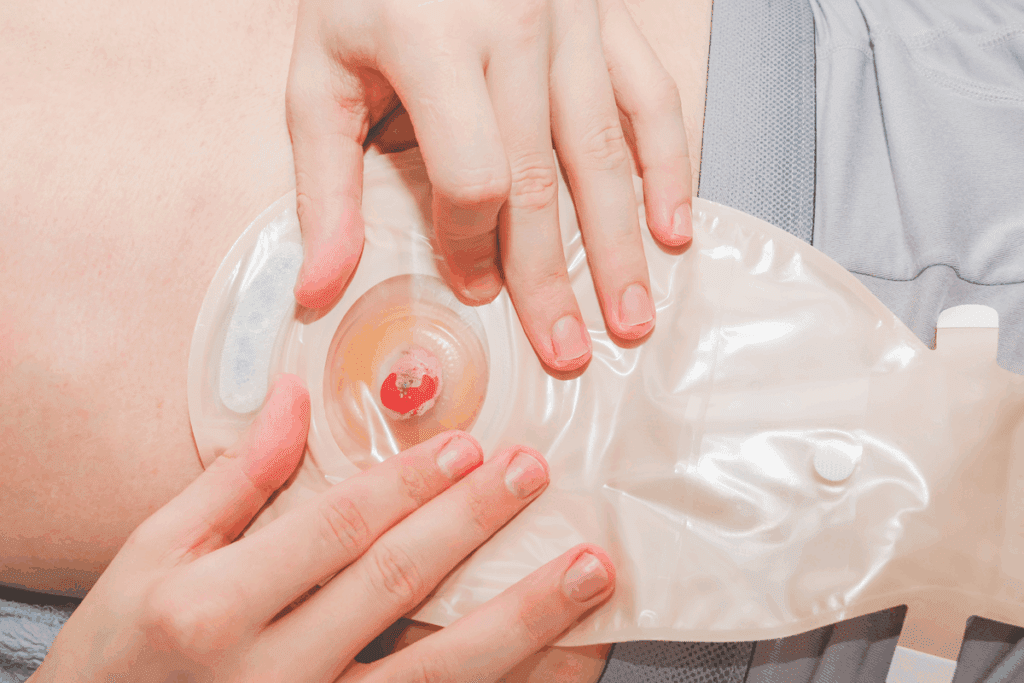
Understanding ileostomy diversion is key for those facing bowel surgery. We’ll cover the basics, like what it is, why it’s done, and if it’s short-term or long-term.
What Is an Ileostomy and Why It’s Performed
An ileostomy is a surgery that makes an opening in the belly. This opening, called a stoma, lets waste from the small intestine go outside. It’s needed when parts of the intestine are damaged or removed.
It’s used for conditions like Crohn’s disease, ulcerative colitis, and colon cancer. The goal is to let the bowel heal or bypass a sick part.
Common Conditions Requiring Bowel Diversion
Ileostomy is often needed for several health issues. Here are some common ones:
- Crohn’s disease: A chronic inflammatory bowel disease that can damage the digestive tract.
- Ulcerative colitis: A condition with chronic inflammation and ulcers in the colon and rectum.
- Colon or rectal cancer: Cancer may need the removal of the affected bowel part.
- Bowel injuries: Damage to the intestines from trauma requires diversion.
Condition | Description | Role of Ileostomy |
Crohn’s Disease | Chronic inflammatory bowel disease | Allows bowel to heal, reduces complications |
Ulcerative Colitis | Chronic inflammation and ulcers in colon and rectum | Bypasses diseased portion, promotes recovery |
Colon or Rectal Cancer | Cancer affecting the colon or rectum | May be used to divert waste during or after cancer treatment |
Temporary vs. Permanent Diversions
Ileostomy diversion can be either short-term or long-term. It depends on the condition and the patient’s health. Temporary ileostomies help the bowel heal after surgery or treatment.
Permanent ileostomies are for when a big part of the bowel is removed or not working. The choice between temporary and permanent depends on the patient’s situation and health.
