Infectious diseases specialists diagnose and treat infections from bacteria, viruses, fungi, and parasites, focusing on fevers, antibiotics, and vaccines.
Send us all your questions or requests, and our expert team will assist you.

The diagnostic evaluation of Hepatitis B is a sophisticated process that relies on the interpretation of a complex array of serological markers and molecular quantification. At Liv Hospital, the diagnostic pathway is designed not only to confirm the presence of the virus but to precisely stage the infection, assess the degree of liver injury, and determine the patient’s eligibility for treatment. The evaluation moves beyond a simple binary positive/negative result to construct a detailed immunological and virological profile of the patient. This precision is vital for distinguishing between acute infection, chronic active hepatitis, and the inactive carrier state.
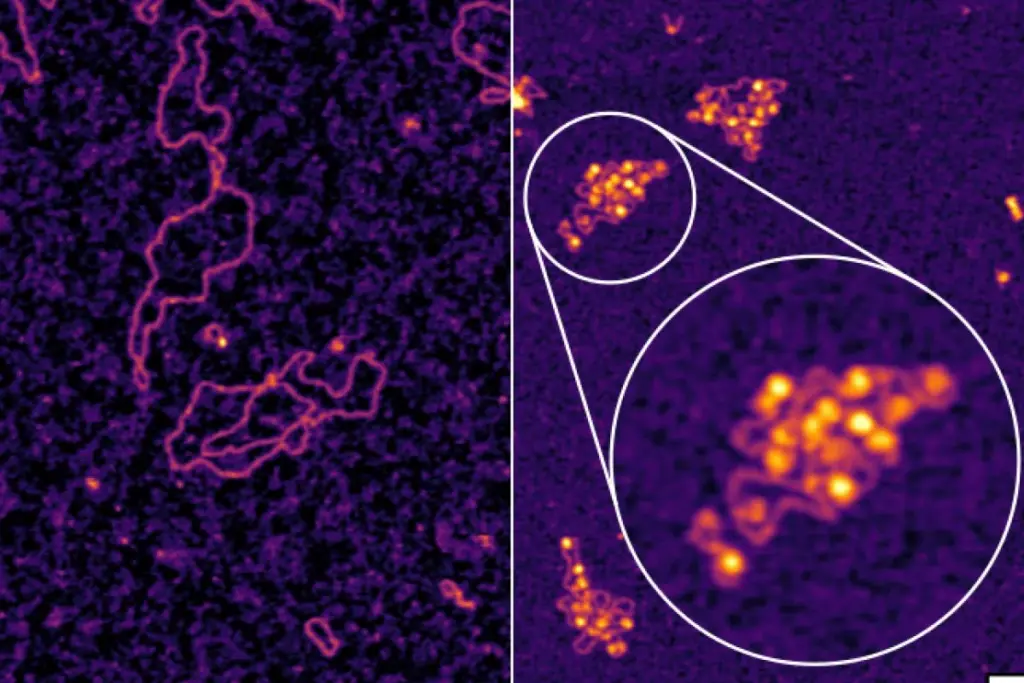
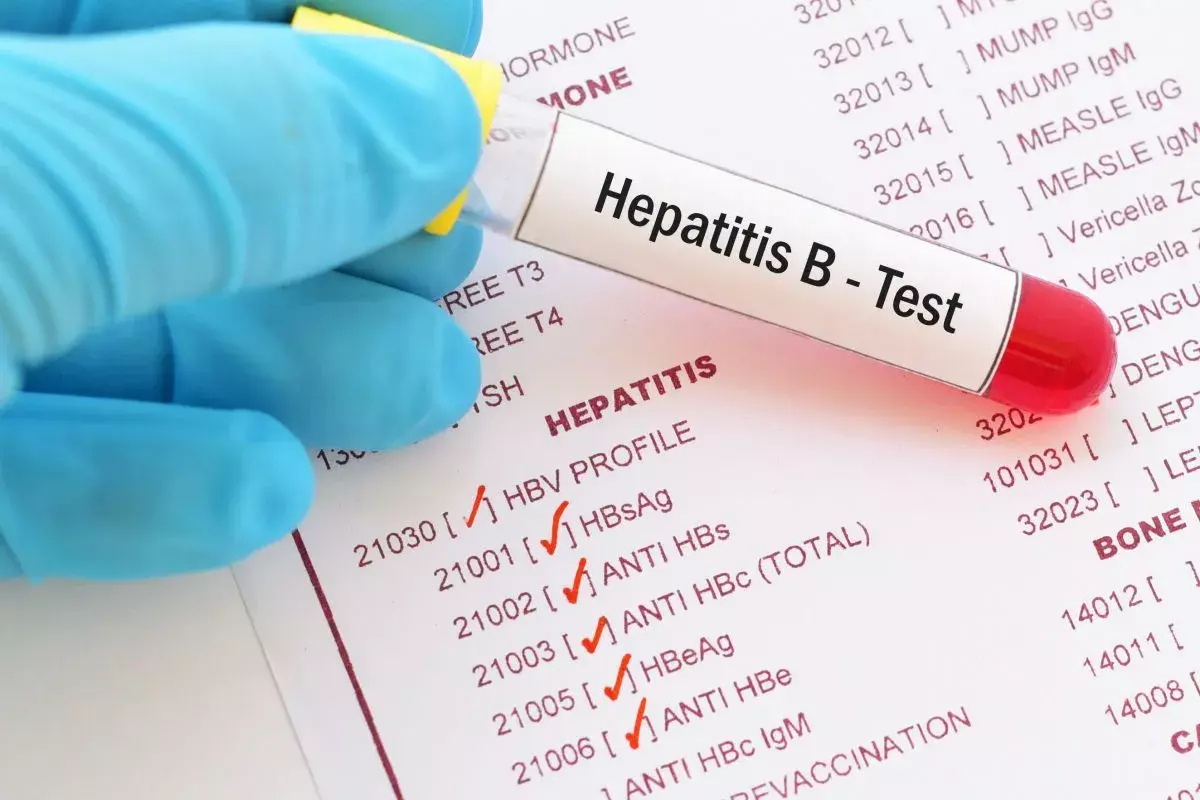
The diagnosis of Hepatitis B relies on detecting specific viral antigens (viral proteins) and antibodies (host immune proteins) in the blood. The interpretation of these markers provides a timeline of the infection.
Hepatitis B e-Antigen (HBeAg):
This protein is secreted by infected cells during active viral replication. Its presence indicates high infectivity. Seroconversion, or the loss of HBeAg and the development of anti-HBe is a key therapeutic endpoint signaling a reduction in viral replication.
While serology defines the status of the infection, molecular diagnostics quantify the burden of the disease. Measurement of HBV DNA by Polymerase Chain Reaction (PCR) is the gold standard for assessing viral replication.

Evaluating the impact of the virus on the liver parenchyma is a critical component of the diagnostic phase. Chronic inflammation leads to fibrosis, which must be staged accurately.
Liver Biopsy:
While less common due to the advent of elastography, liver biopsy remains the gold standard for equivocal cases. It involves the histological examination of liver tissue to assess the grade of necroinflammation and the stage of fibrosis, and to rule out other co-existing liver pathologies.
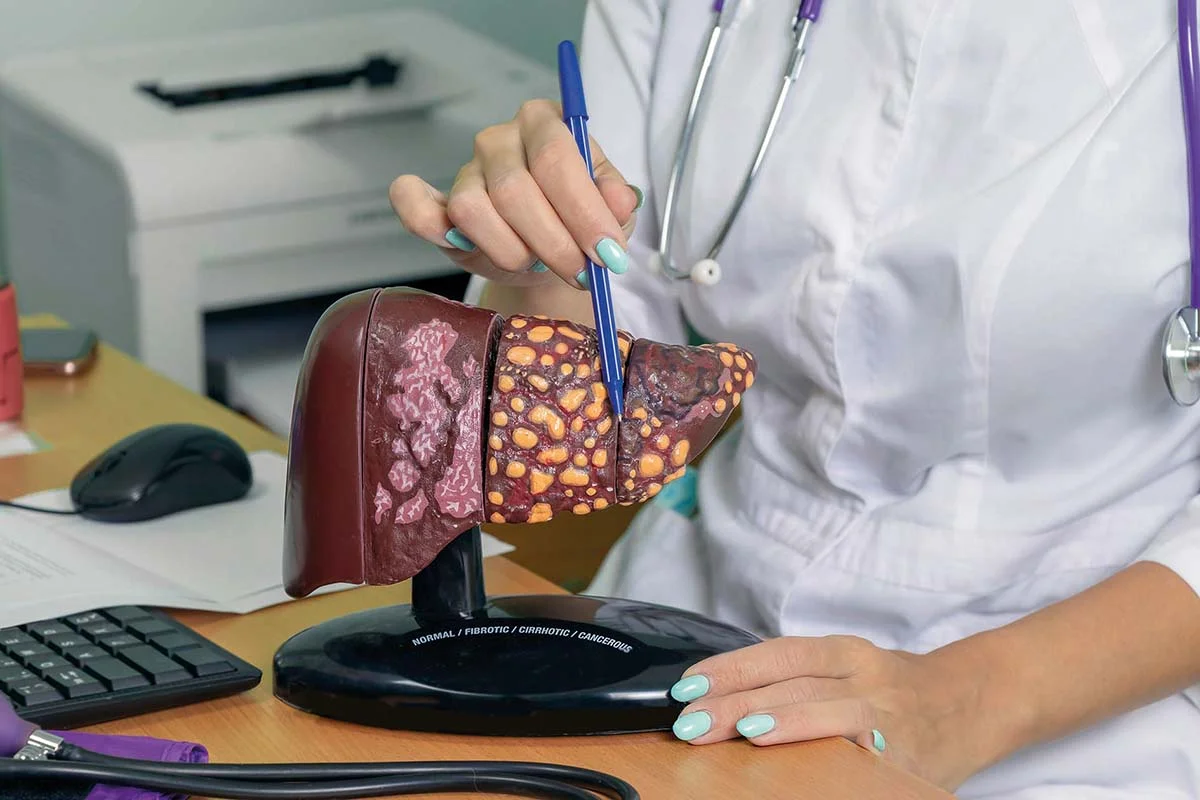
Given the oncogenic potential of HBV, the diagnostic evaluation includes rigorous screening for liver cancer.
Because Hepatitis B shares transmission routes with other viruses, a complete evaluation includes screening for co-infections with Hepatitis C (HCV), Hepatitis D (HDV), and Human Immunodeficiency Virus (HIV). Co-infection with HDV, a defective satellite virus that requires HBV for replication, causes the most severe form of chronic viral hepatitis and requires specific testing protocols.

Send us all your questions or requests, and our expert team will assist you.
If your test results show a negative Hepatitis B surface antigen (HBsAg) and a positive antibody to the surface antigen (anti-HBs), it typically means you are immune to Hepatitis B. This immunity could result from a past infection your body successfully cleared, or from vaccination. In either case, you are protected from future infection and cannot transmit the virus.
Knowing you have the virus is only the first step. The HBV DNA test (viral load) tells the doctor exactly how much virus is circulating in your blood. This information is crucial for deciding whether you need treatment right now. It helps predict the risk of liver damage and is the most essential tool for monitoring the effectiveness of antiviral medications.
The window period is a specific timeframe during an acute Hepatitis B infection. It occurs when the surface antigen (HBsAg) has disappeared from the blood (as the body clears it), but the protective antibody (anti-HBs) has not yet appeared at detectable levels. During this gap, a person might test negative for both, potentially leading to a missed diagnosis if the core antibody (anti-HBc) is not also checked.
No, a liver biopsy is no longer always necessary. Modern medicine uses non-invasive technologies such as Transient Elastography (FibroScan). This technology uses sound waves to measure liver stiffness, which correlates with the extent of scarring (fibrosis). It is painless, quick, and avoids the risks of bleeding or pain associated with a needle biopsy.
Yes, specific markers help distinguish the two. The presence of IgM antibody to the core antigen (IgM anti-HBc) is the defining marker for acute infection. If this marker is absent but the surface antigen (HBsAg) and total core antibody (anti-HBc IgG) are present, it indicates a chronic disease of long duration.


Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)