End Ileostomy: The Standard Approach
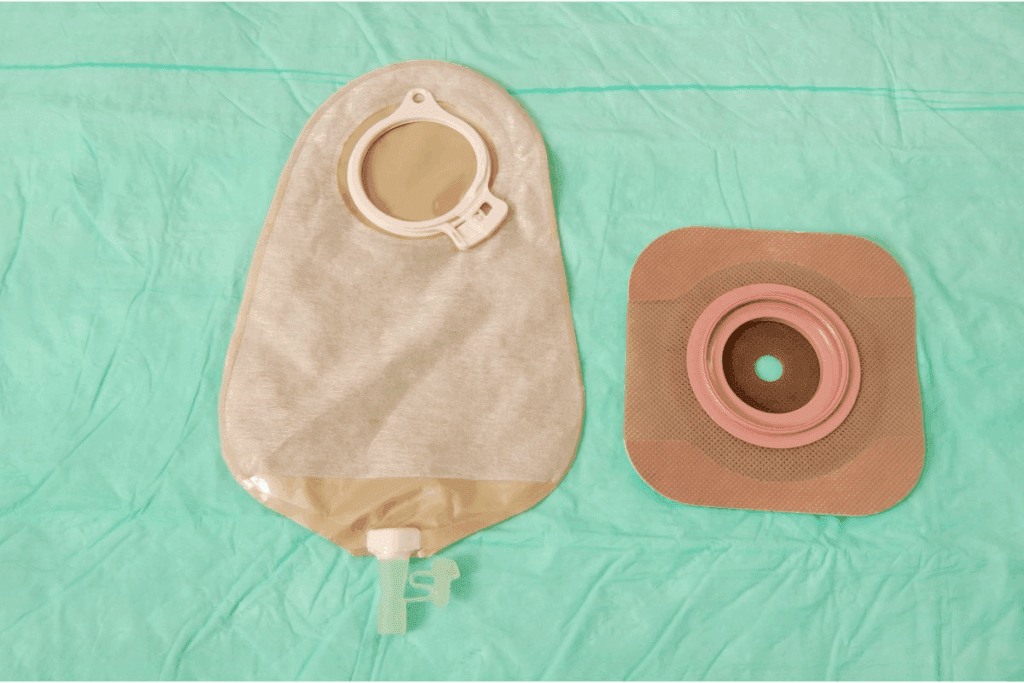
End ileostomy is a common surgery for many gut problems. It makes a stoma by bringing part of the ileum out through the belly. The other part is sealed inside.
Surgical Procedure and Technique
Making an end ileostomy needs careful planning and skill. We start by cutting the belly and finding the ileum. Then, we bring one end out to make the stoma. The other end is closed and goes back inside.
Key steps in the procedure include:
- Identifying the appropriate location for the stoma
- Creating a small incision for the stoma
- Securing the ileum to the abdominal wall
- Forming the stoma to ensure proper function
Stoma Formation and Appearance
The stoma is usually pink or red and 2-3 cm wide. It looks different on everyone, but it’s often even with the skin or a bit out.
Daily Management and Output Characteristics
Looking after an end ileostomy means taking care of the stoma and its output. The output is mostly liquid or semi-liquid. It can be more active after eating.
Characteristics of the output include:
Output Characteristic | Description |
Consistency | Liquid to semi-liquid |
Color | Yellowish to greenish |
Volume | Varies, often higher after meals |
People with an end ileostomy should watch their water intake to stay hydrated. Drinking lots of water and using oral rehydration solutions is a good idea.
Diverting Loop Ileostomy: Temporary Relief
The diverting loop ileostomy is a temporary solution for bowel issues. It involves creating a stoma from a small intestine loop. This allows fecal matter to be diverted.
Surgical Construction and Appearance
A surgeon makes a loop stoma by pulling a small intestine part through the abdomen. The loop is supported by a rod until it heals, usually in a few days to a week. The stoma looks like a loop on the abdomen, with two openings.
Key aspects of the surgical construction include:
- Careful selection of the intestinal loop to ensure proper diversion
- Creation of an appropriate stoma size to facilitate easy management
- Secure fixation of the loop to prevent complications
90% Reversal Rate Advantage
A diverting loop ileostomy has a high reversal rate, about 90%. This means most patients can have their ileostomy reversed. It’s a temporary fix until the bowel heals.
The high reversal rate is advantageous because it:
- Offers patients a chance to regain normal bowel function
- Reduces the long-term commitment to ileostomy management
- May improve quality of life after reversal
Managing Dehydration and Renal Concerns
Patients with a diverting loop ileostomy risk dehydration due to high stoma output. It’s important to manage dehydration to avoid kidney problems.
Strategies for managing dehydration include:
- Increasing fluid intake to compensate for stoma output
- Monitoring urine output and color to assess hydration status
- Adjusting diet to include electrolyte-rich foods or supplements
Understanding a diverting loop ileostomy’s construction, benefits, and risks helps patients manage their treatment and recovery. Proper dehydration management is key to a successful outcome.
Continent Ileostomy (Kock Pouch): Pouch-Based Ileostomy Diversion
The Kock pouch, or continent ileostomy, is a new way to manage ileostomy. It makes life easier for patients. This surgery creates a special pouch inside the body. It lets patients control their ileostomy more easily.
Construction and Internal Reservoir Design
To make a continent ileostomy, a part of the ileum is folded back. This forms a pouch inside the body. The pouch holds fecal matter until the patient empties it.
The pouch is made by folding and sewing the ileum. It can hold 500 to 1000 ml of fecal matter.
Valve Mechanism and Drainage Process
The Kock pouch has a special valve. This valve stops leaks from the stoma. It’s made during surgery by folding the ileum.
Draining the pouch is easy. Patients use a catheter through the stoma. They do this several times a day, as needed.
Ideal Candidates and Contraindications
Not everyone is right for a continent ileostomy. The best candidates are healthy and motivated. They also need to be able to use the catheter.
Those who can’t manage the pouch well shouldn’t get it. This includes people with serious health problems or disabilities. Also, those with Crohn’s disease might not be good candidates because of the risk of the disease coming back.
Criteria | Ideal Candidates | Contraindications |
Health Status | Good overall health | Significant cognitive impairment, severe physical disability |
Motivation | High motivation to manage ileostomy | Lack of motivation or compliance |
Manual Dexterity | Sufficient manual dexterity to perform drainage | Severe arthritis or other conditions affecting hand function |
Loop Colostomy as an Alternative Diversion Method
Loop colostomy is a unique way to divert the bowel. It brings a part of the colon to the skin, making a stoma. This stoma lets waste leave the body without going through the lower colon or rectum. Knowing how it works and compares to other methods is key.
Anatomical Placement and Function
A loop colostomy makes a loop of the colon stick out through the skin. It’s then opened to create a stoma. This stoma lets waste go out, avoiding the lower parts of the colon or rectum. Where the stoma is placed depends on the patient’s needs and the surgeon’s choice.
Comparison to Loop Ileostomy
Loop colostomy and loop ileostomy are both for temporary bowel diversion. But they use different parts of the intestine. Loop ileostomy uses the ileum, while loop colostomy uses the colon. The choice depends on the condition, affected area, and the patient’s health.
Lower Dehydration Risk but Higher Prolapse Rates
Loop colostomy has a lower risk of dehydration than loop ileostomy. The colon absorbs water better than the ileum. But, loop colostomy has a higher risk of stoma prolapse. Proper care and follow-up are needed to manage this risk.
Characteristics | Loop Colostomy | Loop Ileostomy |
Dehydration Risk | Lower | Higher |
Prolapse Risk | Higher | Lower |
Intestinal Segment | Colon | Ileum |
Knowing these differences helps manage patient expectations and outcomes. Choosing the right diversion method improves patient care and quality of life.
IPAA (J-Pouch): Restorative Proctocolectomy
Restorative proctocolectomy with ileal pouch-anal anastomosis (IPAA), also known as J-pouch surgery, is a complex procedure. It offers a cure for some gastrointestinal conditions. This surgery removes the diseased colon and rectum but keeps the anal sphincter. This helps patients stay continent.
The IPAA procedure is for those with ulcerative colitis or familial adenomatous polyposis. It creates a pouch from the small intestine. This way, patients don’t need a permanent ostomy, improving their life quality.
Multi-Stage Surgical Approach
The IPAA procedure is done in stages. First, the colon is removed, and the ileal pouch is created. After a few months, the pouch is connected to the anus. Sometimes, a temporary ileostomy is made to help the pouch heal.
This staged approach helps avoid complications. It ensures the pouch heals well before it’s used for stool storage and evacuation.
Internal Pouch Construction Techniques
Creating the internal pouch is key in IPAA. Surgeons often use a “J” configuration. But, “S” and “W” configurations are used too. The “J-pouch” is made by folding the ileum back and stapling or suturing it.
Pouch Configuration | Description | Advantages |
J-Pouch | Most common configuration, easier to construct | Simplified surgical process, good functional outcomes |
S-Pouch | Provides larger reservoir capacity | Better for patients requiring larger pouch volume |
W-Pouch | Further increases reservoir capacity | Ideal for patients with specific anatomical needs |
Temporary Ileostomy During Healing
A temporary ileostomy is made during IPAA to let the pouch heal. This ileostomy is reversed later when the pouch is healed enough.
“The use of a temporary ileostomy in IPAA surgery significantly reduces the risk of complications, such as pelvic sepsis, by allowing the pouch to heal in a sterile environment.” – Medical Expert, Gastrointestinal Surgeon
The choice to make a temporary ileostomy depends on several factors. These include the patient’s health, the surgery’s complexity, and the surgeon’s preference.
Brooke Ileostomy: The Traditional End Ileostomy
The Brooke ileostomy technique is a key method in surgery today. It was created to make end ileostomies better. This method has been around for a long time because it works well.
Historical Development and Technique
The Brooke ileostomy was made to improve the end ileostomy. It makes the ileum stick out to form a stoma. This change helped avoid problems like skin irritation and leaks.
We will look at how it started and its technical details. These have made it a mainstay in surgery.
Everted Stoma Construction
Making an everted stoma is key in the Brooke ileostomy. By turning the ileum out, surgeons make a stoma that sticks out. This lowers the chance of problems and makes patients do better.
Key steps in everted stoma construction include:
- Careful selection of the stoma site
- Precise eversion of the ileum
- Secure fixation of the stoma to the abdominal wall
Modern Applications and Modifications
Even though the Brooke ileostomy is old, new surgery methods have made changes. These updates aim to cut down on problems and make patients’ lives better.
Aspect | Traditional Brooke Ileostomy | Modern Modifications |
Stoma Construction | Everted ileum | Variations in eversion technique |
Complication Rate | Lower than flush stomas | Further reduced with modern techniques |
Patient Outcomes | Improved manageability | Enhanced quality of life |
The Brooke ileostomy is always getting better. Ongoing research and practice aim to make it even better for patients.
Double-Barrel Ileostomy: Divided Stoma Approach
A double-barrel ileostomy creates two stomas from the ileum. This is done for specific reasons. It’s used when the ileum needs to be divided for treatment or testing.
Surgical Construction and Appearance
To make a double-barrel ileostomy, the ileum is split into two parts. The proximal limb connects to the upper GI tract. The distal limb connects to the lower GI tract or the rest of the intestine.
The stomas look different, but they’re usually close together on the belly. The proximal stoma is more active and handles the main flow of waste.
Functional Differences Between Proximal and Distal Limbs
The proximal limb diverts waste, making it more active. It’s key for handling the main flow of waste.
The distal limb has little to no output. It’s not the main flow but is important for future use or tests.
Clinical Indications and Specific Uses
Double-barrel ileostomy is used in several situations:
- Severe intestinal disease or trauma needing diversion
- Need for diagnostic access to both the proximal and distal intestine
- Situations where future reconnection is anticipated
Clinical Scenario | Indication for Double-Barrel Ileostomy | Benefits |
Severe Intestinal Disease | Diversion of fecal matter to allow healing | Reduces risk of complications, promotes healing |
Intestinal Trauma | Temporary diversion to manage trauma | Allows for recovery, reduces morbidity |
Diagnostic Needs | Access to both proximal and distal intestine | Facilitates diagnostic procedures, potentially avoids additional surgeries |
In conclusion, the double-barrel ileostomy is a valuable surgical method. It has specific uses and benefits. Knowing how it works and when it’s used is key for healthcare and patients.
Living with an Ileostomy: Practical Considerations
Living with an ileostomy can be tough, but it’s possible to live well. You need to make some key adjustments to feel good. These changes help you stay healthy and happy.
Dietary Adjustments and Hydration
Starting with the right diet is key. Drinking lots of water is important because your ileostomy can make you lose a lot of fluids. Try to drink 8-10 glasses of water a day. This amount can change based on how active you are and your personal needs.
Eating a balanced diet is also important. Foods high in fiber might be hard to digest at first. So, start with small amounts. Also, avoid foods that can make gas or smells, like beans and broccoli, if they bother you.
Food Type | Recommended | To Be Avoided |
Proteins | Lean meats, fish, eggs | High-fat meats |
Fruits | Bananas, applesauce | High-fiber fruits like berries |
Vegetables | Cooked vegetables | Raw, high-fiber vegetables |
Physical Activity and Lifestyle Adaptations
Being active is good for your health, even with an ileostomy. But, avoid heavy lifting or bending at first. This helps prevent problems with your stoma.
Wear comfy clothes that don’t press on your stoma. Use the right ostomy bags and accessories for an active life.
Psychological Impact and Support Resources
The mental side of living with an ileostomy is important too. Getting support from doctors, support groups, and family is key. Talking to others who have gone through the same thing can be really helpful.
There are many resources like counseling, online forums, and support groups. They offer advice and emotional support. This helps you deal with the changes and live a good life.
By choosing the right foods, staying hydrated, being active, and getting mental support, you can manage your ileostomy well. You can live a fulfilling life despite the challenges.
Conclusion: Selecting the Right Ileostomy Diversion
Choosing the right ileostomy diversion is very important. It greatly affects how we manage bowel conditions. We’ve looked at different ileostomy types, like end ileostomy, diverting loop ileostomy, and continent ileostomy. Each has its own benefits and features.
It’s key to know the differences between these types. The right choice depends on your health, medical condition, and what you prefer. For example, a continent ostomy might be good for some, as it doesn’t need an external bag.
Every ileostomy type has its own perks and is best for certain people. By thinking about these points and talking to doctors, you can pick the best option for you. This can really improve your life quality.
FAQ
What is an ileostomy diversion?
An ileostomy diversion is a surgery that makes a hole in the belly. This hole, called a stoma, lets stool go outside the body instead of through the anus.
What is the difference between a temporary and permanent ileostomy?
A temporary ileostomy is for healing and can be reversed. It’s used after surgery or injury. A permanent ileostomy is for long-term needs, like with some diseases or cancer.
What are the different types of ileostomy diversion?
There are several types. These include end ileostomy, diverting loop ileostomy, and continent ileostomy (Kock pouch). Others are Brooke ileostomy and double-barrel ileostomy.
What is a continent bowel meaning in the context of ileostomy?
A continent bowel is a pouch made in surgery. It stores stool for controlled release, like in a Kock pouch ileostomy.
How is dehydration managed in patients with ileostomy?
To fight dehydration, patients drink more water. They also watch their output and adjust their diet. Medications can help slow down bowel movements.
Where is an ileostomy typically placed?
Surgeons usually place an ileostomy in the right lower belly. They consider the patient’s body and their own preference.
Can patients with ileostomy have bowel movements through the anus?
Usually, no. A permanent ileostomy diverts stool away from the anus. But, some may regain function after certain surgeries or with certain types of ileostomy.
What is the role of temporary ileostomy during IPAA (J-Pouch) surgery?
A temporary ileostomy is used during IPAA surgery. It helps the pouch heal, reducing risks of problems.
What are the advantages of diverting loop ileostomy?
Diverting loop ileostomy is reversible, making it good for temporary use. It might allow for normal bowel function later.
What is the difference between loop ileostomy and loop colostomy?
Loop ileostomy diverts the small intestine’s end, while loop colostomy diverts the colon. Ileostomy risks dehydration, while colostomy risks prolapse.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC10781852/


































